ANATOMY AND PHYSIOLOGY HESI A2 PRACTICE TEST
This Anatomy and Physiology HESI A2 practice test helps you apply theoretical knowledge to exam-style scenarios. It emphasizes understanding how body systems work together, a common theme in HESI A2 questions.
Topics Covered
Organ Systems
Body Functions
System Interactions
Regulation and Control
00:00
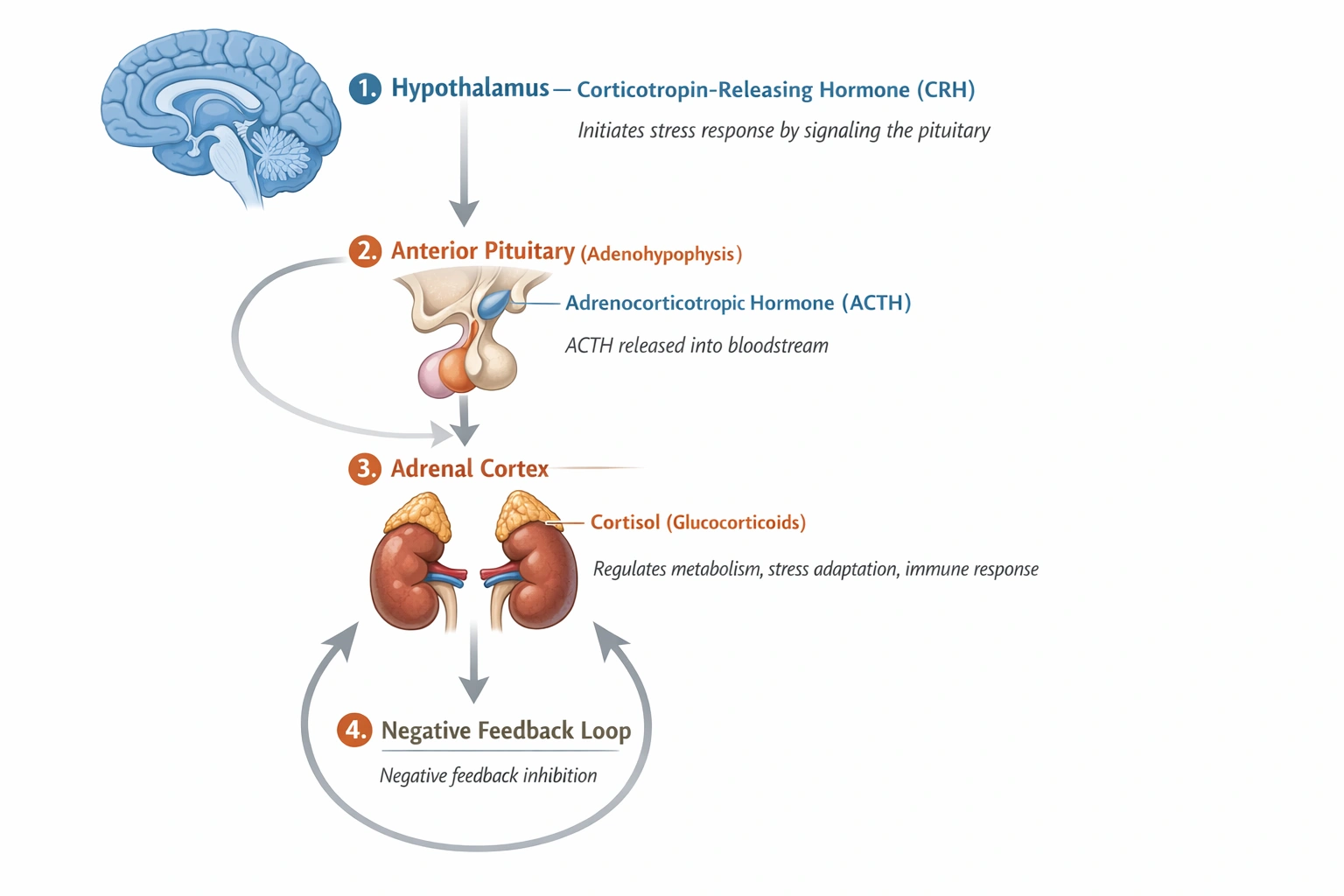
Which of the following glands produces the (ACTH)?
A.
adrenal gland
B. anterior lobe of the pituitary
C. hypothalamus
D. thyroid gland
Rationale
The anterior lobe of the pituitary gland produces the ACTH.
This hormone is synthesized as part of a larger precursor molecule called pro-opiomelanocortin (POMC). Its primary function is to stimulate the adrenal cortex to release glucocorticoids, mainly cortisol, which are critical for stress response and metabolism.
A. Adrenal gland
The adrenal glands are the target organ for ACTH, not its source. The adrenal cortex responds to ACTH stimulation by producing hormones like cortisol and aldosterone. Therefore, while intimately involved in the ACTH pathway, the adrenal glands do not produce ACTH themselves.
B. Anterior lobe of the pituitary
The anterior pituitary is the definitive producer of ACTH. It releases this tropic hormone into the bloodstream in response to stimulation by Corticotropin-Releasing Hormone (CRH) from the hypothalamus, forming a key axis in the body's endocrine regulation.
C. Hypothalamus
The hypothalamus plays a crucial regulatory role by producing Corticotropin-Releasing Hormone (CRH). CRH travels to the anterior pituitary via a specialized portal system to trigger the release of ACTH. However, the hypothalamus does not produce ACTH; it controls its secretion indirectly.
D. Thyroid gland
The thyroid gland produces thyroid hormones (T3 and T4), which regulate metabolism, growth, and development. It is not involved in the synthesis or secretion of ACTH, which is part of a entirely different hormonal axis (the hypothalamic-pituitary-adrenal axis).
Conclusion:
ACTH is synthesized and secreted specifically by the anterior lobe of the pituitary gland. It acts as a vital chemical messenger within the hypothalamic-pituitary-adrenal (HPA) axis to regulate the body's stress response.
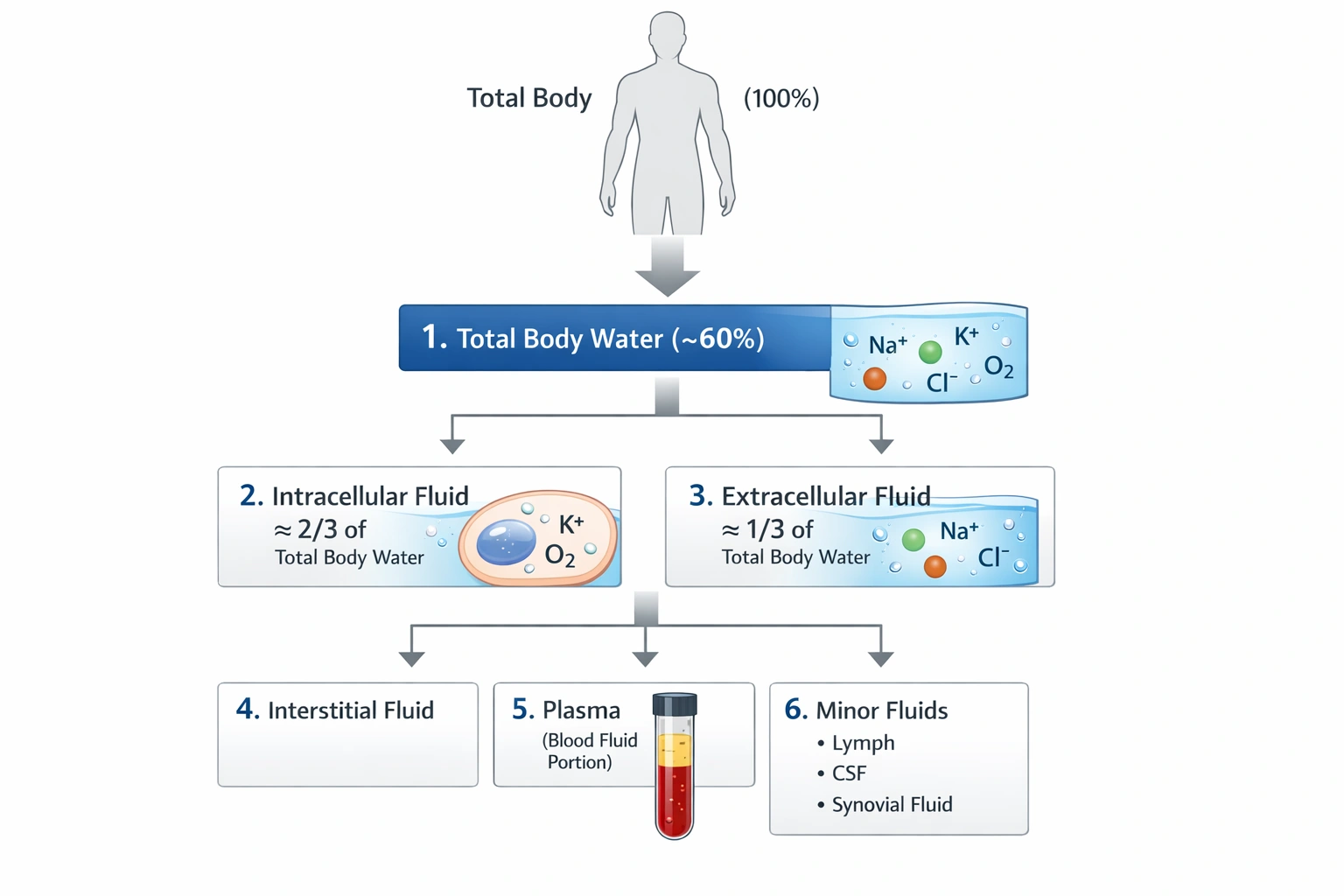
Body fluid is primarily
A.
blood
B. electrolytes
C. oxygen
D. water
Rationale
Body fluid is primarily water.
Body fluid refers to all the water‑based solutions within the body, including intracellular fluid (inside cells) and extracellular fluid (such as plasma, interstitial fluid, and transcellular fluid). Water constitutes approximately 50--60% of total adult body weight and serves as the essential solvent and medium for all biochemical reactions, nutrient transport, temperature regulation, and waste removal.
A) Blood
Blood is a specific and vital type of extracellular body fluid, composed of plasma and formed elements. However, the total volume of blood represents only a fraction of the body's total fluid content. Body fluid is a broader category that includes intracellular fluid, interstitial fluid, lymph, cerebrospinal fluid, and others. Therefore, blood is an important component but not the primary substance of body fluid as a whole.
B) Electrolytes
Electrolytes, such as sodium, potassium, and calcium ions, are essential solutes dissolved within body fluids. They are critical for nerve conduction, muscle contraction, and fluid balance. However, they are not the fluid itself. They are components dissolved in the primary solvent, which is water, and constitute a relatively small percentage of total body mass.
C) Oxygen
Oxygen is a dissolved gas that is transported within the blood plasma and bound to hemoglobin in red blood cells. It is a crucial element for cellular metabolism but is not a liquid component of the body. Body fluids are liquid in nature, whereas oxygen is a gaseous molecule carried within those fluids.
D) Water
Water is the principal chemical component of the human body and the base solvent for all body fluids. Intracellular fluid, the fluid inside cells, and extracellular fluid, which includes plasma and interstitial fluid, are all primarily water. This high water content facilitates nutrient transport, waste removal, and all biochemical reactions, establishing water as the foundational element of body fluids.
Conclusion:
While blood is a familiar body fluid, and electrolytes and oxygen are vital substances carried within body fluids, the fundamental and primary component of all body fluids is water. It is the essential solvent that defines the liquid environment of the human body.
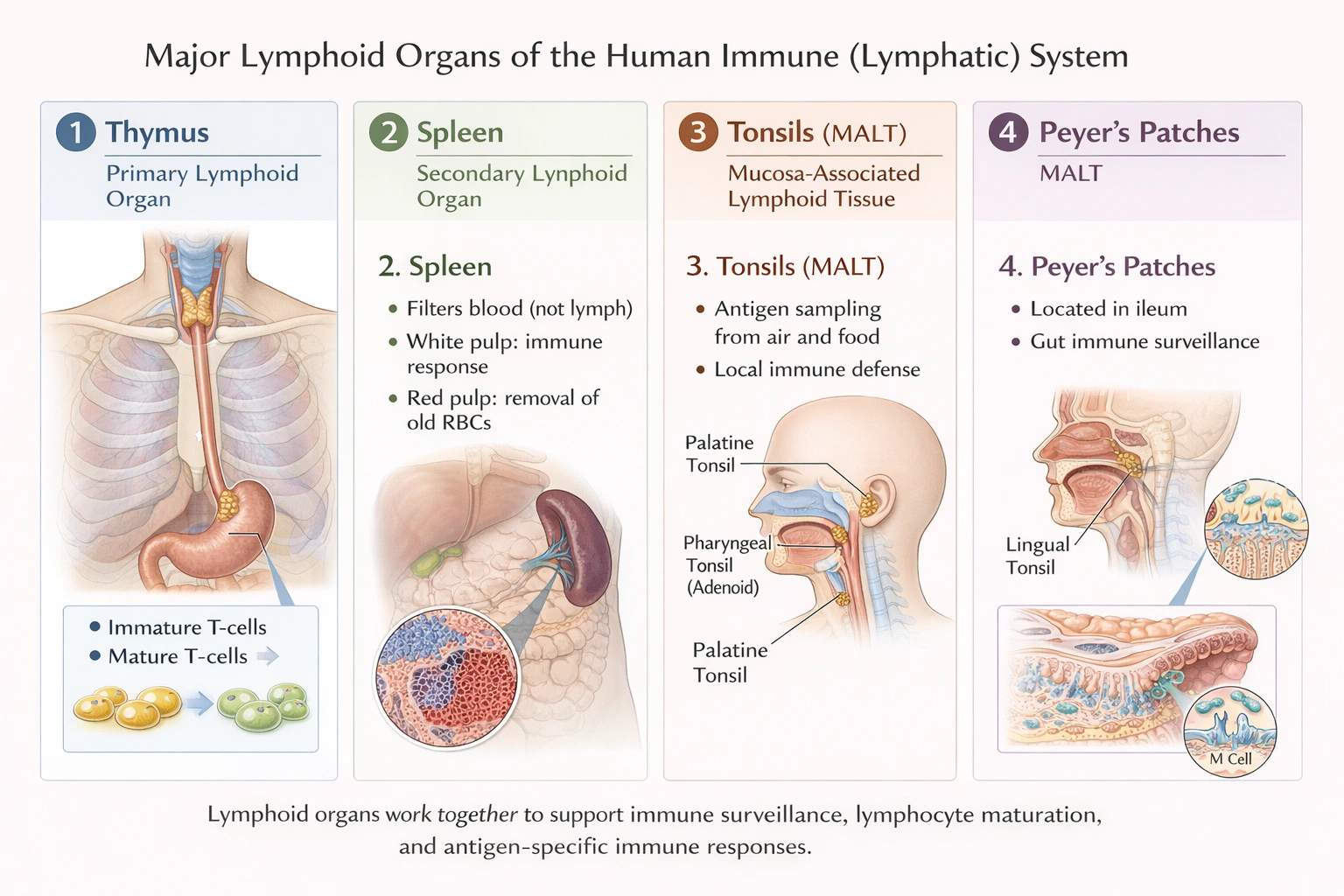
The thymus gland, areas of the spleen, tonsils, and Peyer's patches
A.
are found primarily in the inguinal and axillary areas
B. are organs of the lymph system
C. produce antibodies
D. secrete monocytes that transform into macrophages
Rationale
The thymus gland, spleen, tonsils, and Peyer's patches organs of the lymph system. This system is a network of organs, tissues, and vessels dedicated to immune defense and maintaining fluid balance. These specific structures, while diverse in location and specific function, are classified as primary or secondary lymphoid organs and tissues, forming an integrated network for lymphocyte development, activation, and immune response coordination.
A) Are found primarily in the inguinal and axillary areas
This statement inaccurately generalizes the anatomical location of these organs. While clusters of lymph nodes are indeed concentrated in the inguinal and axillary regions, the listed structures are distributed throughout the body. The thymus is located in the anterior mediastinum, behind the sternum. The spleen resides in the left upper quadrant of the abdomen. The tonsils are embedded in the mucosa of the oropharynx, and Peyer's patches are aggregates of lymphoid tissue found within the wall of the ileum, part of the small intestine. Therefore, they are not primarily located in the groin or armpit areas.
B) Are organs of the lymph system
Each structure listed is a fundamental component of the lymphatic or lymphoid system. The thymus is a primary lymphoid organ responsible for the maturation and selection of T lymphocytes. The spleen is a major secondary lymphoid organ that filters blood and houses lymphocytes for immune responses. The tonsils and Peyer's patches are critical examples of mucosa associated lymphoid tissue, serving as immune sentinel tissues at mucosal entry points in the digestive and respiratory tracts. Together, they represent key anatomical sites for immune function.
C) Produce antibodies
This statement is an oversimplification and not wholly accurate. Antibodies are secreted by plasma cells, which are derived from B lymphocytes. While secondary lymphoid tissues like the spleen, tonsils, and Peyer's patches provide the necessary environment for B cell activation and differentiation into antibody producing plasma cells, the organs themselves are not the producers. Furthermore, the thymus, a primary lymphoid organ, is involved exclusively in T cell development and does not contribute to antibody production at all. Thus, antibody secretion is a function of specific cells within some of these organs, not a defining function of the organs as a whole.
D) Secrete monocytes that transform into macrophages
This statement is incorrect regarding the origin of monocytes. Monocytes are a type of white blood cell produced and released by the bone marrow. These cells circulate in the bloodstream before migrating into various tissues where they differentiate into resident macrophages. The listed lymphoid organs, including the spleen, may contain macrophages and provide sites for monocyte differentiation, but they are not the source of monocyte production or secretion. That role is exclusive to the bone marrow.
Conclusion:
The question presents a group of anatomically distinct structures linked by their common classification within the body's defense and maintenance network. Their unifying characteristic is that they are all integral organs or organized tissues of the lymphatic system. Therefore, the correct answer is that they are organs of the lymph system.
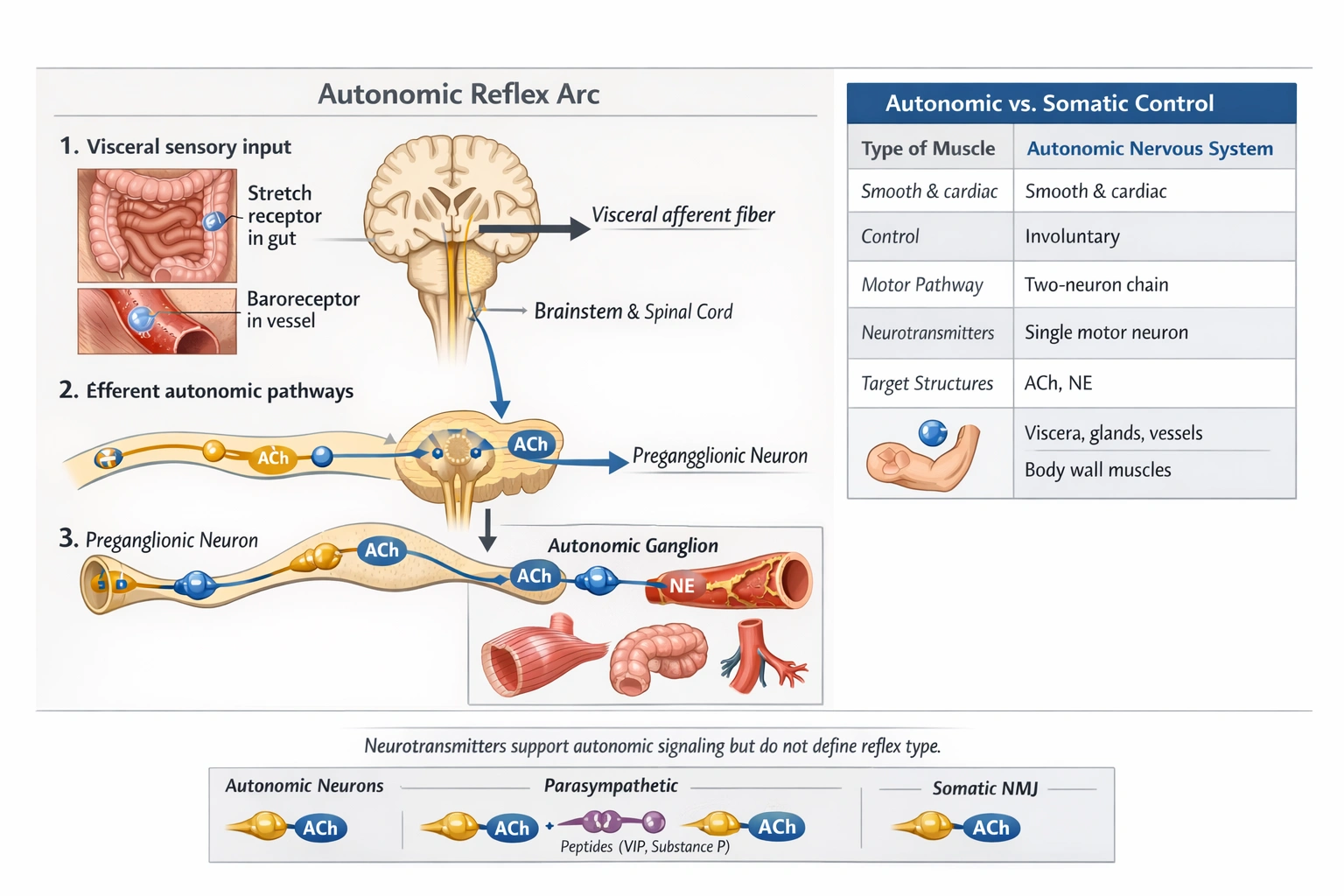
Which of the following regulates activity of smooth muscles?
A.
acetylcholine reflexes
B. autonomic reflexes
C. neuropeptide reflexes
D. somatic reflexes
Rationale
Autonomic reflexes are the regulatory mechanisms that control the activity of smooth muscles.
These involuntary, homeostatic responses are mediated by the autonomic nervous system, which maintains internal balance through subconscious feedback loops. Smooth muscle, found in the walls of hollow organs like the digestive tract, blood vessels, and bladder, is innervated by autonomic motor neurons. Reflex arcs in this system integrate sensory input from visceral receptors and produce automatic motor output to adjust muscle tone, contraction, and organ function without conscious effort.
A) Acetylcholine reflexes
This is not a standard physiological classification of reflexes. Acetylcholine is a key neurotransmitter used in many parts of the nervous system, including both the autonomic and somatic divisions. It is released by all parasympathetic postganglionic neurons and some sympathetic neurons. While many autonomic reflexes involve cholinergic synapses, reflexes are defined by their neural pathways and functions, not by the specific neurotransmitter employed. Therefore, this term is overly narrow and misleading.
