HESI A2 PRACTICE TEST ANATOMY AND PHYSIOLOGY
This HESI A2 Anatomy and Physiology practice test is built to reflect the depth and style of questions found on the exam. It tests your knowledge of body systems, anatomical structures, and physiological processes essential for nursing program entry.
Topics Covered
Body Systems
Anatomical Terminology
Homeostasis
Structure and Function
00:00
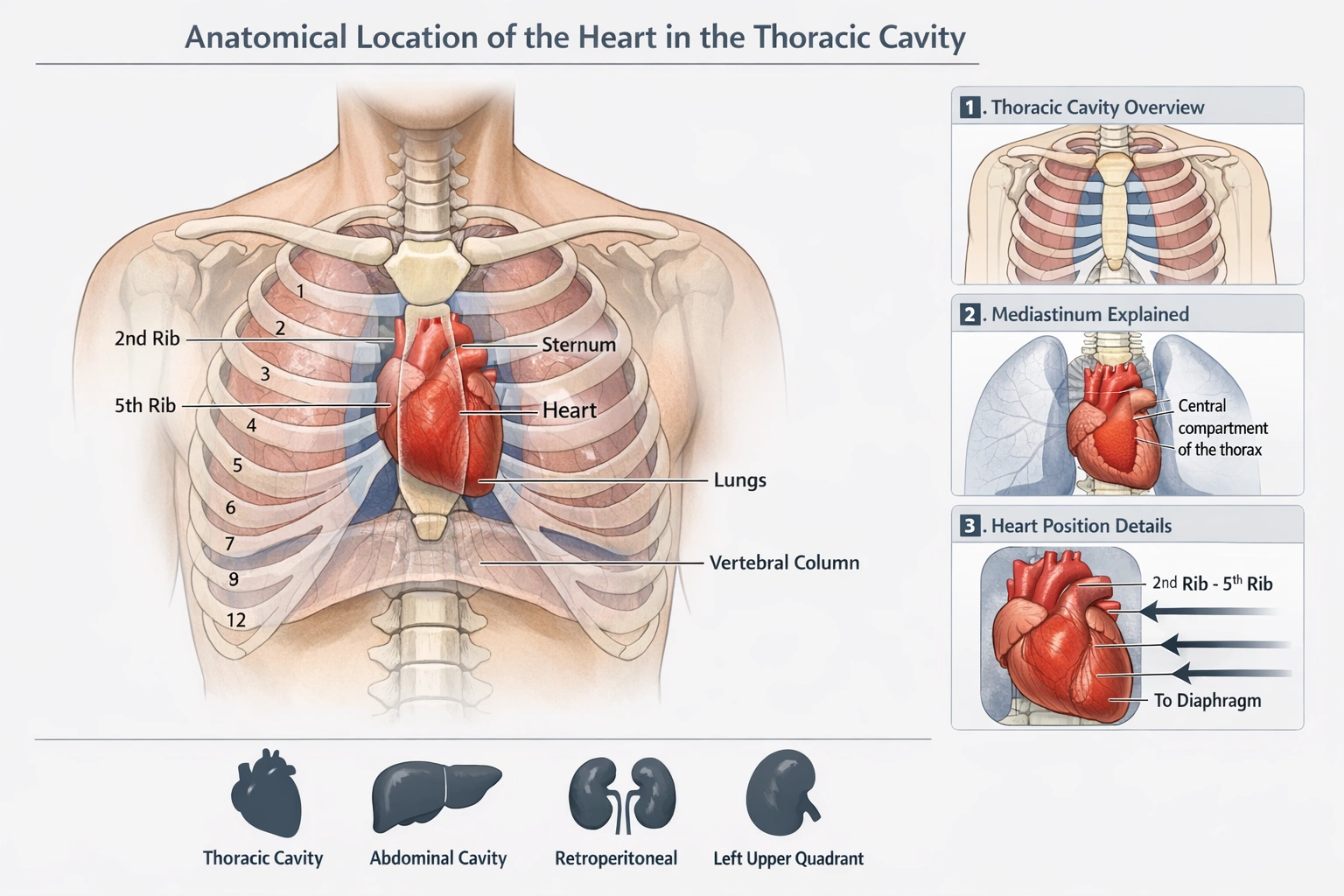
The position of the __________ is located in the mediastinum of the thorax, approximately between the second and fifth ribs. It rests on the diaphragm, lies posterior to the sternum, is bordered by the lungs that overlie it, and lies anterior to the vertebral column.
A.
heart
B. kidneys
C. liver
D. spleen
Rationale
The heart is the organ located in the mediastinum of the thorax between the second and fifth ribs.
The description specifies the mediastinum as the location which is the central compartment of the thoracic cavity it details an anatomical position between the second and fifth ribs resting on the diaphragm posterior to the sternum bordered by the lungs and anterior to the vertebral column all of these are precise and exclusive anatomical relationships of the heart whereas the kidneys liver and spleen are abdominal organs not situated in the thoracic mediastinum
A) Heart
The description in the question exactly matches the heart's anatomical position: it lies within the mediastinum, spans the area from the second to fifth ribs, sits on the diaphragm, is located behind the sternum, is flanked by the lungs, and lies in front of the thoracic vertebral column. No other organ fits this specific set of thoracic and midline relationships.
B) Kidneys
The kidneys are not located in the thorax and do not match any of the positional clues. They are retroperitoneal organs found in the posterior abdominal cavity, lateral to the upper lumbar vertebrae (approximately T12 to L3). They lie far below the diaphragm and are not associated with the second to fifth ribs, the sternum, or the mediastinum. Their placement is entirely abdominal, not thoracic.
C) Liver
The liver is primarily an abdominal organ, situated in the right upper quadrant beneath the diaphragm. While it is protected by the lower ribs (around ribs 7--11), it is not located in the mediastinum or between the second and fifth ribs. Its position is mostly to the right of the midline, not centered behind the sternum, and it does not lie anterior to the vertebral column in the manner described. The liver's abdominal location excludes it from the thoracic landmarks given.
