NLN NEX SCIENCE PRACTICE TEST
Prepare for nursing school admission by strengthening your understanding of essential science concepts commonly assessed on the entrance exam.
Topics Covered
Human anatomy and physiology
Basic biology principles
Chemistry fundamentals
Body systems overview
Scientific reasoning
Health-related science concepts
00:00
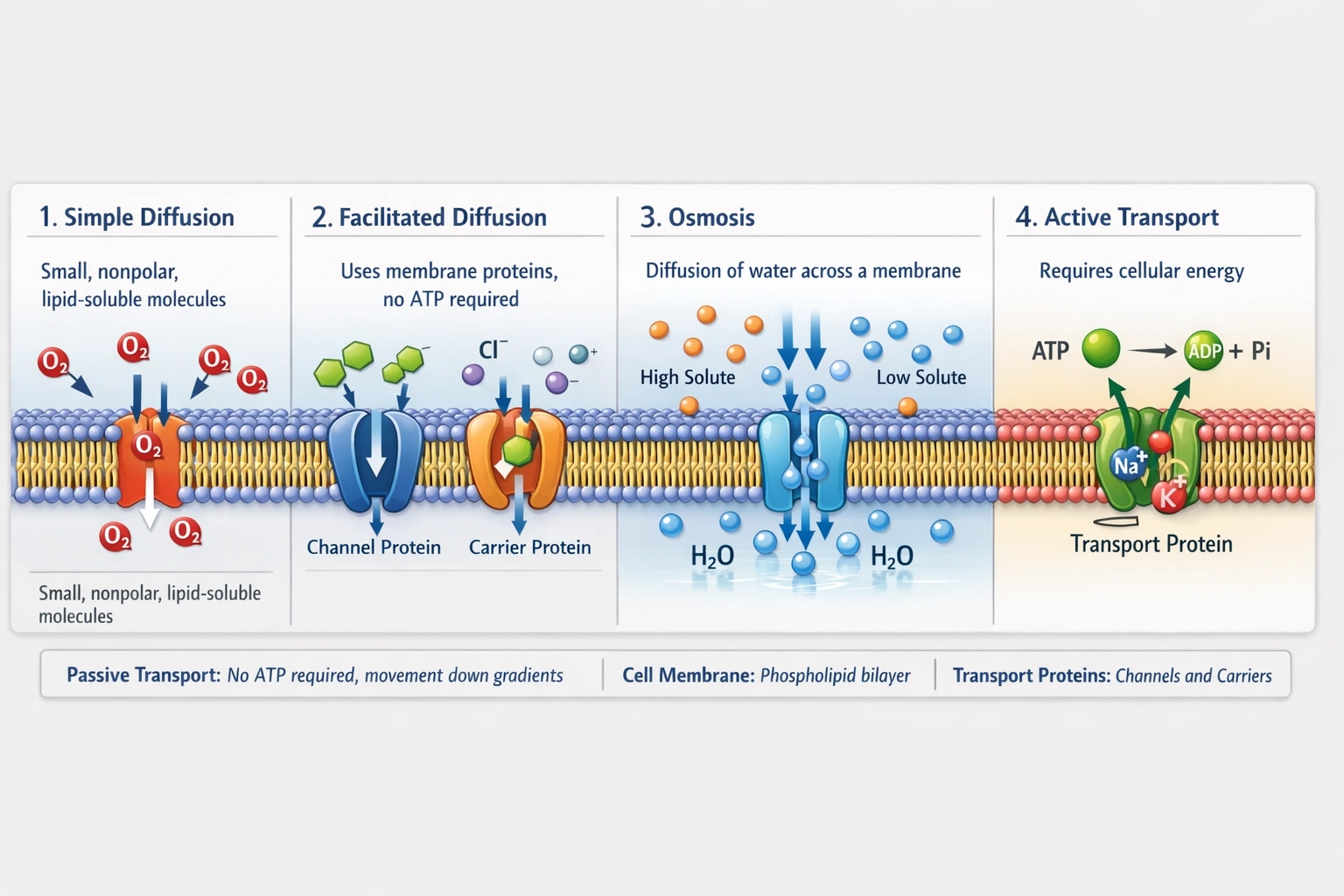
What types of molecules can move through a cell membrane by passive transport?
A.
Complex sugars
B. Non-lipid soluble molecules
C. Oxygen
D. Molecules moving from areas of low concentration to areas of high concentration
Rationale
Oxygen moves through cell membranes via passive transport as a small, nonpolar, lipid-soluble molecule that diffuses directly through the phospholipid bilayer down its concentration gradient without energy expenditure or protein assistance.
Passive transport encompasses diffusion and osmosis mechanisms where molecules move spontaneously down electrochemical gradients without cellular energy input—restricted to small, nonpolar molecules that dissolve in membrane lipids or specific substances using channel/carrier proteins without ATP hydrolysis.
A) Complex sugars
Complex sugars (e.g., sucrose, starch) are large, polar molecules that cannot diffuse through the hydrophobic lipid bilayer interior. They require facilitated diffusion via specific carrier proteins (e.g., GLUT transporters for glucose) or active transport against gradients. Even simple monosaccharides like glucose need protein assistance; complex polysaccharides cannot cross membranes intact and must be hydrolyzed extracellularly first.
B) Non-lipid soluble molecules
Non-lipid soluble (hydrophilic/polar) molecules cannot dissolve in the membrane's hydrophobic core and thus cannot diffuse directly through the bilayer. They require transport proteins—either channel proteins forming hydrophilic pores (e.g., aquaporins for water) or carrier proteins undergoing conformational changes (e.g., glucose transporters). Without these proteins, non-lipid soluble molecules remain membrane-impermeable regardless of concentration gradients.
C) Oxygen
Oxygen (O₂) is a small, nonpolar diatomic molecule with high lipid solubility that dissolves readily in the phospholipid bilayer's hydrophobic region. It diffuses passively down partial pressure gradients—from alveoli (high pO₂) into pulmonary capillaries (low pO₂), then from systemic capillaries into oxygen-depleted tissues. This simple diffusion requires no membrane proteins or energy expenditure, exemplifying ideal passive transport for respiratory gas exchange essential to aerobic metabolism.
D) Molecules moving from areas of low concentration to areas of high concentration
Movement against concentration gradients defines active transport requiring energy input (ATP hydrolysis or electrochemical coupling), not passive transport. Passive transport exclusively moves substances down gradients (high → low concentration) driven by entropy increase. Low-to-high movement violates the second law of thermodynamics without energy coupling—making this option fundamentally incompatible with passive transport definition.
Conclusion:
Passive transport mechanisms permit only specific molecule types to cross membranes without energy: small nonpolar molecules (O₂, CO₂, N₂) via simple diffusion through lipids; small uncharged polar molecules (H₂O, urea) slowly via lipid solubility or rapidly via channel proteins; and ions/polar molecules via facilitated diffusion through selective protein channels/carriers—all moving exclusively down electrochemical gradients. Oxygen exemplifies ideal passive transport as a small nonpolar gas diffusing directly through lipids. Options A and B describe molecules requiring protein assistance (still passive if down-gradient, but not simple diffusion), while D describes active transport. Option C correctly identifies a molecule utilizing pure passive diffusion—fundamental to respiratory physiology where oxygen delivery depends entirely on gradient-driven membrane permeability without cellular energy expenditure.
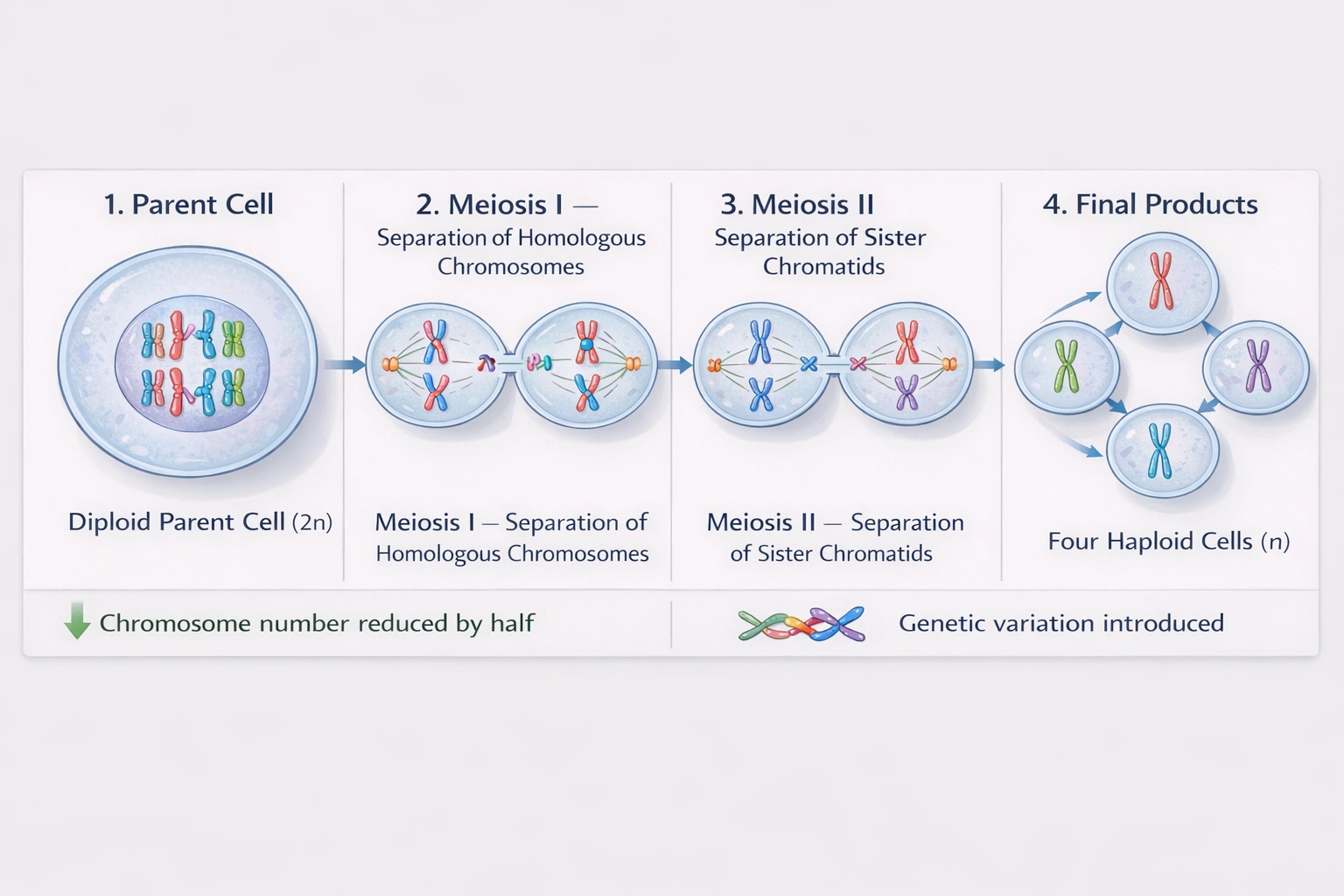
How many daughter cells are formed from one parent cell during meiosis?
A.
One
B. Two
C. Three
D. Four
Rationale
Meiosis produces four haploid daughter cells from a single diploid parent cell through two consecutive divisions (meiosis I and II) without intervening DNA replication, reducing chromosome number by half for sexual reproduction.
Meiosis I separates homologous chromosome pairs (reduction division), yielding two haploid cells with duplicated chromosomes; meiosis II separates sister chromatids (equational division), producing four haploid gametes each containing unduplicated chromosomes—enabling fertilization to restore diploidy.
A) One
Single daughter cell production characterizes asymmetric cell division (e.g., stem cell self-renewal) or failed cytokinesis—not meiosis. Meiosis fundamentally increases cell number while reducing ploidy, making single-cell output incompatible with its reproductive purpose of generating multiple gametes for genetic diversity.
B) Two
Mitosis produces two diploid daughter cells genetically identical to the parent. Meiosis I alone yields two haploid cells, but these undergo meiosis II to produce four final gametes. Stopping after meiosis I would yield cells with duplicated chromosomes unsuitable for fertilization—biologically nonfunctional as gametes require unduplicated haploid chromosomes.
C) Three
No standard eukaryotic cell division process yields three daughter cells. Unequal cytokinesis might theoretically produce three cells in rare pathological conditions, but meiosis follows strictly symmetrical division patterns producing four functional gametes (sperm) or one functional gamete plus polar bodies (oogenesis)—never three viable products.
D) Four
Spermatogenesis exemplifies standard meiotic output: one diploid spermatogonium undergoes meiosis I → two haploid secondary spermatocytes; each undergoes meiosis II → four haploid spermatids that mature into spermatozoa. Oogenesis produces one functional ovum plus two or three polar bodies (which degenerate), but the meiotic mechanism still generates four cellular products—only one becomes the functional gamete due to asymmetric cytokinesis conserving cytoplasm for embryonic development. The fundamental meiotic process creates four haploid nuclei regardless of cytoplasmic distribution.
Conclusion:
Meiosis' defining outcome is four haploid cells from one diploid precursor—essential for halving chromosome number prior to fertilization. While oogenesis modifies cytoplasmic distribution to produce one large ovum and small polar bodies, the nuclear division mechanism still generates four haploid nuclei through two sequential divisions. Option D correctly identifies the universal meiotic product count fundamental to sexual reproduction's chromosome number stability across generations. This four-cell output enables genetic recombination diversity through independent assortment and crossing over—cornerstones of evolutionary adaptation that distinguish meiosis from mitotic cloning.
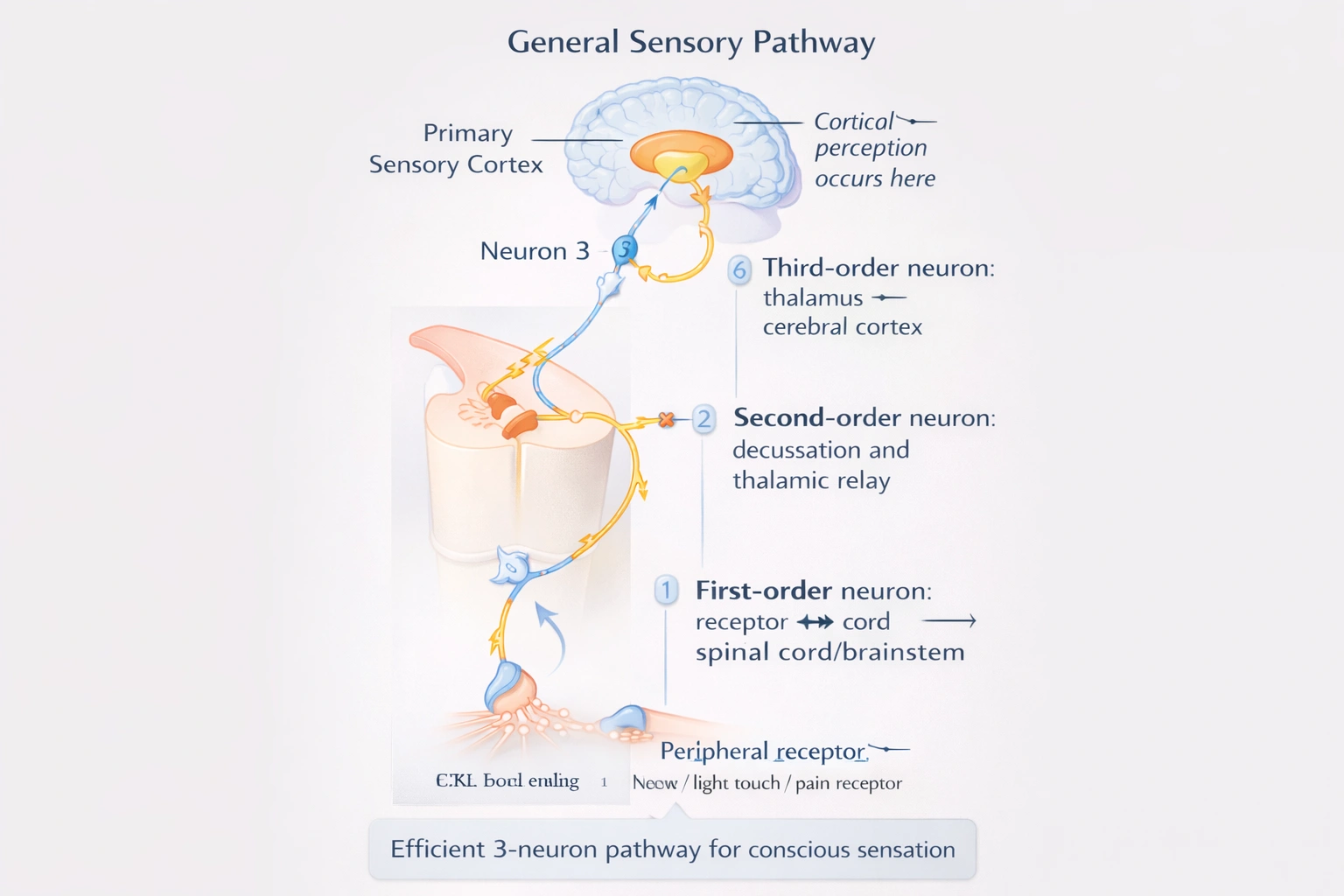
How many neurons generally make up a sensory pathway?
A.
1
B. 2
C. 3
D. 4
Rationale
Most conscious sensory pathways consist of three neurons connecting peripheral receptors to the cerebral cortex: first-order neurons (receptor to spinal cord/brainstem), second-order neurons (decussating to thalamus), and third-order neurons (thalamus to cortex).
This three-neuron chain enables sensory information transmission from body periphery to conscious perception centers while incorporating essential processing steps including decussation (crossing to opposite brain hemisphere) and thalamic relay/integration.
A) 1
Single-neuron pathways exist only for some autonomic reflexes or invertebrate nervous systems—not for conscious sensation in vertebrates. Direct receptor-to-cortex connections would lack essential processing stages (decussation, thalamic gating/modulation) required for organized sensory perception and contralateral representation in the cortex.
B) 2
Two-neuron pathways occur in some unconscious proprioceptive circuits (e.g., spinocerebellar tracts to cerebellum) but not for conscious sensation reaching the cortex. Cortical sensory perception universally requires thalamic relay—making two-neuron chains insufficient for conscious awareness. The thalamus serves as the "gateway to cortex" for all sensory modalities except olfaction.
C) 3
The three-neuron organization characterizes major conscious sensory pathways:
• Dorsal column-medial lemniscus pathway (fine touch, vibration, proprioception): First-order neurons enter spinal cord and ascend ipsilaterally to medulla; second-order neurons decussate in medulla and project to thalamus; third-order neurons project from thalamus to primary somatosensory cortex.
• Spinothalamic tract (pain, temperature, crude touch): First-order neurons synapse in dorsal horn; second-order neurons decussate in spinal cord and ascend to thalamus; third-order neurons project to cortex.
• Visual pathway: Retinal ganglion cells (first-order) → lateral geniculate nucleus (second-order) → primary visual cortex (third-order).
• Auditory pathway: Spiral ganglion neurons (first-order) → cochlear nuclei/inferior colliculus/medial geniculate nucleus (second-order processing) → primary auditory cortex (third-order).
D) 4
Four-neuron chains occur rarely in specialized pathways (e.g., some olfactory circuits) but aren't the general pattern for somatic sensation. Most sensory systems optimize transmission efficiency with three neurons—adding a fourth would introduce unnecessary synaptic delay without significant processing benefit for conscious perception.
Conclusion:
The three-neuron sensory pathway represents a conserved vertebrate neuroanatomical pattern balancing transmission speed with essential processing requirements: peripheral transduction (first-order), decussation and initial integration (second-order), and cortical delivery with attentional modulation (third-order via thalamus). Option C correctly identifies this universal organization fundamental to sensory neuroscience—explaining why cortical lesions produce contralateral sensory deficits (due to decussation at second-order neuron level) and why thalamic damage causes profound sensory impairment despite intact peripheral pathways. This tripartite organization enables both rapid reflex responses (via spinal cord branching) and conscious perception through cortical processing.