B) Autonomic reflexes
The autonomic nervous system, through its sympathetic and parasympathetic divisions, exclusively governs the involuntary regulation of smooth muscle, cardiac muscle, and glands. Autonomic reflexes are unconscious feedback loops that maintain homeostasis. For example, the baroreceptor reflex adjusts blood vessel tone to regulate pressure, and the gastrocolic reflex coordinates smooth muscle contractions in the digestive tract for peristalsis. These reflexes involve sensory signals from internal organs, integration in the brainstem or spinal cord, and motor output via autonomic nerves to smooth muscle tissue.
C) Neuropeptide reflexes
This is not a recognized category of neural reflexes. Neuropeptides, such as substance P or vasoactive intestinal peptide, are signaling molecules that often act as neuromodulators or co-transmitters within the nervous system. They can influence pain perception, inflammation, and local blood flow, and may modulate autonomic activity. However, the fundamental architecture for regulating smooth muscle is built around autonomic reflex arcs, not reflexes defined by a specific class of chemical messengers.
D) Somatic reflexes
Somatic reflexes pertain to the somatic nervous system, which controls voluntary skeletal muscles. These are rapid, involuntary motor responses to external stimuli, such as the stretch reflex that causes a knee jerk. The efferent pathway of a somatic reflex involves a single motor neuron that directly innervates skeletal muscle at the neuromuscular junction. This system does not innervate or control smooth muscle, which is entirely under autonomic regulation.
Conclusion:
Smooth muscle, responsible for critical involuntary functions in internal organs, is regulated by subconscious feedback mechanisms of the autonomic nervous system. These autonomic reflexes integrate sensory information from within the body to automatically adjust muscle activity, ensuring physiological stability. The correct answer is therefore autonomic reflexes.
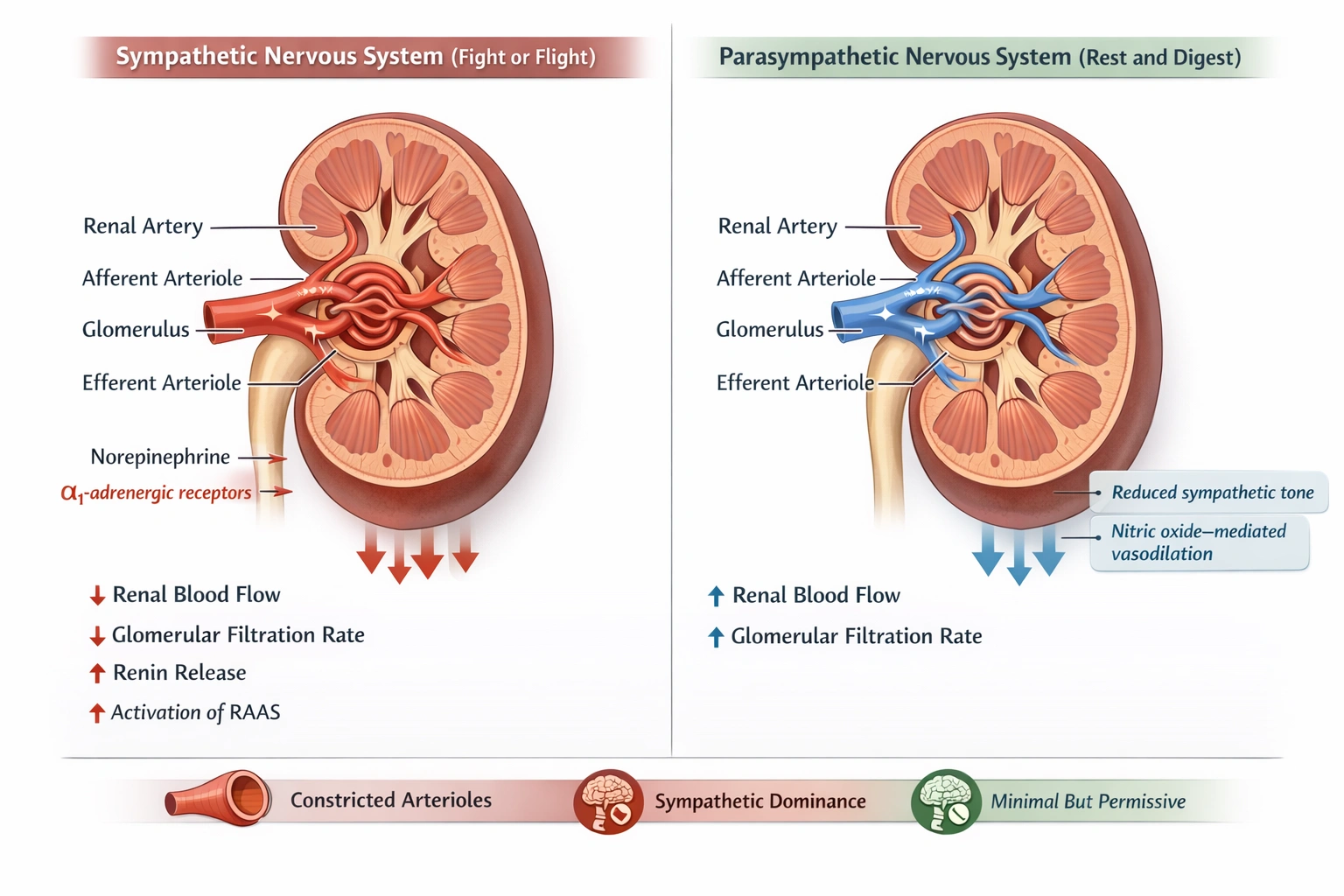
Renal system nerve fibers regulate blood flow. Sympathetic fibers __________ and parasympathetic fibers __________.
A.
constrict arterioles, dilate arterioles
B. dilate arterioles, constrict arterioles
C. constrict venules, dilate venules
D. dilate venules, constrict venules
Rationale
In the renal system, sympathetic nerve fibers constrict arterioles, while parasympathetic fibers promote arteriolar dilation.
This opposing control mechanism regulates renal blood flow and glomerular filtration in response to the body's physiological needs. Sympathetic activation, often during stress or low blood pressure, causes vasoconstriction to reduce flow and trigger hormonal responses, whereas parasympathetic activity supports a baseline state of vasodilation and increased perfusion.
A) Constrict arterioles, dilate arterioles
Sympathetic fibers release norepinephrine, which binds to alpha-1 adrenergic receptors on the smooth muscle of renal arterioles (both afferent and efferent), causing potent vasoconstriction. This reduces renal blood flow and glomerular filtration rate and stimulates the renin-angiotensin-aldosterone system. Parasympathetic influence, though less direct, promotes vasodilation, often by reducing sympathetic tone or releasing vasodilatory substances, thereby increasing renal blood flow.
B) Dilate arterioles, constrict arterioles
This reverses the established physiological roles of the autonomic nervous system. Sympathetic activation does not cause renal arteriolar dilation; its primary vascular effect in the kidney is constriction. Parasympathetic fibers are not known to cause arteriolar constriction in this context. This option is anatomically and functionally incorrect.
C) Constrict venules, dilate venules
This option incorrectly shifts the focus from arterioles to venules. While autonomic nerves can influence venous tone, the primary regulation of renal blood flow and filtration occurs at the arteriolar level. The afferent and efferent arterioles are the key resistance vessels controlling glomerular pressure. Venular control is more relevant to systemic venous return, not the precise regulation of renal perfusion.
D) Dilate venules, constrict venules
This is incorrect for two reasons. First, it focuses on venules instead of the arterioles that are the main site of renal blood flow regulation. Second, it misassigns the autonomic functions: sympathetic activation typically causes venoconstriction (not dilation) to increase venous return, while parasympathetic effects on venules are minimal and not primarily constrictive.
Conclusion:
The autonomic nervous system exerts precise control over kidney function by targeting arteriolar smooth muscle. Sympathetic stimulation constricts these vessels to reduce renal blood flow, while parasympathetic activity facilitates dilation to enhance it, making the constrict/dilate pairing the correct description of their roles.
Life is best defined in terms of
A.
breathing and respiration
B. functions performed by all living things
C. movement of fluid and other materials throughout the organism
D. processes included with ingestion and digestion
Rationale
Life is best defined by the set of fundamental functions performed by all living things.
This definition encompasses the essential processes that distinguish living entities from non-living matter, focusing on properties such as cellular organization, metabolism, homeostasis, growth, reproduction, response to stimuli, and the capacity for adaptation through evolution. A definition based on these universal functions is scientifically robust because it includes every known form of life, from bacteria and archaea to plants, fungi, and animals, regardless of their specific structures or environmental niches.
A) Breathing and respiration
This definition is incorrect because it is far too specific and excludes a vast diversity of life. Breathing, as a mechanical process of gas exchange, is only present in certain complex animals. Respiration, in the biochemical sense of aerobic energy production, is also not universal. Many organisms, such as anaerobic bacteria and archaea, thrive without oxygen and utilize alternative metabolic pathways like fermentation or anaerobic respiration. Therefore, using these processes as a definition would incorrectly classify entire domains of life as non-living.
B) Functions performed by all living things
Life is defined by a common suite of functions and characteristics that all living systems exhibit. These include the ability to maintain homeostasis, to metabolize energy, to grow and develop, to reproduce and pass on genetic information, to respond to environmental stimuli, and to evolve over time. This functional definition is inclusive, applying equally to a single-celled amoeba, a redwood tree, and a human being.
C) Movement of fluid and other materials throughout the organism
This describes internal transport systems, which are necessary for large, multicellular organisms to distribute nutrients and remove wastes. However, it is not a defining feature of all life. Unicellular organisms and simple multicellular life forms rely entirely on diffusion across cell membranes for exchange and do not possess circulatory systems. Consequently, this characteristic is a specialization of certain complex body plans, not a universal criterion for life.
D) Processes included with ingestion and digestion
These processes are specific to heterotrophic nutrition, where organisms consume and break down organic matter. They do not apply to autotrophs, such as plants, algae, and many bacteria, which produce their own nutrients through photosynthesis or chemosynthesis. Since a major portion of the living world does not ingest or digest food, this definition fails to encompass all forms of life.
Conclusion:
A valid definition of life must apply to every organism without exception. Defining life solely by processes like breathing, internal transport, or ingestion is exclusionary and fails to capture the true essence of living systems. The only accurate approach is to define life in terms of the fundamental, shared functions that collectively sustain and perpetuate biological organization.

Which of the following is TRUE regarding cellular organization?
A.
Living matter is always divided into small units known as cells
B. Cells vary in size, shape, and function, yet all have important characteristics in common
C. Cell response time and duration varies slowly over time
D. All members of one species of cell in one region of the body have similar characteristics
Rationale
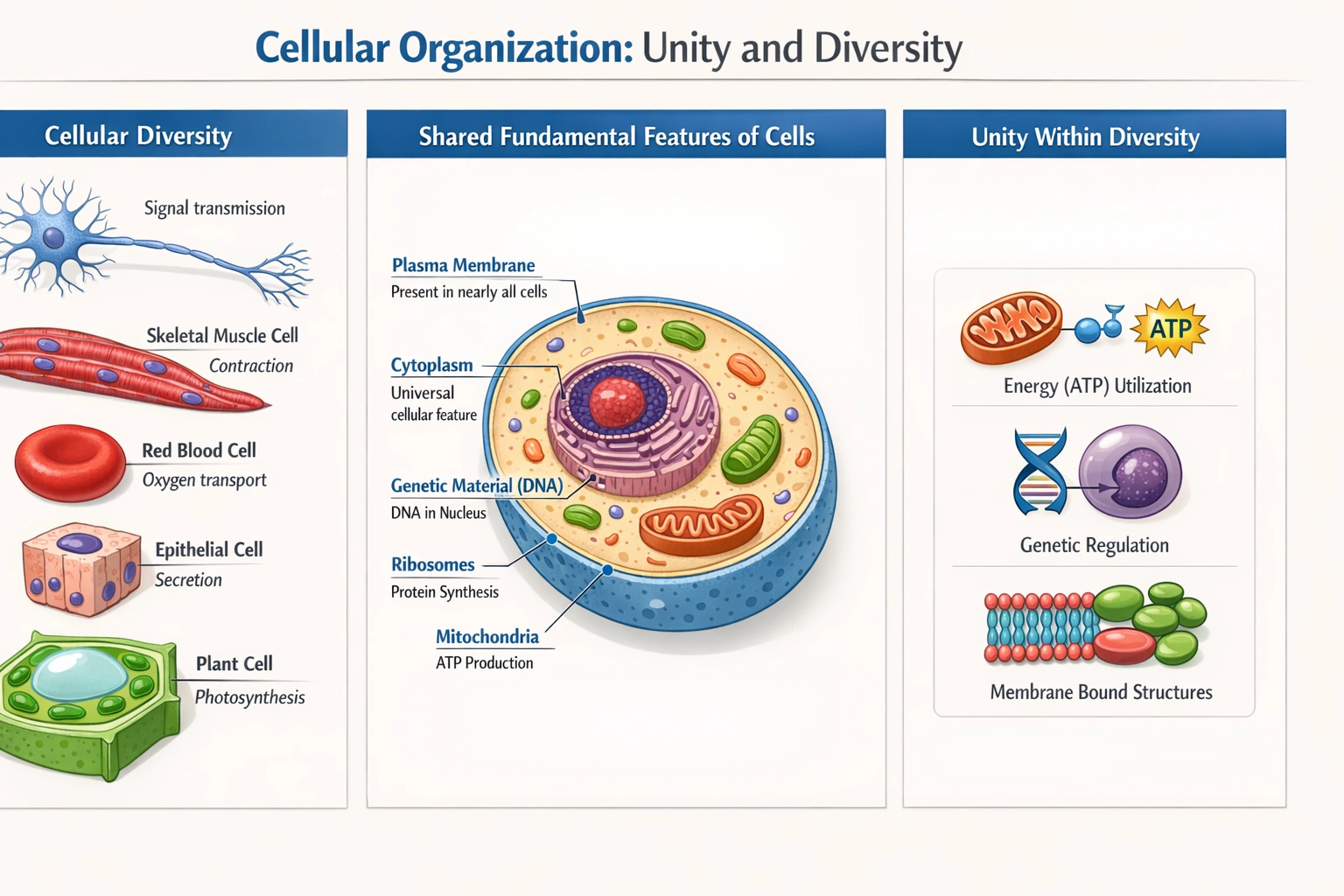
Cells vary in size, shape, and function, yet all have important characteristics in common.
This principle of "unity within diversity" is a cornerstone of cell biology, acknowledging that while a neuron, a red blood cell, and a plant cell appear and act differently, they all operate under the same basic biochemical and organizational rules.
A) Living matter is always divided into small units known as cells
This statement is an oversimplification of the Cell Theory. While it is true that all living organisms are composed of cells, the phrasing "living matter is always divided" can be misleading. First, viruses often considered non-living entities are not cellular. More importantly, within complex organisms, there are structures like syncytia (e.g., skeletal muscle fibers or the syncytiotrophoblast in the placenta) where multiple nuclei exist within a single, continuous mass of cytoplasm not divided into individual cells by membranes. These exceptions mean that living organization is not always neatly packaged into discrete, separate cellular units, though the cell remains the basic structural and functional unit of life.
B) Cells vary in size, shape, and function, yet all have important characteristics in common
This is the correct and most comprehensive statement. Cellular diversity is immense:
- Size: Ranges from bacterial cells like Mycoplasma (0.1 micrometers) to single cells like an ostrich egg (over 15 centimeters).
- Shape: Includes spherical white blood cells, disk-shaped red blood cells, branching neurons, columnar gut epithelial cells, and flat squamous cells.
- Function: Encompasses contraction (muscle cells), electrical signaling (neurons), oxygen transport (erythrocytes), photosynthesis (plant mesophyll cells), and antibody production (plasma cells).
Despite this diversity, all cells share universal features: a plasma membrane that encloses the cytoplasm, genetic material (DNA) that directs cellular activities, ribosomes for protein synthesis, and the use of adenosine triphosphate (ATP) as an energy currency. This balance of variety and unity is a foundational concept in biology.
C) Cell response time and duration varies slowly over time
This statement is incorrect and biologically unsupported. Cellular response times are not governed by a universal principle of gradual change. Instead, they are highly specific and depend on the stimulus, the signaling pathway involved, and the cell type. A neuron can generate an action potential in milliseconds, a pancreatic beta cell may secrete insulin over minutes in response to glucose, and a cell undergoing differentiation might change its gene expression profile over days or weeks. There is no inherent, slow temporal drift in response dynamics; each response is precisely tuned to its physiological purpose.
D) All members of one species of cell in one region of the body have similar characteristics
This is an overgeneralization. While cells of the same type within a tissue often share a broad classification, significant functional and molecular heterogeneity frequently exists. For example, hepatocytes (liver cells) exhibit "zonation": cells in the periportal region of the liver lobule are specialized for processes like gluconeogenesis, while those in the perivenous region are more involved in glycolysis and detoxification. Similarly, fibroblasts in different connective tissue regions or macrophages in different organs can have distinct functional profiles based on their local microenvironment. Therefore, even within one cell type in a specific region, individual cells can have important specialized characteristics.
Conclusion:
Cellular organization is best understood through the lens of both diversity and commonality. The only statement that fully captures this essential biological truth is that cells, despite vast differences in their form and function, are united by a core set of structural and metabolic features fundamental to all life.
__________ controls the functions of cells.
A.
Autonomic nervous system
B. Thyroid gland
C. Hormones
D. Metabolism
Rationale
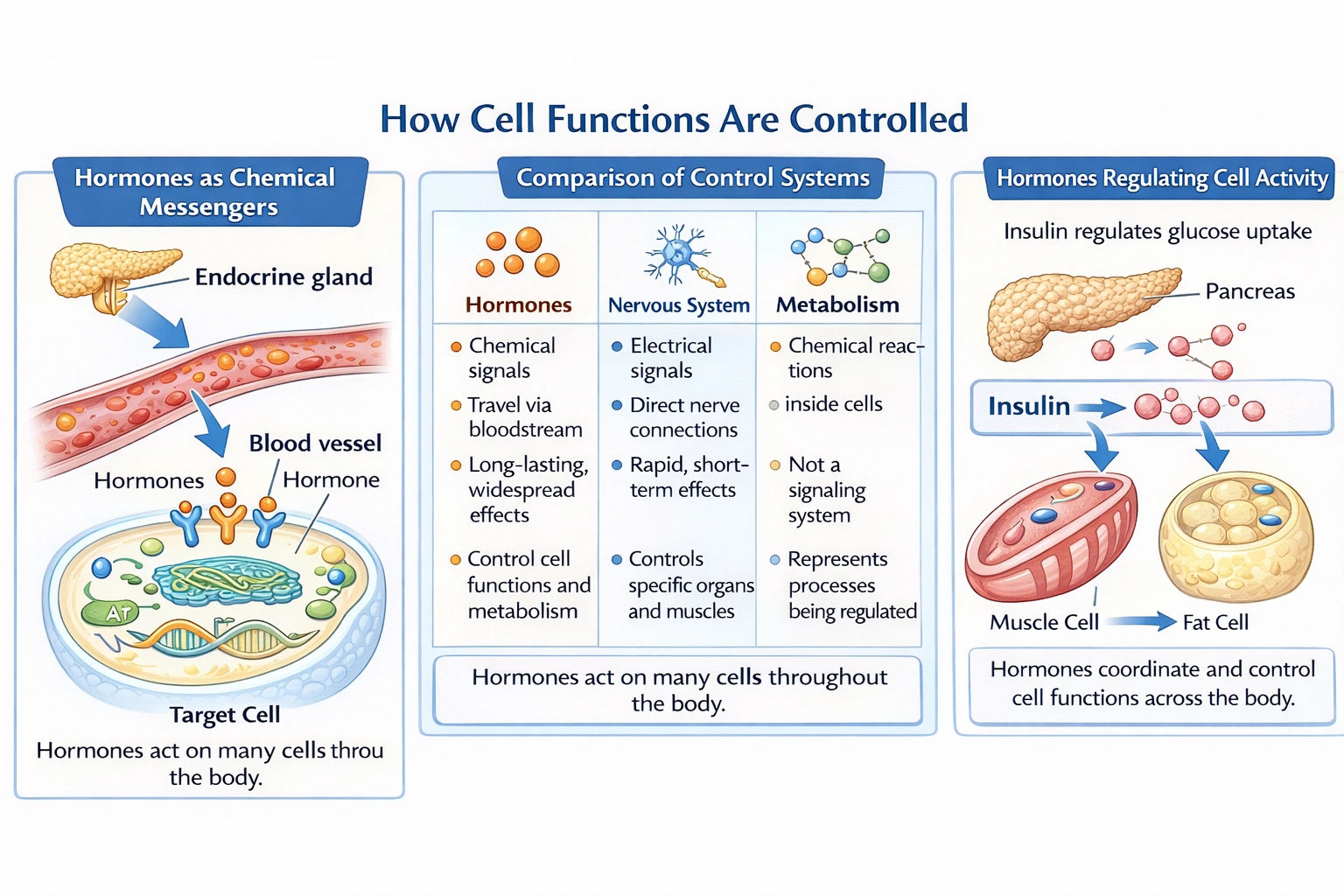
Hormones are chemical messengers secreted by glands and tissues directly into the bloodstream.
They travel throughout the body and bind to specific receptors on or within target cells. This binding initiates cellular changes that regulate a vast array of functions, including metabolism, growth, reproduction, mood, and homeostasis. While other options like the autonomic nervous system provide rapid, specific regulatory signals, and specific glands like the thyroid are sources of hormones, the general and comprehensive control of cellular function is achieved through the diverse and integrated system of hormonal signaling.
(A) Autonomic nervous system primarily controls involuntary physiological processes like heart rate and digestion through direct neural connections. Its control is rapid and specific to innervated tissues, but it does not govern the broad, long-term biochemical functions of all cells in the way hormones do.
(B) Thyroid gland is one specific endocrine organ that produces hormones (T3 and T4) crucial for regulating metabolism. However, it is only one source of hormonal control. Cellular functions are coordinated by many hormones from various glands (e.g., insulin from the pancreas, cortisol from adrenals), not by a single gland.
(D) Metabolism is the collective term for all chemical reactions within a cell. It is the process that is controlled, not the controller itself. Hormones are key regulators that direct the rate and pathways of metabolic activity.
Conclusion:
While the autonomic nervous system provides rapid neural control and specific glands like the thyroid produce important regulatory hormones, it is the broad category of hormones that serves as the fundamental chemical signaling system for integrating and controlling the diverse functions of cells across the entire organism.
The follicle stimulating hormone (FSH) induces which of the following in males?