D) Spleen
The spleen is an abdominal organ located in the left upper quadrant, tucked beneath the diaphragm and behind ribs 9--11. It lies laterally and posterolaterally, not in the midline or within the mediastinum. It has no relationship to the sternum or the second to fifth ribs, and it is not bordered by the lungs in the same central thoracic way. Its peripheral abdominal placement contradicts all the described positional cues.
Conclusion:
The question outlines a distinct set of anatomical landmarks---the mediastinum, the span from the second to fifth ribs, a position resting on the diaphragm, placement posterior to the sternum and anterior to the vertebral column, and lateral borders formed by the lungs. Only the heart satisfies every element of this description. The kidneys, liver, and spleen are all abdominal organs that fail to meet these thoracic and midline criteria, making the heart the unequivocally correct identification.
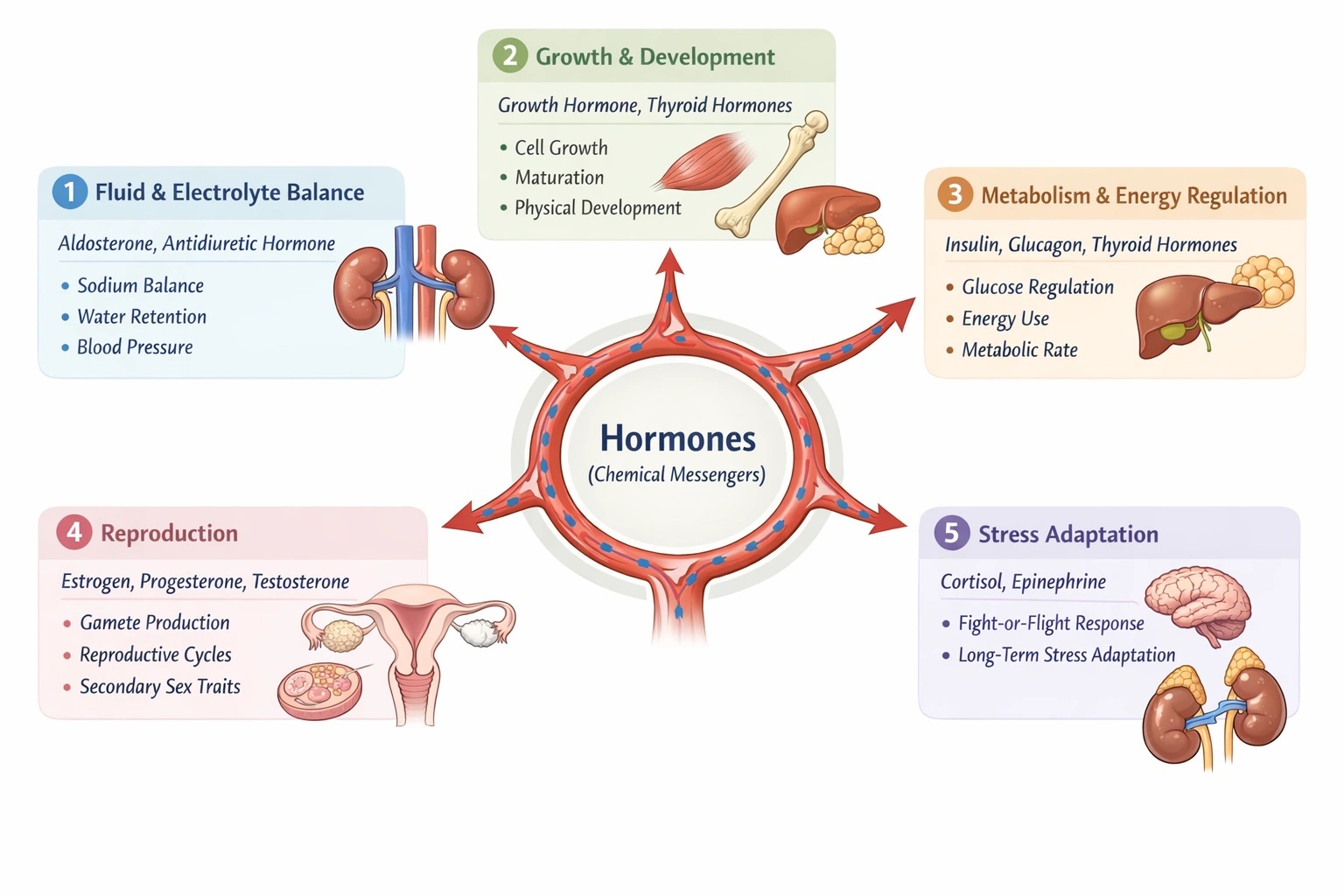
__________ regulate(s) fluid and electrolyte balance, reproduction, growth and development, adaptation to stress, and metabolism.
A.
Glands
B. Gonads
C. Hormones
D. Vasopressin
Rationale
Hormones regulate fluid and electrolyte balance, reproduction, growth and development, adaptation to stress, and metabolism.
Hormones are the signaling molecules secreted by endocrine glands that travel through the bloodstream to target organs to coordinate and regulate all the listed physiological processes while glands are the organs that produce hormones gonads are a specific type of gland primarily involved in reproduction and vasopressin is a single hormone specific to fluid balance making hormones the correct comprehensive answer.
A. Glands
Glands, such as the pituitary or adrenal glands, are the organs that synthesize and release hormones. While they are the crucial sources of these regulators, they themselves are not the regulatory signals. The statement describes the action of regulation, which is performed by the substances (hormones) the glands secrete.
B. Gonads
The gonads (testes and ovaries) are a specific type of endocrine gland. They produce sex hormones vital for reproduction and development of secondary sexual characteristics. However, their function is specialized and does not encompass the regulation of fluid balance, overall metabolism, or the body's comprehensive stress response.
C. Hormones
Hormones are the definitive signaling molecules that integrate the body's systems, acting on distant target cells to evoke precise responses that maintain homeostasis across all the listed functions.