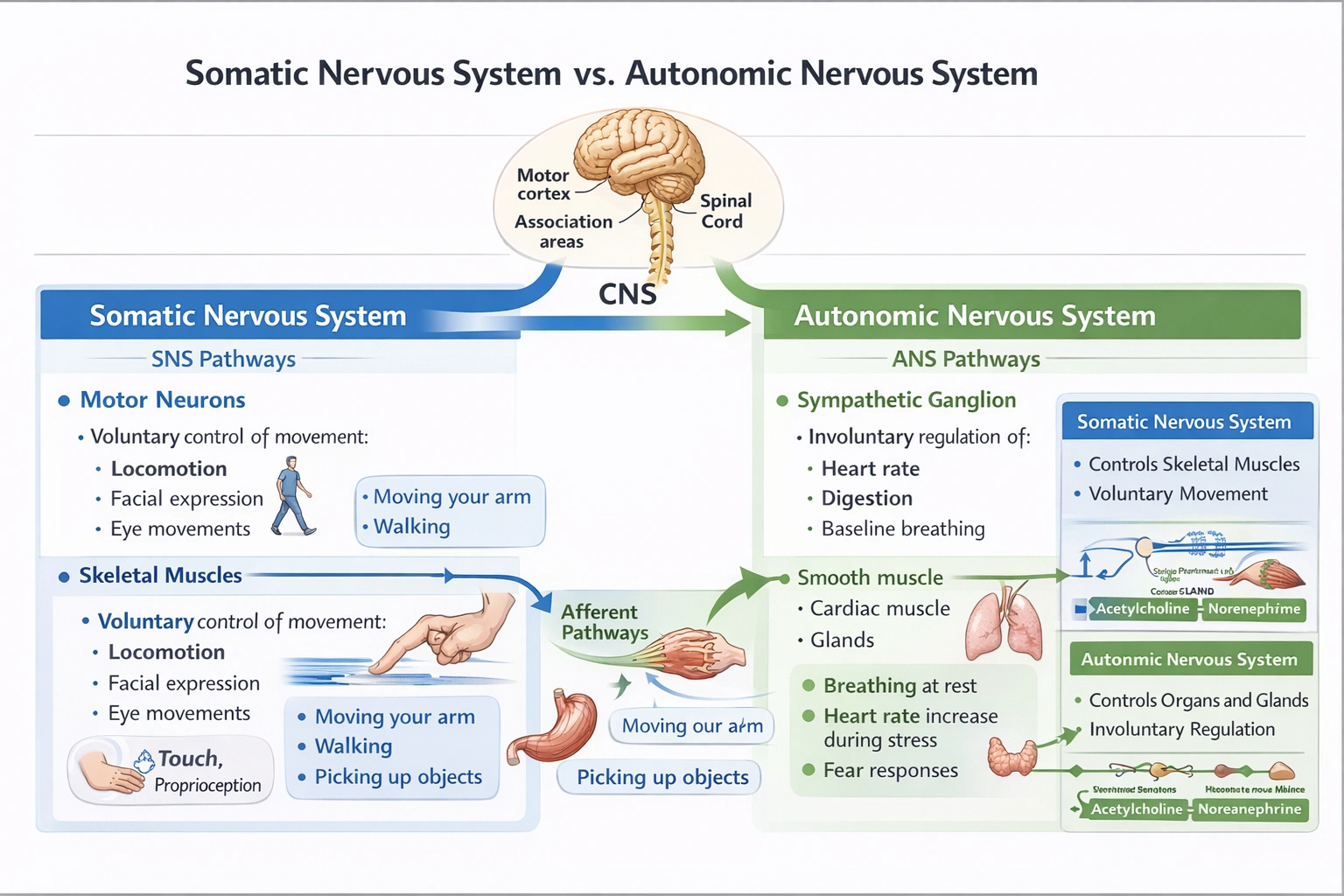
The somatic nervous system is responsible for which of the following?
A.
Breathing
B. Thought
C. Movement
D. Fear
Rationale
The somatic nervous system controls voluntary skeletal muscle contraction enabling conscious movement, posture maintenance, and reflexive responses—distinguished from autonomic regulation of visceral functions and central processing of cognition/emotion.
Somatic efferent pathways originate in motor cortex and brainstem nuclei, projecting via spinal nerves to skeletal muscles with single-neuron connections (no ganglia) using acetylcholine as neurotransmitter at neuromuscular junctions.
A) Breathing
Breathing involves both autonomic control (medullary respiratory centers maintaining baseline rhythm involuntarily) and limited somatic influence (voluntary breath holding or deep inhalation via diaphragm/intercostal muscle control). However, primary respiratory regulation is autonomic—breathing continues during sleep/unconsciousness without somatic input. The somatic system contributes only to voluntary modulation, not fundamental respiratory control.
B) Thought
Thought represents cognitive processing within the central nervous system (cerebral cortex, association areas)—not a function of peripheral nervous system divisions. The somatic nervous system comprises peripheral nerves connecting CNS to skeletal muscles/sensory receptors; it doesn't generate thoughts but may execute motor outputs resulting from cognitive decisions.
C) Movement
Voluntary movement execution defines the somatic nervous system's primary efferent function: motor neurons in ventral horn of spinal cord and cranial nerve motor nuclei project axons directly to skeletal muscle fibers, triggering contraction upon acetylcholine release at neuromuscular junctions. This enables conscious control of locomotion, manipulation, facial expression, and eye movements—distinguishing somatic from autonomic control of smooth/cardiac muscle. Somatic afferent pathways also convey conscious sensation (touch, proprioception) essential for movement coordination.
D) Fear
Fear involves limbic system processing (amygdala, hypothalamus) triggering autonomic responses (increased heart rate, sweating via sympathetic activation) and hormonal cascades (adrenaline release). While fear may produce somatic manifestations (freezing, fleeing movements), the emotional experience and physiological arousal stem from autonomic and central mechanisms—not somatic nervous system function per se.
Conclusion:
The somatic nervous system specializes in voluntary control of skeletal musculature and conscious perception of external stimuli—enabling purposeful interaction with the environment through movement and sensation. Option C correctly identifies movement as its defining responsibility, distinguishing it from autonomic regulation of visceral functions (breathing baseline, fear responses) and central cognitive processes (thought). This division proves clinically significant: somatic nerve damage causes paralysis/numbness in specific dermatomes/myotomes, while autonomic dysfunction produces blood pressure instability, digestive impairment, or temperature dysregulation—requiring different diagnostic and therapeutic approaches.
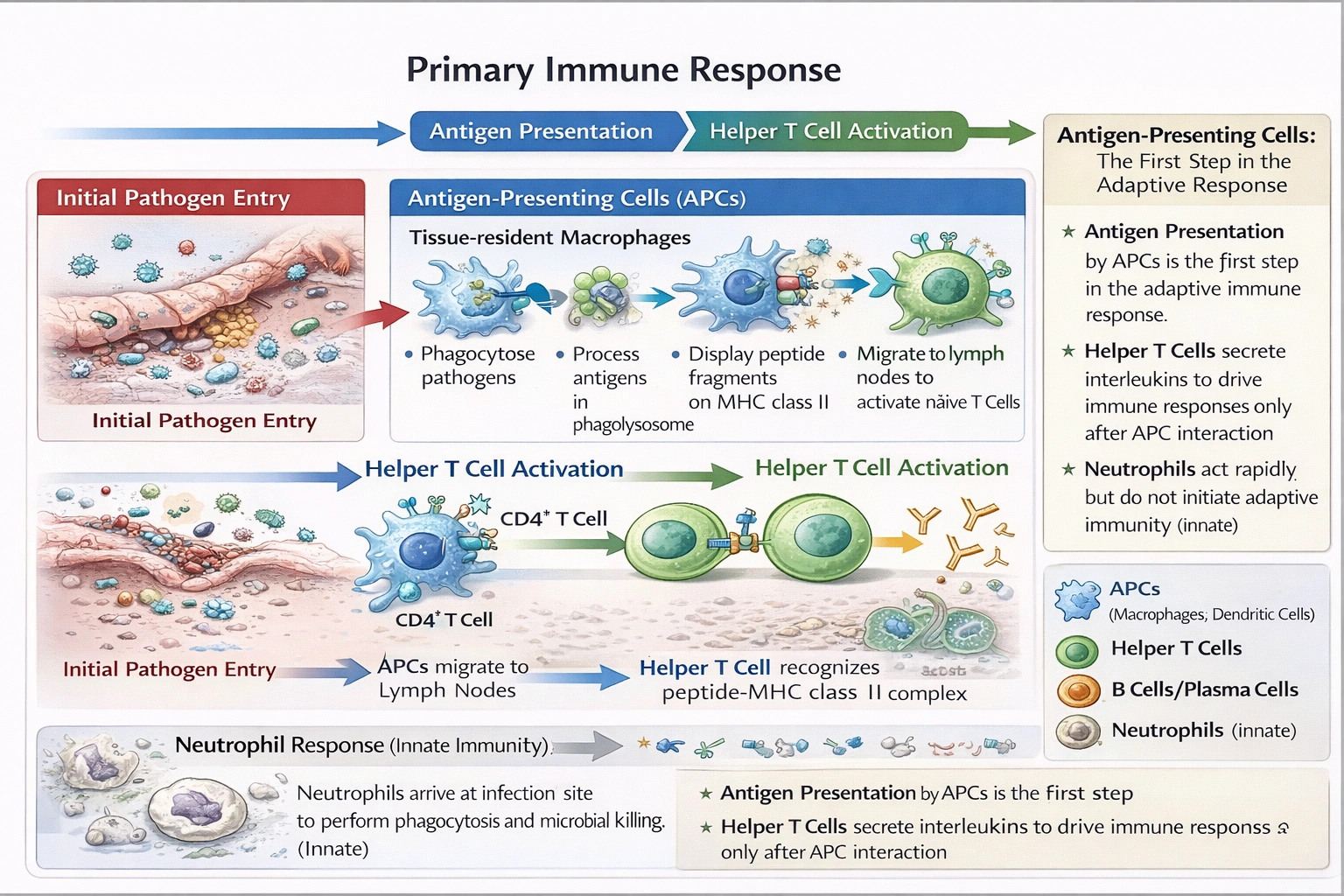
Which is the first event to happen in a primary immune response?
A.
Macrophages phagocytose pathogens and present their antigens.
B. Neutrophils aggregate and act as cytotoxic, nonspecific killers of pathogens.
C. B lymphocytes make pathogen-specific antibodies.
D. Helper T cells secrete interleukins to activate pathogen-fighting cells.
Rationale
Macrophages and dendritic cells perform initial pathogen phagocytosis and antigen presentation to T lymphocytes—constituting the essential first step that bridges innate and adaptive immunity by processing foreign material for specific immune recognition.
Antigen-presenting cells (APCs) internalize pathogens through phagocytosis, degrade them in phagolysosomes, and display peptide fragments bound to MHC class II molecules on their surface—enabling naïve T cell activation that orchestrates subsequent adaptive responses.
A) Macrophages phagocytose pathogens and present their antigens
Upon pathogen entry, tissue-resident macrophages and dendritic cells immediately recognize pathogen-associated molecular patterns (PAMPs) via pattern recognition receptors (TLRs, mannose receptors). They phagocytose invaders within minutes to hours, process antigens through proteolytic degradation, and migrate to lymph nodes displaying peptide-MHC II complexes. This antigen presentation to CD4⺠T cells represents the mandatory gateway to adaptive immunity—without it, B cells and cytotoxic T cells cannot mount pathogen-specific responses. Dendritic cells are particularly efficient APCs, but macrophages also contribute significantly to initial antigen capture and presentation.
B) Neutrophils aggregate and act as cytotoxic, nonspecific killers of pathogens
Neutrophils respond rapidly (within hours) as first responders to infection sites via chemotaxis, executing phagocytosis and releasing antimicrobial granules—but they don't present antigens to initiate adaptive immunity. Neutrophils function purely within innate immunity, lacking MHC II expression required for T cell activation. Their aggregation occurs concurrently with or shortly after macrophage phagocytosis but doesn't trigger the antigen-specific cascade defining primary adaptive responses.
C) B lymphocytes make pathogen-specific antibodies
Antibody production by plasma cells (differentiated B cells) occurs days after initial exposure—representing a late adaptive response requiring prior T cell help (for protein antigens) or extensive cross-linking (for polysaccharide antigens). B cells cannot produce antibodies without first encountering antigen directly (via BCR) AND receiving cytokine signals from activated helper T cells—making this a downstream event dependent on prior antigen presentation and T cell activation.
D) Helper T cells secrete interleukins to activate pathogen-fighting cells
Helper T cell activation requires two signals: (1) TCR binding to peptide-MHC II on APCs, and (2) costimulatory signals (B7-CD28 interaction). Only after receiving these signals do helper T cells proliferate and secrete interleukins (IL-2, IL-4, IFN-γ) to activate B cells, cytotoxic T cells, and macrophages. This represents the second major step in adaptive immunity—dependent on prior antigen presentation by macrophages/dendritic cells.
Conclusion:
The primary immune response sequence follows strict dependency: antigen capture/presentation (APCs) → T cell activation → B cell/T cell proliferation/differentiation → antibody production/cytotoxic activity. Macrophage/dendritic cell phagocytosis and antigen presentation constitutes the indispensable first event enabling all subsequent adaptive responses—without it, the immune system cannot recognize specific pathogens for targeted elimination. Option A correctly identifies this gateway step, while other options describe dependent downstream events (D, C) or parallel innate responses (B) that don't initiate adaptive immunity. Understanding this sequence proves essential for vaccine design (requiring effective antigen presentation) and immunodeficiency diagnosis (APC defects cause severe combined immunodeficiency).
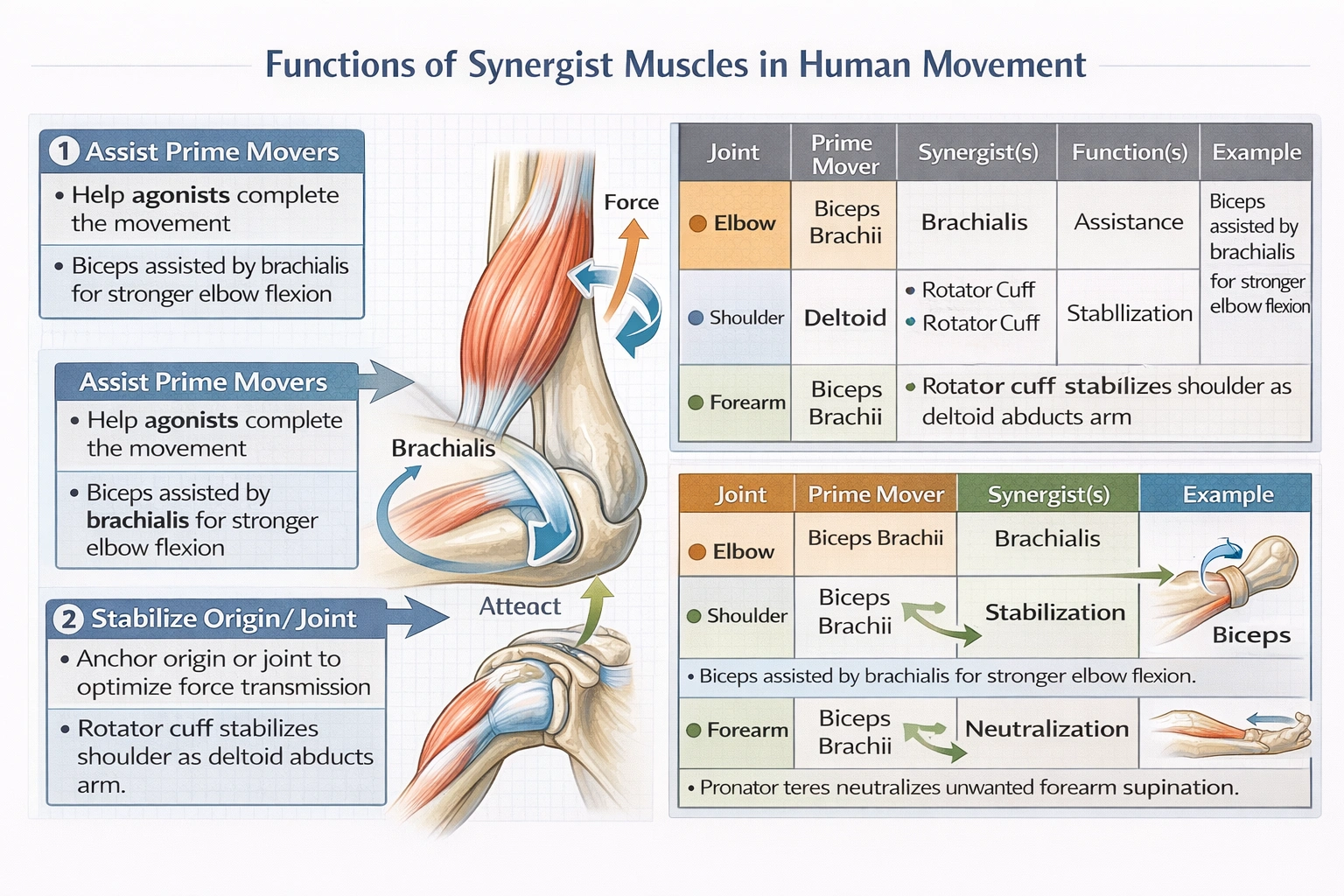
The function of synergists can best be described as which of the following?
A.
I. They assist primary movers in completing the specific movement; II. They stabilize the point of origin and provide extra pull near the insertion; III. They help prevent unwanted movement at a joint
B. I. They assist primary movers in completing the specific movement; II. They stabilize the point of origin and provide extra pull near the insertion; III. They help prevent unwanted movement at a joint
C. I. They assist primary movers in completing the specific movement; II. They stabilize the point of origin and provide extra pull near the insertion; III. They help prevent unwanted movement at a joint
D. I. They assist primary movers in completing the specific movement; II. They stabilize the point of origin and provide extra pull near the insertion; III. They help prevent unwanted movement at a joint
Rationale
Synergist muscles perform all three functions: assisting prime movers in executing desired movements, stabilizing origins to enhance force transmission, and preventing extraneous joint motions that would reduce movement efficiency—collectively optimizing biomechanical precision and power.
Synergists represent a functional muscle classification (alongside agonists/prime movers, antagonists, and fixators) defined by their supportive roles rather than primary force generation—enabling complex coordinated movements impossible with prime movers acting alone.
I. They assist primary movers in completing the specific movement
Synergists supplement prime mover force when additional power is required or when the prime mover's line of pull doesn't perfectly align with the desired movement axis. For example, during elbow flexion:
• Prime mover: Brachialis (optimal flexor regardless of forearm position)
• Synergist: Biceps brachii (assists flexion especially when forearm supinated)
• Synergist: Brachioradialis (assists flexion especially when forearm mid-pronated)
Without synergists, movements would be weaker and limited to narrow joint angles where prime movers operate most efficiently. Synergists extend the effective range and power of movements through complementary force vectors.
II. They stabilize the point of origin and provide extra pull near the insertion
Synergists often function as "fixators" stabilizing proximal joints to provide stable origins for distal prime movers—a critical function for force transmission efficiency. During shoulder abduction:
• Prime mover: Deltoid (abducts humerus)
• Synergist/fixator: Rotator cuff muscles (supraspinatus, infraspinatus, teres minor, subscapularis) stabilize humeral head in glenoid fossa
Without rotator cuff stabilization, deltoid contraction would superiorly translate the humeral head rather than producing pure abduction—demonstrating how synergists stabilize origins to convert muscle pull into desired movement at insertions. Similarly, wrist flexors stabilize the hand during finger flexion to prevent wrist collapse.
III. They help prevent unwanted movement at a joint
Synergists neutralize secondary actions of prime movers that would produce undesired joint motions. The biceps brachii exemplifies this dual role:
• Desired action: Elbow flexion (prime mover function with brachialis)
• Undesired secondary action: Forearm supination (would rotate hand during pure flexion tasks)
During tasks requiring pure elbow flexion without rotation (e.g., lifting a suitcase with palm facing body), pronator teres acts as a synergist to counteract biceps' supination tendency—preventing unwanted rotational movement while permitting desired flexion. This "neutralizing" function enables movement precision essential for skilled motor tasks.
Conclusion:
Synergists serve multifaceted supportive roles essential for efficient, precise movement: augmenting prime mover force (I), stabilizing origins to optimize force transmission (II), and neutralizing unwanted secondary movements (III). These functions often overlap within single muscles—rotator cuff muscles simultaneously stabilize the shoulder (II) while assisting deltoid abduction (I) and preventing humeral head translation (III). Option D correctly identifies all three synergist functions as integral to their biomechanical role—distinguishing synergists from pure prime movers (only I) or pure fixators (only II). Understanding synergist functions proves clinically significant: synergist weakness causes movement compensations (e.g., shoulder hiking during arm elevation with weak rotator cuff), while synergist overactivity contributes to movement disorders like spasticity patterns after stroke. Rehabilitation must address synergist function restoration for normal movement quality.