A.
excitation of smooth muscles in the genitalia
B. inactivation of spermatogenesis
C. regulation of bulbourethral gland fluid
D. stimulation of seminiferous tubules of the testes
Rationale
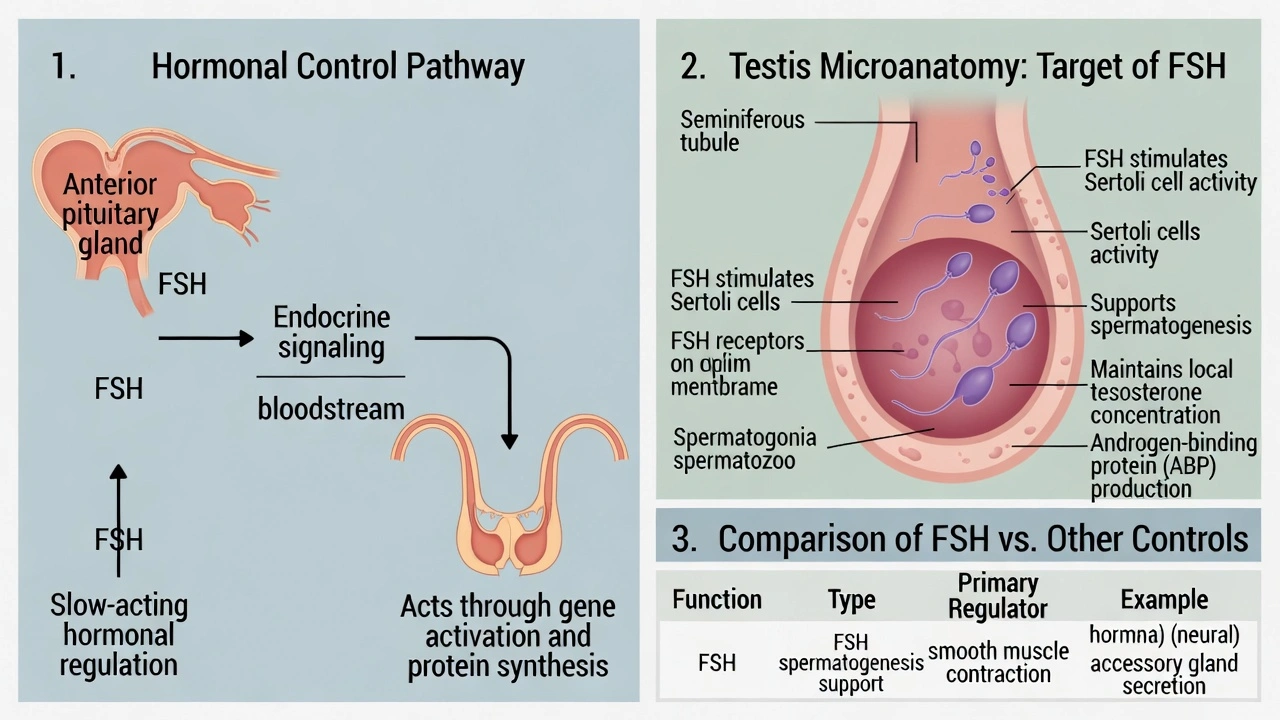
Follicle-stimulating hormone (FSH) in males induces stimulation of the seminiferous tubules of the testes.
In males, FSH is a glycoprotein hormone secreted by the anterior pituitary gland. Its primary target is the seminiferous tubules within the testes, where it binds to receptors on Sertoli cells. FSH promotes Sertoli cell function, including the production of androgen‑binding protein (ABP) and other supportive factors, thereby creating a local environment essential for the initiation, maintenance, and regulation of spermatogenesis.
A. excitation of smooth muscles in the genitalia
This function is governed by the autonomic nervous system, not by FSH. Smooth muscle contraction in structures such as the vas deferens, prostate, and erectile tissue of the penis is mediated by neurotransmitters. For example, parasympathetic stimulation leads to vasodilation and erection via nitric oxide release, while sympathetic stimulation triggers emission and ejaculation. These are rapid, nerve-mediated events. FSH, in contrast, is a slow-acting endocrine hormone whose effects occur over hours to days through gene activation and protein synthesis. Its receptors are not found on smooth muscle cells, and it plays no part in the direct excitation of genital muscles.
B. inactivation of spermatogenesis
This statement directly contradicts the established physiological role of FSH. FSH is a critical activator and sustainer of spermatogenesis. Its action on Sertoli cells creates the necessary microenvironment within the seminiferous tubules for germ cell survival and maturation. Inactivation or failure of spermatogenesis typically results from a deficiency of FSH, interference with its action, or from the negative feedback effects of hormones like inhibin (which is produced by Sertoli cells in response to FSH to regulate pituitary secretion). Therefore, FSH promotes, not inactivates, sperm production.
C. regulation of bulbourethral gland fluid
The bulbourethral glands (Cowper's glands) are accessory reproductive glands whose primary function is to secrete a clear, alkaline mucus during sexual arousal. This secretion lubricates the urethra and neutralizes any residual acidic urine. The process is primarily under neural control, triggered by parasympathetic nerve signals in response to tactile or psychological stimulation. The glands do not possess receptors for FSH, and their secretory activity is independent of pituitary gonadotropins. FSH's role is restricted to testicular function and does not extend to regulating the secretory activity of accessory sex glands.
D. stimulation of seminiferous tubules of the testes
This is the precise and correct function of FSH in males. The seminiferous tubules are the sperm-producing factories of the testes. FSH acts directly on these tubules by binding to FSH receptors on the cytoplasmic membranes of Sertoli cells. This stimulation causes Sertoli cells to synthesize and secrete androgen-binding protein (ABP), which maintains a high local concentration of testosterone---a hormone also vital for spermatogenesis. Furthermore, FSH promotes Sertoli cell function in nurturing developing sperm cells through all stages of spermatogenesis, from spermatogonia to spermatozoa. This action is fundamental to male fertility.
Conclusion:
The principal and defining action of Follicle-Stimulating Hormone in the male reproductive system is the stimulation of the seminiferous tubules within the testes to support and maintain sperm production. This endocrine function is distinct from the neural mechanisms controlling sexual response and glandular secretion. A clear understanding of FSH's specific target and action is crucial in reproductive physiology and in diagnosing conditions related to male infertility.
Prolactin (PRL) targets/stimulates
A.
female mammary glands.
B. production of testosterone by the testes.
C. suppression of milk production prior to birth.
D. uterine contractions.
Rationale
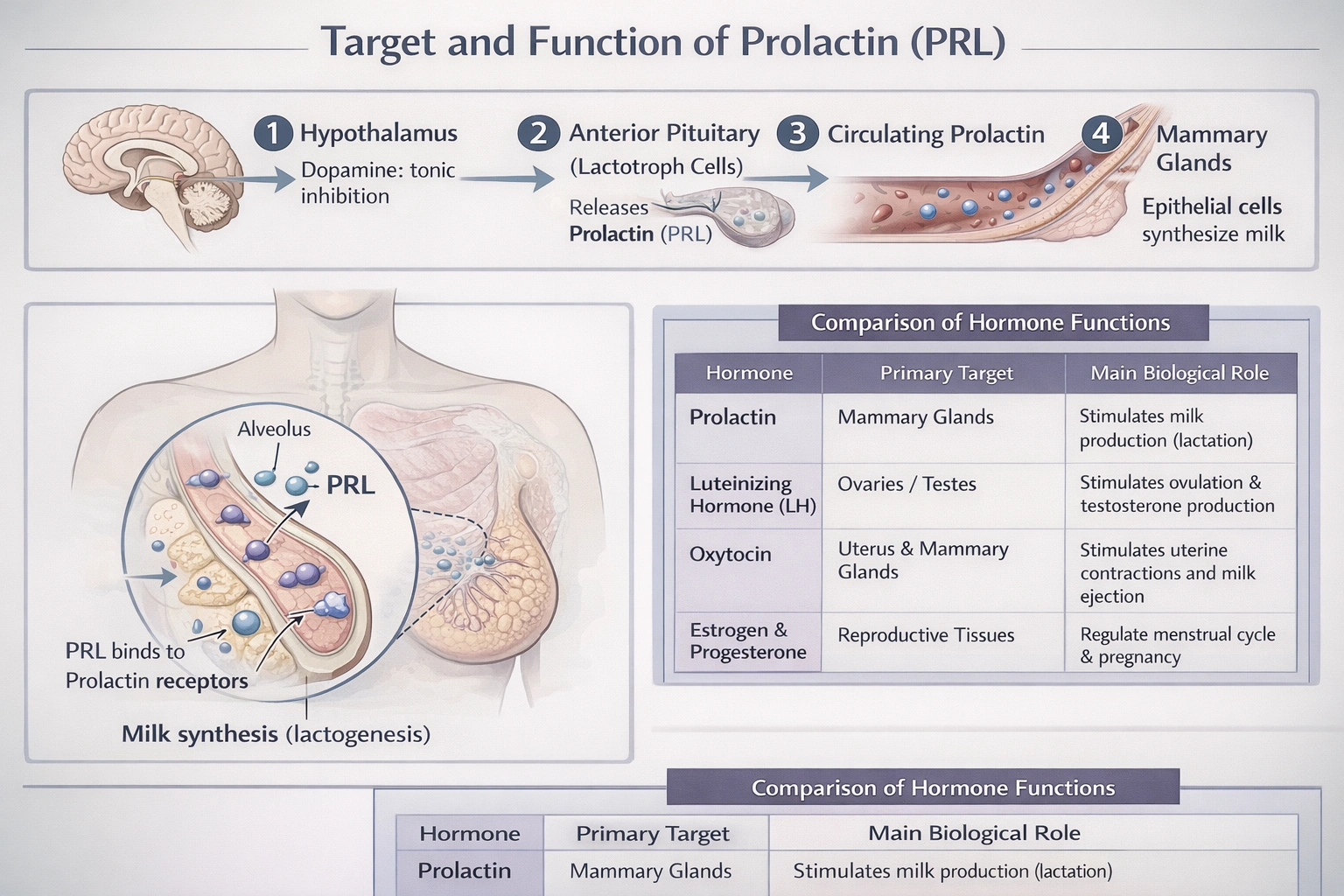
Prolactin (PRL) targets and stimulates the female mammary glands. This anterior pituitary hormone is essential for mammary gland development (mammogenesis) during pregnancy and is the primary hormonal driver of milk synthesis (lactogenesis) postpartum. Prolactin secretion is tonically inhibited by dopamine from the hypothalamus and is stimulated by factors such as thyrotropin-releasing hormone (TRH) and, most potently, by the suckling reflex via neural pathways that inhibit dopamine release.
A. female mammary glands.
Prolactin binds to specific transmembrane receptors on alveolar epithelial cells in the mammary glands, activating JAK-STAT signaling pathways. This stimulates the transcription of genes for milk proteins (casein, lactalbumin), lipids, and lactose. During pregnancy, rising estrogen levels stimulate lactotroph hyperplasia, increasing prolactin secretion, but high estrogen and progesterone levels inhibit prolactin's action at the alveolar level. After parturition, the drop in these steroids allows prolactin to fully initiate lactation, which is then maintained by the neuroendocrine suckling reflex.
B. production of testosterone by the testes.
Testosterone production by Leydig cells is primarily regulated by luteinizing hormone (LH). Prolactin receptors exist in the testes, and normal levels may support Leydig cell function, but prolactin is not a direct stimulator. Pathologically elevated prolactin (hyperprolactinemia) suppresses hypothalamic gonadotropin-releasing hormone (GnRH) pulse frequency, leading to reduced LH and FSH secretion. This results in secondary hypogonadism, characterized by low testosterone and impaired spermatogenesis, demonstrating an inhibitory, not stimulatory, role.
C. suppression of milk production prior to birth.
Lactation is suppressed during pregnancy by the high circulating levels of estrogen and progesterone produced by the placenta. These steroids competitively inhibit prolactin binding to its receptor and block downstream signaling in mammary alveolar cells. Prolactin levels are actually high during pregnancy, preparing the breast for lactation, but its effector pathway is pharmacologically blocked. The suppression is lifted physiologically once the placenta is delivered and steroid levels plummet.
D. uterine contractions.
Uterine contractions during labor (parturition) and the milk ejection reflex (let-down) are mediated by the posterior pituitary hormone oxytocin. Oxytocin acts on Gq-protein-coupled receptors in the myometrium and on myoepithelial cells surrounding mammary alveoli. While prolactin and oxytocin are both involved in reproduction, their functions are sequential and distinct: prolactin governs the production of milk, while oxytocin governs the ejection of milk and uterine motility.
Conclusion:
Prolactin's definitive and primary target is the female mammary gland, where it directly regulates the biochemical synthesis of milk. Its role is often misconstrued with other reproductive hormones, but it is specific to lactogenesis. The other options describe functions of other hormonal systems gonadotropins for
testosterone, placental steroids for prenatal inhibition, and oxytocin for muscular contractions.
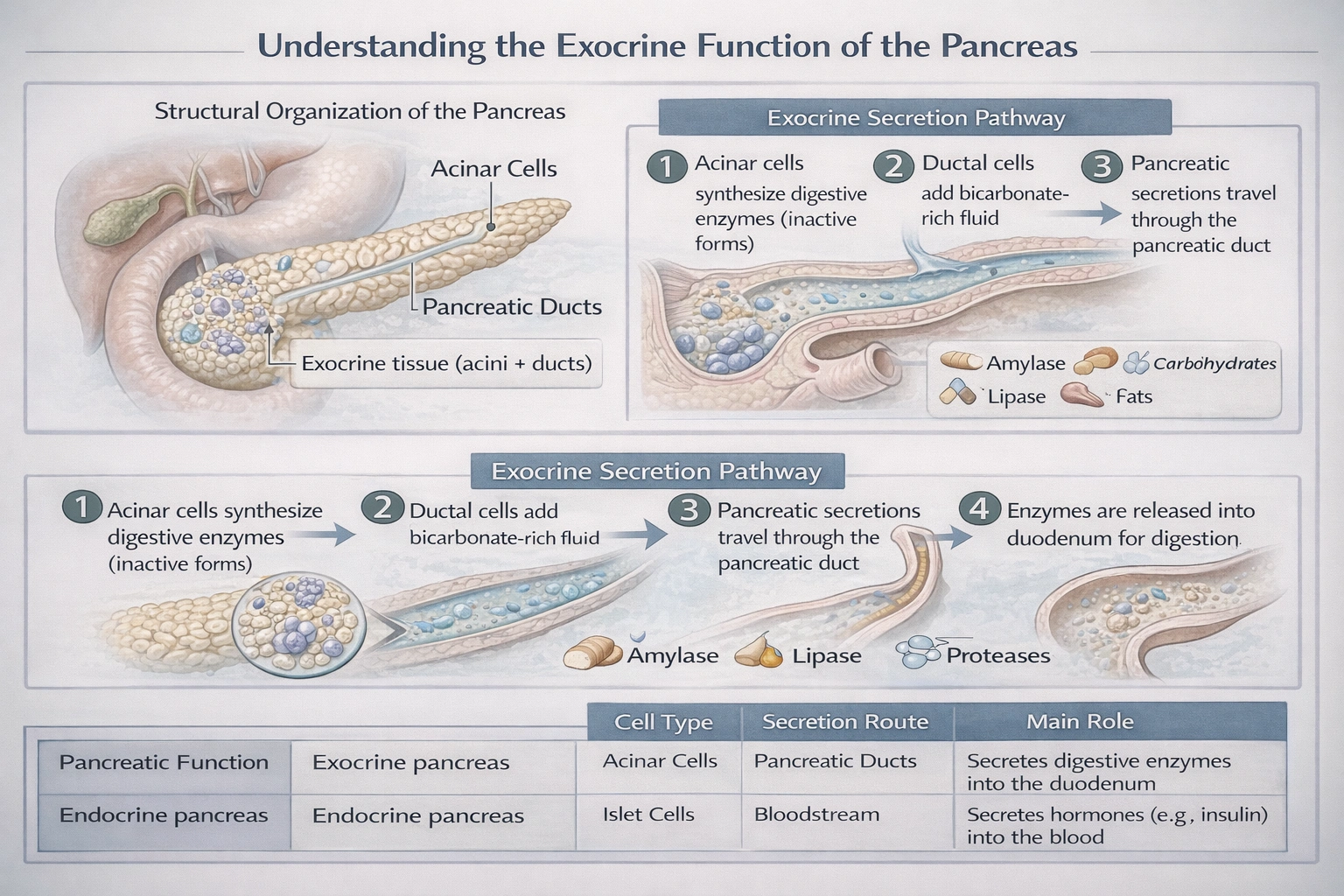
The exocrine function of the pancreas
A.
controls delta cells in the Islets of Langerhans.
B. controls osteoclasts.
C. produces insulin.
D. secretes pancreatic digestive enzymes.
Rationale
The exocrine function of the pancreas is to secrete digestive enzymes into the gastrointestinal tract.
This is accomplished by the acinar cells, which synthesize and store potent enzymes, and the ductal cells, which secrete a bicarbonate-rich fluid. Together, these secretions travel through the pancreatic duct to the duodenum, where they play an essential role in breaking down carbohydrates, fats, and proteins in ingested food.
A. controls delta cells in the Islets of Langerhans.
Delta cells are endocrine cells within the pancreatic islets that produce somatostatin, a hormone that locally inhibits the release of insulin and glucagon. The exocrine pancreas, composed of acini and ducts, is structurally and functionally separate from the endocrine islets. Exocrine secretions are directed into ducts, not the bloodstream, and do not exert regulatory control over endocrine cells. Endocrine cell regulation is governed by blood glucose levels, autonomic nerves, and hormonal signals.
B. controls osteoclasts.
Osteoclasts are bone-resorbing cells regulated by hormones such as parathyroid hormone (PTH) and calcitonin, and by local factors like RANK ligand. The pancreas, whether exocrine or endocrine, has no known physiological role in osteoclast formation or activity. Bone metabolism is outside the functional scope of pancreatic physiology.
C. produces insulin.
Insulin is a peptide hormone produced by the beta cells of the pancreatic islets, which are part of the endocrine pancreas. Its secretion into the bloodstream regulates blood glucose levels. The exocrine pancreas, in contrast, secretes its products into a ductal system leading to the gut. Insulin production is a classic endocrine function, not an exocrine one.
D. secretes pancreatic digestive enzymes.
This is the definitive function of the exocrine pancreas. Acinar cells synthesize and secrete enzymes such as pancreatic amylase (for starch), lipase (for triglycerides), and proteases like trypsinogen (for proteins). These enzymes are released in an inactive form to prevent autodigestion and become activated in the duodenum. This exocrine secretion is vital for complete macronutrient digestion.
Conclusion:
The exocrine pancreas functions as a digestive gland, secreting enzymes essential for intestinal digestion. Its role is entirely separate from the endocrine functions of the pancreatic islets, which include insulin production and the regulation of other endocrine cells.
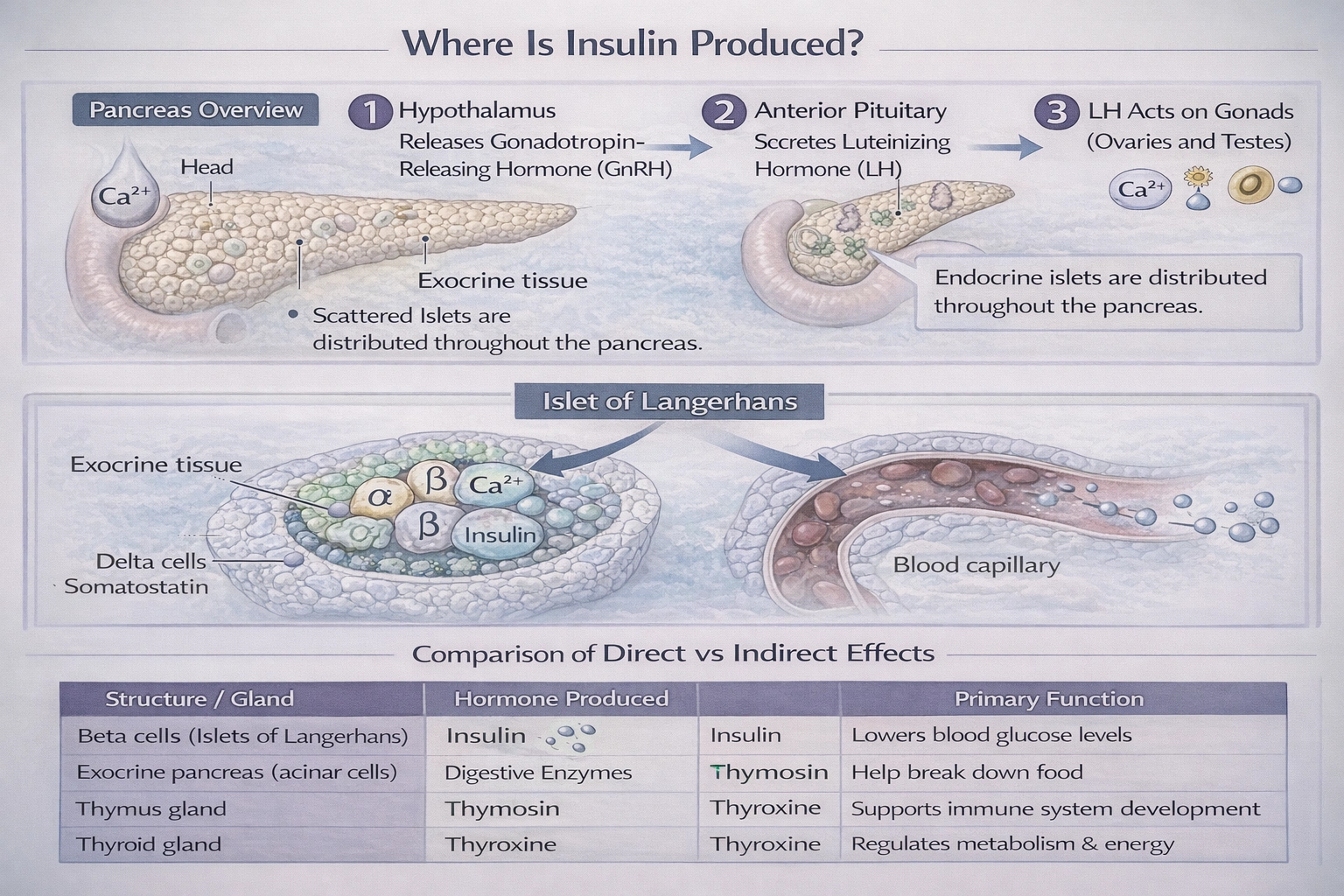
Insulin is produced in the
A.
anterior portion of the pancreas.
B. beta cells of the Islets of Langerhans.
C. thymus gland.
D. posterior lobe of the thyroid gland.
Rationale
Insulin is produced in the beta cells of the Islets of Langerhans.
Insulin is a peptide hormone essential for regulating blood glucose levels.
It is synthesized, stored, and secreted by the beta cells (β-cells), which are one of several endocrine cell types located within the Islets of Langerhans in the pancreas. These islets are scattered throughout the pancreatic tissue and function as the endocrine portion of the pancreas, with beta cells specifically responsible for insulin production in response to elevated blood glucose.
A. anterior portion of the pancreas.
The pancreas is not functionally divided into anterior and posterior regions with respect to hormone production. The Islets of Langerhans, which house insulin-producing beta cells, are distributed throughout the entire gland, though they may be more concentrated in the tail. Insulin synthesis is a microscopic, cellular function that does not correspond to a gross "anterior portion" of the organ, making this description anatomically misleading.