D. Vasopressin
Vasopressin, or antidiuretic hormone (ADH), is a specific hormone that plays a critical role in regulating water retention and blood pressure. Its function is primarily limited to aspects of fluid balance. It does not have a primary role in governing reproduction, growth, development, or broad metabolic processes.
Conclusion:
The question requires the term that broadly and directly governs all the listed, diverse physiological processes. Only the general class of hormones fits this description, serving as the body's primary long-distance chemical communicators for systemic integration and control.
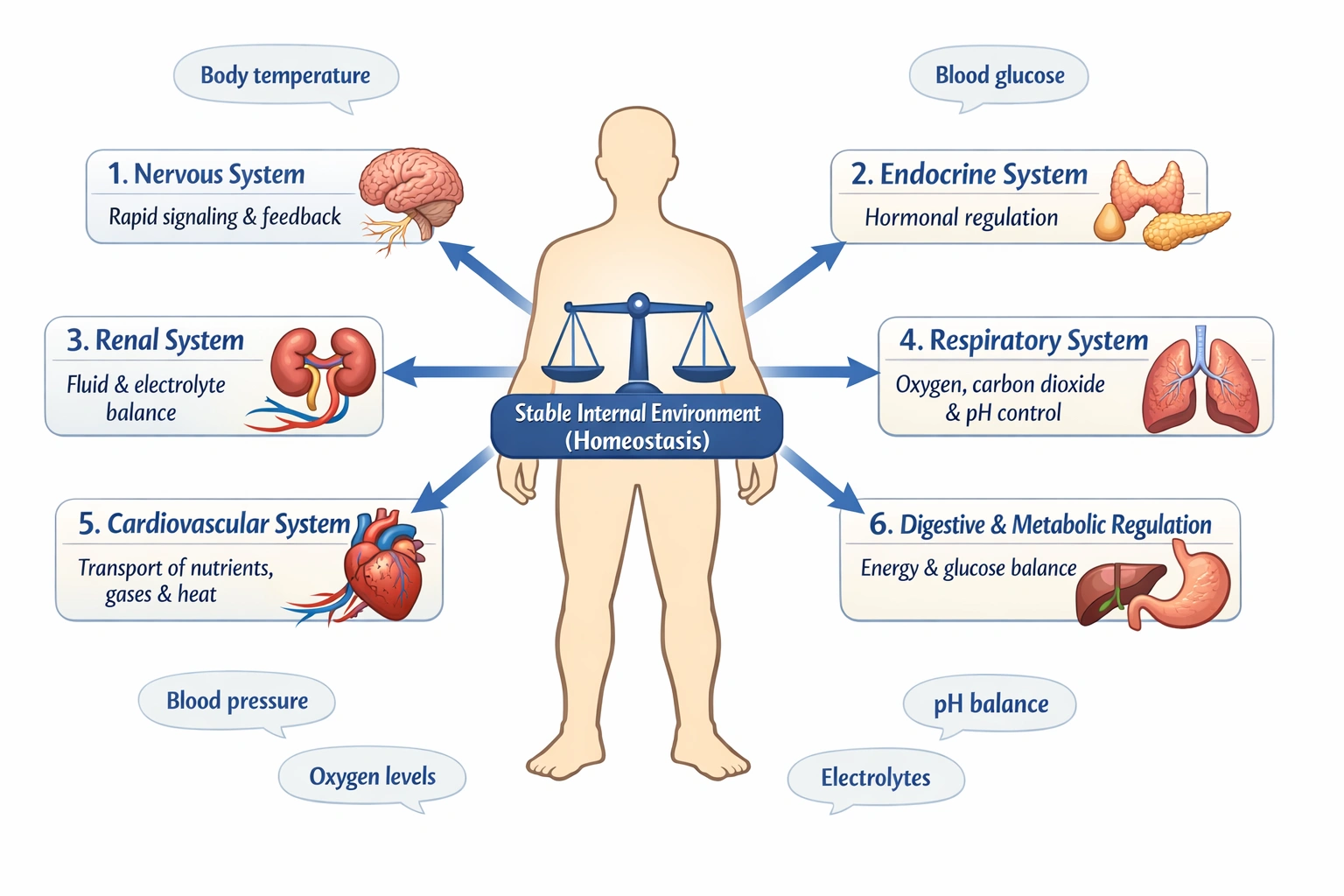
Homeostasis is a state of equilibrium
A.
where fluid balance exists when water in equals water out
B. When all solutes in the body are dissolved or suspended in water
C. When the distribution of body fluids among body fluid compartments is regulated
D. within the body when all body systems are balanced
Rationale
Homeostasis is a state of equilibrium within the body when all body systems are balanced.
It refers to the dynamic, self‑regulating process by which the body maintains a stable internal environment despite changes in external conditions. This balance involves multiple interacting systems including temperature, pH, fluid and electrolyte levels, blood pressure, and metabolism all kept within narrow, life‑sustaining ranges through feedback mechanisms..
A) Where fluid balance exists when water in equals water out
This statement accurately describes a state of fluid balance, which is one important component of homeostasis. However, it is too limited in scope. Homeostasis encompasses the regulation of all bodily systems, not merely the intake and output of water.
B) When all solutes in the body are dissolved or suspended in water
This describes the physical medium of body fluids that solutes are carried in water. While true, this is a passive description of composition and does not refer to the active, regulatory processes that characterize homeostasis.
C) When the distribution of body fluids among body fluid compartments is regulated
This describes a specific homeostatic process, namely osmoregulation, which maintains fluid balance between intracellular and extracellular compartments. It is a vital example of homeostasis in action but represents only one of many such regulatory systems.
D) Within the body when all body systems are balanced
It captures the comprehensive essence of homeostasis as the maintenance of a stable internal state through the integrated, balanced function of all the body's systems, including nervous, endocrine, circulatory, and renal systems.