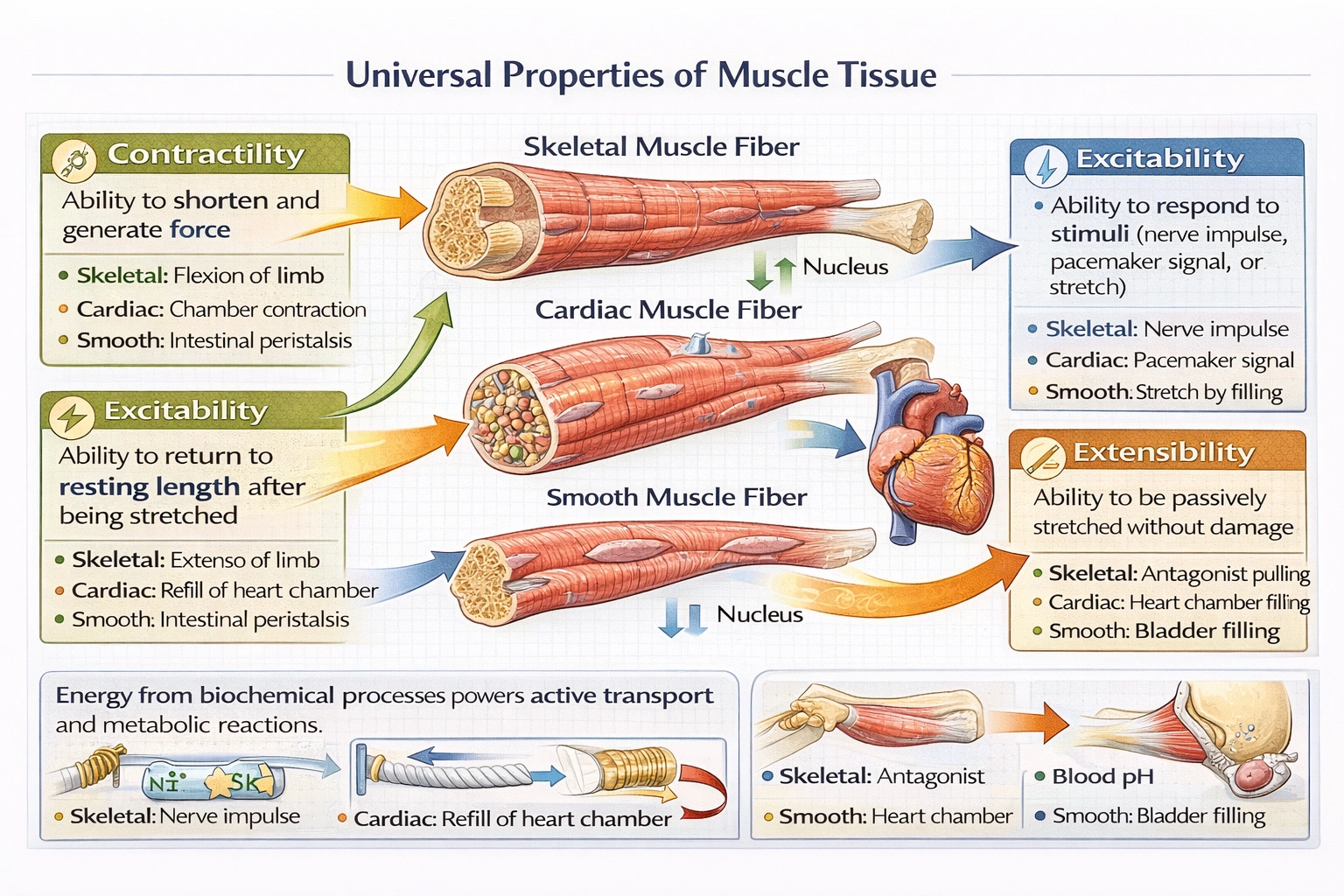
Which of the following correctly lists the four properties that all types of muscle tissue share?
A.
Contractile, excitable, elastic, extensible
B. Contractile, voluntary, elastic, extensible
C. Contractile, excitable, voluntary, extensible
D. Contractile, excitable, elastic, voluntary
Rationale
The four properties shared by all types of muscles are: Contractile, excitable, elastic, extensible.
These four properties constitute the universal functional characteristics enabling muscle tissue to generate force, respond to neural/hormonal signals, and accommodate length changes during movement cycles—distinguishing muscle from other tissue types while accommodating structural variations among muscle subtypes.
A) Contractile, excitable, elastic, extensible
• Contractility: All muscle types generate active tension through actin-myosin cross-bridge cycling powered by ATP hydrolysis—skeletal muscles pull bones, cardiac muscle ejects blood, smooth muscle propels contents through hollow organs.
• Excitability (irritability): All respond to electrochemical stimuli—skeletal via somatic motor neurons, cardiac via pacemaker cells and autonomic nerves, smooth via autonomic nerves, hormones, or stretch.
• Elasticity: All contain elastic components (titin in striated muscle, elastin/connective tissue in smooth muscle) enabling recoil after contraction or stretching—essential for cyclic function (heart refilling, intestinal peristalsis).
• Extensibility: All can be passively lengthened beyond resting length by antagonistic muscles (skeletal), chamber filling (cardiac), or luminal distension (smooth)—without structural damage within physiological ranges.
These properties operate universally: even involuntary cardiac and smooth muscles exhibit all four—voluntary control isn't required for these fundamental mechanical/physiological capabilities.
B) Contractile, voluntary, elastic, extensible
"Voluntary" control applies only to skeletal muscle—cardiac and smooth muscles operate involuntarily under autonomic regulation. Including "voluntary" excludes two of three muscle types from the shared property set, violating the question's requirement for properties common to all muscle tissues. Voluntary control represents a functional specialization, not a universal muscle property.
C) Contractile, excitable, voluntary, extensible
This option again incorrectly includes "voluntary" while omitting "elasticity"—a critical universal property. Without elasticity, muscles couldn't return to resting length after contraction, preventing cyclic function essential for all muscle types (e.g., heart couldn't refill between beats without elastic recoil). Elasticity is indispensable and universal; voluntary control is neither.
D) Contractile, excitable, elastic, voluntary
This option includes the non-universal "voluntary" property while omitting "extensibility"—equally critical for function. Without extensibility, muscles couldn't be lengthened by antagonistic forces or filling pressures—skeletal joints couldn't extend fully, the heart couldn't fill with blood, and hollow organs couldn't accommodate contents. Extensibility enables the length changes fundamental to muscle's mechanical role; voluntary control remains subtype-specific.
Conclusion:
The four universal muscle properties—contractility, excitability, elasticity, and extensibility—enable force generation, stimulus response, length recovery, and passive stretching respectively—forming the functional foundation shared across skeletal, cardiac, and smooth muscle despite their structural and control differences. Option A correctly identifies this complete universal set, while options B, C, and D erroneously substitute the non-universal "voluntary" property for one of the essential mechanical properties (elasticity or extensibility). Understanding these shared properties proves essential for comprehending muscle physiology across organ systems—recognizing that cardiac muscle's automaticity or smooth muscle's slow contractions represent variations on a universal functional theme rather than fundamentally different tissue capabilities. This knowledge informs clinical reasoning: muscle weakness could stem from impaired contractility (myopathy), excitability (channelopathy), elasticity (fibrosis), or extensibility (contracture)—requiring different diagnostic approaches despite shared tissue origin.
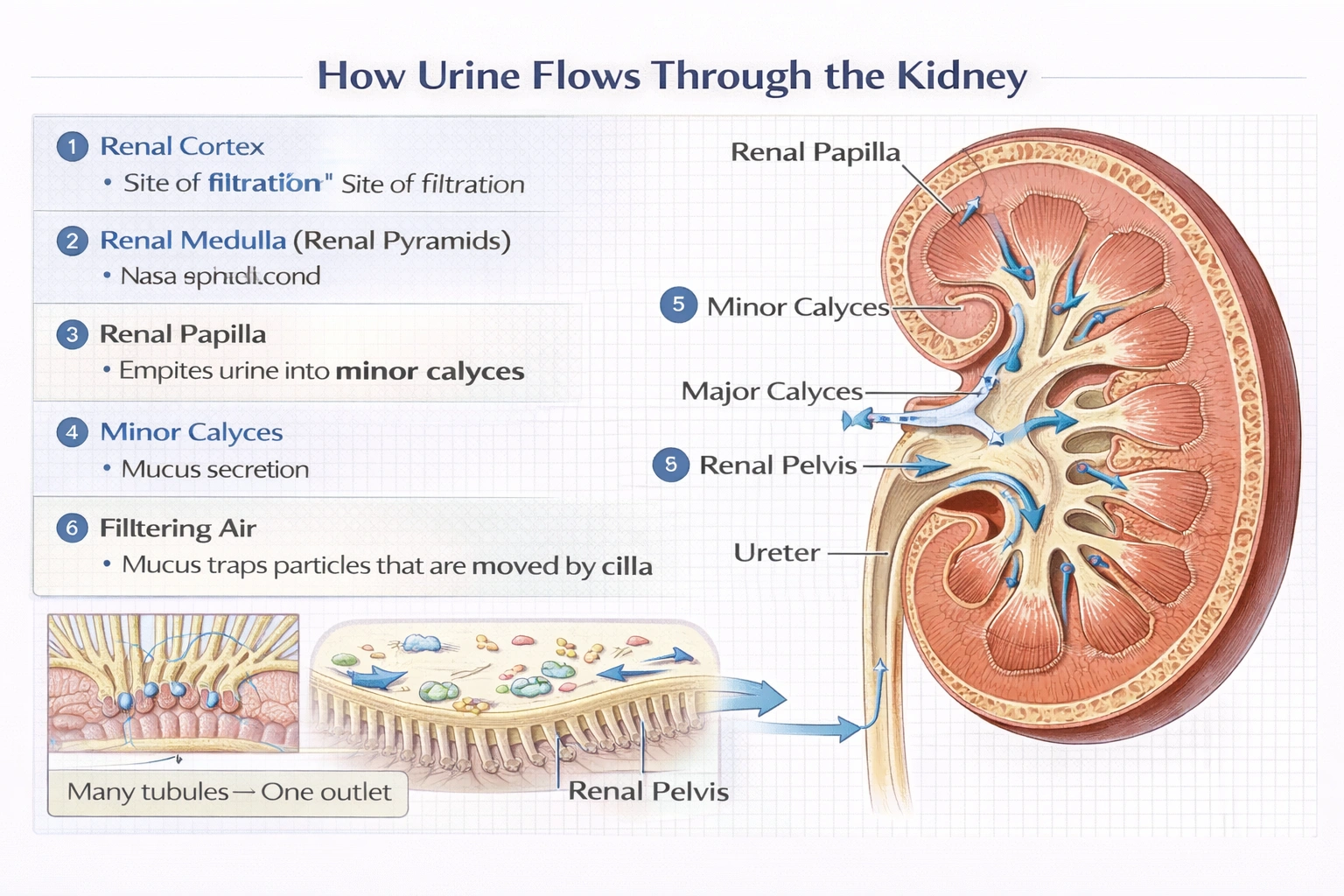
Which of the following structures acts like a funnel by delivering the urine from the millions of the collecting tubules to the ureters?
A.
The renal pelvis
B. The renal cortex
C. The renal medulla
D. Bowman's capsule
Rationale
The renal pelvis functions as a funnel-shaped conduit that collects urine from the calyces (which receive output from collecting ducts) and channels it into the ureter for transport to the urinary bladder serving as the kidney's central urine collection and exit structure.
The renal pelvis represents the expanded proximal end of the ureter within the renal sinus, branching into major and minor calyces that cup the renal papillae where collecting ducts empty creating an efficient drainage system converging millions of nephron outputs into a single transport vessel.
A) The renal pelvis
Urine flow pathway:
1. Collecting ducts from nephrons converge at renal papillae (tips of medullary pyramids)
2. Minor calyces (8–12 per kidney) cup individual papillae, receiving urine directly from duct orifices
3. Minor calyces merge into 2–3 major calyces
4. Major calyces converge into the single renal pelvis
5. Renal pelvis narrows to form the ureter at the ureteropelvic junction
This funnel architecture efficiently aggregates urine from approximately 1.2 million nephrons per kidney into one ureter—preventing backflow through peristaltic contractions of pelvic smooth muscle and maintaining unidirectional flow despite pressure fluctuations during bladder filling/emptying.
B) The renal cortex
The cortex contains glomeruli, proximal/distal convoluted tubules, and cortical nephron segments—but no urine collection structures. It's the outer granular layer where filtration and early reabsorption occur, not a conduit for urine transport. Cortical tissue surrounds but doesn't channel urine toward ureters; urine must first pass through medullary collecting ducts before reaching drainage structures.
C) The renal medulla
The medulla contains loops of Henle, vasa recta, and collecting ducts arranged in pyramids—but the medulla itself doesn't funnel urine. Collecting ducts traverse the medulla and empty at papillae into calyces, but the medullary tissue provides the structural framework rather than functioning as the drainage conduit. The medulla's role is concentration via countercurrent multiplication—not collection and transport.
D) Bowman's capsule
Bowman's capsule initiates urine formation by receiving glomerular filtrate at the nephron's beginning—not collecting finished urine at the end. It's a cup-shaped structure surrounding the glomerulus where blood plasma filtration occurs, producing primitive urine that then undergoes modification through tubular segments. Bowman's capsule represents the starting point of nephron processing, not the terminal collection point before ureteral transport.
Conclusion:
The renal pelvis uniquely serves as the kidney's central urine collection funnel—integrating outputs from millions of nephrons through the calyceal system into a single ureteral channel. Options B, C, and D describe nephron components or kidney regions involved in urine formation and modification, not final collection and transport. Option A correctly identifies the renal pelvis as the anatomical structure fulfilling the funnel function described—essential knowledge for understanding urinary obstruction pathologies (e.g., pelviureteric junction obstruction causing hydronephrosis) and interpreting radiological imaging of the collecting system. The pelvis's funnel design optimizes drainage efficiency while minimizing stasis that could promote infection or stone formation.
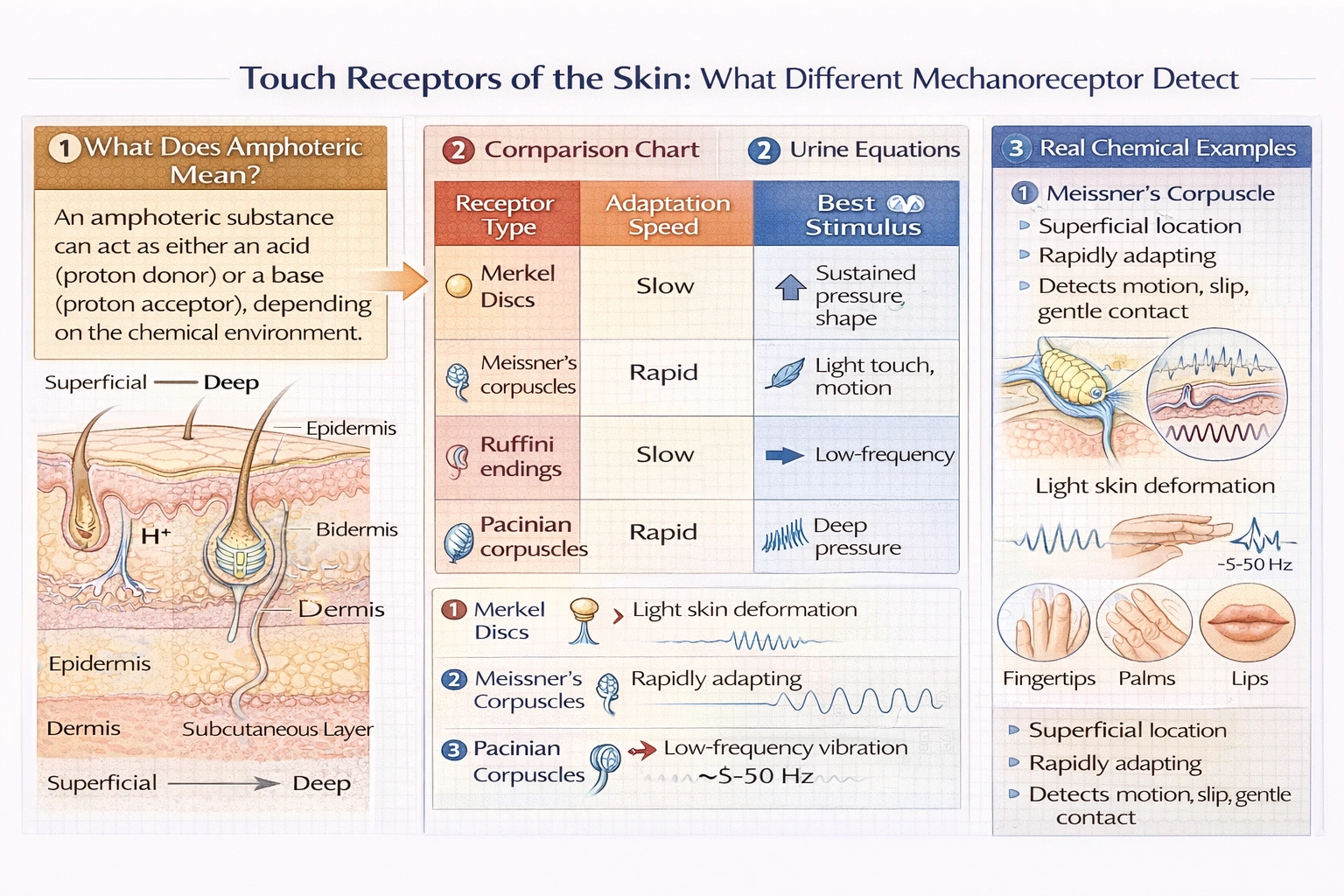
Which of the following touch receptors respond to light touch and slower vibrations?
A.
Merkel's discs
B. Pacinian corpuscles
C. Meissner's corpuscles
D. Ruffini endings
Rationale
Meissner's corpuscles (tactile corpuscles) detect light touch and low-frequency vibrations (5–50 Hz) through rapid adaptation—concentrated in glabrous skin of fingertips, lips, and palms where fine tactile discrimination occurs.
These encapsulated nerve endings reside in dermal papillae just beneath the epidermis, with layered connective tissue surrounding sensory nerve terminals that deform under light pressure—generating action potentials that signal object contact, texture, and slow vibration to the central nervous system.
A) Merkel's discs
Merkel discs (Merkel cell-neurite complexes) detect sustained pressure, texture, and object shape through slow adaptation—providing continuous signaling during prolonged contact essential for form recognition and static touch discrimination. Located in epidermal basal layer of fingertips and lips, they respond to edges, points, and curvature but not vibration. Their sustained firing enables Braille reading and object identification through stationary contact—distinct from vibration detection.
B) Pacinian corpuscles
Pacinian corpuscles detect high-frequency vibrations (50–700 Hz) and deep pressure through rapid adaptation—responding only to stimulus onset/offset rather than sustained pressure. Located deep in dermis/subcutaneous tissue, their onion-like lamellar structure filters out constant pressure while amplifying vibration—ideal for sensing tool handle vibrations or distant impacts through surfaces. They don't respond to light touch (require significant force) or slow vibrations (filtered out by lamellae).
C) Meissner's corpuscles
Meissner's corpuscles specialize in light dynamic touch and slow vibrations:
• Location: Dermal papillae of glabrous skin (fingertips, palms, soles, lips, tongue)
• Structure: Elongated encapsulated endings with Schwann cell layers surrounding nerve terminals
• Function: Rapidly adapting receptors firing primarily at stimulus onset/offset
• Sensitivity: Threshold ~0.05–0.1 g force; optimal vibration frequency 5–50 Hz
• Role: Detecting slip (object movement across skin), light stroking, fabric texture, and low-frequency vibration essential for fine motor control and object manipulation
Their superficial location and rapid adaptation make them ideal for detecting subtle skin deformation during delicate manipulative tasks—distinguishing them from deeper vibration detectors (Pacinian) or sustained pressure receptors (Merkel).
D) Ruffini endings
Ruffini endings detect skin stretch, sustained pressure, and joint angle changes through slow adaptation—signaling continuous deformation during hand shaping around objects or joint movement. Located deep in dermis and joint capsules, they respond to lateral skin stretch rather than perpendicular pressure or vibration. Their sustained firing contributes to proprioception and grip force adjustment but not light touch or vibration detection.
Conclusion:
Meissner's corpuscles uniquely specialize in light touch and slow vibration detection among cutaneous mechanoreceptors—combining superficial location, rapid adaptation, and frequency sensitivity optimized for fine tactile discrimination during object manipulation. Option C correctly identifies this receptor type, distinguishing it from sustained pressure detectors (A, D) and high-frequency vibration sensors (B). Understanding receptor specificity proves essential for clinical neurology: Meissner's corpuscle loss (e.g., leprosy) impairs fine touch and slip detection causing object dropping, while Pacinian loss affects vibration sense used in neurological exams. This functional specialization enables the somatosensory system to extract multiple stimulus dimensions simultaneously through parallel receptor channels—each optimized for distinct mechanical features critical for environmental interaction.
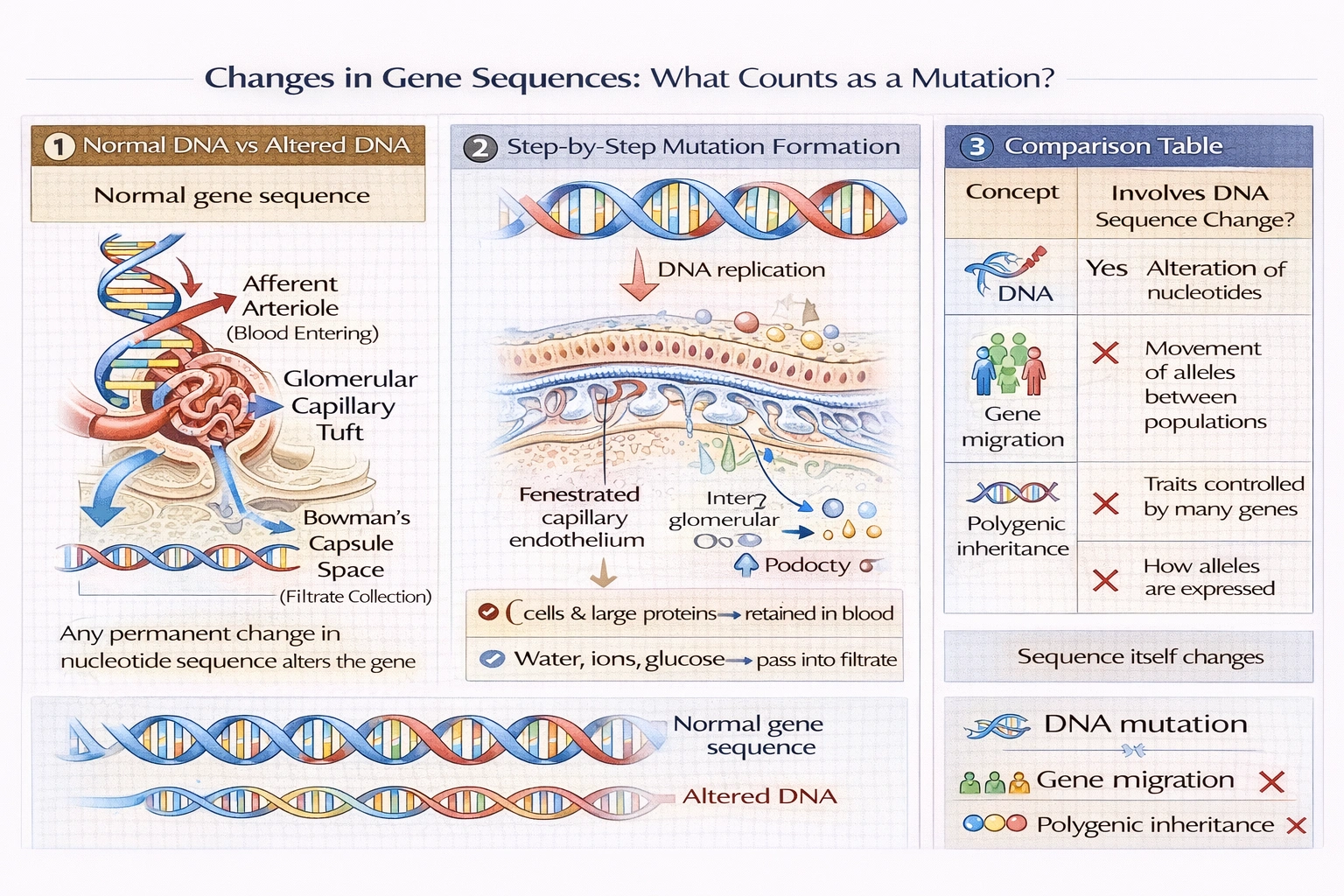
What is an alteration in the normal gene sequence called?