B. beta cells of the Islets of Langerhans.
The Islets of Langerhans are distinct endocrine micro-organs scattered within the exocrine tissue of the pancreas. Beta cells constitute approximately 60--70% of the islet cells. They synthesize insulin from its precursor, proinsulin, which is then processed into mature insulin and stored in secretory granules. When blood glucose rises, beta cells release insulin into the capillary network, from which it enters the portal circulation to exert metabolic effects on the liver, muscle, and adipose tissue.
C. thymus gland.
The thymus is a primary lymphoid organ situated in the anterior mediastinum. It is responsible for the maturation and differentiation of T-lymphocytes and secretes hormones such as thymosin, thymopoietin, and thymulin, which support immune function. The thymus does not participate in glucose homeostasis and does not produce insulin. Its endocrine role is strictly limited to immune system regulation.
D. posterior lobe of the thyroid gland.
The thyroid gland consists of two lateral lobes connected by an isthmus and produces thyroid hormones (T3 and T4) from follicular cells and calcitonin from parafollicular C-cells. It does not possess a distinct "posterior lobe"; such terminology is more appropriate for the pituitary gland. More importantly, no part of the thyroid gland synthesizes insulin. The thyroid's function centers on metabolism, growth, and calcium balance, not glucose regulation.
Conclusion:
Insulin is synthesized exclusively by the beta cells located within the pancreatic Islets of Langerhans. This precise cellular localization is fundamental to understanding glucose metabolism and disorders such as diabetes mellitus. The other options refer either to incorrect anatomical divisions of the pancreas or to entirely different organs involved in immune function or metabolic regulation unrelated to insulin production
Hormones
A.
are classified by the type of secretion they produce.
B. determine the release of the antidiuretic hormone (ADH) by plasma osmolality to decrease water absorption.
C. regulate fluid and electrolyte balance, reproduction, growth and development, and adaptation to stress and metabolism.
D. influence humoral immunity by destroying antibodies.
Rationale
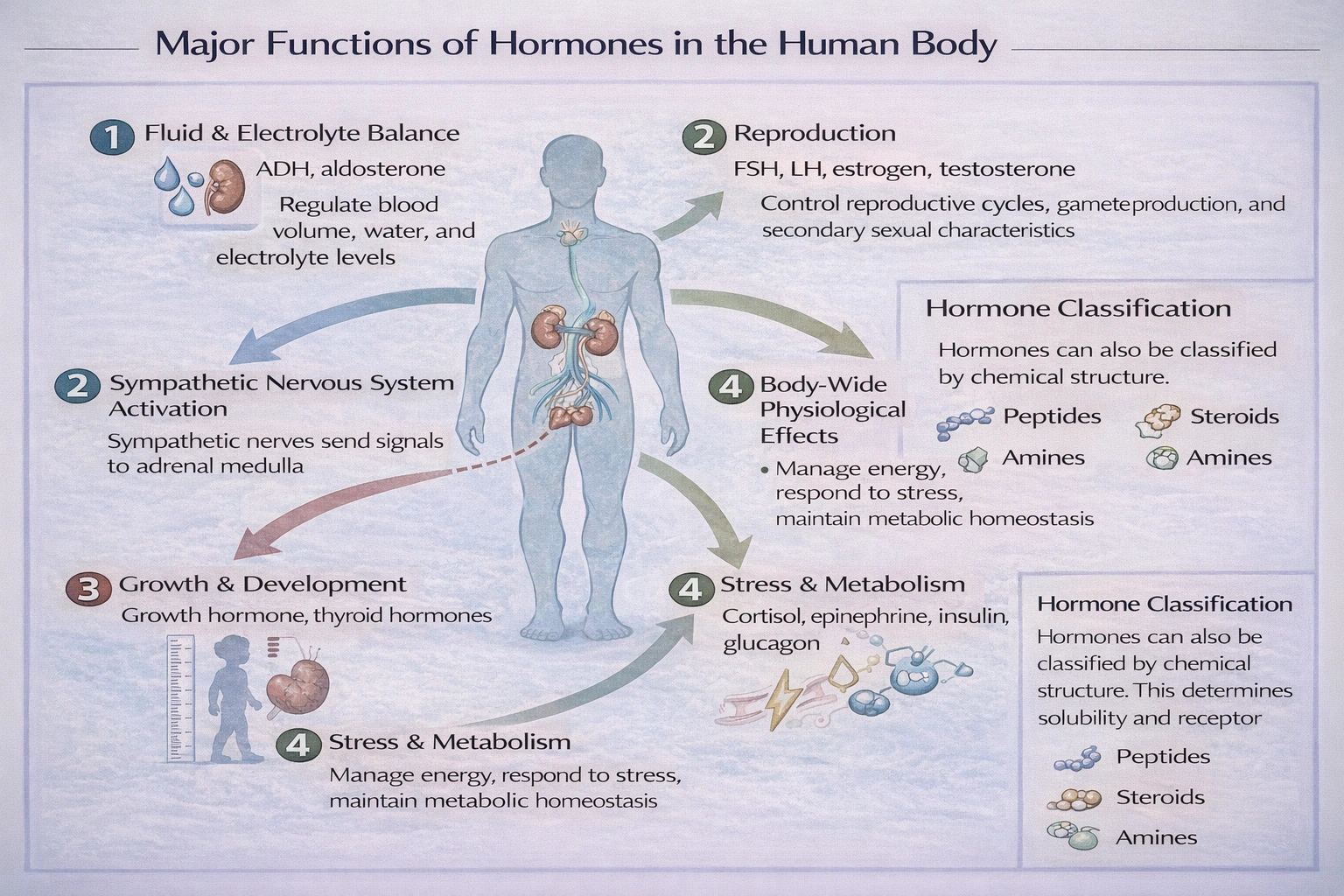
Hormones regulate fluid and electrolyte balance, reproduction, growth and development, and adaptation to stress and metabolism.
Hormones are chemical messengers secreted by endocrine glands into the bloodstream to coordinate and regulate a wide range of physiological processes. Their primary functions include maintaining homeostasis in fluid and electrolyte balance (e.g., aldosterone, ADH), controlling reproductive cycles and functions (e.g., estrogen, testosterone, FSH, LH), directing growth and development (e.g., growth hormone, thyroid hormones), and managing the body's response to stress and metabolism (e.g., cortisol, epinephrine, insulin, glucagon). This broad, integrative role is the defining characteristic of the endocrine system.
Options:
A. are classified by the type of secretion they produce.
Hormones are classified based on their chemical structure such as peptides, steroids, or amines which determines their solubility, receptor interaction, and mechanism of action. The "type of secretion" (endocrine, exocrine, paracrine) refers to the gland's mode of release, not a classification of the hormones themselves.
B. determine the release of the antidiuretic hormone (ADH) by plasma osmolality to decrease water absorption.
ADH release is indeed triggered by increased plasma osmolality or low blood volume. However, its renal action is to increase water absorption, not decrease it. ADH inserts aquaporin channels in kidney collecting ducts, enhancing water reabsorption to concentrate urine and conserve body water.
C. regulate fluid and electrolyte balance, reproduction, growth and development, and adaptation to stress and metabolism.
This accurately summarizes the core integrative functions of the endocrine system. For example, aldosterone regulates sodium and potassium balance; gonadotropins and sex steroids control reproduction; growth hormone and thyroid hormones drive growth and development; and cortisol and catecholamines manage stress responses and metabolic adaptation.
D. influence humoral immunity by destroying antibodies.
While some hormones (like glucocorticoids) can modulate immune function, they do not directly destroy antibodies. Antibodies are degraded through normal catabolic processes, and immune regulation involves complex feedback, not hormone-mediated antibody destruction.
Conclusion:
Hormones act systemically to maintain homeostasis across critical life processes. Option C correctly captures the broad, regulatory scope of endocrine function, distinguishing it from structural classification, specific hormone actions, or secondary immune effects.
. The parathyroid hormone and calcitonin work together to control the level of
A.
androgens in the blood
B. calcium in the blood
C. pepsin in the blood
D. progesterone in the blood
Rationale
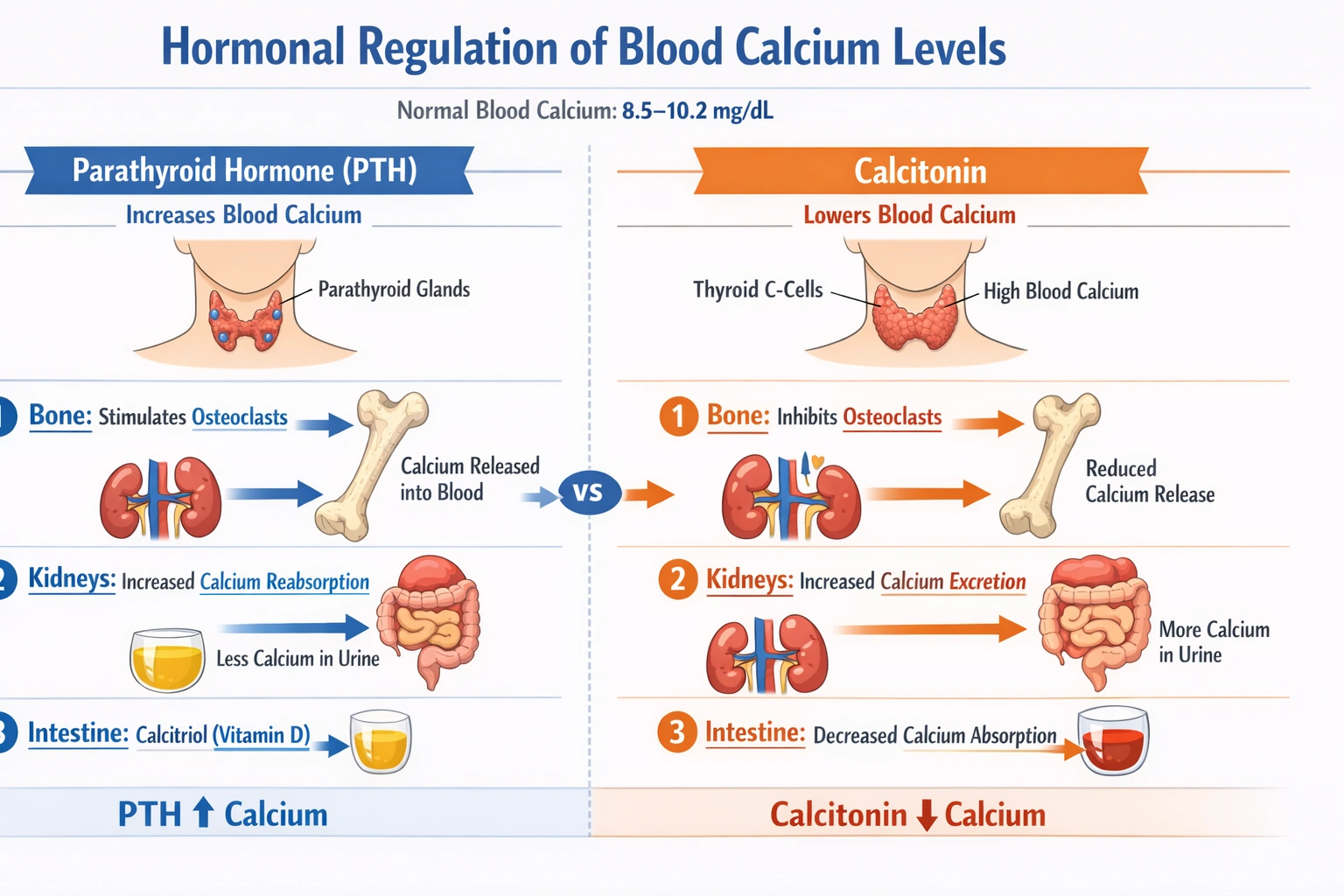
The parathyroid hormone and calcitonin work together to control the level of calcium in the blood.
This dual-hormone system provides precise regulation of ionized calcium concentration, which is critical for neuromuscular excitability, blood coagulation, enzyme function, and skeletal integrity.
A. androgens in the blood
Androgens (e.g., testosterone, dihydrotestosterone) are steroid hormones produced primarily by the testes in males, the ovaries in females, and the adrenal cortex in both sexes. Their synthesis and secretion are regulated by the hypothalamic-pituitary-gonadal axis via luteinizing hormone (LH). Parathyroid hormone and calcitonin have no known influence on androgen synthesis, metabolism, or feedback control.
B. calcium in the blood
Parathyroid hormone (PTH), secreted by the chief cells of the parathyroid glands in response to low ionized calcium, raises blood calcium by: (1) stimulating osteoclast activity and bone resorption, (2) increasing renal calcium reabsorption in the distal tubules, and (3) enhancing intestinal calcium absorption indirectly by stimulating renal production of calcitriol (active vitamin D). Calcitonin, secreted by thyroid C-cells in response to high ionized calcium, lowers blood calcium by: (1) inhibiting osteoclast activity and bone resorption, and (2) increasing renal calcium excretion. Their opposing actions fine-tune serum calcium within a narrow range (approximately 8.5--10.2 mg/dL).
C. pepsin in the blood
Pepsin is a proteolytic enzyme secreted by gastric chief cells as inactive pepsinogen. It is activated by stomach acid and functions exclusively within the gastric lumen to digest dietary proteins. Under normal conditions, pepsin is not present in active form in the bloodstream, and its secretion is regulated by local factors (e.g., gastrin, vagal stimulation) and gastric pH, not by systemic calcium-regulating hormones.
D. progesterone in the blood
Progesterone is a steroid sex hormone produced by the corpus luteum, placenta, and adrenal cortex. Its secretion is controlled primarily by luteinizing hormone (LH) and human chorionic gonadotropin (hCG). It prepares and maintains the endometrium for pregnancy and has no physiological link to the calcium-homeostatic actions of PTH and calcitonin.
Conclusion:
Parathyroid hormone and calcitonin form a complementary hormonal pair dedicated exclusively to the regulation of blood calcium levels. Their antagonistic actions on bone, kidney, and (indirectly) the intestine are essential for calcium homeostasis, a function completely separate from the control of sex hormones, digestive enzymes, or other blood constituents.
Which of the following chambers of the heart has the thickest wall?
A.
Left atrium
B. Left ventricle
C. Right atrium
D. Right ventricle
Rationale
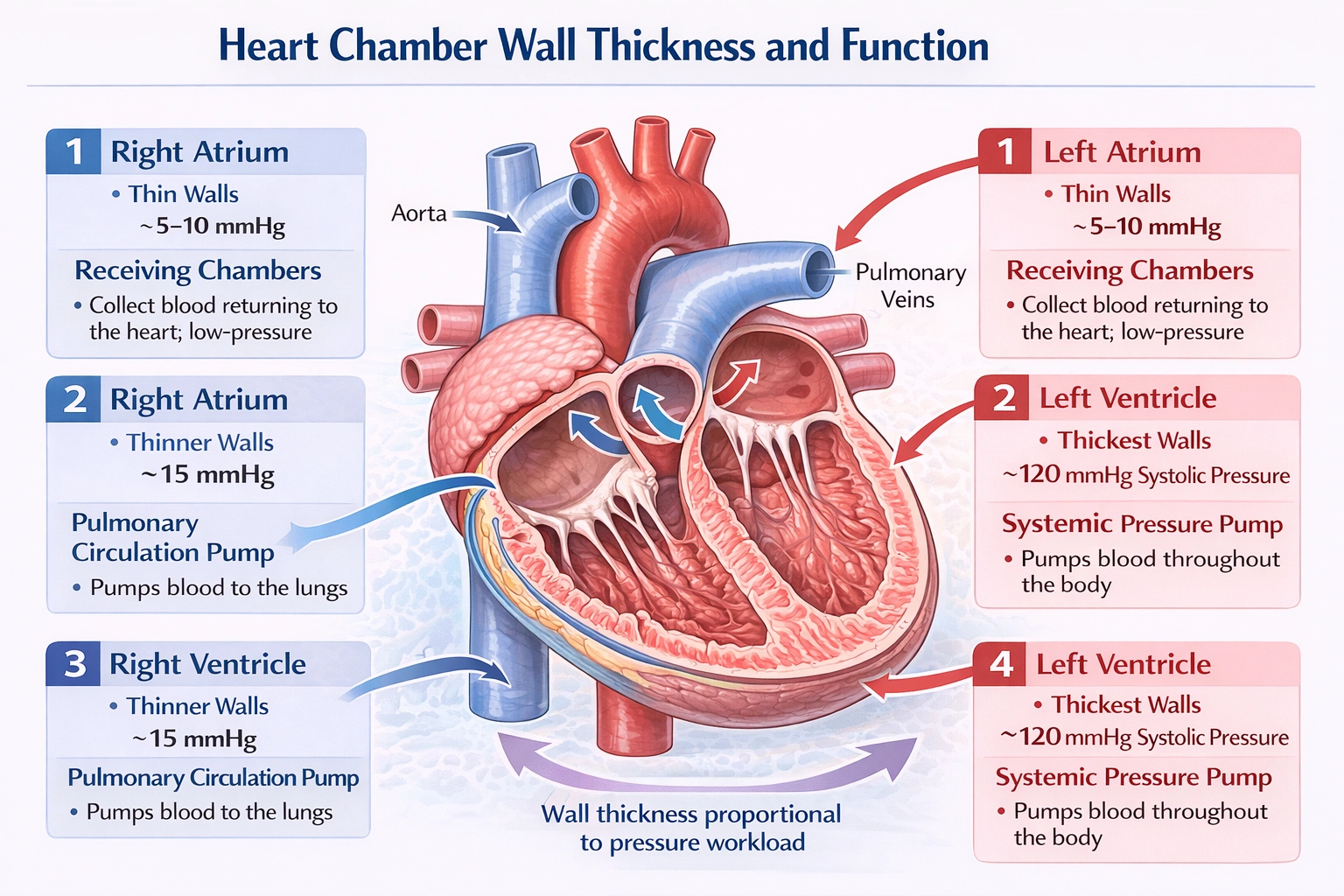
The chamber of the heart with the thickest wall is the left ventricle.
This structural adaptation is directly related to its physiological function: it must generate sufficient pressure to pump oxygenated blood through the entire systemic circulation against the high resistance of the body's arterial network. The thickness of the ventricular wall is proportional to the pressure it must develop; the left ventricle works against a mean arterial pressure of approximately 90--100 mmHg, whereas the right ventricle pumps into the low-pressure pulmonary circuit (mean pulmonary arterial pressure of about 15 mmHg).
A. Left atrium
The left atrium serves as a receiving chamber for oxygenated blood returning from the lungs via the pulmonary veins. Its primary role is to act as a reservoir and conduit, directing blood into the left ventricle during ventricular diastole. The pressure within the atria is low (normally around 5--10 mmHg), so the atrial walls are thin, consisting mainly of a thin layer of myocardium overlying the endocardium. While it contributes a final 20--30% to ventricular filling during atrial systole, it does not require a thick muscular wall.
B. Left ventricle
The left ventricle is the powerhouse of the heart. Its wall is composed of a thick, spiraling mass of cardiac muscle, typically 8--15 mm thick in a healthy adult about three times thicker than the right ventricular wall. This substantial myocardium is necessary to produce the forceful contractions that eject blood into the aorta at systolic pressures of around 120 mmHg. The left ventricle's architecture, including the papillary muscles and trabeculae carneae, is optimized for generating high pressure rather than volume.
C. Right atrium
The right atrium receives deoxygenated blood from the superior and inferior venae cavae and the coronary sinus. Like the left atrium, it is a low-pressure chamber that functions mainly as a passive conduit. Its thin wall is adequate for delivering blood to the right ventricle with a minimal contracting force. The right atrial appendage and the crista terminalis are internal features, but they do not contribute significant muscular thickness.
D. Right ventricle
The right ventricle pumps blood into the pulmonary trunk and onward to the lungs. Because the pulmonary circulation offers much lower resistance, the right ventricle functions as a volume pump rather than a pressure pump. Its wall is considerably thinner (about 3--5 mm) and is crescent-shaped in cross-section, adapting to the low-pressure workload. While it can generate significant volume output, it does not develop the high wall tension or require the myocardial mass of the left ventricle.
Conclusion:
The thickness of the heart chamber walls is a direct reflection of their hemodynamic responsibilities. The left ventricle, tasked with systemic perfusion, possesses the thickest myocardial wall. The atria and right ventricle, operating under lower pressures, have proportionally thinner walls.
Coronary arteries branch off of the __________ to supply oxygenated blood to the heart.
A.
aorta
B. inferior vena cava
C. pulmonary artery
D. right coronary vein
Rationale
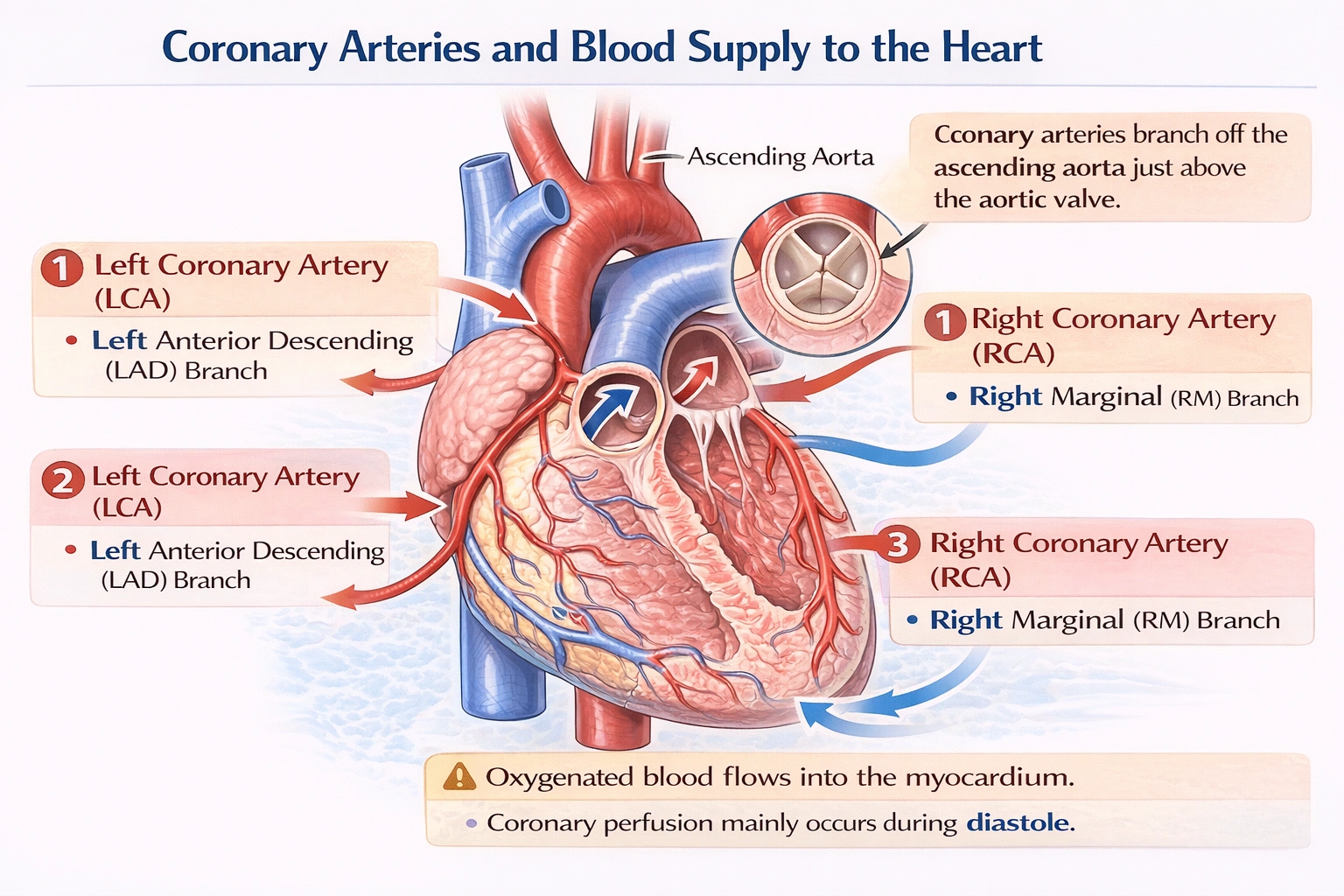
Coronary arteries branch off of the aorta to supply oxygenated blood to the heart.