Conclusion:
Homeostasis is the fundamental physiological concept of maintaining a stable internal environment. While fluid balance and solute distribution are specific examples of homeostatic control, the term itself refers to the overall, systemic balance of all bodily functions. Therefore, the correct and most complete definition is that homeostasis is a state of equilibrium within the body when all body systems are balanced.
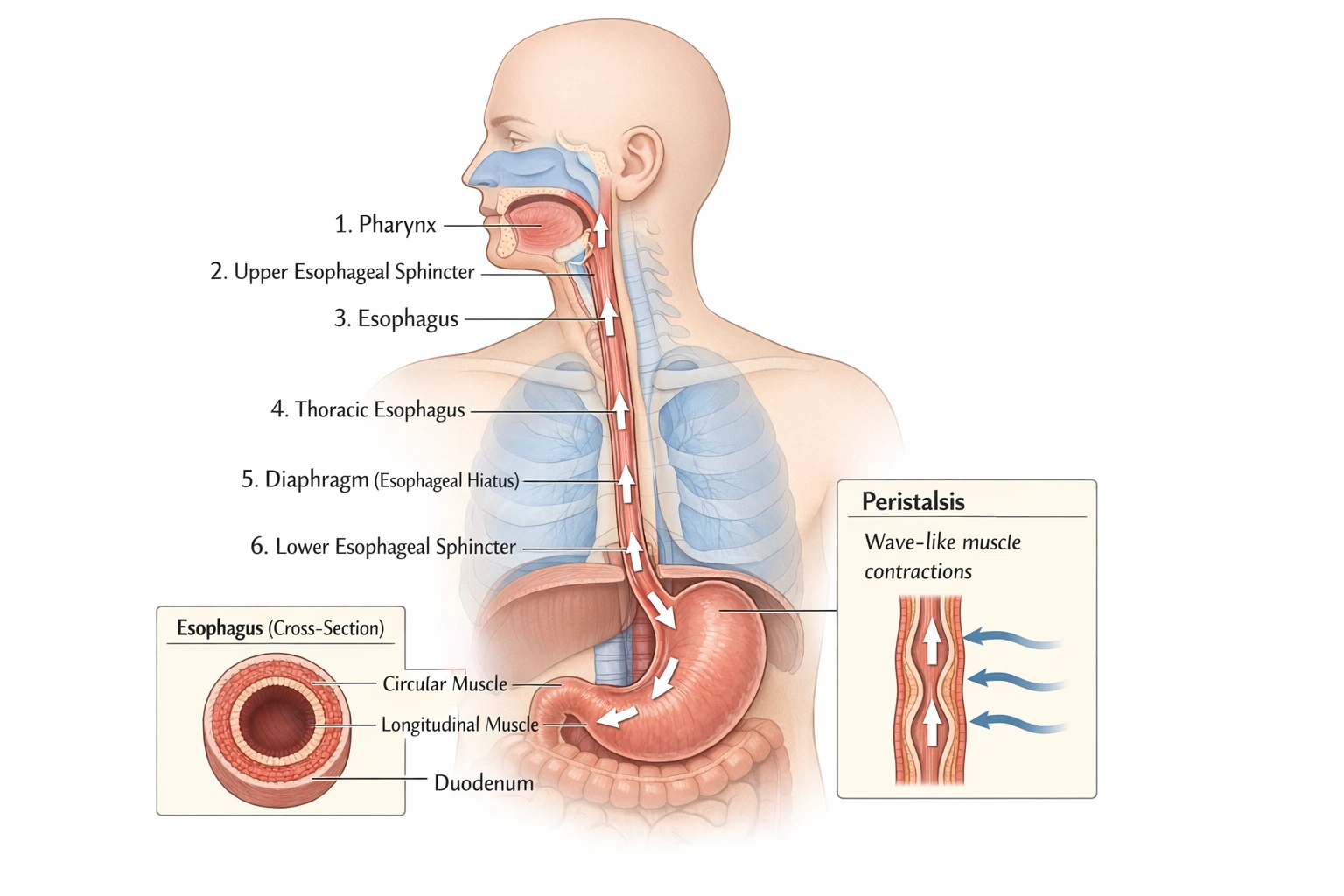
Which of the following is essential for absorption of vitamin B12 in the small intestine?
A.
amylase
B. chyme
C. hydrochloric acid
D. intrinsic factor
Rationale
Intrinsic factor is a glycoprotein essential for the absorption of vitamin B12 in the small intestine.
Secreted by the parietal cells of the gastric mucosa, it binds specifically to dietary B12 in the duodenum. This binding forms a complex that protects the vitamin from degradation and allows it to be recognized and absorbed by specific receptor sites in the terminal ileum. Without intrinsic factor, vitamin B12 cannot be absorbed, leading to deficiency regardless of dietary intake, as seen in conditions like pernicious anemia.
A) Amylase
Amylase is a digestive enzyme secreted by the salivary glands and pancreas. Its sole function is to catalyze the breakdown of starch into simpler sugars. It plays no role in the binding, transport, or absorption mechanisms of vitamin B12 within the gastrointestinal tract.
B) Chyme
Chyme is the semi-fluid mass of partially digested food and gastric secretions that passes from the stomach into the small intestine. While it is the vehicle that carries vitamin B12 into the duodenum, chyme itself is not a specific agent of absorption. Its presence is a condition of digestion but not the essential factor for B12 uptake.
C) Hydrochloric acid
Hydrochloric acid, secreted by the stomach's parietal cells, plays an important preliminary role. It denatures dietary proteins, thereby releasing bound vitamin B12 so it becomes bioavailable. However, this acidic environment alone is insufficient for absorption. The liberated B12 must still bind with intrinsic factor for successful uptake, making hydrochloric acid a necessary preparatory agent but not the essential absorbing factor.
D) Intrinsic factor
Intrinsic factor is the specific glycoprotein whose presence is absolutely required for the physiological absorption of vitamin B12. It acts as a binding and escort protein, facilitating the vitamin's transport through the intestinal lumen and its subsequent receptor-mediated endocytosis in the ileum. No other substance can substitute for this function.