A.
DNA mutation
B. Gene migration
C. Polygenetic inheritance
D. Incomplete dominance
Rationale
A DNA mutation represents any permanent change in the nucleotide sequence, including substitutions, insertions, deletions, duplications, or rearrangements that may alter gene function, expression, or regulation.
Mutations arise from replication errors, environmental mutagens (radiation, chemicals), or spontaneous chemical changes (deamination, depurination) serving as the ultimate source of genetic variation essential for evolution while potentially causing disease when disrupting critical gene functions.
A) DNA mutation
DNA mutations encompass all sequence alterations:
• Point mutations: Single base changes (substitutions like sickle cell HbS: GAG→GTG)
• Frameshift mutations: Insertions/deletions altering reading frame (e.g., CFTR ΔF508 deletion)
• Chromosomal mutations: Large-scale changes (translocations like Philadelphia chromosome in CML)
Mutations may be:
• Germline: Inherited through gametes, affecting all offspring cells
• Somatic: Occurring in body cells after fertilization, affecting only descendant clones (e.g., cancer mutations)
The term "DNA mutation" precisely describes sequence alterations at the molecular level—distinguishing it from broader genetic phenomena like migration or inheritance patterns.
B) Gene migration
Gene migration (gene flow) describes movement of alleles between populations through organism migration and breeding—not sequence alteration within an individual's DNA. It changes population allele frequencies but doesn't modify the DNA sequence itself. Confusing population genetics processes with molecular genetic changes represents a categorical error migration redistributes existing variants; mutation creates new variants.
C) Polygenetic inheritance
Polygenic inheritance describes traits influenced by multiple genes (e.g., height, skin color) not sequence alterations. It explains continuous trait variation through additive effects of many loci, but doesn't involve changes to DNA sequences themselves. Polygenic traits can exist with completely normal gene sequences; the term describes inheritance patterns, not molecular alterations.
D) Incomplete dominance
Incomplete dominance describes heterozygous phenotypes intermediate between homozygous phenotypes (e.g., red × white snapdragons → pink offspring)—an expression pattern resulting from normal gene sequences with partial dominance relationships. It reflects how alleles interact during expression, not alterations to the DNA sequence itself. The underlying DNA sequences remain unchanged; only phenotypic expression differs from complete dominance patterns.
Conclusion:
DNA mutation specifically denotes alterations in nucleotide sequence—the molecular basis for genetic variation and many diseases. Option A correctly identifies this fundamental genetic concept, distinguishing it from population-level processes (B), inheritance patterns (C), or expression phenomena (D) that don't involve sequence changes. Understanding mutation as the source of new genetic variation proves essential for evolutionary biology (raw material for natural selection), medical genetics (disease causation), and biotechnology (directed mutagenesis for protein engineering). While migration, polygenic inheritance, and dominance patterns shape how genetic variation manifests and spreads, only mutation creates novel sequence variants—the ultimate origin of all genetic diversity.
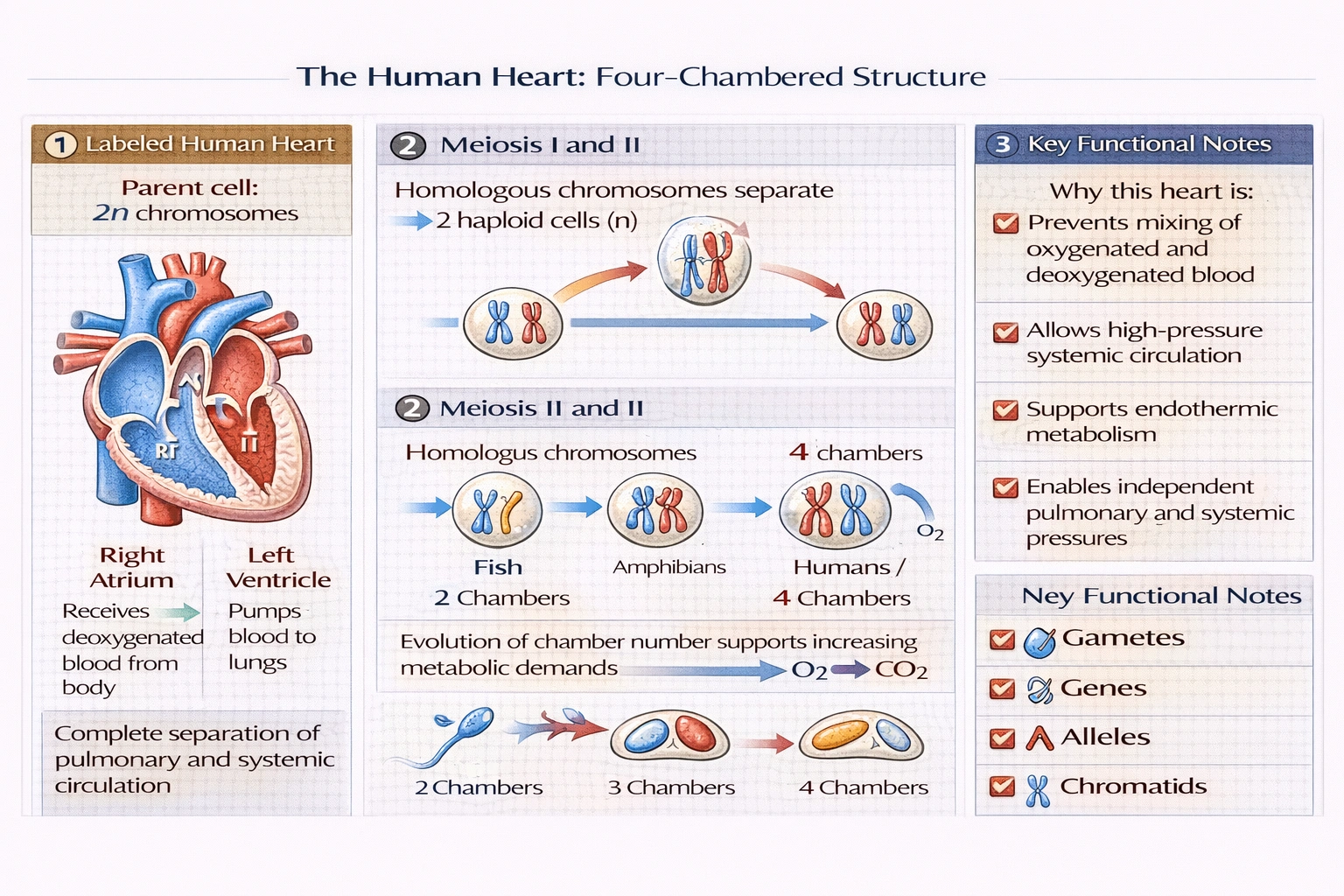
The heart is divided into __ chambers.
A.
2
B. 3
C. 4
D. 5
Rationale
The heart contains four chambers. The human heart consists of two upper atria and two lower ventricles separated by septa, creating a dual-pump system where the right side handles pulmonary circulation and the left side manages systemic circulation—enabling efficient separation of oxygenated and deoxygenated blood essential for endothermic metabolism.
A) 2
A two-chambered heart (one atrium, one ventricle) exists only in fish, where blood passes sequentially through heart → gills → body → heart in a single circuit. This arrangement cannot support the high-pressure systemic circulation required by mammals and birds, making it incompatible with human cardiovascular anatomy.
B) 3
Three-chambered hearts (two atria, one ventricle) characterize amphibians and most reptiles, allowing partial separation of oxygenated and deoxygenated blood. However, the single ventricle permits mixing of blood streams, reducing oxygen delivery efficiency—insufficient for human metabolic demands requiring complete separation achieved only with four chambers.
C) 4
The four-chambered heart comprises right atrium (receives deoxygenated blood from body), right ventricle (pumps to lungs), left atrium (receives oxygenated blood from lungs), and left ventricle (pumps to body). Complete interatrial and interventricular septa prevent blood mixing, enabling high-pressure systemic circulation (left ventricle) independent of low-pressure pulmonary circulation (right ventricle)—a prerequisite for mammalian endothermy and sustained activity levels.
D) 5
No vertebrate possesses a five-chambered heart. This option represents an anatomical impossibility—cardiac chamber number follows strict evolutionary patterns tied to circulatory demands, with four chambers representing the maximum complexity in terrestrial vertebrates. Additional chambers would disrupt coordinated contraction sequences essential for effective pumping.
Conclusion:
Four chambers represent the definitive mammalian cardiac architecture enabling complete separation of pulmonary and systemic circuits—critical for maintaining high metabolic rates and body temperature regulation. Options A and B describe ancestral cardiac designs insufficient for human physiology, while D is anatomically nonexistent. The four-chambered structure optimizes oxygen delivery efficiency by preventing blood mixing and allowing independent pressure regulation in each circuit—fundamental to human cardiovascular function and endurance capacity.
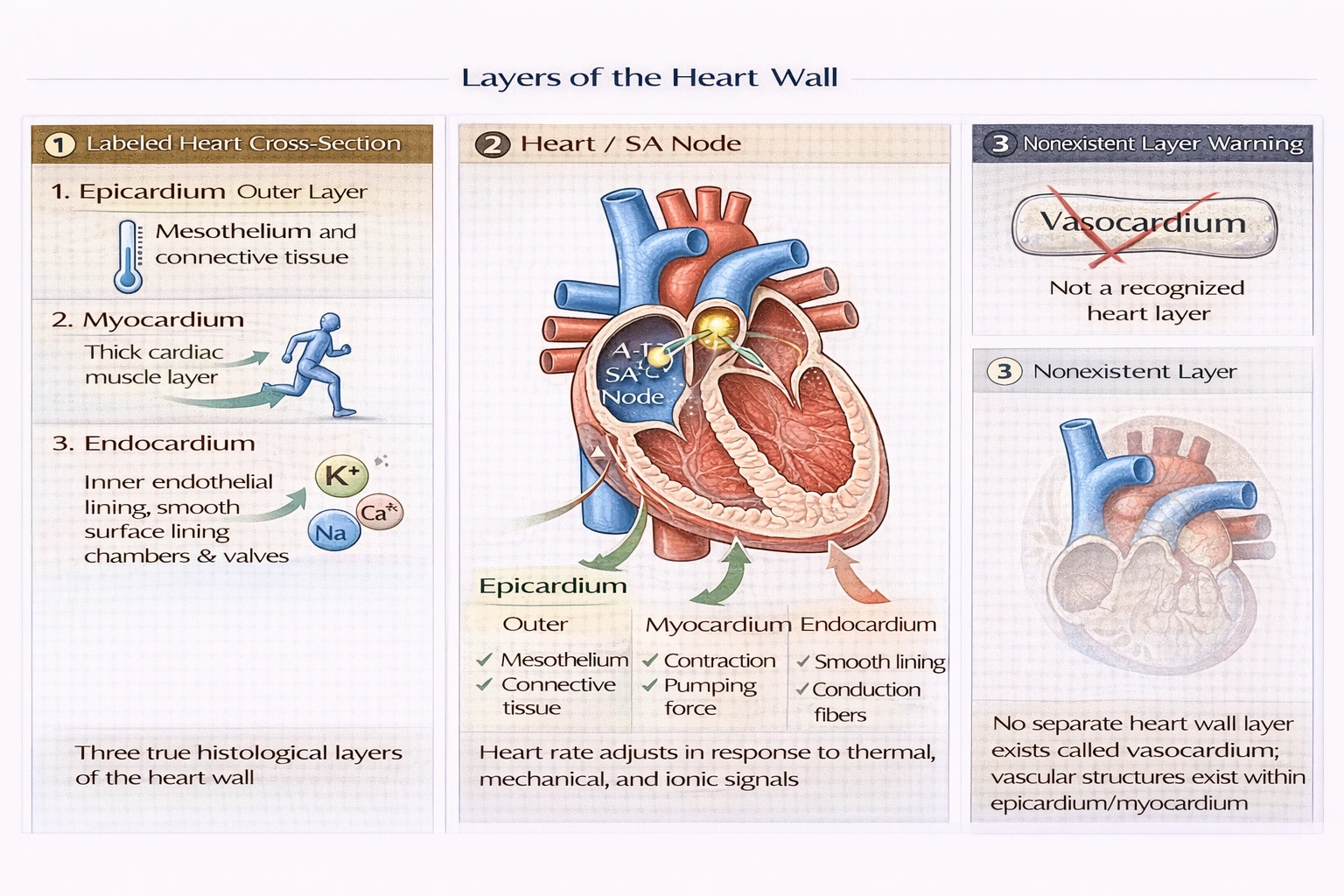
Which of the following is not considered a layer of the heart?
A.
epicardium
B. endocarcium
C. myocardium
D. vasocardium
Rationale
"Vasocardium" is not a recognized layer of the heart. The heart wall comprises three histologically distinct layers—epicardium (visceral pericardium), myocardium (cardiac muscle), and endocardium (endothelial lining)—each with specialized structural and functional roles in cardiac physiology.
A) epicardium
The epicardium forms the outermost heart layer, consisting of mesothelium (simple squamous epithelium) overlying adipose and connective tissue containing coronary vessels and nerves. It represents the visceral layer of the serous pericardium, providing mechanical protection, reducing friction during contraction, and housing the vascular supply essential for myocardial oxygenation—particularly critical given the heart's continuous metabolic demands.
B) endocarcium
This option contains a spelling error; the correct term is "endocardium"—the innermost layer lining chambers and valves with endothelium continuous with blood vessel endothelium. Though misspelled as "endocarcium," it refers to a genuine cardiac layer. The endocardium provides a smooth, non-thrombogenic surface minimizing turbulence and clot formation, contains Purkinje fibers of the conduction system, and participates in paracrine signaling regulating myocardial function—making it anatomically and functionally essential despite the typographical error.
C) myocardium
The myocardium constitutes the thick middle layer composed of cardiac muscle arranged in spiral bundles enabling efficient wringing contraction that ejects blood. Its thickness varies by chamber (left ventricle thickest due to systemic pressure demands) and contains specialized conduction tissue (AV node, Bundle of His). Myocardial integrity determines contractile force—damage from infarction directly reduces ejection fraction, demonstrating this layer's central role in pump function.
D) vasocardium
"Vasocardium" is not an anatomical term in cardiac histology or embryology. No recognized heart layer bears this name—vascular structures exist within the epicardium and myocardium (coronary arteries, capillaries) but don't constitute a separate wall layer. This fabricated term likely confuses "vasa vasorum" (vessels supplying large vessel walls) with cardiac anatomy or misrepresents the pericardium (fibrous sac surrounding the heart). Standard cardiac wall organization recognizes only three layers—any fourth purported layer lacks histological or functional basis.
Conclusion:
Cardiac wall organization follows a consistent three-layer pattern across vertebrate species—epicardium, myocardium, and endocardium—each with defined embryological origins and physiological functions. Option D introduces a non-existent term ("vasocardium") with no basis in anatomical literature, while option B's misspelling ("endocarcium" for endocardium) still references a genuine structure. Recognizing authentic cardiac layers proves essential for interpreting imaging studies, surgical approaches, and pathological processes—misidentifying layers could lead to procedural errors such as incorrect catheter placement or misdiagnosis of wall abnormalities.
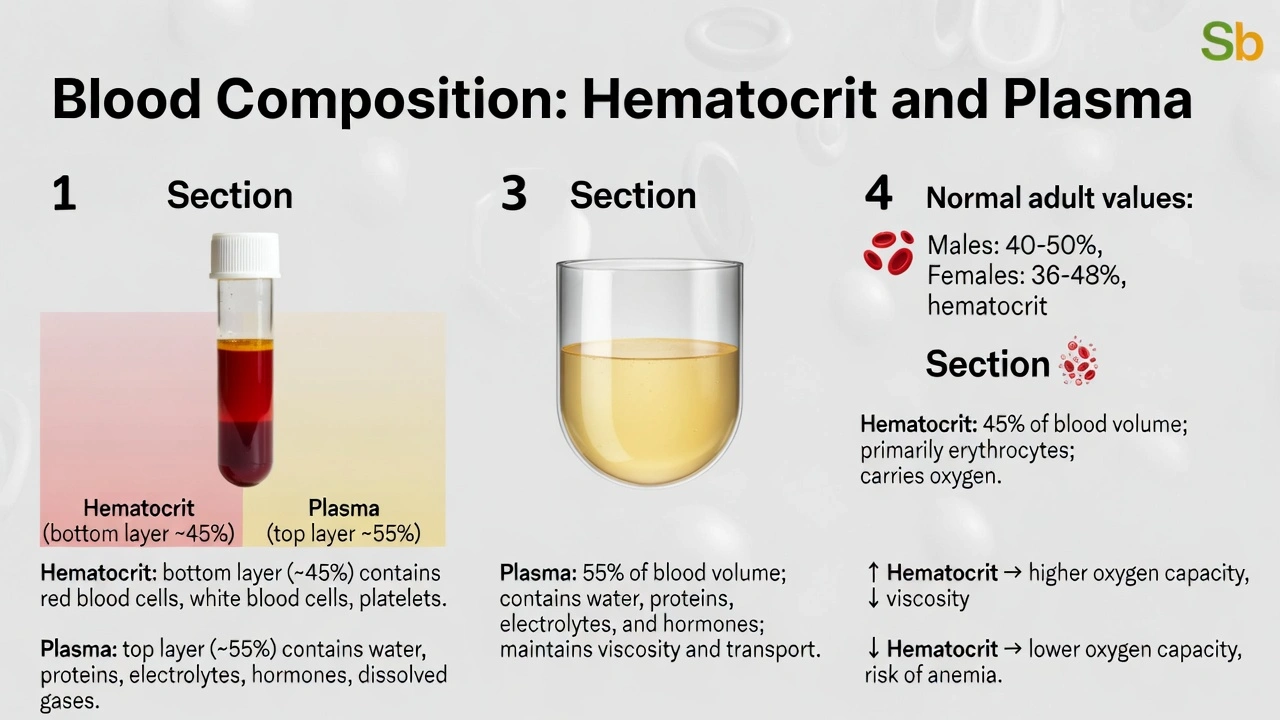
Blood is made of approximately __% hematocrit and __% plasma.
A.
45,55
B. 55,45
C. 50,25
D. 25,75
Rationale
Blood consists of approximately 45% hematocrit and 55% plasma. Hematocrit represents the volume percentage of formed elements (primarily erythrocytes, plus leukocytes and platelets) in centrifuged blood, while plasma constitutes the liquid matrix containing water, proteins, electrolytes, hormones, and dissolved gases—maintaining this ratio ensures optimal viscosity for circulation and oxygen-carrying capacity.
A) 45, 55
This ratio reflects normal adult values: males average 40–50% hematocrit (typically 45%), females 36–48% (typically 42%), with plasma comprising the remainder. This balance optimizes blood viscosity—higher hematocrit increases oxygen capacity but elevates viscosity impairing flow; lower hematocrit reduces viscosity but compromises oxygen delivery. The 45/55 ratio represents evolutionary optimization for mammalian circulatory efficiency, verified through clinical centrifugation measurements and hematology analyzers.
B) 55, 45
This inverted ratio would indicate polycythemia (excess red blood cells)—a pathological state increasing blood viscosity and thrombosis risk. Hematocrit exceeding 52% in males or 48% in females requires investigation for causes like polycythemia vera, chronic hypoxia, or doping. Such elevation impairs microcirculatory flow and increases cardiac workload—demonstrating why the normal ratio favors plasma majority for optimal rheological properties.
C) 50, 25
These values sum to only 75%, violating conservation of volume—blood components must total 100%. This mathematical impossibility indicates a distractor option without physiological basis. Even in extreme dehydration where hematocrit may reach 60%, plasma never drops below 40% without life-threatening hemoconcentration causing circulatory collapse.