The left and right coronary arteries arise directly from the ascending aorta, just above the aortic valve. They are the first branches of the aorta and are uniquely positioned to deliver freshly oxygenated bloodunder high systemic pressure to the myocardium (heart muscle). This ensures that the heart receives its own dedicated blood supply to meet its high metabolic demands.
A. aorta
The left and right coronary arteries are the first branches of the ascending aorta. The left coronary artery typically arises from the left aortic sinus and divides into the left anterior descending and circumflex arteries. The right coronary artery originates from the right aortic sinus. This aortic origin guarantees that the heart muscle is perfused with oxygen-rich blood under the highest pressure in the systemic circulation, which is especially crucial during diastole when coronary filling is maximal.
B. inferior vena cava
The inferior vena cava is a major venous structure that returns deoxygenated blood from the lower body to the right atrium. Arteries, by definition, carry blood away from the heart, and the coronary circulation is an arterial system. No arteries branch from major veins; their embryological origins, histological structures, and pressure characteristics are fundamentally different.
C. pulmonary artery
The pulmonary artery carries deoxygenated blood from the right ventricle to the lungs. Its blood has a low oxygen saturation. The myocardium requires a constant, high-supply of oxygenated blood, which would not be provided by a vessel carrying deoxygenated blood. The coronary arteries are part of the systemic, not pulmonary, arterial tree.
D. right coronary vein
The right coronary vein is a component of the cardiac venous drainage system, collecting deoxygenated blood from the heart wall and delivering it to the coronary sinus or directly into the right atrium. Vessels do not branch from veins to form arteries; the vascular circuit flows from arteries to capillaries to veins. An artery cannot originate from a vein.
Conclusion:
The coronary arteries uniquely arise from the base of the aorta, providing a dedicated, high-pressure supply of oxygenated blood to the cardiac muscle itself. This distinguishes them from venous structures or vessels of the pulmonary circuit.
Blood in the venous system of the body flows
A.
away from the heart.
B. in a figure-eight pattern.
C. toward the heart.
D. under constant high pressure.
Rationale
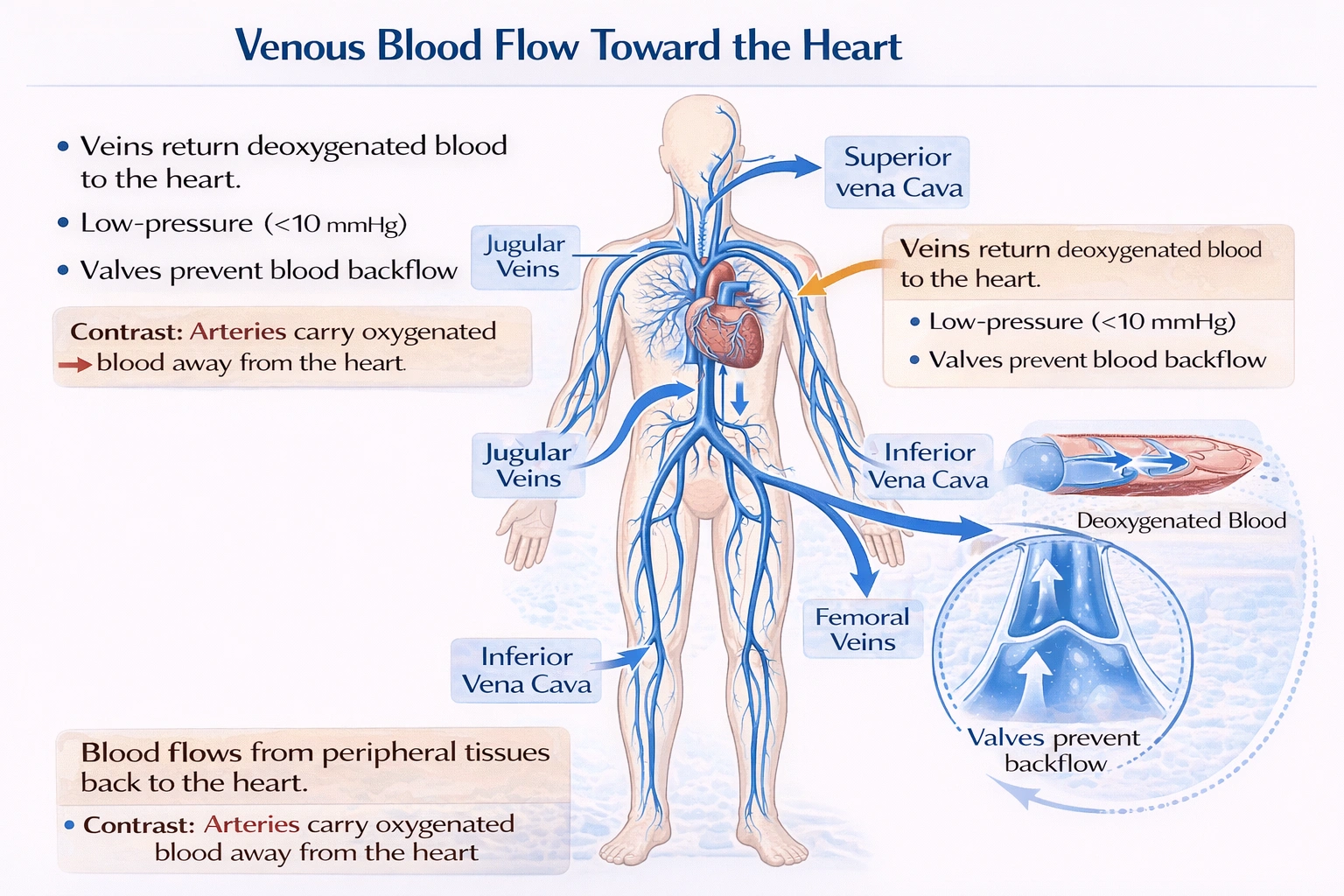
Blood within the systemic venous system flows toward the heart. Veins are the vessels responsible for returning deoxygenated blood from the body's tissues back to the right atrium of the heart, completing the circulatory loop so that blood can be re-oxygenated in the lungs.
A. away from the heart.
This is the defining function of arteries, not veins. The systemic arteries carry oxygenated blood away from the left ventricle to the tissues. The pulmonary arteries, while carrying deoxygenated blood, also conduct blood away from the heart (the right ventricle) toward the lungs.
B. in a figure-eight pattern.
This description does not correspond to any standard pattern of blood flow in the human body. The circulatory system is largely arranged in two serial loops: the systemic circuit (left heart to body and back to right heart) and the pulmonary circuit (right heart to lungs and back to left heart). This is sometimes conceptually described as a "double circuit," but not as a figure-eight.
C. toward the heart.
This is the correct description for veins. The venous system includes superficial and deep veins, which often contain valves to prevent backflow, and they ultimately converge into the superior and inferior venae cavae, which empty into the right atrium. This unidirectional return flow is essential for maintaining cardiac preload and continuous circulation.
D. under constant high pressure.
Venous pressure is significantly lower than arterial pressure. Systemic venous pressure is typically less than 10 mmHg, compared to arterial pressures around 120/80 mmHg. Veins are thin-walled, compliant vessels that act as capacitance vessels, holding a large portion of the blood volume at low pressure. Pressure in veins is not constant; it fluctuates with respiration, muscle contraction, and cardiac cycle.
Conclusion:
The primary direction of blood flow in systemic veins is toward the heart, facilitating the return of blood to the central circulation. This contrasts with the high-pressure, away-from-the-heart flow in arteries.
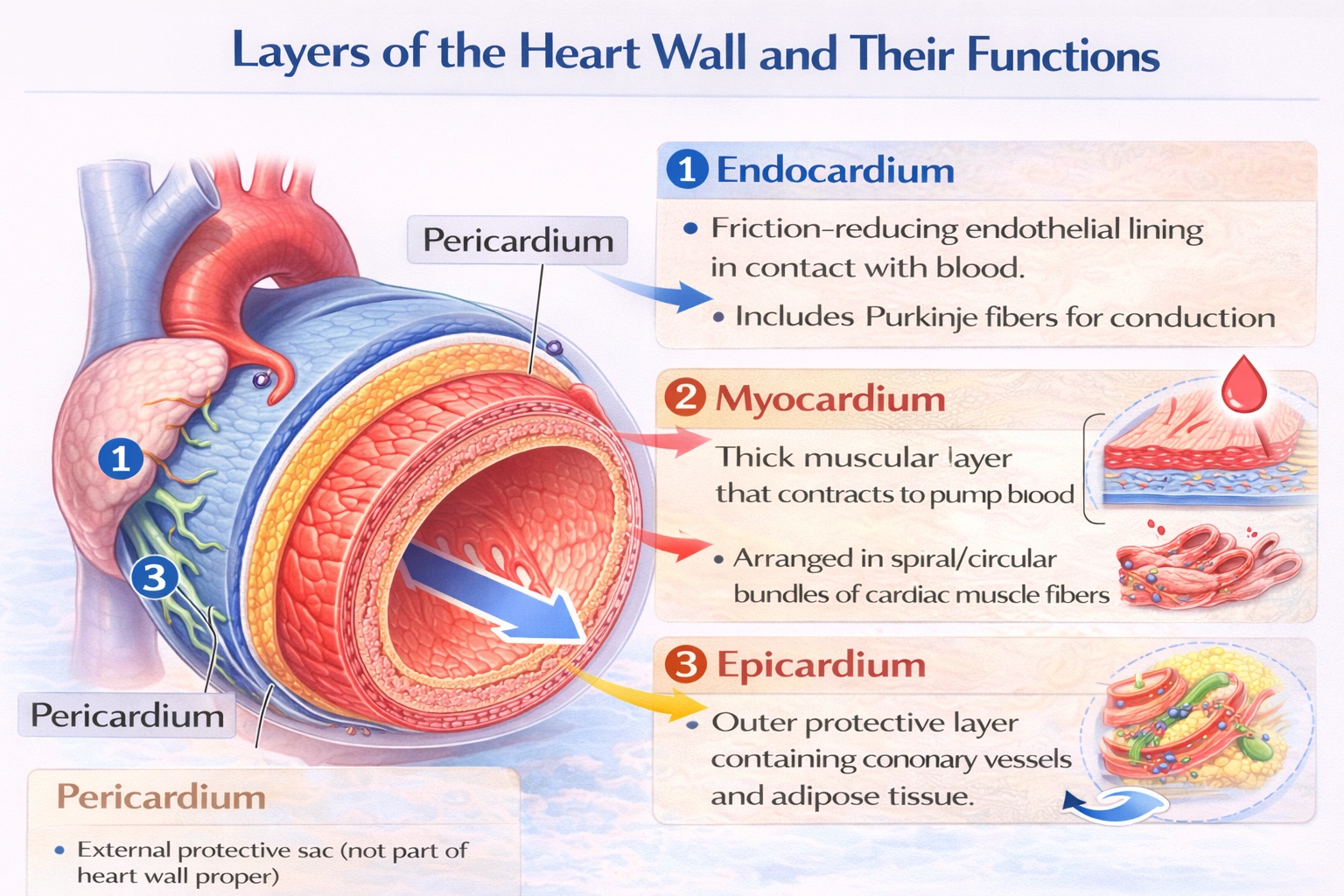
The innermost layer of the heart wall is the
A.
endocardium
B. epicardium
C. myocardium
D. pericardium
Rationale
The innermost layer of the heart wall is the endocardium.
This thin, smooth membrane lines the interior chambers of the heart the atria and ventricles and covers the surfaces of the heart valves. Composed of a single layer of endothelial cells overlying a thin layer of connective tissue, it provides a friction‑reducing surface for blood flow and is continuous with the endothelial lining of the great vessels.
A. endocardium
The endocardium is the innermost lining of the heart. Its endothelial cells are in direct contact with the blood and secrete substances that prevent clotting, modulate vascular tone, and regulate inflammatory responses. This layer also houses specialized cardiac conduction fibers (Purkinje fibers) in the subendocardial tissue, integrating its role in smooth blood flow with the heart's electrical system.
B. epicardium
The epicardium, or visceral layer of the serous pericardium, is the outermost layer of the heart wall proper. It is a serous membrane composed of mesothelial cells and underlying connective and adipose tissue. It protects the heart surface, contains coronary vessels and nerves, and secretes pericardial fluid into the pericardial cavity to reduce friction during cardiac contraction. It is external to the myocardium and does not contact the blood‑filled chambers.
C. myocardium
The myocardium is the thick, muscular middle layer responsible for the heart's pumping action. It consists of cardiac muscle cells (cardiomyocytes) arranged in spiral bundles, interconnected by intercalated discs. While it is the dominant layer in mass and function, it lies between the endocardium and epicardium, not at the innermost position.
D. pericardium
The pericardium is a double‑walled sac that encloses the heart and the roots of the great vessels. It consists of an outer fibrous pericardium and an inner serous pericardium (parietal and visceral layers). It anchors the heart in the mediastinum, prevents over‑distension, and provides a lubricated environment. It is not a layer of the heart wall itself but a separate protective structure.
Conclusion:
The endocardium is definitively the innermost layer of the heart wall, providing a critical interface between the blood and the cardiac tissues. The myocardium is the muscular pump, the epicardium is the outer protective coat, and the pericardium is an external sac all distinct from the internal endothelial lining.
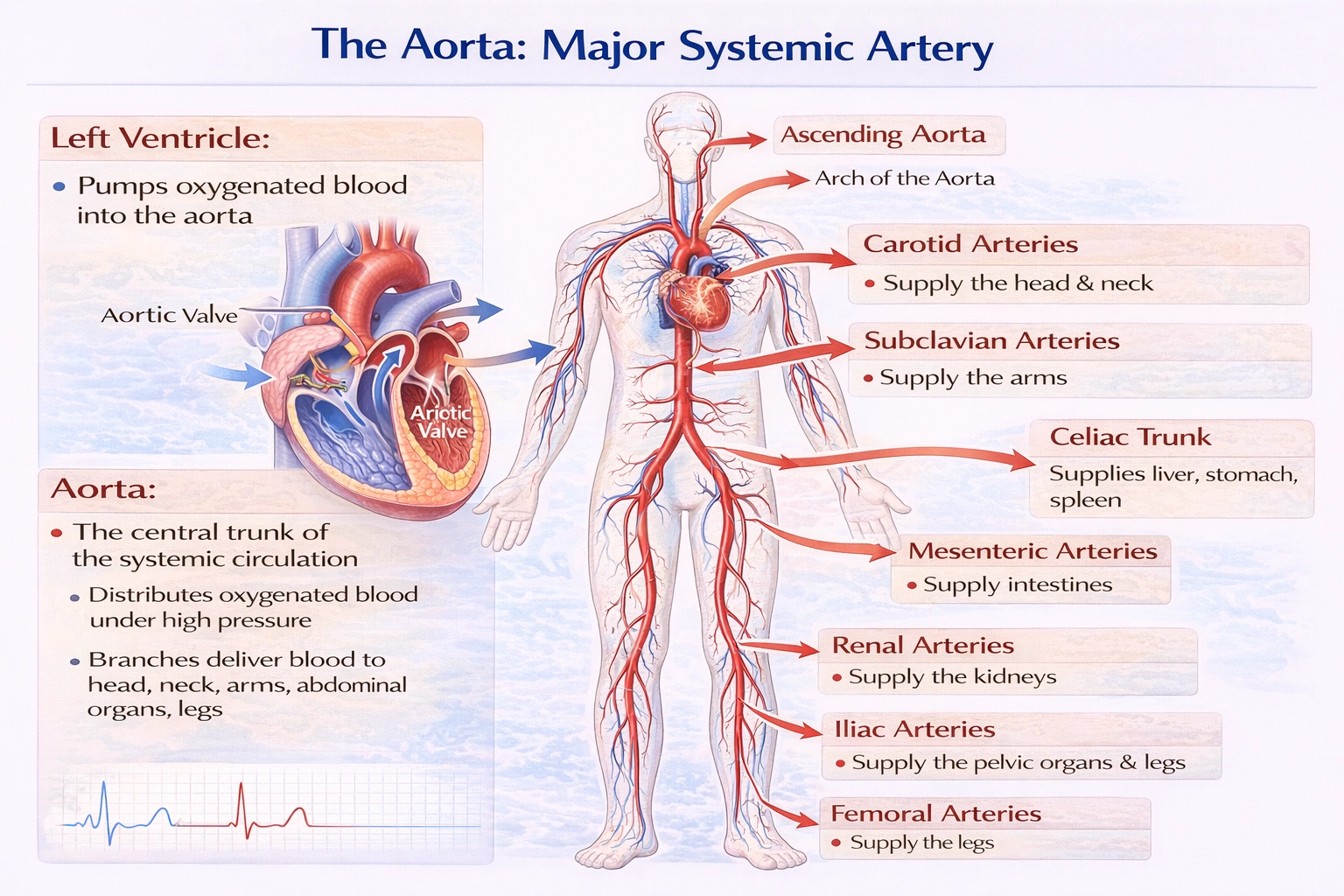
The major systemic artery in the body is the
A.
aorta
B. carotid
C. femoral
D. pulmonary
Rationale
The major systemic artery in the body is the aorta.
The aorta is the largest artery in the human body and serves as the primary conduit for oxygenated blood leaving the heart. Originating from the left ventricle, it ascends, arches, and descends through the thoracic and abdominal cavities, giving rise to all major arterial branches that supply oxygen-rich blood to every organ and tissue except the lungs.
A. aorta
The aorta is the main trunk of the systemic arterial system. It begins at the aortic valve, extends as the ascending aorta, forms the aortic arch, and continues as the descending aorta (thoracic and abdominal sections). Its numerous branches---including the coronary, carotid, subclavian, celiac, mesenteric, renal, and iliac arteries---ensure that all body regions receive oxygenated blood under high pressure.
B. carotid
The carotid arteries are vital branches of the aortic arch that supply the head and neck. While essential for cerebral and facial circulation, they are secondary vessels within the systemic tree and do not represent the central arterial trunk.
C. femoral
The femoral artery is a major peripheral artery in the lower limb, arising from the external iliac artery. It is crucial for supplying the thigh and leg but is a distal branch of the aortic system, not the primary systemic artery.
D. pulmonary
The pulmonary artery is a large artery that carries deoxygenated blood from the right ventricle to the lungs. It belongs to the pulmonary circulation, not the systemic circulation, and therefore does not distribute oxygenated blood throughout the body.
Conclusion:
The aorta is unequivocally the major systemic artery, functioning as the central outflow channel from the left ventricle and the origin of the entire systemic arterial network. While the carotid and femoral arteries are important systemic branches, and the pulmonary artery is a major vessel in its own circuit, only the aorta meets the criteria of being the principal systemic artery.
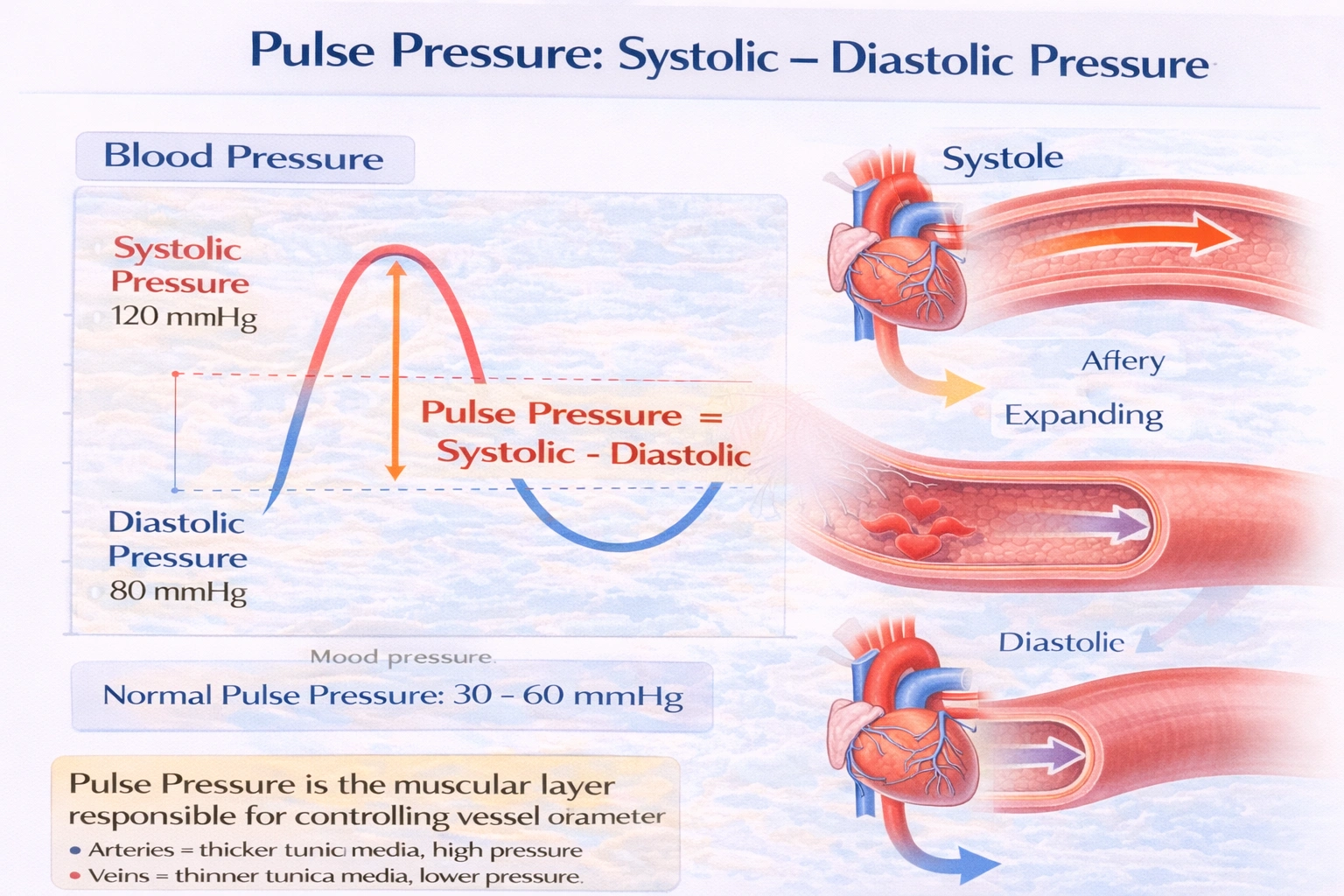
Systolic pressure minus diastolic pressure equals
A.
cardiac output
B. mean arterial pressure
C. pulse pressure
D. venous pressure
Rationale
Systolic pressure minus diastolic pressure equals pulse pressure.