Conclusion:
The question asks for the element that is essential for vitamin B12 absorption in the small intestine. While hydrochloric acid prepares the vitamin for absorption, only intrinsic factor directly enables its uptake into the bloodstream. Therefore, the correct and essential factor is intrinsic factor
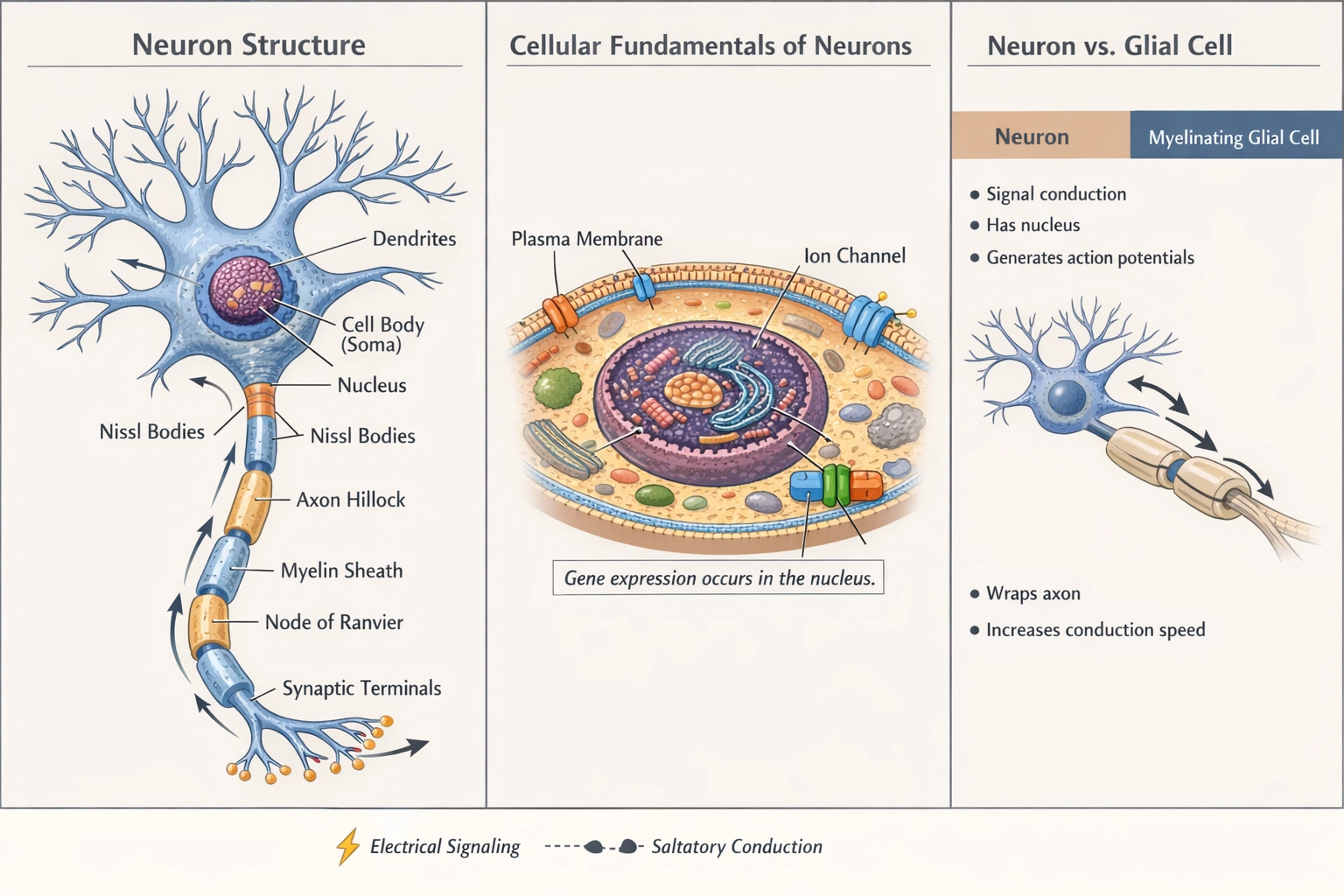
Neurons
A.
contain no special structures
B. have a nucleus that contains genes
C. have no cell membrane
D. speed conduction time along nerve fibers
Rationale
Neurons, like all eukaryotic cells, possess a nucleus that houses the cell's genetic material.
This nucleus, located within the cell body or soma, contains the DNA that encodes the genes necessary for neuronal function, including the synthesis of proteins vital for neurotransmitter production, cellular maintenance, and signaling. This is a foundational cellular characteristic, not unique to neurons but essential for their survival and specialized activities.
A) Contain no special structures
This statement is incorrect. Neurons are among the most structurally specialized cells in the body, with distinct components tailored for communication. These include dendrites for receiving signals, an axon for transmitting electrical impulses, synaptic terminals for releasing neurotransmitters, and often a myelin sheath for insulation. The cell body itself contains specialized organelles like Nissl bodies, which are involved in protein synthesis.
B) Have a nucleus that contains genes
The presence of a membrane bound nucleus containing chromosomal DNA is a defining feature of eukaryotic cells, including neurons. The genes within this nucleus provide the instructions for all neuronal functions and are crucial for the cell's long term health and ability to respond to metabolic demands.
C) Have no cell membrane
This statement is false. All living cells are enclosed by a plasma membrane, and neurons are no exception. The neuronal cell membrane is critically important as it maintains the cell's integrity, regulates ion flow, establishes the resting membrane potential, and contains the receptors and channels necessary for generating and conducting nerve impulses.
D) Speed conduction time along nerve fibers
This statement is misleading. While the conduction speed along a neuron's axon is increased, this is not an intrinsic action of the neuron itself. The increase in speed is primarily due to the presence of a myelin sheath, which is formed by supporting glial cells called oligodendrocytes in the central nervous system and Schwann cells in the peripheral nervous system. The neuron provides the axon, but the myelination that speeds conduction is provided by these helper cells.