D) 25, 75
This ratio indicates anemia (low red cell mass)—hematocrit below 36% in females or 40% in males. While plasma percentage increases relatively, absolute plasma volume often remains normal or decreases in chronic anemia; the elevated plasma percentage reflects reduced cellular elements rather than expanded plasma. Severe anemia (hematocrit <25%) causes tissue hypoxia despite adequate plasma volume—demonstrating why the normal 45/55 balance is physiologically essential.
Conclusion:
The 45% hematocrit/55% plasma ratio represents the homeostatically maintained balance optimizing oxygen transport capacity against circulatory resistance—critical for tissue perfusion across diverse metabolic demands. Option A provides the accurate normal values, while other options represent pathologies (B, D) or mathematical impossibilities (C). Clinically, hematocrit measurement guides transfusion decisions: values below 21% typically require transfusion in stable patients, while values above 60% may warrant phlebotomy in polycythemia—highlighting the narrow physiological range where this ratio supports optimal cardiovascular function.
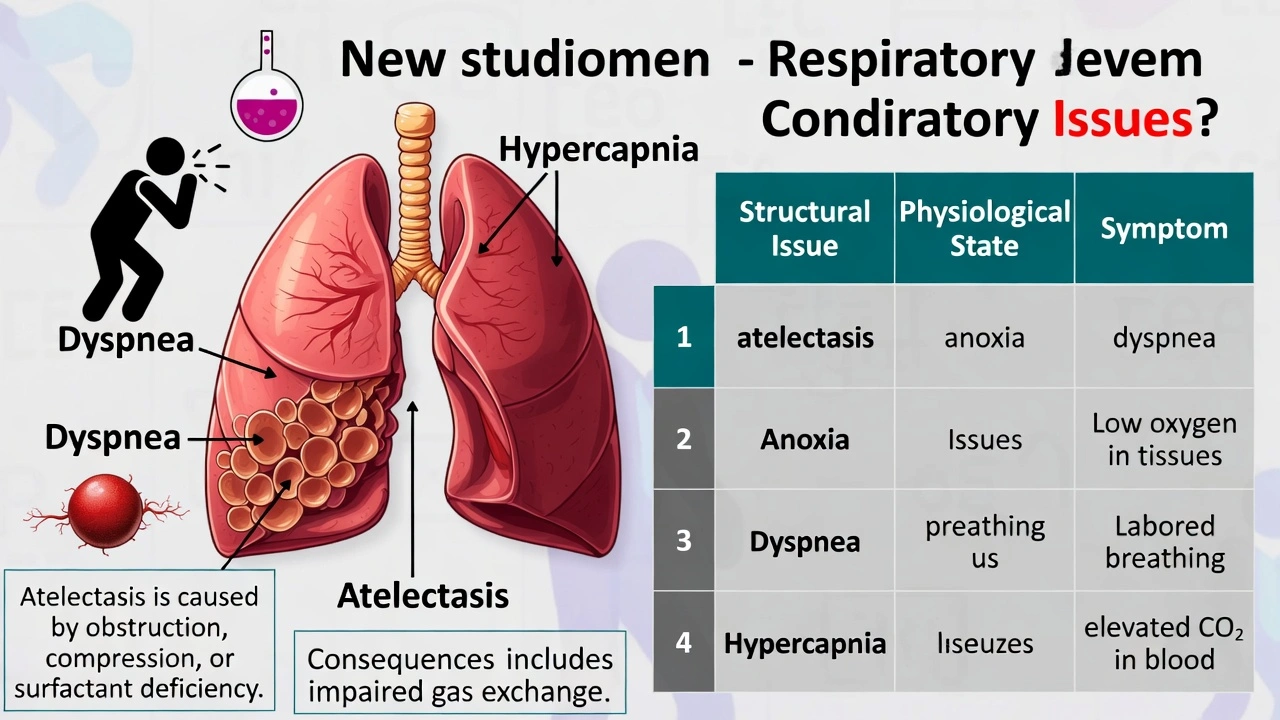
Which of the following terms matches the definition: collapse of a lung.
A.
anoxia
B. atelectasis
C. dyspnea
D. hypercapnia
Rationale
Atelectasis describes lung collapse. Atelectasis refers to partial or complete collapse of lung tissue with loss of volume due to deflation of alveoli—resulting from airway obstruction, external compression, or surfactant deficiency—and impairs gas exchange by reducing ventilated lung surface area.
A) anoxia
Anoxia denotes complete absence of oxygen supply to tissues—more severe than hypoxia (reduced oxygen). It represents a physiological state causing cellular damage, not a structural lung condition. While atelectasis can cause anoxia in affected lung regions, anoxia itself describes oxygen deprivation rather than physical collapse—confusing consequence with structural pathology.
B) atelectasis
Atelectasis originates from Greek ateles (incomplete) + ektasis (expansion). Types include:
• Obstructive: Mucus plug, foreign body, or tumor blocking airways preventing alveolar inflation
• Compressive: Pleural effusion or pneumothorax exerting external pressure collapsing lung tissue
• Microatelectasis: Surfactant deficiency (e.g., in premature infants with RDS) increasing alveolar surface tension causing collapse
Radiographically, atelectasis appears as increased opacity with volume loss signs (elevated diaphragm, shifted fissures). Treatment targets the underlying cause—bronchoscopy for obstruction, chest tube for pneumothorax—distinguishing it from other respiratory conditions requiring different interventions.
C) dyspnea
Dyspnea describes the subjective sensation of difficult or labored breathing—not a structural abnormality. It represents a symptom that may result from atelectasis, heart failure, asthma, or anxiety—but isn't synonymous with lung collapse. Patients with small atelectatic areas may experience no dyspnea, while severe dyspnea can occur with fully expanded lungs in pulmonary edema—demonstrating these are distinct clinical concepts.
D) hypercapnia
Hypercapnia refers to elevated arterial carbon dioxide levels (>45 mmHg)—a gas exchange abnormality that may result from atelectasis reducing ventilated alveolar surface area, but isn't the collapse itself. Hypercapnia also occurs in COPD, drug overdose, or neuromuscular disease without lung collapse—making it a potential consequence rather than the structural condition described in the question.
Conclusion:
Atelectasis specifically denotes physical collapse of lung tissue with loss of aeration—distinct from oxygenation states (anoxia), symptoms (dyspnea), or blood gas abnormalities (hypercapnia) that may accompany but don't define the condition. Option B provides the precise pathological term essential for accurate diagnosis and treatment: postoperative atelectasis requires incentive spirometry, while obstructive atelectasis needs bronchoscopic intervention—therapies targeting the collapse mechanism rather than secondary symptoms. Mislabeling this condition could delay appropriate intervention, potentially progressing to pneumonia or respiratory failure if untreated.
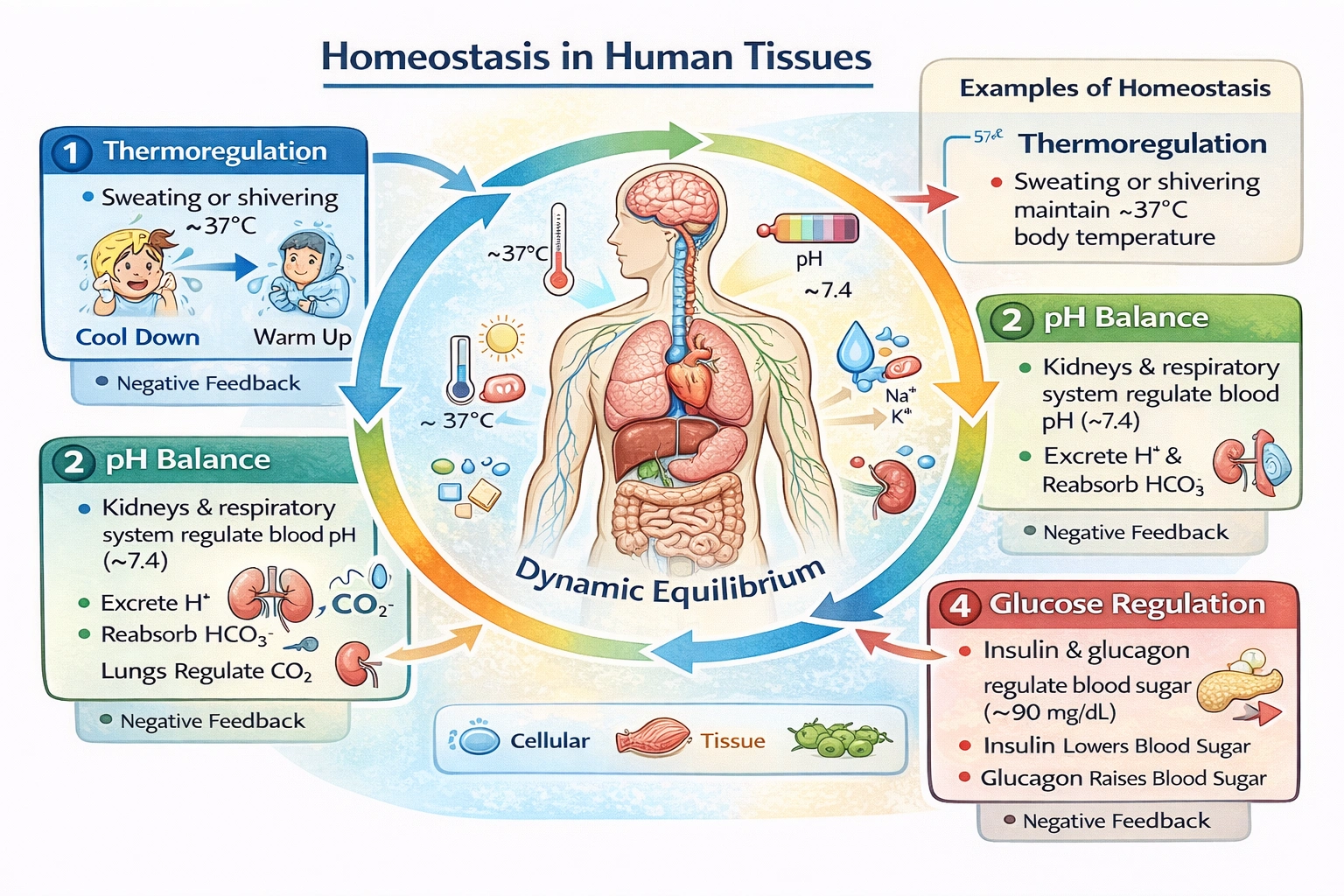
___ is a state of equilibrium within tissues.
A.
peristalsis
B. stomatitis
C. homeostasis
D. synergy
Rationale
Homeostasis maintains equilibrium within tissues. Homeostasis represents the dynamic physiological processes that maintain stable internal conditions—such as temperature, pH, fluid balance, and electrolyte concentrations—despite external environmental fluctuations, through negative feedback mechanisms operating at cellular, tissue, and systemic levels.
A) peristalsis
Peristalsis describes rhythmic smooth muscle contractions propelling contents through hollow organs (esophagus, intestines)—a specific motility mechanism unrelated to equilibrium maintenance. While peristalsis contributes to digestive homeostasis indirectly, it is not the overarching state of equilibrium itself.
B) stomatitis
Stomatitis refers to inflammation of the oral mucosa—typically caused by infection, irritation, or autoimmune conditions—representing a pathological disruption of equilibrium rather than equilibrium maintenance. Inflammation constitutes a homeostatic response to injury but isn't synonymous with homeostasis.
C) homeostasis
Homeostasis operates through multiple regulatory systems:
• Thermoregulation: Hypothalamus triggers sweating or shivering to maintain 37°C core temperature
• pH balance: Renal bicarbonate reabsorption and respiratory CO₂ elimination maintain blood pH at 7.35–7.45
• Fluid balance: ADH and aldosterone regulate water/sodium retention to preserve blood volume
• Glucose regulation: Insulin and glucagon maintain blood glucose within 70–100 mg/dL
These processes exemplify dynamic equilibrium—continuous adjustment rather than static constancy—enabling cellular function despite environmental challenges.
D) synergy
Synergy describes cooperative interaction where combined effects exceed individual contributions (e.g., muscle groups working together)—a functional principle rather than an equilibrium state. While synergistic actions may support homeostasis, synergy itself doesn't define the equilibrium condition.
Conclusion:
Homeostasis constitutes the fundamental biological principle of internal stability maintenance through regulated feedback systems—essential for cellular survival and organismal function. Option C correctly identifies this core physiological concept, distinguishing it from specific mechanisms (A), pathologies (B), or interaction principles (D). Understanding homeostasis proves critical for comprehending disease pathophysiology (e.g., diabetes as homeostatic failure of glucose regulation) and therapeutic interventions aimed at restoring equilibrium.
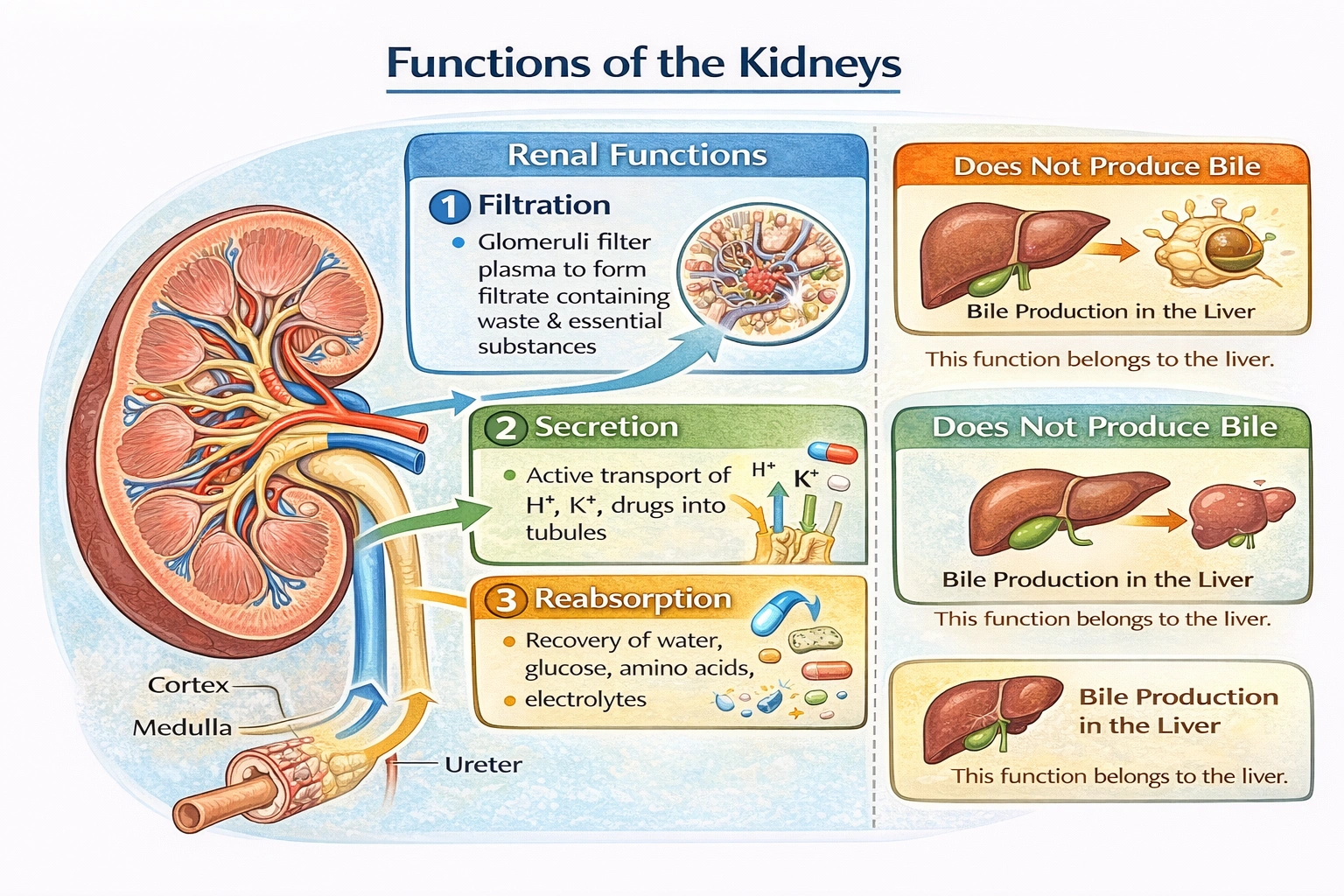
Which of the following functions are not related to the kidneys?
A.
filtration
B. bile production
C. secretion
D. re-absorption
Rationale
Bile production is not a kidney function. The kidneys perform filtration of blood plasma through glomeruli, secretion of waste products and drugs into tubules, and reabsorption of essential substances—but bile synthesis occurs exclusively in the liver and storage in the gallbladder, with no renal involvement in bile production or metabolism.
A) filtration
Glomerular filtration represents the kidney's primary function—filtering approximately 180 liters of plasma daily through glomerular capillaries into Bowman's capsules. This ultrafiltration removes water, ions, glucose, amino acids, and waste products (urea, creatinine) while retaining blood cells and large proteins—initiating urine formation essential for waste elimination and fluid balance.
B) bile production
Bile production occurs in hepatocytes of the liver—comprising bile salts (for fat emulsification), bilirubin (hemoglobin breakdown product), cholesterol, and electrolytes. Bile flows through hepatic ducts to the gallbladder for concentration/storage, then enters the duodenum via the common bile duct during digestion. Kidneys play no role in bile synthesis, secretion, or enterohepatic circulation—making this function entirely hepatic rather than renal.
C) secretion
Tubular secretion actively transports substances from peritubular capillaries into renal tubules—eliminating hydrogen ions (for pH regulation), potassium (for electrolyte balance), and organic acids/drugs (penicillin, creatinine) not adequately filtered. This process fine-tunes urine composition beyond filtration capabilities, enabling precise homeostatic control of blood chemistry.
D) re-absorption
Tubular reabsorption recovers approximately 99% of filtered water and essential solutes—glucose and amino acids completely reabsorbed in proximal tubule via active transport; sodium, chloride, and water reabsorbed throughout nephron segments according to hormonal regulation (aldosterone, ADH). This conservation mechanism prevents catastrophic fluid/electrolyte loss while concentrating waste products for excretion.
Conclusion:
Kidney functions center on blood filtration, selective secretion, and extensive reabsorption to maintain homeostasis—while bile production belongs exclusively to hepatic physiology. Option B correctly identifies the non-renal function, critical for understanding organ system specialization: confusing renal and hepatic functions could lead to misdiagnosis (e.g., attributing jaundice to kidney disease rather than liver dysfunction) or inappropriate treatment targeting the wrong organ system.
The outer layer of the eye is the ___
A.
cornea
B. sclera
C. retina
D. rods
Rationale
The sclera forms the outer layer of the eye. The sclera constitutes the tough, fibrous, opaque outer coat covering approximately five-sixths of the eyeball—providing structural integrity, attachment points for extraocular muscles, and protection for internal structures—while the transparent cornea forms only the anterior one-sixth of this outer fibrous tunic.
A) cornea
The cornea is the transparent anterior portion of the fibrous tunic—comprising five layers (epithelium, Bowman's layer, stroma, Descemet's membrane, endothelium)—responsible for approximately two-thirds of the eye's refractive power. While part of the outer coat, it represents only a specialized anterior segment, not the complete outer layer which is predominantly scleral tissue.
B) sclera
The sclera consists of dense irregular collagen bundles providing:
• Structural support: Maintains spherical shape against intraocular pressure (15–20 mmHg)
• Muscle attachment: Six extraocular muscles insert onto sclera for eye movement
• Protection: Shields delicate internal structures (retina, lens) from mechanical damage
• Continuity: Anteriorly blends with cornea at limbus; posteriorly perforated by optic nerve
Its opaque white appearance (due to irregular collagen scattering light) distinguishes it from transparent cornea—clinically visible as the "white of the eye" surrounding the colored iris.
C) retina
The retina forms the innermost neural layer—containing photoreceptors (rods/cones), bipolar cells, ganglion cells, and supporting glia—that transduces light into neural signals. It lies internal to the choroid (vascular layer) and sclera, separated from the outer coat by the suprachoroidal space—making it anatomically distant from the eye's external surface.
D) rods
Rods are photoreceptor cells within the retina specialized for low-light vision—containing rhodopsin pigment and concentrated in peripheral retina. As cellular components of the inner neural layer, rods represent microscopic structures rather than macroscopic anatomical layers—confusing cellular elements with tissue organization levels.
Conclusion:
The sclera constitutes the predominant outer fibrous layer providing structural integrity—distinct from the specialized transparent corneal segment anteriorly, vascular middle layer (choroid), or neural inner layer (retina). Option B correctly identifies the sclera as the primary outer coat, essential for understanding ocular anatomy: scleral thinning (staphyloma) compromises structural integrity, while scleritis causes severe pain due to rich innervation—conditions requiring accurate anatomical knowledge for diagnosis and management.