Pulse pressure is calculated by subtracting the diastolic blood pressure from the systolic blood pressure. This value represents the force that the heart generates with each contraction and provides insight into arterial stiffness and stroke volume. A normal pulse pressure is typically between 30 and 60 mmHg, and variations can indicate cardiovascular health status.
A. cardiac output
Cardiac output is the volume of blood pumped by the heart per minute, calculated as heart rate multiplied by stroke volume. It is not derived from a simple subtraction of pressure values.
B. mean arterial pressure
Mean arterial pressure (MAP) is the average pressure in the arteries throughout one cardiac cycle. It is estimated using the formula: MAP = Diastolic Pressure + (Pulse Pressure / 3). It is a weighted average, not a direct subtraction.
C. pulse pressure
This is correct. Pulse pressure is defined as the difference between systolic and diastolic blood pressures. It reflects the fluctuation in arterial pressure during a heartbeat and is influenced by heart contractility, arterial elasticity, and vascular resistance.
D. venous pressure
Venous pressure refers to the blood pressure in the venous system, which is significantly lower than arterial pressure. It is measured directly or estimated clinically but is not calculated from systolic and diastolic arterial pressures.
Conclusion:
Pulse pressure is the specific hemodynamic parameter obtained by subtracting diastolic pressure from systolic pressure. This calculation helps assess cardiovascular function, while the other terms represent different measurements of cardiac performance or vascular pressure.
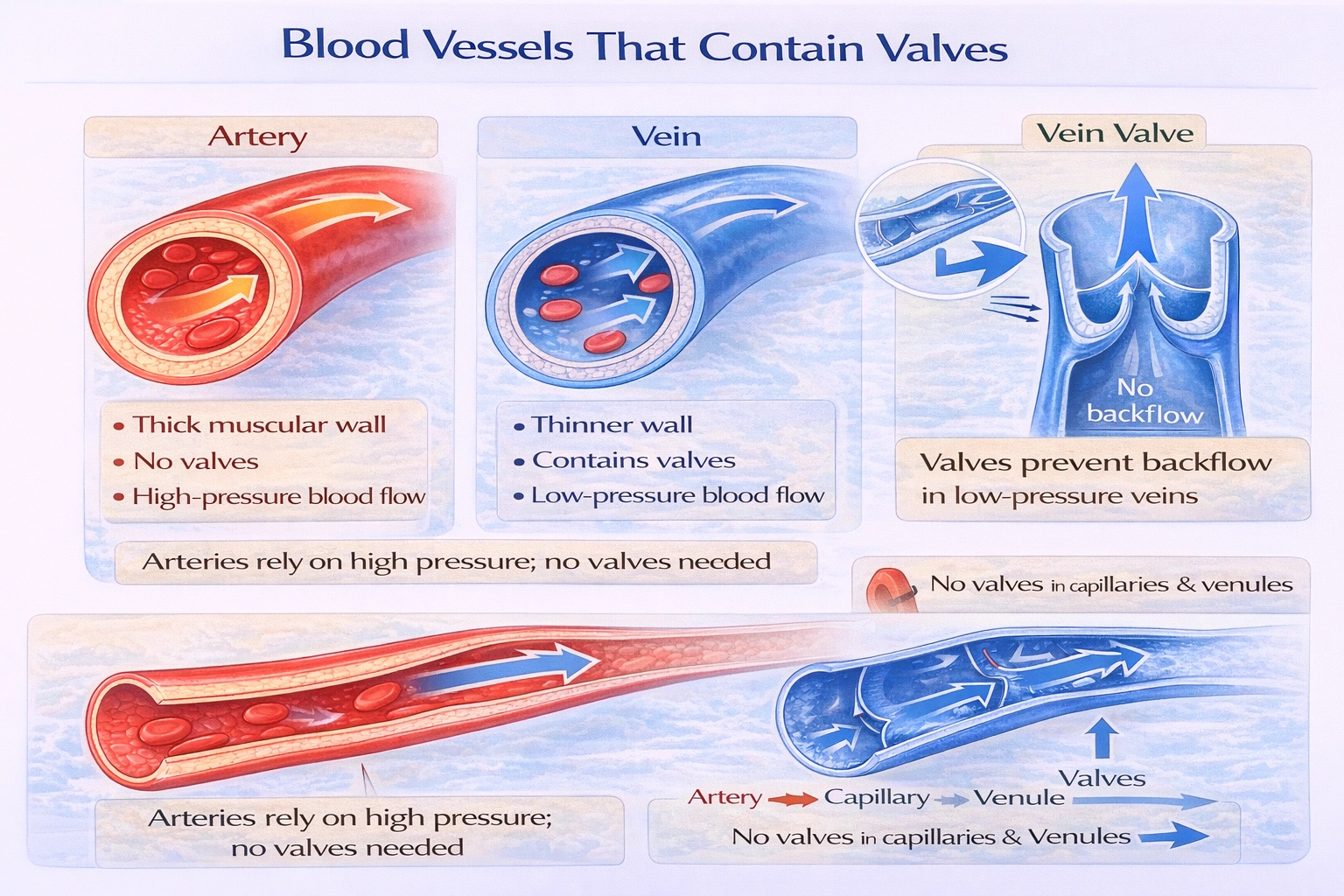
Blood vessels that contain valves are
A.
arteries
B. capillaries
C. veins
D. venules
Rationale
Blood vessels that contain valves are veins.
Valves are folds of the tunica intima (inner lining) that form bicuspid structures within the lumen of many veins. Their function is to prevent the backflow of blood, especially in extremities where blood must flow against gravity under low pressure. This ensures unidirectional movement toward the heart.
A. arteries
Arteries carry blood under high pressure generated by ventricular contraction, which propels blood forward and minimizes backflow. With the exception of the semilunar valves at the heart's exits (aortic and pulmonary valves), arteries do not contain internal valves in their walls.
B. capillaries
Capillaries are microscopic exchange vessels composed of a single layer of endothelial cells. They lack any structural specializations such as valves, smooth muscle, or connective tissue layers.
C. veins
This is correct. Valves are a characteristic feature of many veins, particularly in the limbs. They allow blood to move toward the heart while closing to prevent retrograde flow, which is essential for maintaining venous return against gravity.
D. venules
Venules are small veins that collect blood from capillaries. Their walls are thin, with minimal smooth muscle, and they generally do not contain well-developed valves. Valves become more prominent in larger, medium-sized veins where gravitational challenges are greater.
Conclusion:
Valves are a defining structural adaptation of veins, enabling efficient return of blood to the heart under low-pressure conditions. Arteries, capillaries, and venules lack such valves due to their different hemodynamic roles.
The tonsils, thymus, spleen, and lymph nodes can be grouped together as
A.
digestive organs.
B. endocrine glands.
C. lymphoid organs.
D. respiratory structures.
Rationale
The tonsils, thymus, spleen, and lymph nodes can be grouped together as lymphoid organs.
These four structures are integral components of the lymphatic and immune systems. They are classified as lymphoid organs because they are composed primarily of lymphoid tissue, which is rich in lymphocytes (such as B cells and T cells) and other immune cells. Their collective functions involve the production, maturation, activation, and housing of lymphocytes, as well as the filtration of body fluids to remove pathogens and foreign particles.
A. digestive organs
While the tonsils are located in the pharyngeal region near the entrance of the digestive and respiratory tracts, their primary function is immunological, not digestive. The thymus, spleen, and lymph nodes have no direct role in the mechanical or chemical breakdown of food. Therefore, this category does not accurately describe the group.
B. endocrine glands
Endocrine glands secrete hormones directly into the bloodstream. Although the thymus has an endocrine function secreting hormones like thymosin that promote T cell maturation the tonsils, spleen, and lymph nodes are not primarily endocrine in function. Their main roles are related to immune surveillance and response, not hormonal secretion.
C. lymphoid organs
This is the correct classification.
Tonsils are masses of lymphoid tissue in the pharynx that trap pathogens entering through the mouth or nose.
Thymus is a primary lymphoid organ where T lymphocytes mature and become immunocompetent.
Spleen is the largest secondary lymphoid organ; it filters blood, removes old red blood cells, and mounts immune responses against blood-borne pathogens.
Lymph nodes are distributed along lymphatic vessels and filter lymph, removing debris and pathogens while activating lymphocytes.
All share the common purpose of supporting immune function.
D. respiratory structures
Only the tonsils have an anatomical association with the respiratory pathway, but their role is immunological. The thymus is located in the mediastinum, the spleen in the abdomen, and lymph nodes throughout the body; none participate in gas exchange or other core respiratory functions.
Conclusion
The tonsils, thymus, spleen, and lymph nodes are unified by their structure and function as key organs of the lymphatic and immune systems. Their primary roles involve immune cell production, filtration, and immune response activation, correctly categorizing them as lymphoid organs.
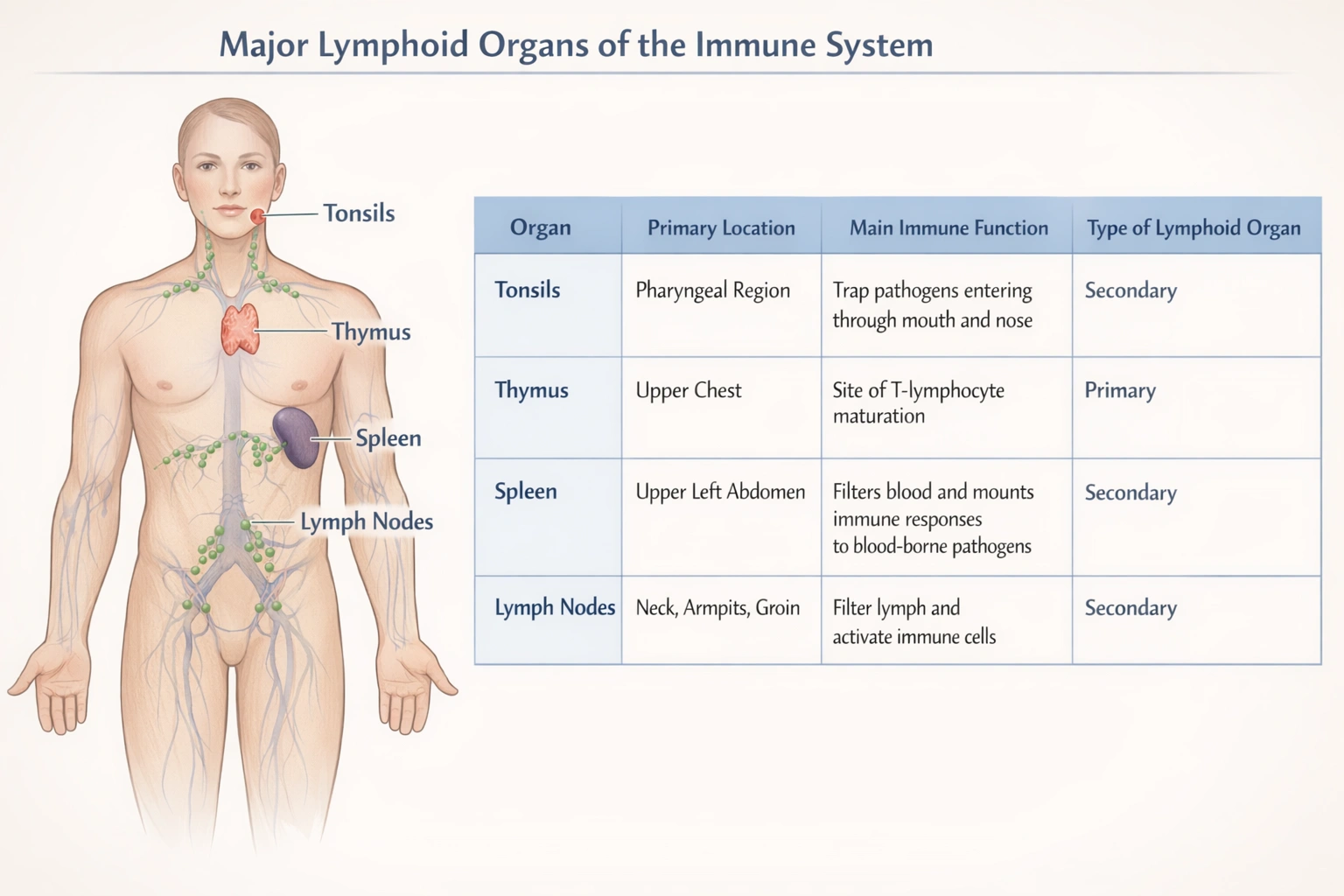
Sensible fluid loss occurs from which of the following?
A.
kidneys
B. lungs
C. skin
D. small intestine
Rationale
Sensible fluid loss occurs from the kidneys.
Fluid loss from the body is categorized as either sensible or insensible. Sensible fluid loss refers to output that is consciously perceived and readily measurable. The most significant and regulated form of sensible loss is urine produced by the kidneys. Urine output is controlled by hormones like antidiuretic hormone (ADH) and aldosterone, allowing the body to precisely adjust water and solute excretion to maintain fluid balance. An individual is aware of the urge to urinate and can measure the volume voided.
A. kidneys
Correct. Urine output is the primary example of sensible fluid loss. It is perceptible, measurable, and subject to physiological regulation. The average daily urine output is about 1 to 2 liters, but this can vary widely based on hydration, hormone levels, and kidney function.
B. lungs
The lungs contribute to insensible fluid loss. Water evaporates continuously from the respiratory surfaces during breathing, and this loss is not consciously perceived under normal conditions. It amounts to roughly 300 to 400 mL per day and is not regulated for the purpose of fluid balance but is influenced by respiratory rate and air humidity.
C. skin
The skin contributes to both insensible and sensible loss. Insensible perspiration is the passive diffusion and evaporation of water through the skin (about 300 to 400 mL/day), which is not felt. Sensible loss from the skin occurs specifically through active sweating (diaphoresis) in response to heat or exercise, which is perceptible and measurable. However, under normal resting conditions, sensible loss from the skin is minimal compared to renal loss.
D. small intestine
While about 8 to 9 liters of fluid enter the gastrointestinal tract daily, the vast majority is reabsorbed. The fluid lost in formed stool is a minor sensible loss (typically 100 to 200 mL per day). Although measurable, it is not a major regulated route for daily fluid balance compared to renal output.
Conclusion
The kidneys are the primary source of sensible fluid loss in the form of urine. This loss is both perceptible and subject to precise physiological control, making it central to the body's regulation of fluid volume and composition. Other routes, like the lungs and skin, contribute more to insensible loss, while gastrointestinal loss is comparatively small.
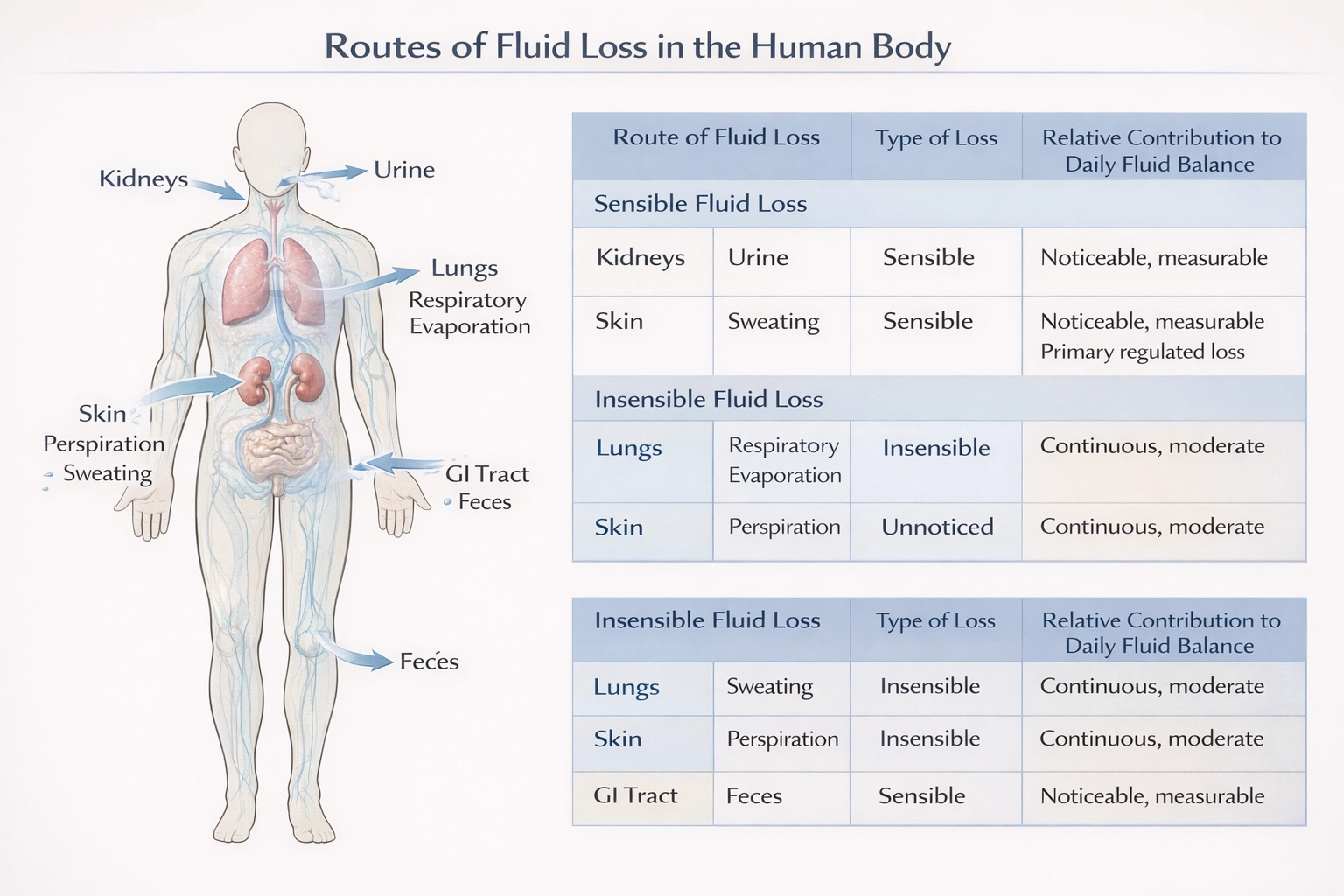
A __________ solution contains fewer dissolved particles than are found in normal cells and blood.
A.
hypertonic
B. hypotonic
C. permeable
D. semipermeable
Rationale
A hypotonic solution contains fewer dissolved particles than are found in normal cells and blood.
Tonicity compares the effective solute concentration of two solutions separated by a semipermeable membrane. It predicts the direction of net water movement and its effect on cell volume. A solution with a lower solute concentration relative to the intracellular fluid is classified as hypotonic.
(A) hypertonic: A hypertonic solution has a higher concentration of solutes than the intracellular fluid. This creates an osmotic gradient that pulls water out of cells, leading to cell shrinkage or crenation.
(B) hypotonic: A hypotonic solution has a lower solute concentration than the intracellular fluid. This establishes an osmotic gradient driving water into cells, causing them to swell and potentially lyse.
(C) permeable: Permeability is a characteristic of a membrane, describing which substances can cross it. It does not describe the solute concentration of a solution.
(D) semipermeable: Semipermeable (or selectively permeable) also describes a type of membrane that allows some molecules to pass while blocking others. It is not a term used to categorize solutions based on concentration.
Conclusion
The term "hypotonic" specifically defines a solution with a lower effective solute concentration than cellular fluid, leading to osmotic water influx and cellular swelling.
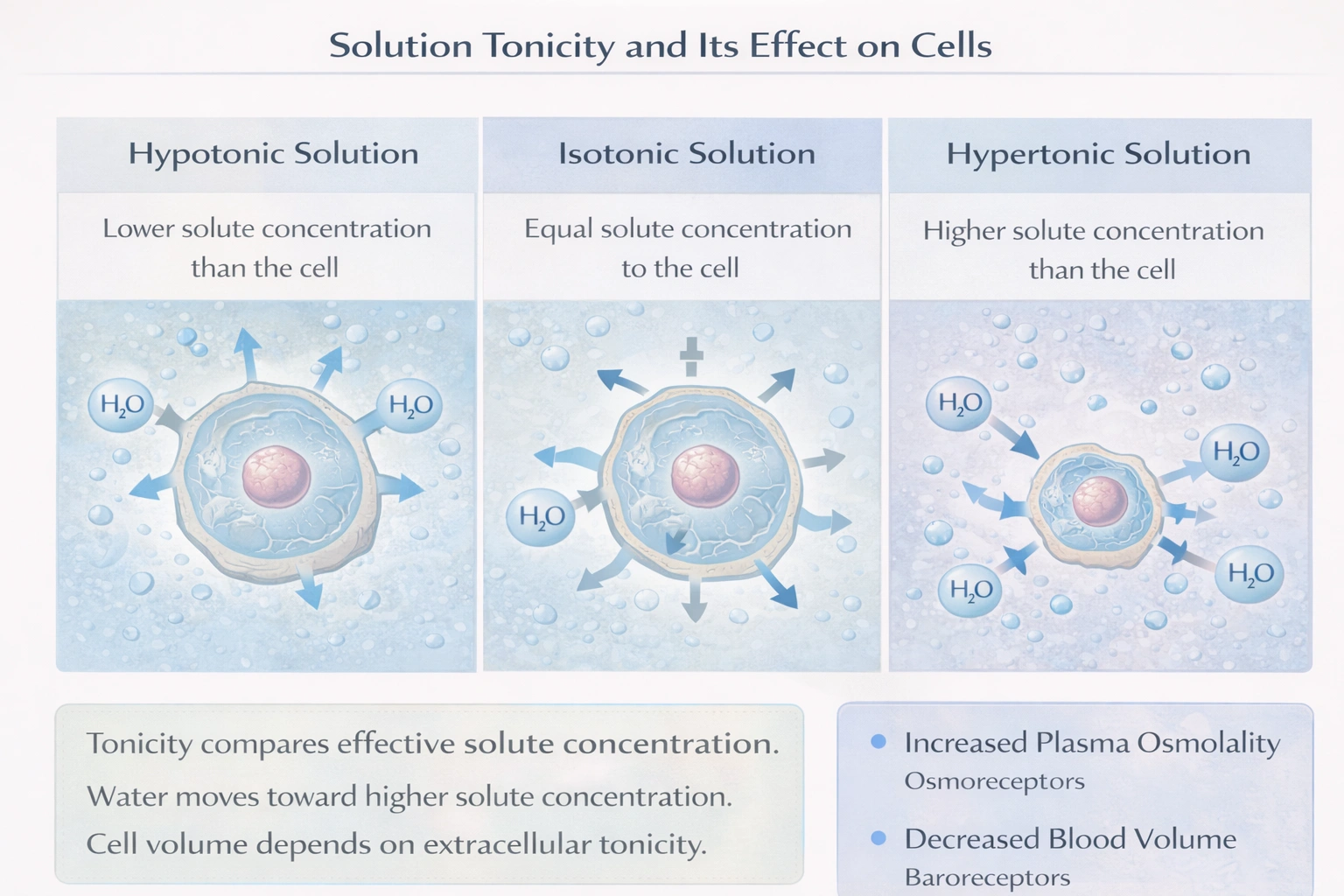
Which of the following is necessary for myocardial stimulation?