Conclusion:
The question addresses basic cellular features of neurons. While they possess highly specialized structures for communication, the most fundamentally correct statement among the choices is that neurons, as living cells, contain a nucleus with genes. This is a universal characteristic of eukaryotic cells and is indispensable for neuronal existence and function.
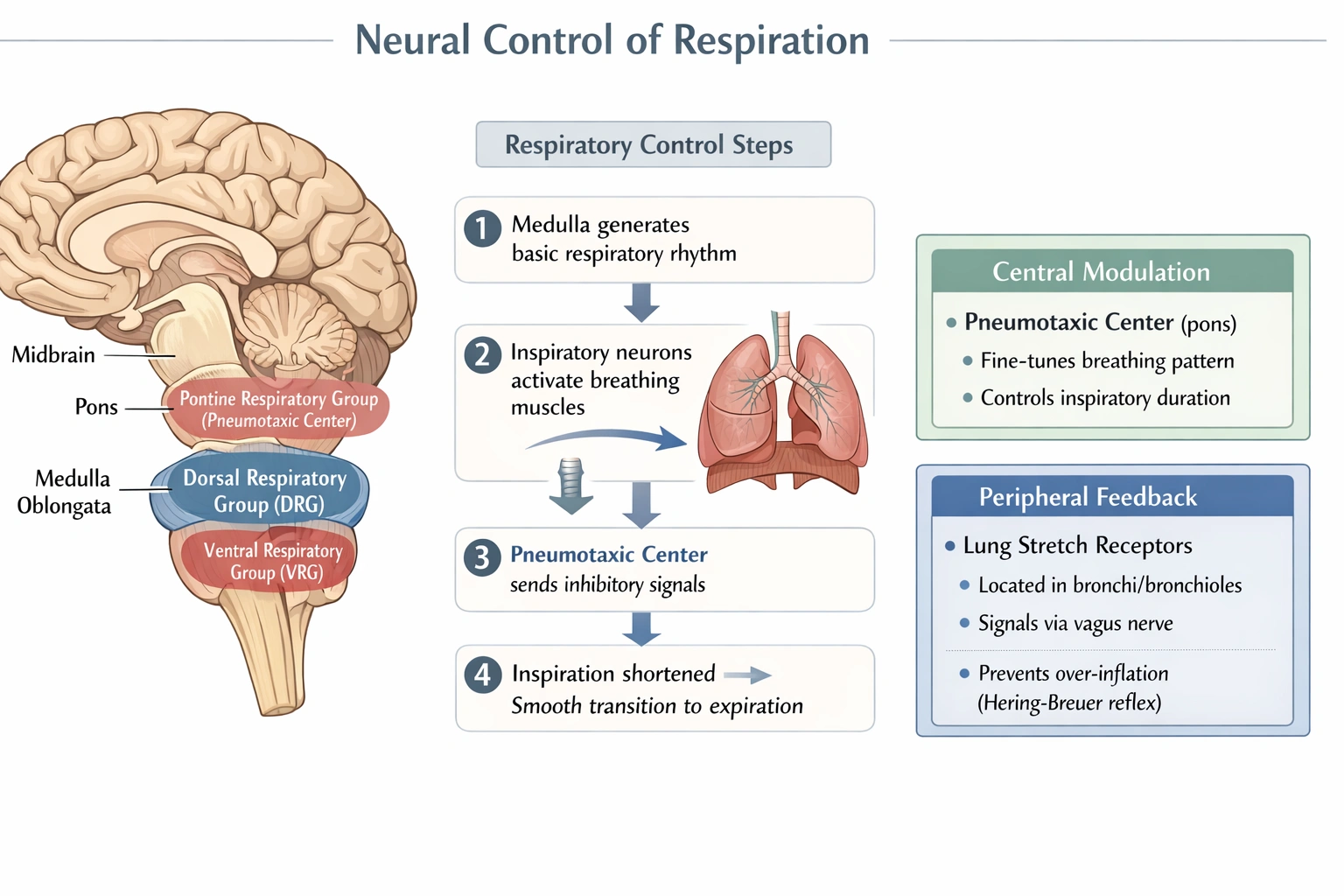
The pneumotaxic area of respiration is located in the
A.
brain stem
B. medulla
C. pons
D. stretch receptors
Rationale
The pneumotaxic area of respiration is located specifically within the pons of the brainstem.
This center, also known as the pontine respiratory group, does not generate the primary respiratory rhythm but instead fine-tunes it by sending inhibitory signals to the inspiratory centers in the medulla. Its action limits the duration of inspiration, promotes the transition to expiration, and influences respiratory rate.
A) Brain stem
While technically correct that the pneumotaxic area is within the brainstem, this answer is too imprecise. The brainstem comprises three structures: the midbrain, pons, and medulla. The question requires the specific subdivision where the pneumotaxic center is found.
B) Medulla
The medulla oblongata houses the primary respiratory rhythm generators, specifically the dorsal and ventral respiratory groups. These centers are responsible for initiating the basic, automatic pattern of breathing. The pneumotaxic area is a separate, higher control center located in the pons that regulates the output of these medullary centers.
C) Pons
The pneumotaxic center is situated in the upper part of the pons. It acts as a regulator, providing continuous inhibition to the inspiratory area in the medulla to help control the depth and rate of breathing, preventing overinflation of the lungs.
D) Stretch receptors
Stretch receptors are sensory structures located in the smooth muscle of the airways within the lungs. They are part of a peripheral feedback mechanism called the Hering-Breuer reflex, which signals the medulla to inhibit inspiration when the lungs are adequately inflated. They are not a centralized brain area responsible for respiratory modulation.
Conclusion:
Respiratory control is hierarchically organized within the brainstem. The pneumotaxic center's specific role in modulating breathing pattern is localized to the pons, distinguishing it from the primary rhythm generators in the medulla and the sensory feedback from pulmonary stretch receptors.