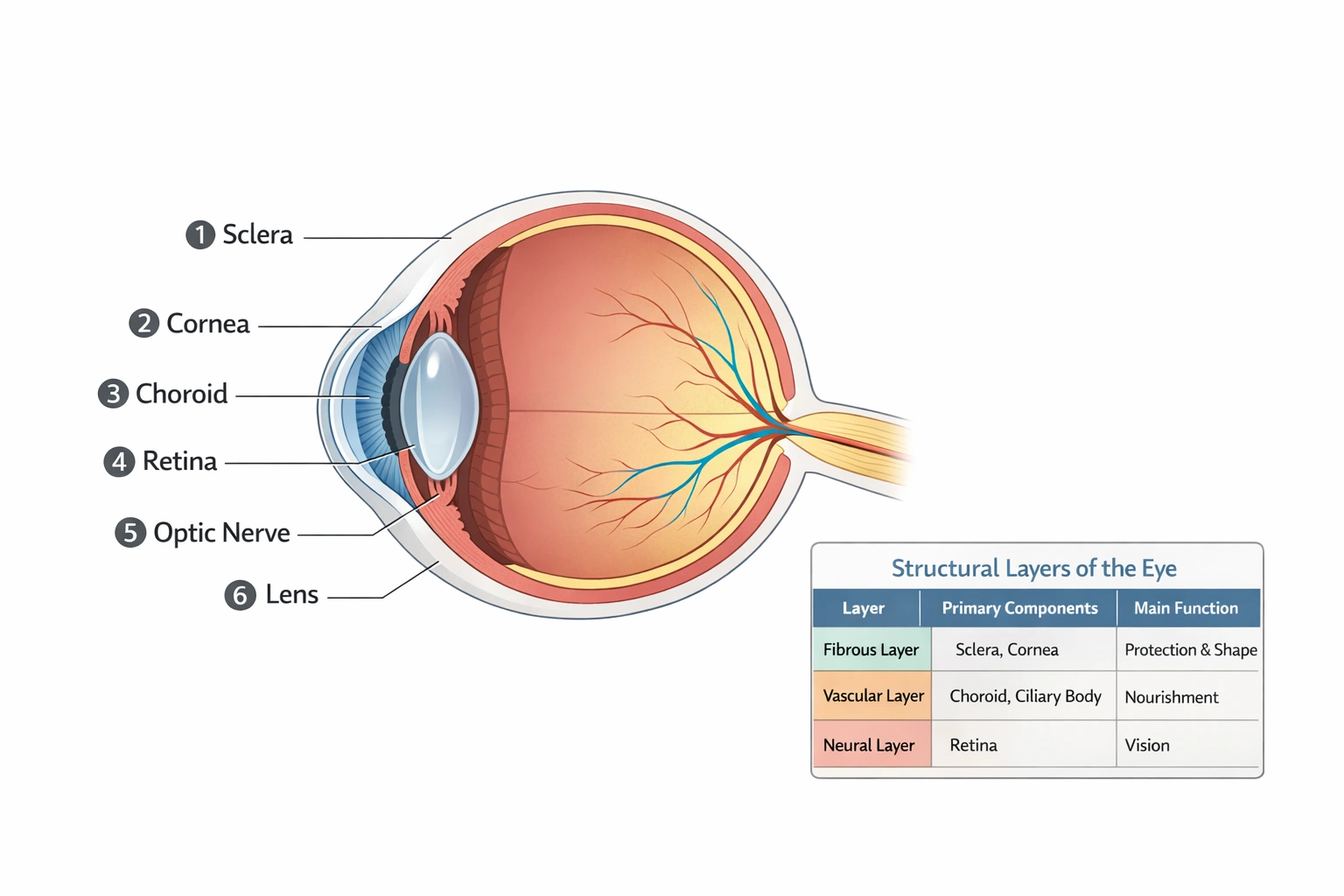
The horizontal rows of the periodic table are called ___
A.
periods
B. columns
C. rows
D. families
Rationale
Horizontal rows are called periods. Periods represent horizontal sequences in the periodic table where elements share the same highest principal quantum number for their outermost electrons—progressing from left to right with increasing atomic number and showing trends in atomic size, ionization energy, and electronegativity due to increasing nuclear charge within the same electron shell.
A) periods
Periods are numbered 1–7 corresponding to the highest principal energy level (n) occupied by electrons in ground state:
• Period 1: 2 elements (H, He) filling 1s orbital
• Periods 2–3: 8 elements each filling s and p orbitals
• Periods 4–5: 18 elements including d-block transition metals
• Periods 6–7: 32 elements including f-block lanthanides/actinides
Elements in the same period exhibit systematic property changes: atomic radius decreases left to right (increasing effective nuclear charge), ionization energy generally increases, and metallic character decreases—demonstrating periodic law within horizontal sequences.
B) columns
Columns describe vertical arrangements—not horizontal rows. Columns are properly termed groups or families (numbered 1–18 in IUPAC system), where elements share valence electron configuration and chemical properties—e.g., group 17 halogens all form -1 anions. Using "columns" for rows confuses spatial orientation fundamental to periodic table organization.
C) rows
While "rows" colloquially describes horizontal arrangements, the precise scientific term is "periods"—reflecting the periodic repetition of chemical properties when elements are arranged by atomic number. "Rows" lacks the conceptual meaning embedded in "periods," which derives from Mendeleev's observation of repeating ("periodic") property patterns at regular intervals—making "periods" the technically correct terminology in chemistry.
D) families
Families refer to groups of elements with similar chemical behavior—typically vertical columns (e.g., alkali metals family = group 1, halogen family = group 17). Some families span multiple groups (e.g., transition metals), but none describe horizontal arrangements. Using "families" for rows misapplies a term reserved for elements sharing chemical characteristics due to identical valence electron configurations.
Conclusion:
Periods represent the scientifically precise term for horizontal rows—embodying the foundational concept of periodicity where properties recur at regular intervals when elements are ordered by atomic number. Option A provides the correct terminology essential for chemical literacy: period number indicates valence shell principal quantum number, while group number indicates valence electron count—enabling prediction of element behavior and compound formation. Confusing periods with groups/families would impair understanding of periodic trends critical for reaction prediction and material design.
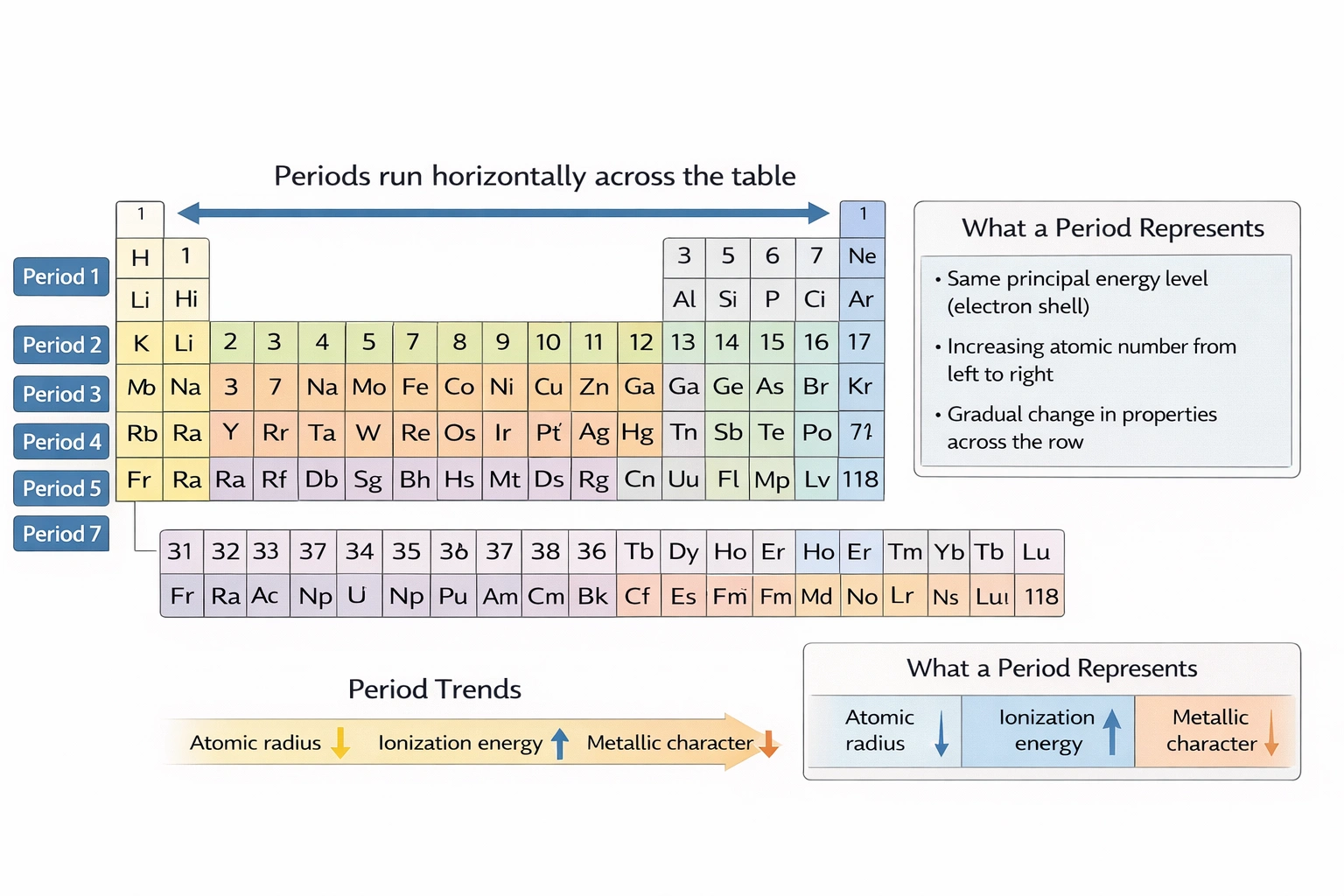
Converting gas into a liquid is known as ___
A.
evaporation
B. transitioning
C. condensation
D. sublimation
Rationale
Condensation converts gas into liquid. Condensation occurs when gas molecules lose sufficient kinetic energy (typically through cooling) to form intermolecular attractions that pull them into the liquid phase—releasing latent heat of vaporization and observable as dew formation, cloud development, or droplets on cold surfaces.
A) evaporation
Evaporation describes liquid-to-gas transition occurring at temperatures below boiling point—driven by high-energy molecules escaping the liquid surface. This process consumes heat (endothermic), cooling the remaining liquid—opposite to gas-to-liquid conversion. Evaporation increases with temperature, surface area, and airflow—fundamental to sweating thermoregulation and distillation processes.
B) transitioning
"Transitioning" is not a scientific term for phase changes—phase transitions have specific names (melting, freezing, vaporization, condensation, sublimation, deposition). Using vague terminology obscures the precise physical mechanisms governing state changes and lacks technical accuracy required in scientific communication.
C) condensation
Condensation mechanisms include:
• Cooling: Gas temperature drops below dew point, reducing molecular kinetic energy below escape threshold
• Compression: Increased pressure forces molecules closer, enhancing intermolecular attraction
• Nucleation: Condensation nuclei (dust, ions) provide surfaces for droplet formation
Examples: atmospheric water vapor condensing into clouds/rain; breath fogging cold glass; distillation apparatus condensers converting vapor back to liquid for collection. Condensation is exothermic—releasing approximately 2260 kJ/kg for water vapor—critical for Earth's heat distribution and industrial heat exchange systems.
D) sublimation
Sublimation describes direct solid-to-gas transition without passing through liquid phase (e.g., dry ice [CO₂] subliming at -78.5°C, mothballs [naphthalene] vaporizing at room temperature). The reverse process (gas-to-solid) is deposition (frost formation). Sublimation bypasses the liquid state entirely—making it distinct from gas-to-liquid condensation.
Conclusion:
Condensation specifically denotes gas-to-liquid phase transition through energy loss—distinct from liquid-to-gas evaporation (A), undefined "transitioning" (B), or solid-gas interconversions (D). Option C provides the precise thermodynamic term essential for understanding weather phenomena (cloud formation), engineering systems (refrigeration cycles), and laboratory techniques (distillation). Misidentifying phase changes could lead to design errors in HVAC systems or misinterpretation of atmospheric processes critical for climate modeling.
An acid is a substance that increases the ___ count in water.
A.
chloride ion
B. hydroxide ion
C. hydrogen ion
D. oxygen
Rationale
Acids increase hydrogen ion concentration in water. According to the Arrhenius definition, acids dissociate in aqueous solution to release hydrogen ions (Hâº), which immediately associate with water molecules to form hydronium ions (H₃Oâº)—lowering pH and conferring characteristic acidic properties like sour taste, reactivity with metals, and ability to neutralize bases.
A) chloride ion
Chloride ions (Clâ») derive from hydrochloric acid dissociation (HCl → H⺠+ Cl) but aren't defining features of acidity—many acids contain no chlorine (acetic acid CH₃COOH, sulfuric acid Hâ‚‚SOâ‚„). Chloride concentration doesn't determine acidity; HCl and NaCl solutions both contain Clâ» but only HCl is acidic. Chloride is a spectator ion in many acid reactions rather than the active acidic component.
B) hydroxide ion
Hydroxide ions (OHâ») characterize bases—not acids—according to Arrhenius theory. Bases increase OHâ» concentration in water (NaOH → Na⺠+ OH), raising pH above 7. Acids and bases have opposing effects: acids increase H⺠while decreasing OHâ» (via Kw = [Hâº][OHâ»] = 10â»Â¹â´), making hydroxide ion increase incompatible with acidic solutions.
C) hydrogen ion
Acid dissociation mechanisms include:
• Strong acids: Complete dissociation (HCl → H⺠+ Cl; Hâ‚‚SOâ‚„ → 2H⺠+ SO²â»)
• Weak acids: Partial dissociation establishing equilibrium (CH₃COOH H⺠+ CH₃COOâ»)
Hydrogen ions immediately hydrate: H⺠+ Hâ‚‚O → H₃O⺠(hydronium ion), with further hydration forming Hâ‚…Oâ‚‚âº, H₉O₄⺠clusters. pH = -log[Hâº] quantifies acidity—each pH unit represents tenfold [Hâº] change (pH 3 has 10× more H⺠than pH 4). This hydrogen ion release defines acidity across all aqueous contexts.
D) oxygen
Oxygen presence doesn't determine acidity—many acids lack oxygen (HCl, HBr, HI = hydrohalic acids), while many oxygen-containing compounds aren't acidic (sucrose Câ‚â‚‚Hâ‚‚â‚‚Oâ‚â‚, ethanol Câ‚‚Hâ‚…OH). Oxygenated acids (oxyacids like HNO₃, Hâ‚‚SOâ‚„) derive acidity from polar O-H bonds facilitating H⺠release—not oxygen presence itself. Dissolved oxygen (Oâ‚‚) in water doesn't affect pH significantly.
Conclusion:
Hydrogen ion concentration exclusively defines aqueous acidity—fundamental to pH concept, acid-base reactions, and buffer systems. Option C correctly identifies this defining characteristic, distinguishing acids from bases (OHâ» producers) and non-acidic compounds. Understanding this principle enables prediction of acid behavior: strong acids fully dissociate yielding high [Hâº], weak acids partially dissociate yielding moderate [Hâº], and pH calculations quantify acidity for applications ranging from pharmaceutical formulation to environmental monitoring of acid rain.
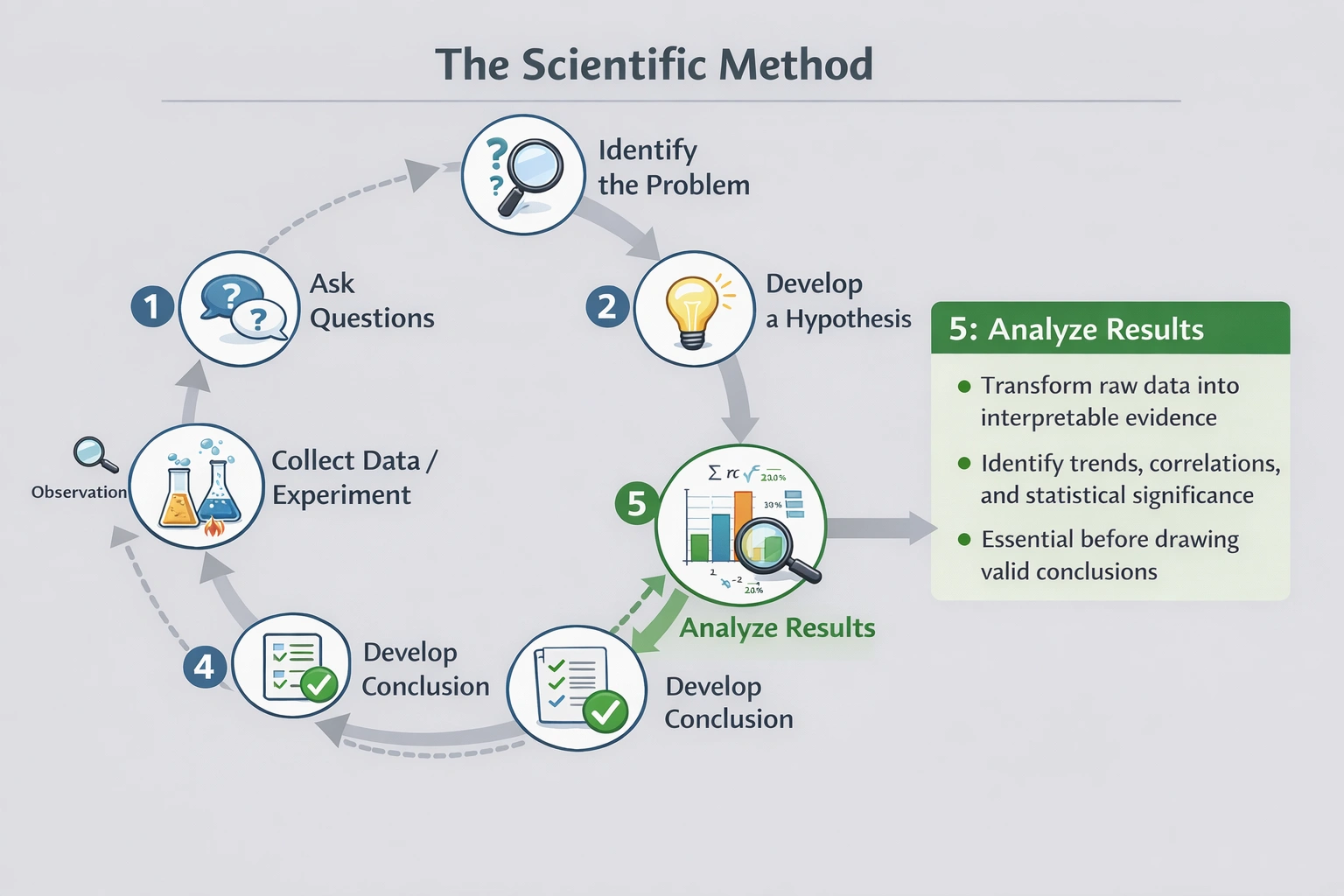
The first four steps of the scientific method are as follows: I. Identify the problem II. Ask questions III. Develop a hypothesis IV. Collect data and experiment on that data Which of the following is the fifth step in the scientific method?
A.
Observe the data
B. Analyze the results
C. Measure the data
D. Develop a conclusion
Rationale
Analyzing the results is the fifth step in the scientific method. After collecting experimental data scientists must systematically process and interpret that information to extract meaningful patterns relationships and statistical significance. This analytical phase transforms raw measurements into evidence that can objectively support or refute the original hypothesis without analysis researchers cannot distinguish genuine effects from random variation or experimental error.
A) Observe the data
Observation occurs continuously throughout the scientific process particularly during initial problem identification and active data collection. By the time step IV concludes observation has already been completed and documented as raw data. Repeating observation without analytical processing merely restates collected information without advancing understanding or evaluating the hypothesis. This option confuses ongoing observational practice with the discrete analytical step required after data collection.
B) Analyze the results
Analysis serves as the essential bridge between data collection and conclusion formation. Scientists apply statistical methods to determine significance identify trends through graphical representation assess measurement errors and evaluate whether outcomes align with hypothesis predictions. This step requires critical evaluation of patterns correlations and deviations before any judgment about hypothesis validity can be made. Without rigorous analysis researchers risk drawing conclusions based on coincidence misinterpreting outliers as meaningful results or overlooking subtle but important relationships embedded in the data set. Analysis transforms numbers and observations into interpretable scientific evidence.
C) Measure the data
Measurement constitutes an integral component of data collection itself not a subsequent step. During experimentation researchers use instruments to quantify variables producing the numerical or categorical records that form the experimental dataset. Once collection concludes the data already exists in measured form. Re-measuring would constitute additional data gathering rather than progression through the methodological sequence. Measurement without analysis yields uninterpreted values lacking scientific meaning and does not advance the investigation toward hypothesis evaluation.
D) Develop a conclusion
Conclusions represent the sixth step following analysis not the fifth. Drawing valid conclusions requires the analytical groundwork of processing data identifying significant patterns calculating statistical confidence and ruling out alternative explanations. Premature conclusion development bypasses critical evaluation potentially mistaking experimental artifacts for genuine effects or attributing random fluctuations to causal relationships. Scientific conclusions must reference analytical findings such as statistical significance levels or pattern recognition results making analysis an indispensable prerequisite that logically precedes conclusion formation.
Conclusion:
The scientific method follows a strict logical sequence where analysis necessarily precedes conclusion formation. Analysis transforms raw experimental output into evaluated evidence enabling objective hypothesis assessment. Without this critical processing step researchers cannot determine whether results genuinely support their predictions or reflect chance occurrences. Option B correctly identifies analysis as the fifth step essential for maintaining scientific rigor preventing bias and ensuring conclusions rest on properly interpreted evidence rather than unprocessed observations. This sequence safeguards against erroneous interpretations that could arise from skipping analytical evaluation before drawing final conclusions.