A.
calcium
B. bicarbonate
C. hydrogen
D. magnesium
Rationale
Calcium is necessary for myocardial stimulation.
Myocardial stimulation requires the process of excitation-contraction coupling, where an electrical signal (action potential) is translated into a mechanical contraction. Calcium ions (Ca²âº) are the essential chemical messenger in this process. During the cardiac action potential, depolarization opens voltage-gated L-type calcium channels in the sarcolemma, allowing a small influx of extracellular Ca²âº. This "trigger" calcium then binds to ryanodine receptors on the sarcoplasmic reticulum (SR), causing a massive release of stored Ca²âº into the cytosol. The resulting surge in intracellular calcium binds to the protein troponin C, initiating the interaction between actin and myosin filaments and producing contraction. Without this calcium signal, electrical stimulation cannot lead to mechanical force generation.
(A) calcium: Calcium ions provide the critical link between depolarization and contraction. Their influx from the extracellular space and release from the SR directly initiate the contractile cycle, making them indispensable for myocardial stimulation.
(B) bicarbonate: Bicarbonate is the primary buffer in the blood and extracellular fluid, crucial for maintaining acid-base balance. While a stable pH is necessary for the optimal function of cardiac enzymes and ion channels, bicarbonate itself does not participate in the excitation-contraction mechanism and is not a direct requirement for stimulation.
(C) hydrogen: Hydrogen ion concentration (pH) influences cardiac function significantly. Acidosis (high H⺠concentration) can depress contractility by interfering with calcium binding to troponin and by affecting ion channel function. However, H⺠ions are not a required trigger for contraction; their abnormal accumulation is instead detrimental to the process.
(D) magnesium: Magnesium plays several supportive roles in cardiac physiology. It acts as a natural calcium channel antagonist, helps stabilize excitable membranes, and is a cofactor for the Naâº/K⺠ATPase and energy-producing enzymes. Its role is primarily modulatory it helps regulate and normalize excitability and rhythm but is not the ion that directly initiates contraction.
Conclusion
Calcium is necessary for myocardial stimulation because its regulated movement into the cytosol serves as the direct biochemical trigger that couples cardiac electrical activity to mechanical contraction.
Roughly one-third of body weight is in the
A.
intracellular fluid compartment.
B. extracellular fluid compartment.
C. kidneys.
D. plasma.
Rationale
Roughly one-third of body weight is in the extracellular fluid compartment
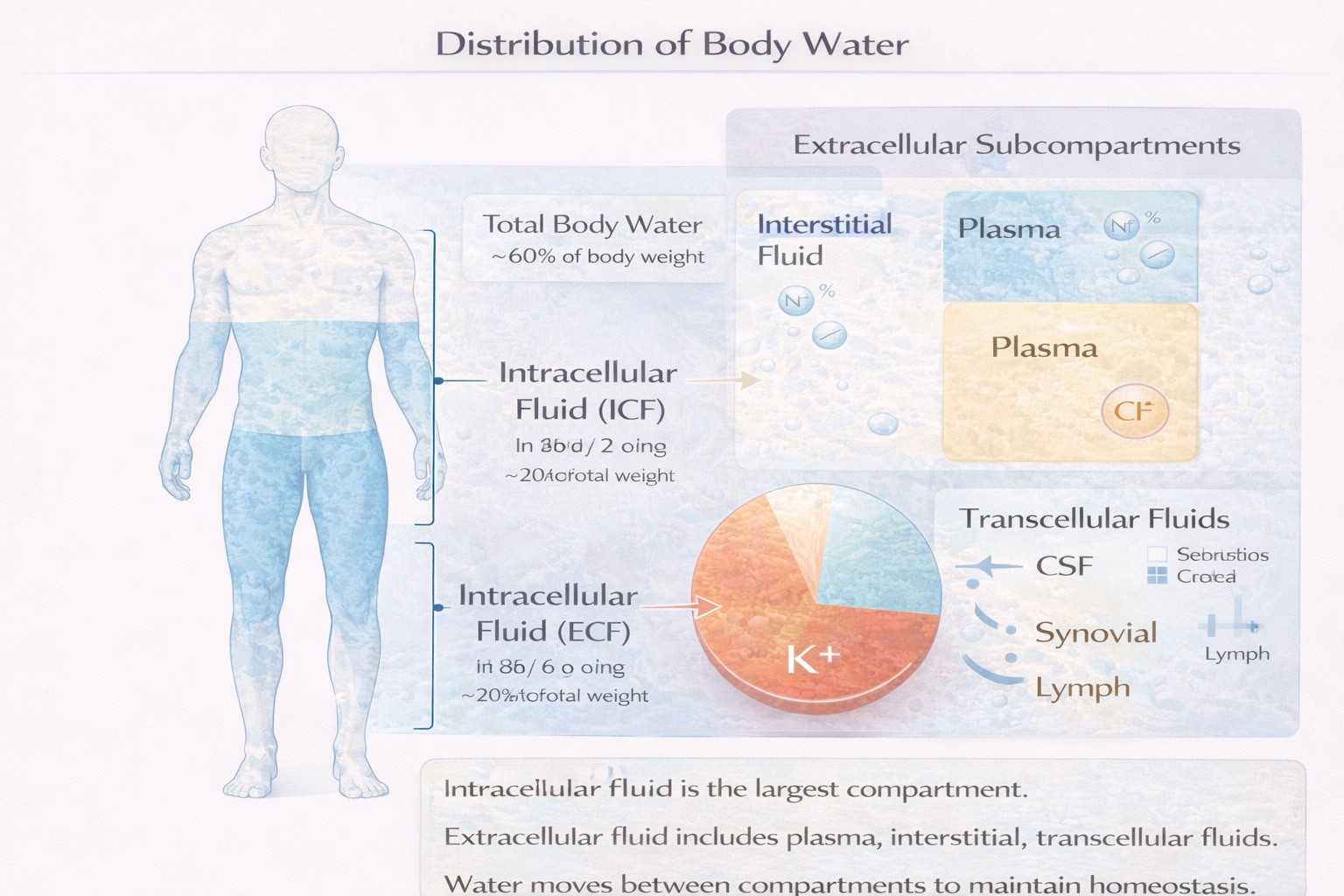
Total body water (TBW) constitutes approximately 60% of an average adult's body weight. This TBW is partitioned into two main compartments: the intracellular fluid (ICF) inside all cells and the extracellular fluid (ECF) outside cells. The ICF is the larger compartment, accounting for about two-thirds of the TBW (or roughly 40% of total body weight). The remaining one-third of the TBW is the ECF, which includes interstitial fluid, blood plasma, lymph, and transcellular fluids (e.g., cerebrospinal, synovial fluid). This one-third of TBW equates to approximately 20% of total body weight.
(A) intracellular fluid compartment: The intracellular fluid compartment is the largest, comprising about two-thirds of total body water, which translates to roughly 40% of body weight. This is twice the proportion stated in the question.
(B) extracellular fluid compartment: The EFC encompasses all fluid outside of cells and accounts for the remaining one-third of total body water, or about 20% of body weight, matching the description "roughly one-third."
(C) kidneys: The kidneys are organs that filter blood and produce urine but constitute only a very small percentage of total body mass and fluid volume. They are not a primary fluid compartment.
(D) plasma: Plasma is the liquid component of blood and is a sub-compartment of the ECF. It represents only about one-fourth of the total ECF volume, equating to roughly 5% of body weight, which is significantly less than one-third.
Conclusion
The extracellular fluid compartment, which includes all fluids outside of cells, accounts for approximately one-third of the body's total water content and about 20% of total body weight.
Which of the following hormones regulates the level of sodium and potassium?
A.
aldosterone
B. calcitonin
C. epinephrine
D. melatonin
Rationale
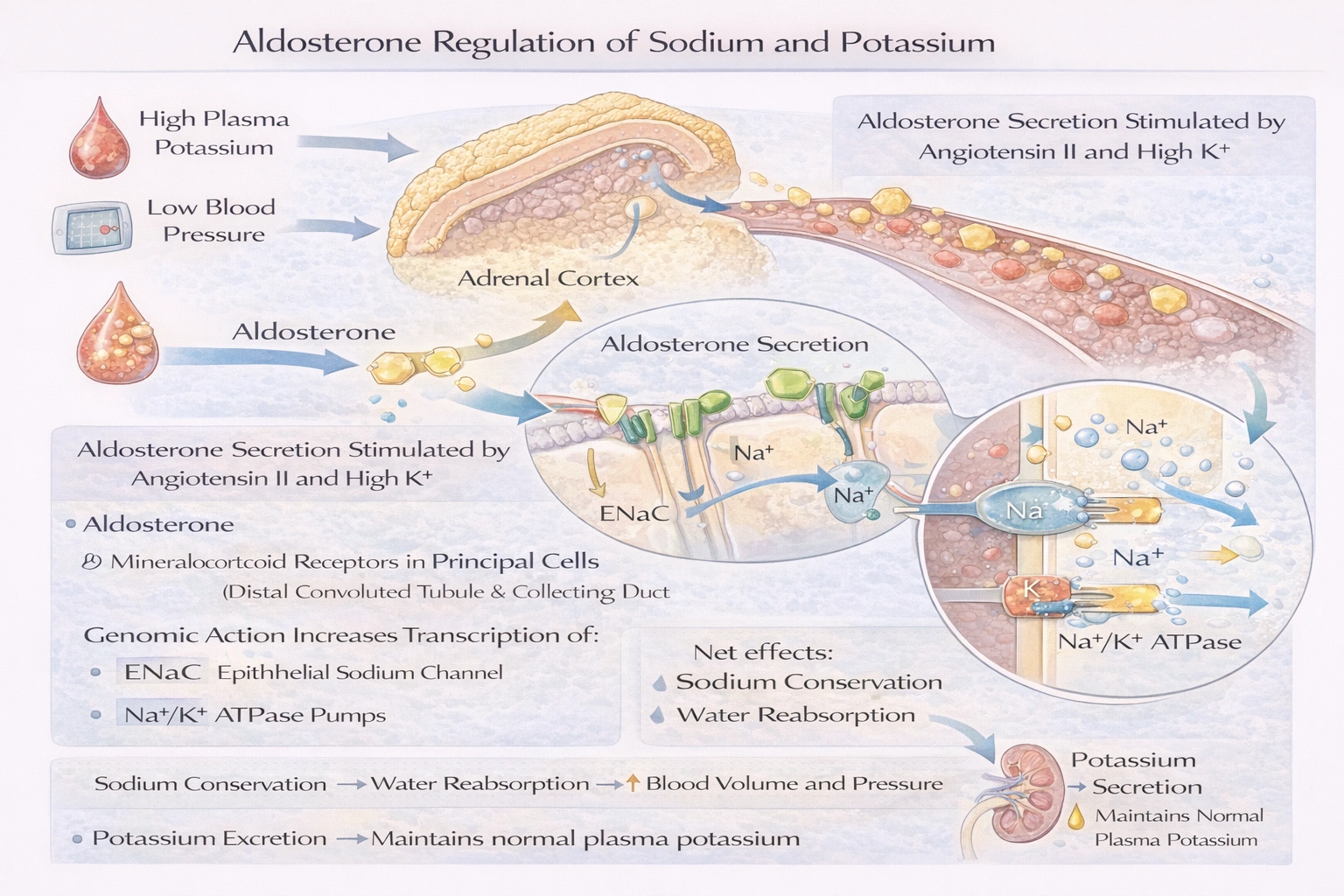
Aldosterone regulates the level of sodium and potassium.
Aldosterone is the primary mineralocorticoid steroid hormone produced in the zona glomerulosa of the adrenal cortex. Its synthesis and secretion are predominantly regulated by the renin-angiotensin system and directly by elevated plasma potassium levels. Angiotensin II, formed from angiotensin I by angiotensin-converting enzyme, binds to receptors on zona glomerulosa cells, activating phospholipase C and increasing intracellular calcium, which stimulates aldosterone synthase activity. High extracellular potassium directly depolarizes these cells, opening voltage-gated calcium channels and also stimulating aldosterone production. Once released, aldosterone circulates bound to albumin and transcortin. It acts on principal cells in the distal nephron's distal convoluted tubule and cortical collecting duct. Being lipid-soluble, it diffuses into the cell and binds to the cytosolic mineralocorticoid receptor. The hormone-receptor complex translocates to the nucleus, acting as a transcription factor to upregulate genes encoding for the epithelial sodium channel (ENaC), the Na+/K+ ATPase pump, and various mitochondrial enzymes involved in ATP production. Increased ENaC insertion into the apical membrane enhances sodium reabsorption from the tubular filtrate. The electrochemical gradient created by sodium reabsorption drives the secretion of potassium (via ROMK channels) and protons (via H+ ATPases) into the lumen. The Na+/K+ ATPase on the basolateral side actively pumps the reabsorbed sodium into the interstitium and imports potassium into the cell, maintaining the gradient. Thus, aldosterone's net effect is the conservation of sodium (and concomitant passive water reabsorption, affecting blood volume and pressure) and the excretion of potassium.
(A) aldosterone: Aldosterone's action is not limited to the kidney; it also affects sodium and potassium transport in sweat glands, salivary glands, and the colon. The hormone's specificity for the mineralocorticoid receptor is protected in the kidney by the enzyme 11β-hydroxysteroid dehydrogenase type 2, which inactivates cortisol that would otherwise bind to the same receptor. Disorders of aldosterone function, such as Conn's syndrome (primary hyperaldosteronism) or Addison's disease (adrenal insufficiency), lead to profound dysregulation of sodium and potassium levels, manifesting as hypertension with hypokalemia or hypotension with hyperkalemia, respectively.
(B) calcitonin: Calcitonin is a 32-amino acid peptide hormone secreted by the parafollicular C-cells of the thyroid gland. Its main physiological role in humans is modest and primarily involved in post-prandial calcium homeostasis. It acts by binding to receptors on osteoclasts, inhibiting their resorptive activity, thereby reducing calcium efflux from bone. In the kidney, it increases excretion of calcium, phosphate, sodium, and potassium, but this is a minor, pharmacologically exploitable effect rather than a primary regulatory one. Calcitonin does not participate in the fine, homeostatic control of sodium and potassium balance; its role is overshadowed by parathyroid hormone in calcium regulation.
(C) epinephrine: Epinephrine is a catecholamine hormone and neurotransmitter synthesized in the adrenal medulla from tyrosine. Released during acute stress via sympathetic nervous system activation, it acts on alpha and beta-adrenergic receptors. Its effects are systemic: increasing heart rate, cardiac output, and bronchodilation, and mobilizing glucose and fatty acids. Concerning potassium, epinephrine (via beta-2 adrenergic receptors) stimulates the Na+/K+ ATPase, promoting a transient shift of potassium from the extracellular fluid into cells, which can lower plasma potassium levels acutely. However, this is a rapid, transient pharmacodynamic effect, not a sustained homeostatic regulatory mechanism for total body potassium or sodium content. The long-term regulation of these electrolytes is managed by aldosterone and renal mechanisms.
(D) melatonin: Melatonin is an indoleamine hormone derived from tryptophan, synthesized primarily in the pineal gland. Its production is tightly controlled by the suprachiasmatic nucleus, the body's master circadian clock, and is suppressed by light. Melatonin's key functions are to convey information about photoperiod length, thereby regulating circadian rhythms, sleep onset, seasonal reproduction, and immune modulation. Its receptors (MT1 and MT2) are found in various tissues, but there is no established pathway through which melatonin directly influences renal sodium or potassium handling or systemic electrolyte balance.
Conclusion: Aldosterone stands as the definitive hormonal regulator of sodium and potassium homeostasis, exerting its effects through genomic mechanisms in target renal cells to promote sodium conservation and potassium excretion, a process vital for maintaining blood pressure, extracellular fluid volume, and cellular membrane potential.
Appetite, regulation of body weight, body temperature, and water balance are associated with which of the following glands?
A.
adrenal
B. hypothalamus
C. parathyroid
D. posterior lobe of the pituitary
Rationale
Appetite, regulation of body weight, body temperature, and water balance are associated with the hypothalamus.
The hypothalamus is a small but supremely complex region of the diencephalon, situated below the thalamus and forming the floor and part of the lateral walls of the third ventricle. It is the primary integration center for homeostasis, linking the autonomic nervous system and the endocrine system. Its functions are localized to specific nuclei:
Appetite & Body Weight: The arcuate nucleus contains two key neuron populations: one co-expressing neuropeptide Y and agouti-related peptide (NPY/AgRP) that stimulates hunger, and another expressing pro-opiomelanocortin (POMC, cleaved to alpha-MSH) that promotes satiety. These neurons integrate peripheral signals like leptin (from adipose tissue), ghrelin (from the stomach), insulin, and peptide YY. They project to the lateral hypothalamus (hunger center, producing orexin) and ventromedial hypothalamus (satiety center), regulating food intake and energy expenditure.
Body Temperature: The preoptic area of the anterior hypothalamus contains thermosensitive neurons that act as the body's thermostat. In response to warming, they trigger heat-loss mechanisms (vasodilation, sweating). In response to cooling, they activate heat-conservation/generation mechanisms (vasoconstriction, shivering thermogenesis, non-shivering thermogenesis via brown adipose tissue).
Water Balance: The supraoptic and paraventricular nuclei contain osmoreceptor cells that monitor plasma osmolality. They stimulate thirst and also synthesize vasopressin (ADH), which is transported to the posterior pituitary for release. Circumventricular organs like the subfornical organ and organum vasculosum of the lamina terminalis, which lack a complete blood-brain barrier, also detect angiotensin II and hypertonicity to drive thirst and ADH release.
The hypothalamus executes these functions through outputs to the pituitary gland (releasing hormones into the hypophyseal portal system for anterior pituitary control, and axonal projections for posterior pituitary hormone release), the autonomic nervous system (via brainstem and spinal cord projections), and behavioral drives.
(A) adrenal: The adrenal glands are peripheral endocrine organs that execute commands from higher centers. While hormones like cortisol (adrenal cortex) can influence metabolism and appetite indirectly, and epinephrine (adrenal medulla) can affect thermogenesis, these glands do not contain the integrative neural circuits that sense body state, compute set points, and initiate coordinated behavioral and physiological responses. They act as effectors in larger regulatory loops controlled by the hypothalamus and pituitary.
(B) hypothalamus: As described, the hypothalamus is the central processing unit for homeostasis. Its nuclei receive a constant stream of neural input (e.g., from the brainstem's nucleus tractus solitarius carrying visceral sensory information) and hormonal feedback. It compares this information to physiological set points and orchestrates efferent responses via both neural (autonomic) and hormonal (pituitary) pathways. Its role in these four processes is direct, integrative, and indispensable.
(C) parathyroid: The parathyroid glands have a single, highly specialized function: the regulation of blood calcium levels via PTH secretion. Their activity is controlled directly by plasma ionized calcium concentration acting on their calcium-sensing receptors. They play no part in the neural integration of appetite, body weight, temperature, or overall water balance. They are not connected to the central neural networks that govern these complex homeostatic parameters.
(D) posterior lobe of the pituitary: The posterior pituitary (neurohypophysis) is an anatomical extension of the hypothalamus, composed of the axonal terminals of hypothalamic neurons. It stores and releases oxytocin and vasopressin, but it does not synthesize these hormones nor does it make regulatory decisions. It is a storage and release depot. The crucial integrative functions sensing osmolality for water balance, receiving metabolic signals for appetite occur within the hypothalamic nuclei themselves (e.g., supraoptic, paraventricular, arcuate). Therefore, while it is involved in the execution of water balance via ADH release, the regulation and association with the other listed functions reside in the hypothalamus.
Conclusion: The hypothalamus is the master neural coordinator for fundamental homeostatic processes, housing specialized nuclei that directly regulate appetite and body weight through integration of metabolic signals, body temperature through thermoreception and effector control, and water balance through osmoreception and ADH/thirst mechanisms, making it the correct association for all the listed functions.
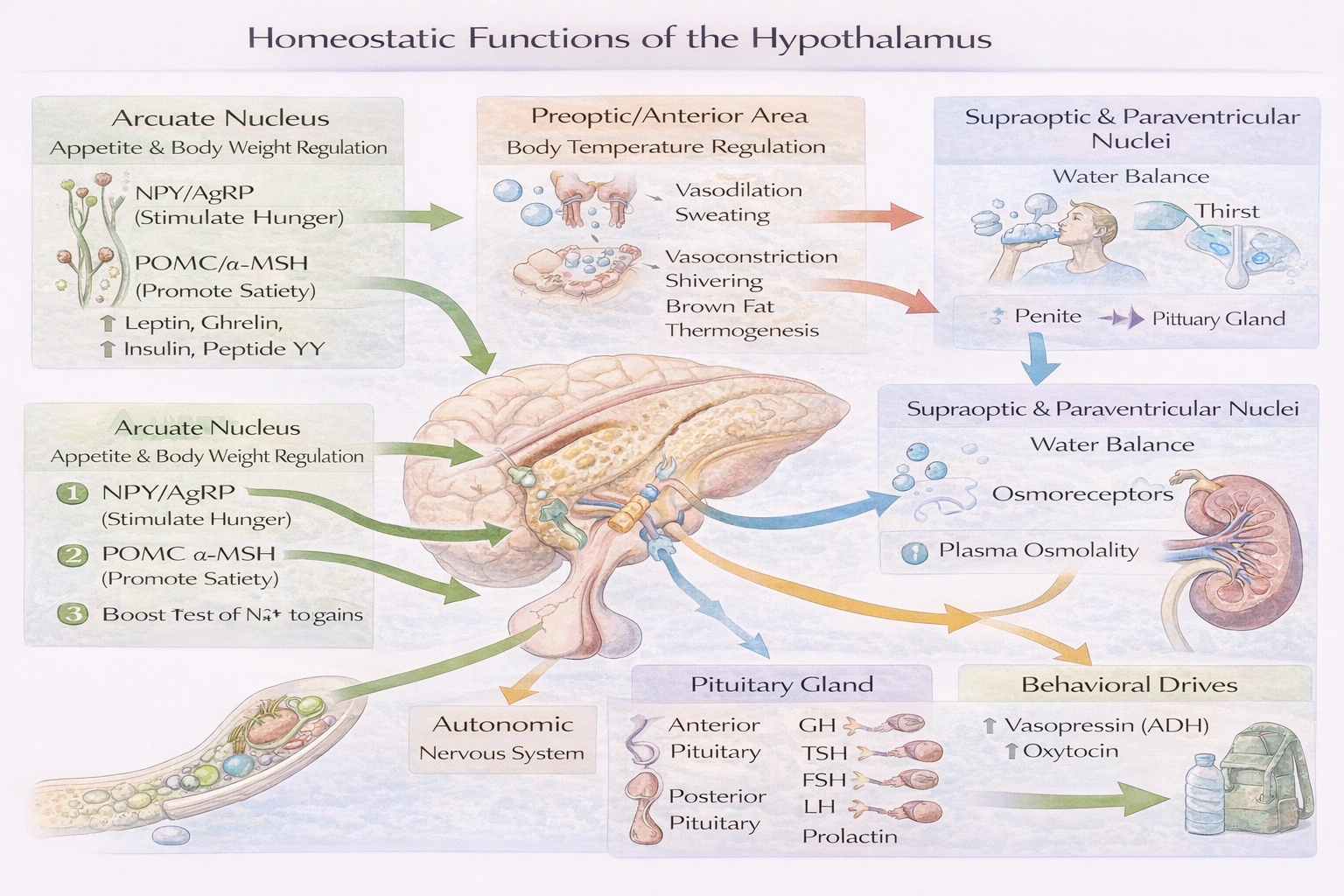
Select the true statement regarding the digestive process.