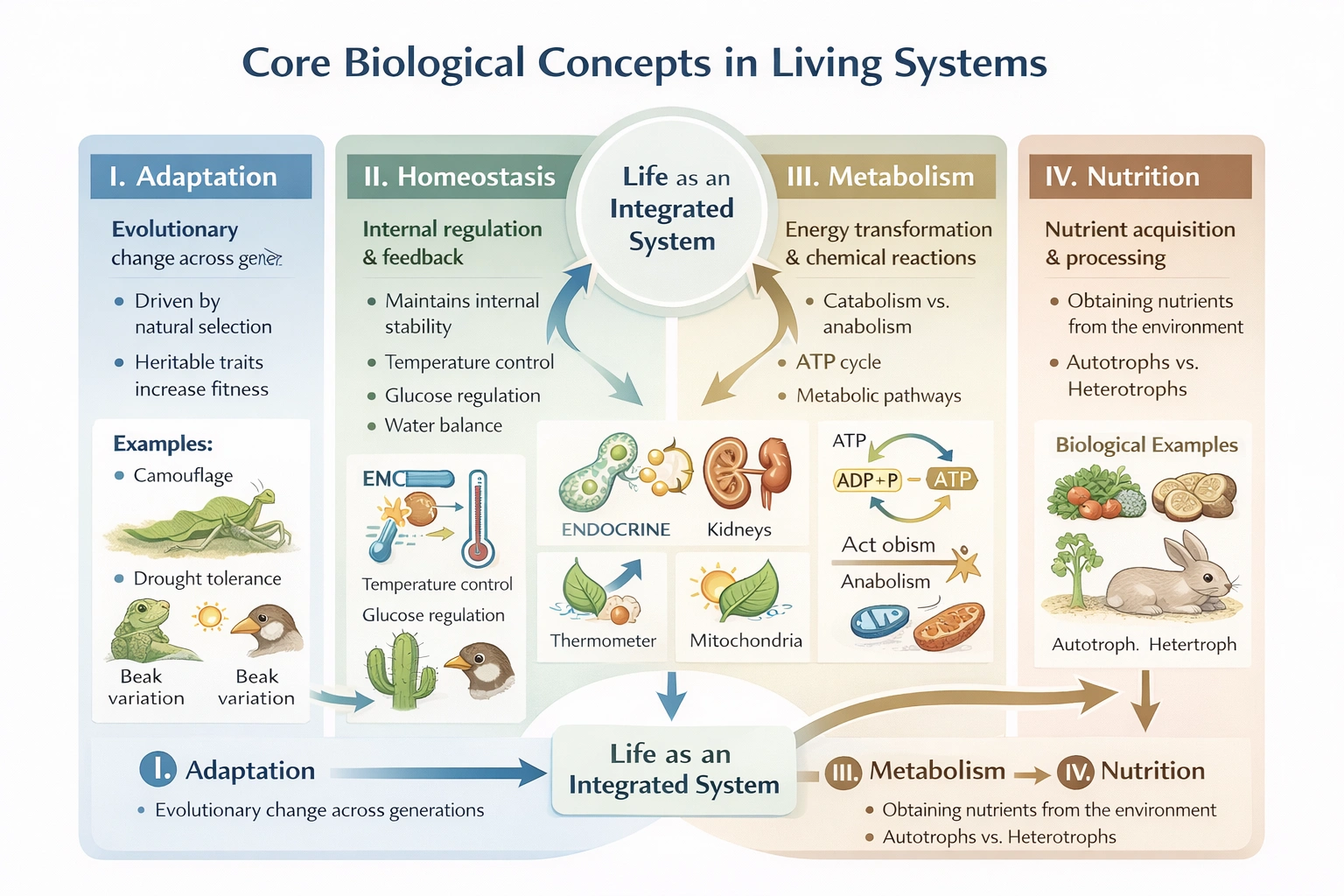
Basic biological concepts include all of the following EXCEPT
A.
adaptation.
B. homeostasis.
C. metabolism.
D. nutrition.
Rationale
The basic biological concepts include adaptations, homeostasis, and metabolism. These are broad, unifying themes that define the characteristics and functions of all living organisms. Nutrition, while a critical physiological process, is typically categorized as a specific application or subset of these broader concepts rather than a core, overarching biological principle in its own right.
A) Adaptation
Adaptation is a fundamental concept in biology, central to the theory of evolution. It refers to the heritable traits in a population that enhance survival and reproductive success in a specific environment. This process, driven by natural selection, explains the diversity of life and the remarkable fit between organisms and their habitats. It is a unifying principle that applies to all species, making it a basic biological concept.
B) Homeostasis
Homeostasis is the essential process by which living organisms maintain a stable internal environment despite external changes. This dynamic equilibrium is maintained through complex feedback systems and is crucial for the optimal functioning of cells and organ systems. Examples include the regulation of body temperature, blood pH, and glucose levels. As a defining characteristic of life, homeostasis is a core biological concept.
C) Metabolism
Metabolism encompasses the entire set of biochemical reactions that occur within an organism to sustain life. It includes both catabolism, the breakdown of molecules to release energy, and anabolism, the synthesis of complex molecules from simpler ones. Metabolism is the basis for energy transfer, growth, and repair, and its presence is a definitive criterion for life. It is universally recognized as a fundamental biological concept.
D) Nutrition
Nutrition is the process by which organisms obtain and utilize food for energy, growth, and maintenance. Although vital, nutrition is often viewed as a component of the broader concept of metabolism (specifically concerning nutrient acquisition and processing) or as a functional requirement for life. In standard lists of unifying biological themes or characteristics of life such as organization, metabolism, homeostasis, reproduction, and adaptation nutrition is not typically presented as a standalone, core conceptual pillar on the same level as the others.
Conclusion:
Adaptation, homeostasis, and metabolism are widely taught and accepted as the fundamental, unifying concepts that underpin the study of biology. Nutrition, though intrinsically important, is generally considered a vital process that supports these core principles rather than a basic conceptual category itself. Therefore, nutrition is the correct exception among the options provided.