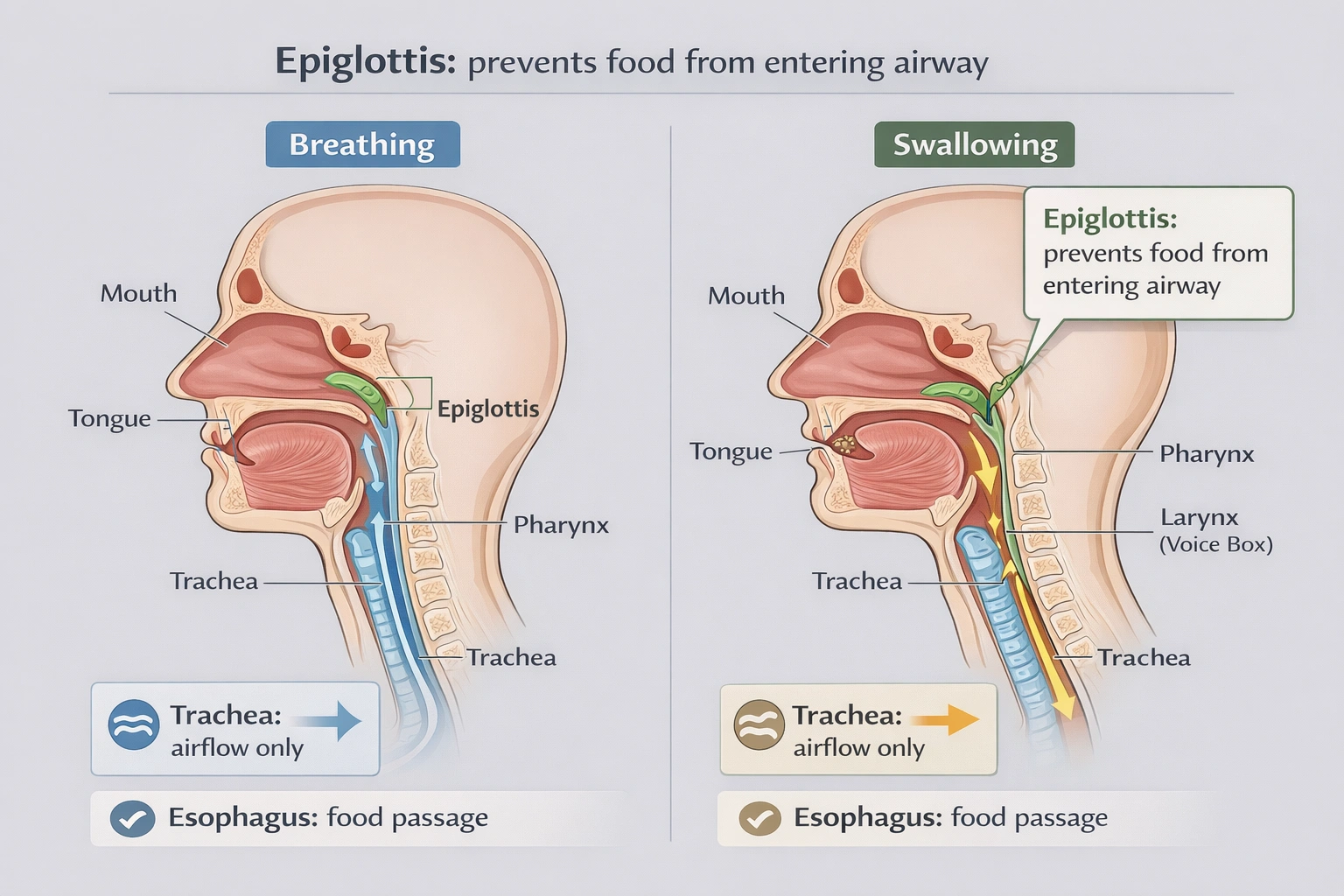
What is the name of the structure that prevents food from entering the airway?
A.
trachea
B. esophagus
C. diaphragm
D. epiglottis
Rationale
The epiglottis prevents food from entering the airway. The epiglottis is a leaf-shaped flap of elastic cartilage located at the base of the tongue that folds backward during swallowing to cover the laryngeal inlet and direct food and liquids into the esophagus rather than the trachea enabling safe passage of ingested material while protecting the respiratory tract from aspiration.
A) trachea
The trachea serves as the airway conduit carrying air to and from the lungs and does not prevent food entry. Instead it represents the passage that requires protection during swallowing. The trachea begins below the larynx and extends to the bronchi with C-shaped cartilaginous rings maintaining its patency for airflow but offering no mechanism to block food entry.
B) esophagus
The esophagus functions as the muscular tube transporting food from the pharynx to the stomach but does not prevent airway entry. It receives food only after the epiglottis has successfully directed material away from the larynx toward the esophageal opening. The esophagus lies posterior to the trachea and serves as the destination for swallowed material rather than the protective structure.
C) diaphragm
The diaphragm is the primary respiratory muscle separating the thoracic and abdominal cavities responsible for inhalation through contraction. It plays no role in swallowing mechanics or airway protection during ingestion. Located far below the larynx the diaphragm functions in breathing not in preventing aspiration of food into the upper airway.
D) epiglottis
During swallowing the epiglottis performs a critical protective reflex. The larynx elevates and the epiglottis flips downward covering the glottis like a lid while the vocal cords close beneath it. This coordinated action directs the food bolus laterally around the larynx into the piriform sinuses and then into the esophagus. Failure of this mechanism causes aspiration pneumonia demonstrating the epiglottis essential role in airway protection.
Conclusion:
The epiglottis serves as the specialized anatomical structure designed specifically to prevent food and liquid entry into the airway during swallowing. Its elastic cartilage composition allows flexible movement to cover the laryngeal inlet precisely when needed while remaining upright during breathing to permit unobstructed airflow. Option D correctly identifies this vital protective structure distinguishing it from airway conduits (trachea, esophagus) or respiratory muscles (diaphragm) that lack this specific protective function.
Organized from high to low, the hierarchy of the human bodys structure is as follows: organism, organ systems, organs, tissues. Which of the following comes next?
A.
molecules
B. atoms
C. cells
D. muscle
Rationale
Cells follow tissues in the structural hierarchy of the human body. Cells represent the fundamental structural and functional units of life forming the building blocks that organize into tissues with specialized cells working cooperatively to perform specific physiological functions making cells the immediate subunit below tissues in the anatomical organization sequence.
A) molecules
Molecules constitute chemical structures smaller than cells including proteins lipids carbohydrates and nucleic acids that perform cellular functions but do not represent the next organizational level after tissues. Molecules assemble to form cellular components organelles and structures but the hierarchical progression moves from tissues to their cellular constituents before descending to molecular components.
B) atoms
Atoms represent the smallest units of chemical elements and form the building blocks of molecules but exist at a lower organizational level than both cells and molecules. The structural hierarchy progresses from macroscopic to microscopic organization with atoms appearing several levels below tissues after cells organelles and molecules making atoms too granular to be the immediate next level.
C) cells
The complete structural hierarchy from largest to smallest follows:
• Organism: Entire living being
• Organ systems: Groups of organs working together (circulatory digestive)
• Organs: Structures of multiple tissue types (heart stomach)
• Tissues: Groups of similar cells performing specific functions (epithelial muscle)
• Cells: Basic structural and functional units of life (neurons erythrocytes)
• Organelles: Cellular substructures (mitochondria nucleus)
• Molecules: Chemical compounds (proteins DNA)
• Atoms: Elemental particles (carbon oxygen)
Tissues by definition consist of groups of similar cells working together making cells the immediate structural components that aggregate to form tissues.
D) muscle
Muscle represents a specific tissue type (one of the four primary tissue categories: epithelial connective muscle nervous) rather than a hierarchical level. Muscle tissue itself consists of muscle cells (myocytes) organized into fibers making muscle a category within the tissue level not the level below tissues.
Conclusion:
Cells form the essential building blocks that organize into tissues establishing cells as the immediate subunit in the structural hierarchy below tissues. Option C correctly identifies this fundamental organizational principle central to anatomy and physiology. Cells represent the smallest units of life capable of independent function while tissues emerge from cellular cooperation. This hierarchy reflects biological organization from whole organism down to atomic structure with each level building upon the one below it providing the framework for understanding how microscopic components create macroscopic bodily functions.
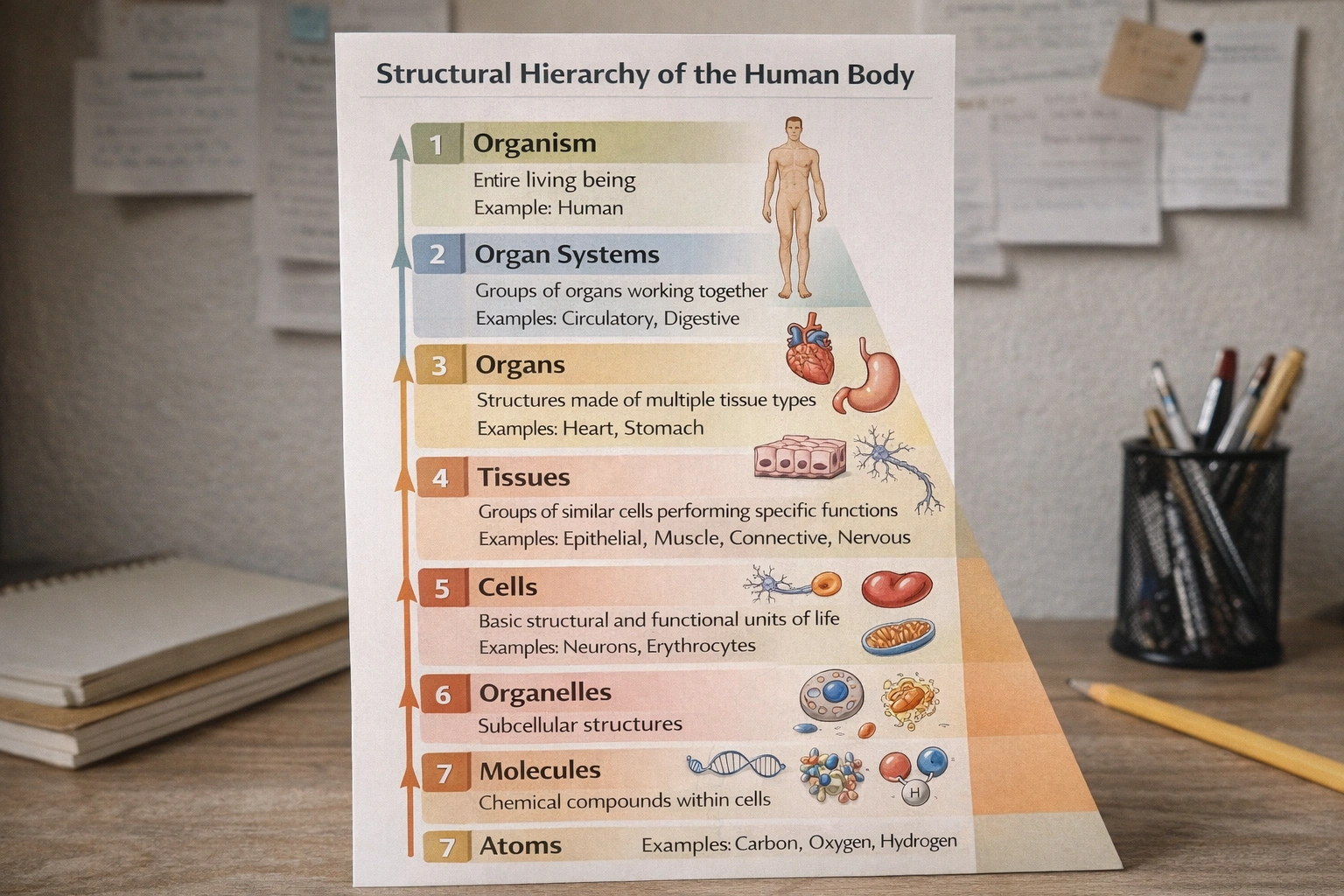
In your garden, you noticed that the tomato plants did better on the north side of your house than the west side and you decided to figure out why. They are both planted with the same soil that provides adequate nutrients to the plant, and they are watered at the same time during the week. Over the course of a week, you begin to measure the amount of sunlight that hits each side of the house and determine that the north side gets more light because the sunlight is blocked by the houses shadow on the west side. What is the name of the factor in your observations that affected the tomato plants growth?
A.
The control
B. The independent variable
C. The dependent variable
D. The conclusion
Rationale
Sunlight exposure represents the independent variable in this experiment. The independent variable is the factor deliberately observed or manipulated by the researcher to determine its effect on the outcome—in this case, the amount of sunlight differing between north and west sides was the measured factor hypothesized to influence plant growth.
A) The control
Controls are factors intentionally kept constant across experimental groups to eliminate alternative explanations for results. In this experiment soil type watering schedule and plant species served as controls because they remained identical on both sides of the house. The sunlight difference was not controlled but rather measured as the varying factor making it not a control variable.
B) The independent variable
The independent variable is the presumed cause that researchers measure or manipulate to observe its effect on the outcome. Here sunlight exposure varied naturally between locations with the north side receiving more light due to reduced shadowing. This variation was identified as the potential explanatory factor for differential plant growth making sunlight the independent variable. The researcher measured this factor to test its relationship with plant performance.
C) The dependent variable
The dependent variable is the measured outcome or effect—in this case the tomato plants' growth performance which differed between locations. The plants growing better on the north side represents the dependent variable because it responds to or depends on the independent variable (sunlight exposure). The question asks for the factor that affected growth not the growth itself making this option incorrect for the query.
D) The conclusion
A conclusion represents the interpretation drawn after analyzing relationships between variables—not the variable itself. The conclusion might state that increased sunlight caused better growth but the sunlight factor itself is not the conclusion. It is the independent variable that informed the conclusion.
Conclusion:
Experimental design requires distinguishing between variables that influence outcomes (independent variables) and the outcomes themselves (dependent variables). In this observational study sunlight exposure served as the independent variable whose variation correlated with plant growth differences. Option B correctly identifies this causal factor essential for understanding experimental methodology and drawing valid scientific inferences from observed patterns.
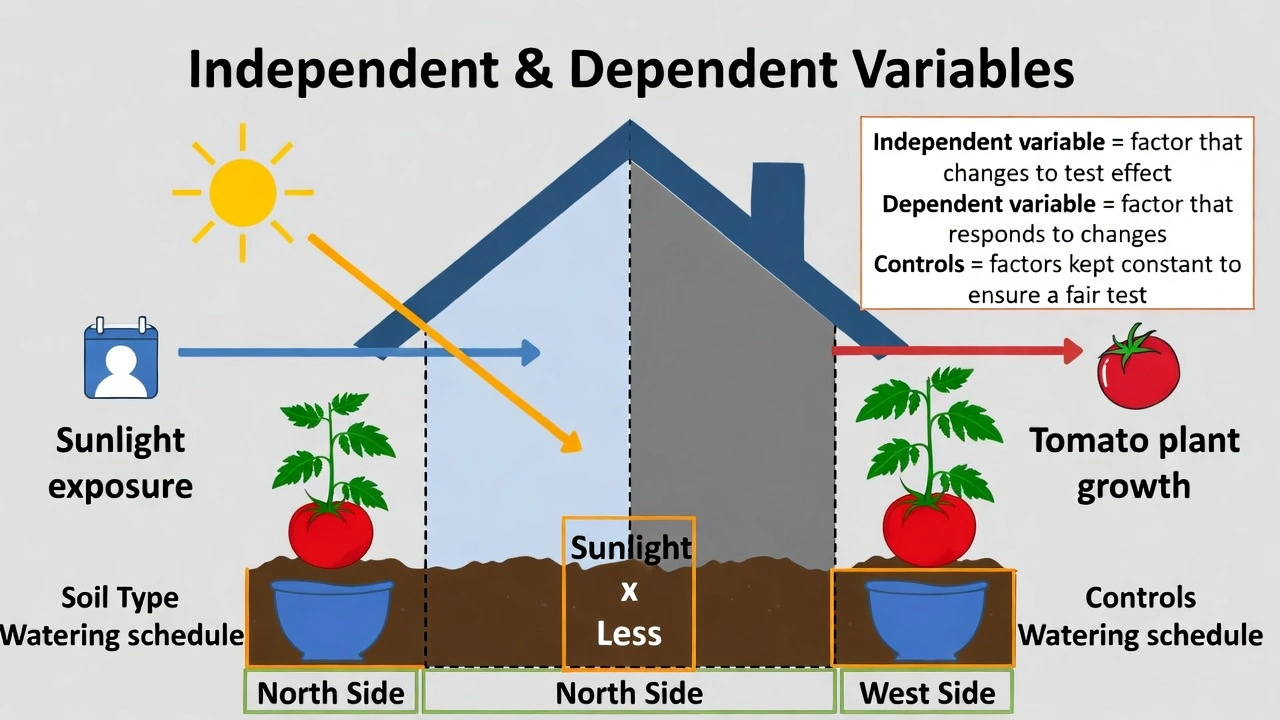
Which of the following best describes the careful ordering of molecules within solids that have a fixed shape?
A.
Physical bonding
B. Polar molecules
C. Metalloid structure
D. Crystalline order
Rationale
Crystalline order describes the precise molecular arrangement in solids with fixed shapes. Crystalline solids feature atoms molecules or ions arranged in highly organized repeating three-dimensional patterns called crystal lattices that produce definite geometric shapes sharp melting points and characteristic cleavage planes distinguishing them from amorphous solids lacking long-range order.
A) Physical bonding
Physical bonding refers to intermolecular forces like hydrogen bonding dipole-dipole interactions or London dispersion forces that influence physical properties but do not specifically describe molecular ordering. While these forces contribute to crystal formation they represent the attractive mechanisms rather than the resulting ordered arrangement itself.
B) Polar molecules
Polarity describes uneven electron distribution within molecules creating partial charges but does not define molecular ordering. Many crystalline solids contain nonpolar molecules arranged in ordered lattices while many polar substances form amorphous solids. Polarity influences solubility and melting points but is not synonymous with crystalline structure.
C) Metalloid structure
Metalloids are elements with properties intermediate between metals and nonmetals (silicon germanium arsenic). Their atomic structure does not define molecular ordering in solids. Metalloids can form crystalline structures but the term describes elemental classification not the ordering principle applicable to all crystalline solids including ionic molecular and metallic crystals.
D) Crystalline order
Crystalline order manifests as:
• Long-range repeating patterns extending throughout the material
• Definite geometric external shapes reflecting internal symmetry
• Sharp melting points where solid transitions completely to liquid at specific temperature
• Characteristic cleavage along crystallographic planes
• X-ray diffraction patterns revealing lattice spacing
Examples include sodium chloride (cubic crystals) quartz (hexagonal prisms) and diamond (tetrahedral networks). All share the fundamental property of molecules arranged in precise predictable positions creating solids with fixed shapes and volumes.
Conclusion:
Crystalline order represents the specific organizational principle that produces solids with fixed geometric shapes through repeating molecular arrangements. Option D correctly identifies this concept distinguishing crystalline solids from amorphous materials like glass or plastic that lack long-range order and therefore do not maintain definite shapes upon fracture. Understanding crystalline structure proves essential for materials science pharmaceutical development and mineral identification where molecular arrangement determines physical properties and functionality.
A(n) ___ is the physical and visible expression of a genetic trait.
A.
Phenotype
B. Allele
C. Gamete
D. Genotype
Rationale
Phenotype represents the physical and visible expression of a genetic trait. Phenotype encompasses all observable characteristics of an organism including morphology physiology and behavior resulting from interactions between its genetic makeup (genotype) and environmental influences.
A) Phenotype
Phenotype includes:
• Physical traits such as eye color height flower color or blood type
• Physiological characteristics like enzyme activity metabolic rate or disease susceptibility
• Behavioral traits in some contexts such as nesting behavior in birds
Phenotypes result from gene expression modified by environmental factors identical genotypes can produce different phenotypes under varying conditions demonstrating the genotype-environment interaction fundamental to biology.
B) Allele
An allele is a specific variant form of a gene occupying a particular locus on a chromosome. Organisms inherit two alleles for each autosomal gene one from each parent. Alleles represent genetic information variants not their physical expression. For example the allele for brown eyes exists as DNA sequence information but the brown eye color itself is the phenotype.
C) Gamete
Gametes are haploid reproductive cells (sperm and egg) that fuse during fertilization to form a diploid zygote. They carry genetic information to offspring but do not represent trait expression. Gametes themselves have minimal phenotypic characteristics beyond motility or size and do not display the traits they may transmit to offspring.
D) Genotype
Genotype refers to the specific genetic makeup of an organism—the particular alleles present at relevant gene loci. Genotype represents the inherited instructions for trait development but not their physical manifestation. For example BB Bb and bb represent genotypes for a flower color gene while purple or white flowers represent the corresponding phenotypes.
Conclusion:
Phenotype and genotype represent complementary concepts in genetics with genotype providing the genetic instructions and phenotype representing their observable expression. Option A correctly identifies phenotype as the physical manifestation of genetic traits essential for understanding inheritance patterns natural selection acting on visible characteristics and gene-environment interactions that produce variation within populations.
Which of the following best describes a section that divides the body into equal upper and lower portions?
A.
Coronal
B. Transverse
C. Oblique
D. Median
Rationale
The transverse plane divides the body into upper and lower portions. The transverse (horizontal) plane runs parallel to the ground cutting horizontally through the body to create superior (upper) and inferior (lower) sections with the exact midpoint creating equal halves.
A) Coronal
The coronal (frontal) plane divides the body into anterior (front) and posterior (back) portions running vertically from side to side perpendicular to the sagittal plane. Examples include a coronal section through the shoulders separating chest from back. This plane does not create upper and lower divisions.