A.
mouth → esophagus → stomach → small intestine → large intestine → anus
B. mouth → esophagus → stomach → small intestine → large intestine → anus
C. mouth → pharnyx → stomach → small intestine → large intestine → anus
D. mouth → esophagus → stomach → small intestine → appendix → large intestine → anus
Rationale
The true statement regarding the digestive process is: mouth → esophagus → stomach → small intestine → large intestine → anus.
The human digestive process follows a strict, unidirectional anatomical and physiological pathway known as the alimentary canal or gastrointestinal (GI) tract. This continuous muscular tube begins at the mouth and ends at the anus, with each specialized segment performing sequential functions. The process initiates with ingestion and mechanical breakdown (mastication) in the mouth. The bolus is then propelled through the pharynx during swallowing (deglutition) and enters the esophagus, which conducts it via peristalsis to the stomach. In the stomach, mechanical churning and chemical digestion (primarily of proteins) occur, converting the bolus into a semi-liquid mixture called chyme. The chyme is then released in controlled amounts through the pyloric sphincter into the small intestine (duodenum, jejunum, ileum), where the vast majority of enzymatic digestion and nutrient absorption takes place, aided by secretions from the liver, gallbladder, and pancreas. The remaining indigestible material, water, and electrolytes then pass through the ileocecal valve into the large intestine (cecum, colon, rectum). Here, water and ions are reabsorbed, transforming the liquid residue into semisolid feces, which are stored until elimination via the anus during defecation. This sequence is non-reversible due to coordinated peristaltic movements and strategically placed sphincters (e.g., lower esophageal, pyloric, ileocecal, anal) that prevent backflow and compartmentalize functions.
(A) mouth → esophagus → stomach → small intestine → large intestine → anus. The bidirectional arrow (→) between the small and large intestine is physiologically false. The ileocecal valve, a functional sphincter at the junction of the ileum (last part of small intestine) and cecum (first part of large intestine), strictly regulates unidirectional flow. It allows ileal contents to enter the cecum but prevents the reflux of colonic material which contains high bacterial loads and potentially pathogenic organisms back into the relatively sterile small intestine. Retrograde movement would lead to bacterial overgrowth and significant pathology.
(B) mouth → esophagus → stomach → small intestine → large intestine → anus. This sequence is anatomically and functionally correct. It accurately depicts the linear progression of ingested material through the primary organs of the GI tract, each with a defined role in processing, digestion, absorption, and finally, excretion. No steps are omitted or out of order, and the directional flow is correctly represented with single-headed arrows.
(C) mouth → pharnyx → stomach → small intestine → large intestine → anus. While the pharynx is indeed a critical structure involved in the voluntary and involuntary phases of swallowing, it is not typically enumerated as a separate, discrete digestive organ in the sequential list of the alimentary canal where digestion and absorption occur. More importantly, the spelling "pharnyx" is a non-standard variant; the correct anatomical term is pharynx. Furthermore, this sequence omits the esophagus, which is the essential muscular tube connecting the pharynx to the stomach. The pharynx passes the bolus to the esophagus; it does not connect directly to the stomach.
(D) mouth → esophagus → stomach → small intestine → appendix → large intestine → anus. This pathway erroneously includes the appendix (vermiform appendix) as a conduit through which digestive material passes. The appendix is a blind-ended tubular diverticulum attached to the posteromedial aspect of the cecum. It is considered a lymphoid organ involved in immune surveillance and possibly serving as a reservoir for gut flora, but it is not part of the continuous flow of luminal contents. Ingested material does not enter or traverse the appendix under normal physiological conditions; it is a cul-de-sac.
Conclusion: The correct, linear, and unidirectional pathway of the digestive tract from ingestion to elimination is definitively represented by option (B): mouth, esophagus, stomach, small intestine, large intestine, and anus.
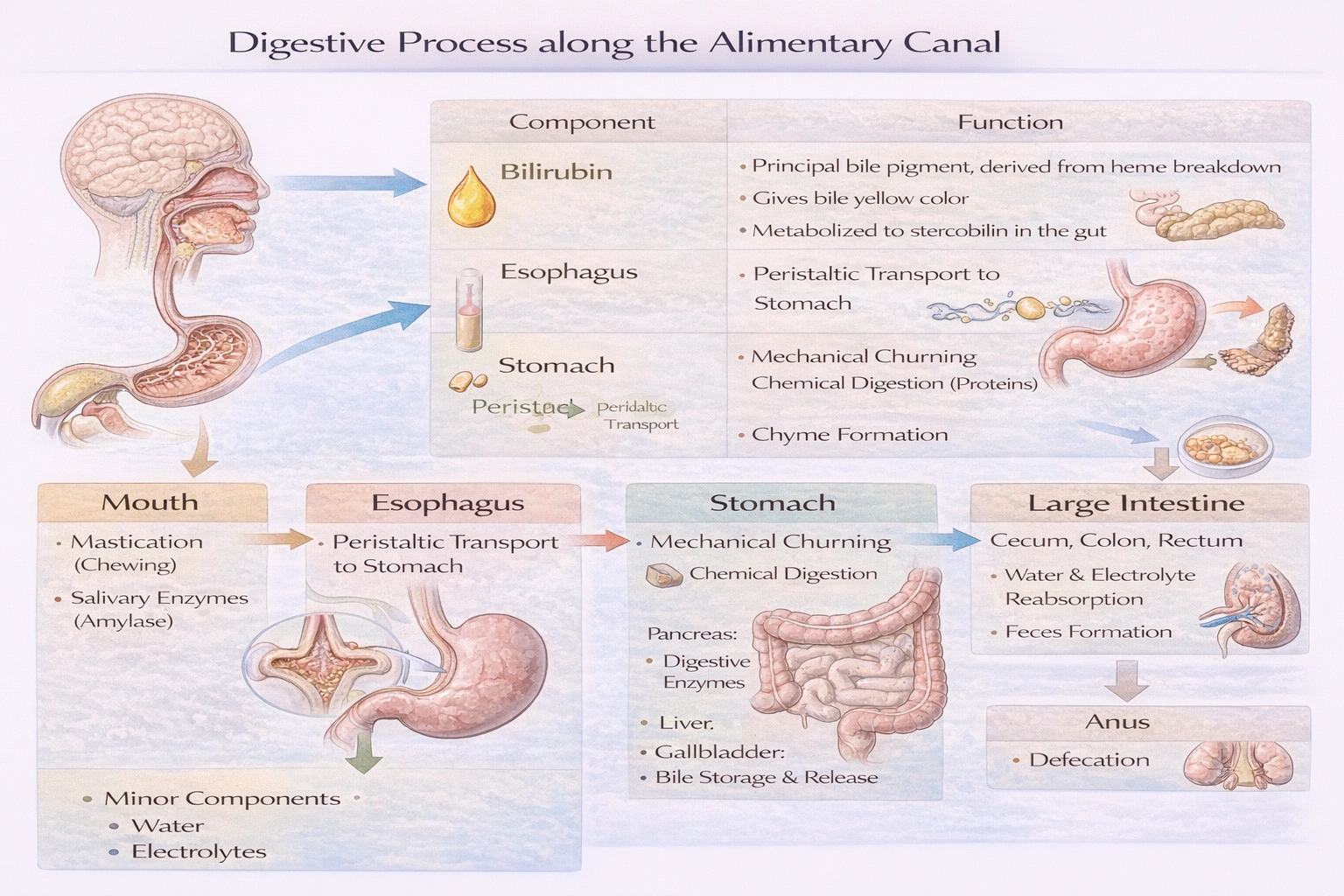
Chemical digestion of food begins in the
A.
esophagus.
B. mouth.
C. pharynx.
D. stomach.
Rationale
Chemical digestion of food begins in the mouth.
Chemical digestion refers to the enzymatic hydrolysis of complex food macromolecules into simpler, absorbable subunits. This process is unequivocally initiated in the oral cavity through the action of saliva, secreted by the major and minor salivary glands. Saliva contains two key digestive enzymes: salivary amylase (ptyalin) and lingual lipase. Salivary amylase catalyzes the cleavage of internal α-1,4 glycosidic bonds in starch (amylose and amylopectin) and glycogen, producing smaller oligosaccharides like maltose, maltotriose, and α-limit dextrins. This enzyme functions optimally at the slightly acidic to neutral pH (6.2-7.4) of the mouth. Lingual lipase, secreted by serous glands (von Ebner's glands) on the dorsum of the tongue, begins the digestion of triglycerides, hydrolyzing them into fatty acids and diglycerides; its activity is sustained and even enhanced in the acidic environment of the stomach. The mechanical process of mastication not only reduces particle size but also creates a vast surface area and ensures thorough mixing with saliva, forming a cohesive bolus. While no significant absorption occurs here, the oral phase is critical for launching the chemical digestion of carbohydrates and fats, reducing the metabolic load on subsequent digestive organs.
(A) esophagus. The esophagus is a muscular tube lined with non-keratinized stratified squamous epithelium. Its function is strictly transport. The secretions from its submucosal mucous glands are solely for lubrication and epithelial protection against mechanical abrasion during peristaltic transit. It contains no enzymatic secretions capable of hydrolyzing carbohydrates, proteins, or lipids. The bolus passes through the esophagus within seconds via primary and secondary peristalsis, undergoing no chemical alteration whatsoever.
(B) mouth. As detailed, the mouth is the correct and initial site. The presence of salivary amylase and lingual lipase provides the biochemical basis for the commencement of digestion. This initial step is not trivial; it can account for up to 30-40% of starch digestion before the enzyme is inactivated by stomach acid. The digestion of triglycerides also starts here, albeit to a lesser initial extent. The oral phase represents the first step in the alimentary canal's enzymatic cascade.
(C) pharynx. The pharynx (throat) is a common muscular passage for both the digestive and respiratory tracts. During the brief pharyngeal phase of swallowing (deglutition), it functions to rapidly propel the bolus from the oropharynx into the esophagus while simultaneously preventing aspiration through the closure of the laryngeal inlet (via elevation of the larynx, folding of the epiglottis, and closure of the vocal folds). It is involved purely in the mechanical process of propulsion and provides no digestive secretions. Its epithelium is protective stratified squamous, not secretory columnar epithelium.
(D) stomach. The stomach is a primary site for the chemical digestion of proteins (via pepsin) and, to a lesser extent, fats (via gastric lipase and the continued action of lingual lipase). However, it is not the initial site. By the time food reaches the stomach, carbohydrate digestion has already been initiated by salivary amylase. The stomach's low pH (1.5-3.5) serves to denature proteins, activate pepsinogen to pepsin, and kill ingested microbes, but it also rapidly inactivates salivary amylase. Thus, while the stomach is a major digestive organ, chemical digestion begins earlier, in the oral cavity.
Conclusion: The oral cavity, through the enzymatic action of salivary amylase and lingual lipase, is the physiological starting point for the chemical digestion of food, specifically targeting dietary carbohydrates and fats.
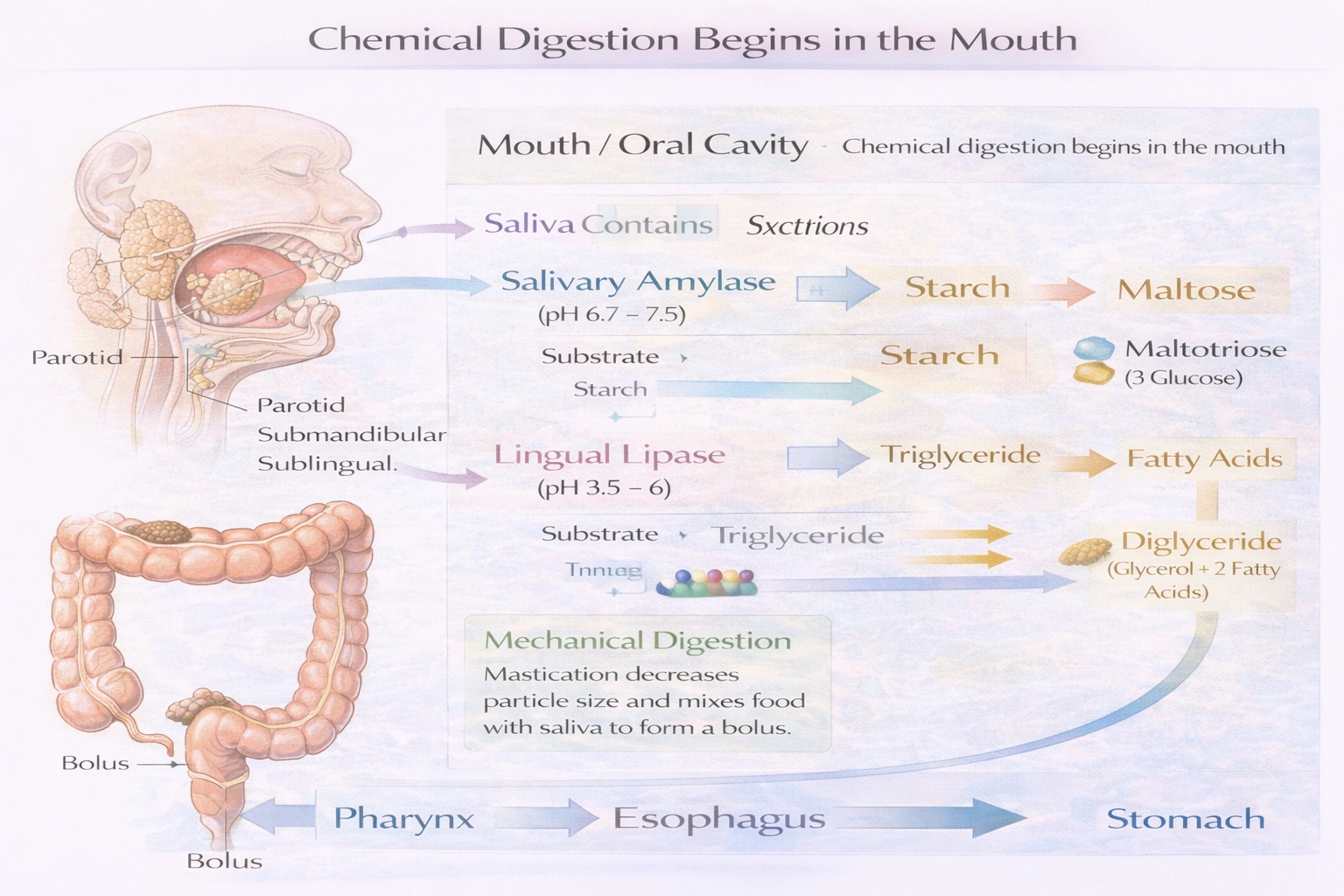
What percentage of digestion occurs in the esophagus?
A.
0%
B. 5-8%
C. 9-11%
D. depends upon the fiber content of the partially digested food
Rationale
The percentage of digestion that occurs in the esophagus is 0%.
In human physiology, "digestion" specifically refers to the breakdown of food, encompassing both mechanical and chemical processes. Chemical digestion, which is quantifiable by the enzymatic hydrolysis of macromolecules, is the relevant metric for this question.
The esophagus is anatomically and functionally designed solely for transport. Its mucosal lining is stratified squamous epithelium, suited for protection against abrasion but not for secretion or absorption. The esophageal glands within the submucosa secrete mucus exclusively for lubrication, facilitating the smooth passage of the bolus via peristaltic waves. Crucially, the esophagus lacks any specialized secretory cells (such as the chief cells of the stomach or the acinar cells of the pancreas) that produce digestive enzymes like amylases, proteases, lipases, or nucleases. The bolus transits the esophagus rapidly (typically within 5-10 seconds), during which its chemical composition remains identical to when it entered from the pharynx. No enzymatic activity acts upon the carbohydrates, proteins, or fats within the esophageal lumen. Therefore, the esophagus contributes 0% to the chemical digestion of food. Its role is exclusively mechanical propulsion.
(A) 0%. This is the physiologically accurate and definitive answer. The esophagus's structure precludes any participation in the chemical digestive process. It is a conduit, not a digestive organ, and serves only to connect the pharynx to the stomach.
(B) 5-8% and (C) 9-11%. These numerical ranges are entirely without foundation in human digestive physiology. No credible research or standard physiological textbook attributes any measurable percentage of nutrient hydrolysis to the esophagus. Such percentages may stem from a fundamental misunderstanding of esophageal function or confusion with other segments like the stomach (where 20-30% of protein digestion might occur) or the small intestine (where the majority of digestion takes place).
(D) depends upon the fiber content of the partially digested food. Dietary fiber (soluble or insoluble) influences several aspects of GI physiology, including gastric emptying rate, colonic transit time, stool bulk, and bacterial fermentation in the colon. However, it has absolutely no bearing on the esophagus's function. The esophagus performs identical transport regardless of bolus composition. Furthermore, humans lack enzymes to digest most dietary fiber (e.g., cellulose, hemicellulose), so even if the esophagus secreted enzymes (which it does not), fiber content would not alter a "percentage of digestion" occurring there. The statement is physiologically irrelevant to esophageal function.
Conclusion: The esophagus serves exclusively as a transit tube with no enzymatic secretory function, thus contributing 0% to the chemical digestion of food.
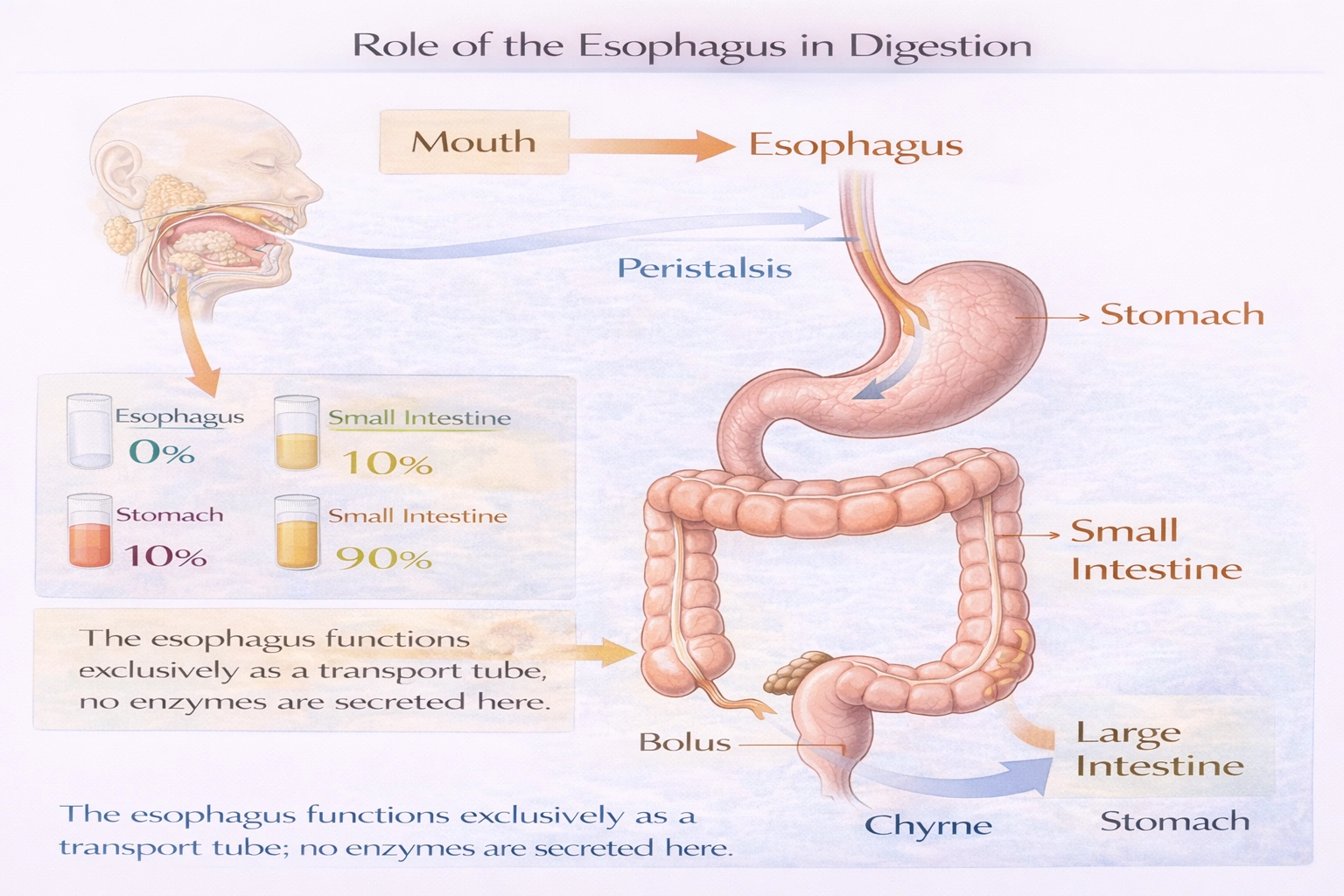
HESI A2 Exams
Biology Quizzes
3 Practice Tests
Biology Quizzes
3 Practice Tests
Chemistry Quizzes
3 Practice Tests
Chemistry Quizzes
3 Practice Tests
Reading Quizzes
4 Practice Tests
Reading Quizzes
4 Practice Tests
Grammar Quizzes
3 Practice Tests
Grammar Quizzes
3 Practice Tests
Vocabulary Quizzes
3 Practice Tests
Vocabulary Quizzes
3 Practice Tests
Physics Quizzes
3 Practice Tests
Physics Quizzes
3 Practice Tests
HESI Quizzes
3 Practice Tests
HESI Quizzes
3 Practice Tests