B) Transverse
The transverse plane runs horizontally parallel to the ground intersecting the body at right angles to both sagittal and coronal planes. A transverse section through the waist creates upper body (torso head arms) and lower body (legs pelvis) portions. A transverse section precisely at the body's midpoint would divide it into equal upper and lower halves. This plane is essential for cross-sectional imaging like CT scans that display horizontal body slices.
C) Oblique
Oblique sections cut diagonally at angles not parallel to any of the three primary anatomical planes. These sections create irregular divisions not standardized upper-lower anterior-posterior or left-right separations. While useful for specific surgical approaches oblique planes do not produce equal standardized body portions and lack the precise orientation required for consistent anatomical description.
D) Median
The median plane is the specific midline sagittal plane that divides the body into equal left and right halves running vertically from front to back through the midline structures (nose umbilicus spine). Sagittal planes parallel to the median plane create unequal left-right portions but none create upper-lower divisions.
Conclusion:
The transverse plane uniquely creates horizontal divisions separating the body into upper and lower portions with a precisely positioned transverse section yielding equal halves. Option B correctly identifies this anatomical plane essential for medical imaging surgical planning and precise anatomical description distinguishing it from vertical planes (coronal median) that create front-back or left-right divisions.
The Punnett square shown here indicates a cross between two parents, one with alleles BB and the other with alleles Bb. Select the correct entry for the upper right box in the Punnett square, which is indicated with the letter, x:
A.
Bb
B. bB
C. BB
D. bb
Rationale
BB is the correct entry for the upper right box in the Punnett square. The upper right box results from combining the second allele from the top parent (B) with the allele from the side parent (B) creating a homozygous dominant genotype.
A) Bb
This would represent a heterozygous genotype resulting from combining a B allele from the top parent with a b allele from the side parent. This combination would appear in the lower right box of the Punnett square not the upper right box.
B) bB
This notation is incorrect as genotypes are conventionally written with the dominant allele first (Bb not bB). The upper right box combines two dominant alleles resulting in BB not a heterozygous genotype.
C) BB
The Punnett square setup shows:
• Top row: B and B alleles (from BB parent)
• Left column: B and b alleles (from Bb parent)
The upper right box combines the second B allele from the top parent with the B allele from the side parent resulting in BB. This homozygous dominant genotype appears in the upper right box while the upper left box would contain BB as well since it combines the first B from top with B from side.
D) bb
This homozygous recessive genotype would require b alleles from both parents but the top parent has only B alleles (BB) making bb impossible in any box of this Punnett square.
Conclusion:
Punnett squares systematically combine alleles from each parent to determine possible offspring genotypes. The upper right box specifically results from the second B allele of the BB parent combining with the B allele of the Bb parent producing BB. Option C correctly identifies this genotype essential for understanding Mendelian inheritance patterns and predicting offspring traits in genetic crosses.
What is the most likely reason that cells differentiate?
A.
Cells differentiate to avoid looking like all the cells around them
B. Cells differentiate so that simple non-specialized cells can become highly specialized cells
C. Cells differentiate so that multicellular organisms will remain the same size
D. Cells differentiate for no apparent reason
Rationale
Cells differentiate to become highly specialized from simple non-specialized cells. Cellular differentiation enables multicellular organisms to develop diverse tissue types with specialized functions from a single fertilized egg through regulated gene expression where different cell lineages activate specific subsets of genes while silencing others creating structural and functional diversity essential for complex organismal physiology.
A) Cells differentiate to avoid looking like all the cells around them
Cellular differentiation follows genetically programmed developmental pathways not aesthetic preferences. Cells differentiate based on positional information morphogen gradients and cell-cell signaling during embryogenesis not to achieve visual variety. Differentiation serves functional purposes not cosmetic diversity.
B) Cells differentiate so that simple, non-specialized cells can become highly specialized cells
Differentiation transforms pluripotent stem cells into specialized cell types with distinct structures and functions:
• Erythrocytes lose nuclei to maximize hemoglobin capacity for oxygen transport
• Neurons develop long axons and dendrites for electrical signal conduction
• Muscle cells accumulate contractile proteins for force generation
• Pancreatic beta cells produce insulin in response to blood glucose levels
This specialization enables division of labor where different tissues perform complementary functions creating organismal complexity impossible with uniform cell types.
C) Cells differentiate so that multicellular organisms will remain the same size
Differentiation relates to cellular specialization not size regulation. Organism size depends on cell number (controlled by cell division rates apoptosis and nutrient availability) not differentiation status. Undifferentiated stem cells can divide extensively while differentiated cells may stop dividing entirely. Size homeostasis involves hormonal regulation growth factors and mechanical constraints unrelated to differentiation per se.
D) Cells differentiate for no apparent reason
Differentiation serves clear adaptive purposes enabling multicellular organisms to develop complex organ systems with specialized functions that enhance survival and reproduction. Single-celled organisms perform all life functions within one cell while multicellular organisms achieve greater efficiency through cellular specialization allowing larger body sizes complex behaviors and environmental adaptation.
Conclusion:
Cellular differentiation provides the foundation for multicellular complexity by enabling specialized cell types to perform specific functions more efficiently than generalized cells could. Option B correctly identifies this fundamental biological principle essential for understanding embryonic development tissue regeneration stem cell therapies and evolutionary transitions to multicellularity.
What type of chemical bond connects the oxygen and hydrogen atoms in a molecule of water?
A.
Static bond
B. Aquatic bond
C. Ionic bond
D. Covalent bond
Rationale
Covalent bonds connect oxygen and hydrogen atoms in water. Water molecules form when oxygen shares electrons with two hydrogen atoms creating polar covalent bonds where electrons spend more time near the electronegative oxygen atom generating partial charges that enable hydrogen bonding between molecules.
A) Static bond
No chemical bond type called "static bond" exists in chemistry. Static electricity involves charge separation but does not describe intramolecular bonding within stable compounds like water.
B) Aquatic bond
"Aquatic bond" is not a recognized chemical term. Water's properties arise from covalent intramolecular bonds and hydrogen intermolecular bonds not a nonexistent "aquatic" bond type.
C) Ionic bond
Ionic bonds involve complete electron transfer creating oppositely charged ions held together by electrostatic attraction as in sodium chloride. Water does not form through electron transfer; oxygen does not fully remove electrons from hydrogen. Instead electrons are shared unequally creating polar covalent bonds. Water molecules remain discrete entities rather than forming ionic lattices.
D) Covalent bond
Oxygen has six valence electrons and requires two more to complete its octet. Each hydrogen has one electron and requires one more to achieve a stable duet configuration. Oxygen shares one electron with each hydrogen forming two single covalent bonds. The bonds are polar because oxygen's higher electronegativity (3.44 versus hydrogen's 2.20) draws shared electrons closer creating a partial negative charge on oxygen and partial positive charges on hydrogens. This polarity enables water's unique properties including high surface tension solvent capabilities and hydrogen bonding.
Conclusion:
Water's molecular structure depends on polar covalent bonding between oxygen and hydrogen atoms. Option D correctly identifies this fundamental chemical principle distinguishing covalent (electron sharing) from ionic (electron transfer) and nonexistent bond types. Understanding water's covalent nature explains its molecular stability while its polarity accounts for emergent properties critical to biological systems and Earth's climate.
What is the name for any substance that stimulates the production of antibodies?
A.
collagen
B. hemoglobin
C. lymph
D. antigen
Rationale
Antigens stimulate antibody production. Antigens are foreign substances (typically proteins or polysaccharides) on pathogens like bacteria viruses or allergens that trigger adaptive immune responses when recognized by B lymphocytes leading to clonal expansion and differentiation into plasma cells that secrete specific antibodies against the antigenic epitopes.
A) collagen
Collagen is a structural protein providing tensile strength in connective tissues (skin bones and tendons). It constitutes the body's most abundant protein but functions mechanically not immunologically. While collagen can become antigenic in autoimmune disorders like rheumatoid arthritis it is not defined by its ability to stimulate antibody production under normal physiological conditions.
B) hemoglobin
Hemoglobin is the oxygen-carrying protein in red blood cells containing iron-rich heme groups that bind oxygen in lungs and release it in tissues. While hemoglobin variants can trigger immune responses in transfusion reactions it serves primarily as a respiratory pigment not as a general antibody-stimulating substance.
C) lymph
Lymph is the fluid derived from interstitial fluid that circulates through lymphatic vessels containing white blood cells proteins and cellular debris. It serves as a transport medium for immune cells and antigens but is not itself a substance that stimulates antibody production. Lymph nodes filter lymph and house immune cells that respond to antigens carried within the lymph.
D) antigen
Antigens possess specific molecular features called epitopes that bind to B cell receptors triggering activation when accompanied by appropriate co-stimulatory signals. Antigen-presenting cells process and display antigen fragments on MHC class II molecules to helper T cells which then provide cytokine signals enabling B cells to proliferate and differentiate. Antibody specificity matches the antigen's molecular structure enabling targeted neutralization opsonization or complement activation against the invading pathogen.
Conclusion:
Antigens represent the fundamental immunological triggers that initiate adaptive humoral immunity through specific B cell activation and antibody production. Option D correctly identifies this essential immunological concept distinguishing antigens from structural proteins (collagen hemoglobin) transport fluids (lymph) or other biological molecules that lack this defining immune-stimulating property.
What kind of bond connects sugar and phosphate in DNA?
A.
hydrogen
B. ionic
C. covalent
D. overt
Rationale
Covalent bonds connect sugar and phosphate groups in DNA. Phosphodiester bonds form when the 5' phosphate group of one nucleotide reacts with the 3' hydroxyl group of the adjacent nucleotide's deoxyribose sugar creating strong covalent linkages that form the sugar-phosphate backbone providing structural stability to the DNA molecule.
A) hydrogen
Hydrogen bonds connect complementary nitrogenous bases between the two DNA strands (adenine-thymine with two hydrogen bonds guanine-cytosine with three hydrogen bonds). These relatively weak bonds allow strand separation during replication and transcription but do not link sugar to phosphate within a single strand.
B) ionic
Ionic bonds involve complete electron transfer creating charged ions held by electrostatic attraction. DNA's sugar-phosphate backbone contains no ionic bonds though the phosphate groups carry negative charges at physiological pH requiring cationic proteins like histones for neutralization. Ionic interactions stabilize DNA-protein complexes but not the covalent backbone structure.
C) covalent
Phosphodiester bonds are covalent linkages formed through dehydration synthesis where a phosphate group bridges two sugar molecules. The phosphate connects to the 5' carbon of one deoxyribose and the 3' carbon of the next creating directional (5'→3') polarity essential for replication and transcription enzymes. These strong bonds (approximately 335 kJ/mol) provide the backbone stability necessary for genetic information preservation across cell divisions.
D) overt
"Overt bond" is not a recognized chemical bond type in biochemistry or molecular biology. This term has no scientific meaning in the context of molecular structure or DNA chemistry.
Conclusion:
The sugar-phosphate backbone of DNA relies on covalent phosphodiester bonds for structural integrity while hydrogen bonds mediate complementary base pairing between strands. Option C correctly identifies the covalent nature of backbone linkages essential for understanding DNA stability replication fidelity and the chemical basis of genetic information storage.
Which kind of radiation has no charge?
A.
beta
B. alpha
C. delta
D. gamma
Rationale
Gamma radiation has no charge. Gamma rays are high-energy electromagnetic radiation (photons) emitted from atomic nuclei during radioactive decay or nuclear reactions possessing no mass and no electrical charge unlike particulate radiation types.
A) beta
Beta radiation consists of high-speed electrons (beta-minus decay) or positrons (beta-plus decay) carrying negative or positive charge respectively. These charged particles ionize matter through electromagnetic interactions and deflect in magnetic fields due to their charge.
B) alpha
Alpha radiation comprises helium nuclei containing two protons and two neutrons carrying a +2 charge. These heavy charged particles produce intense ionization but have limited penetration stopping in paper or skin. The charge enables deflection in electric and magnetic fields.
C) delta
Delta radiation is not a recognized type of nuclear radiation in physics. This term may refer to delta rays (secondary electrons produced by primary radiation) but is not a primary radiation category like alpha beta or gamma.
D) gamma
Gamma rays are photons (electromagnetic radiation) at the highest energy end of the spectrum with wavelengths shorter than 0.01 nanometers. Produced during nuclear de-excitation gamma rays travel at light speed penetrate deeply through matter (requiring dense shielding like lead) and do not deflect in electromagnetic fields due to zero charge and mass.
Conclusion:
Gamma radiation uniquely consists of uncharged photons distinguishing it from charged particulate radiation types (alpha and beta). Option D correctly identifies gamma rays as the neutral radiation form essential for understanding radiation protection principles where gamma's lack of charge enables deep tissue penetration unlike easily stopped charged particles.
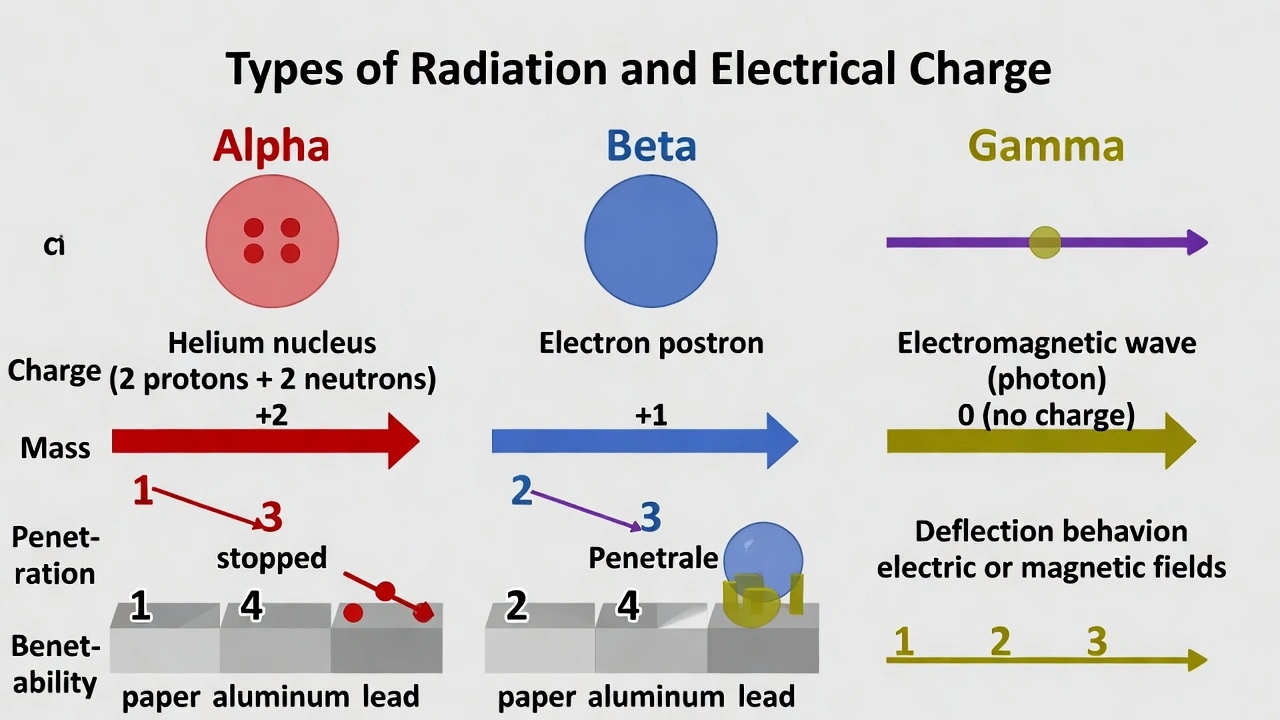
Which of the following devices changes chemical energy into electrical energy?
A.
battery
B. closed electric circuit
C. generator
D. transformer
Rationale
Batteries convert chemical energy into electrical energy. Batteries contain electrochemical cells where spontaneous redox reactions between anode and cathode materials release energy as electrons flow through an external circuit creating electric current with chemical potential energy transforming directly into electrical work.
A) battery
Batteries operate through oxidation-reduction reactions where the anode undergoes oxidation releasing electrons that travel through an external circuit to the cathode where reduction occurs. The electrolyte facilitates ion migration to maintain charge balance. Examples include zinc-carbon batteries (Zn → Zn²⺠+ 2e⻠at anode MnO₂ reduction at cathode) and lithium-ion batteries (LiCoO₂ cathode LiC₆ anode). All convert stored chemical energy directly into electrical energy without moving parts.
B) closed electric circuit
A closed circuit provides a conductive pathway for current flow but does not itself convert energy forms. It enables energy transfer from a source (like a battery) to a load (like a light bulb) but performs no energy transformation. The circuit is a conduit not an energy converter.
C) generator
Generators convert mechanical energy (rotation from turbines engines or other sources) into electrical energy through electromagnetic induction where conductors move through magnetic fields inducing current. Generators transform kinetic energy not chemical energy though the mechanical input might originate from chemical sources like burning fuel in a power plant.
D) transformer
Transformers change alternating current voltage levels through electromagnetic induction between primary and secondary coils but do not convert energy forms. They transfer electrical energy from one circuit to another with minimal loss changing voltage and current magnitudes while conserving power (ignoring small losses). No chemical energy conversion occurs in transformers.
Conclusion:
Batteries uniquely perform direct chemical-to-electrical energy conversion through spontaneous electrochemical reactions. Option A correctly identifies this energy transformation essential for portable power applications distinguishing batteries from circuits (that merely conduct electricity) generators (that convert mechanical energy) and transformers (that modify electrical characteristics without changing energy forms).
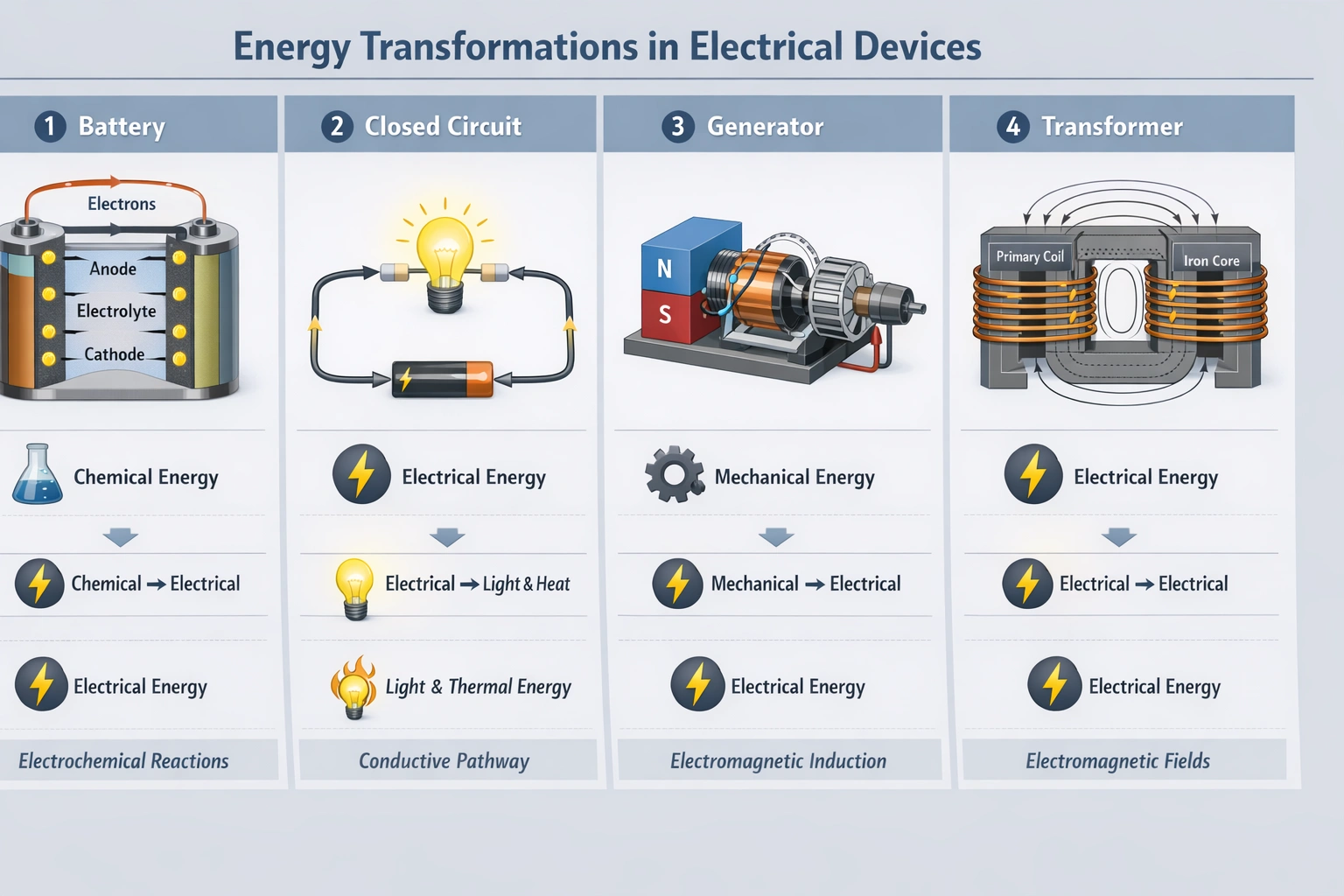
NEX Exams
NEX Quizzes
3 Practice Tests
NEX Quizzes
3 Practice Tests
NEX Quizzes
3 Practice Tests
NEX Quizzes
3 Practice Tests