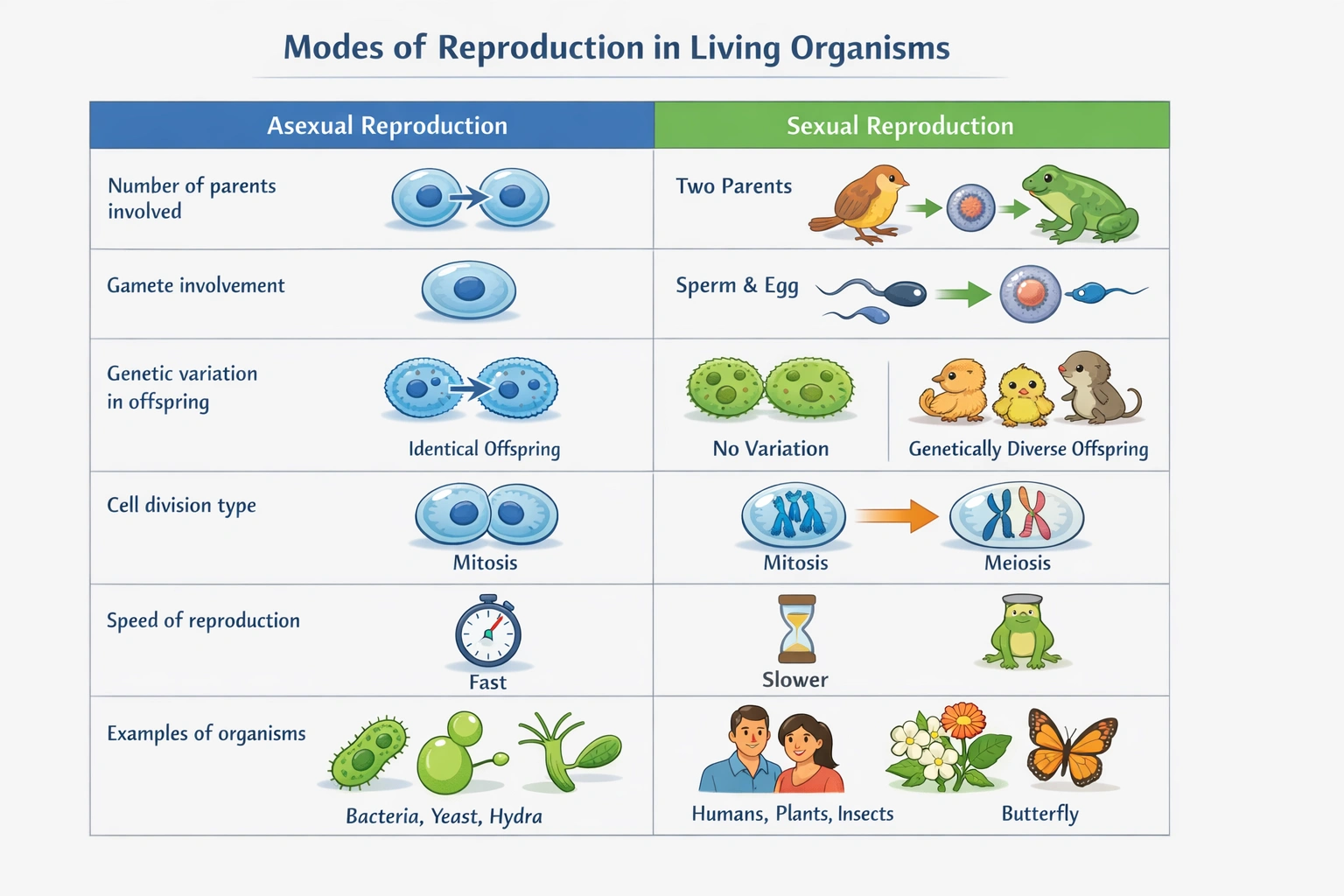
Types of reproduction are 1. Asexual requiring a single parent 2. Asexual requiring two parents 3. Sexual requiring two parents 4. Sexual requiring one parent
A.
1 and 2
B. 3 and 4
C. 1 and 3
D. 2 and 4
Rationale
Asexual reproduction requires a single parent and sexual reproduction typically requires two parents.
These definitions reflect the fundamental biological mechanisms of each mode, where asexual reproduction generates genetically identical offspring without gamete fusion, and sexual reproduction involves the combination of genetic material from two distinct parents to produce genetically diverse offspring.
A) 1 and 2
This option pairs the correct statement that asexual reproduction requires one parent with the incorrect statement that asexual reproduction can require two parents. Since asexual reproduction, by definition, involves only one parent, this pairing is invalid.
B) 3 and 4
This option pairs the correct statement that sexual reproduction usually requires two parents with the incorrect statement that sexual reproduction requires one parent. While rare exceptions like self-fertilization exist, sexual reproduction is standardly defined by biparental contribution, making this pairing inaccurate.
C) 1 and 3
This is the correct answer. It correctly combines the true statements: asexual reproduction requires a single parent, and sexual reproduction requires two parents. These are the standard, foundational definitions in biology.
D) 2 and 4
This option pairs two incorrect statements. Asexual reproduction does not require two parents, and sexual reproduction is not defined as requiring only one parent, making this combination entirely false.
Conclusion:
Reproduction is fundamentally categorized by the number of parents involved and the genetic processes at play. Asexual reproduction is characterized by a single parent producing genetically uniform offspring, whereas sexual reproduction is characterized by two parents contributing genetic material to produce genetically unique offspring. The correct combination reflecting these universal principles is that asexual reproduction requires one parent and sexual reproduction requires two parents.
__________ is an example/are examples of a solution.
A.
Alcohol and water
B. Fog
C. Italian salad dressing
D. White of an egg
Rationale
Alcohol and water is an example of a solution.
A solution is a homogeneous mixture where the components are uniformly dispersed at the molecular or ionic level. This results in a single-phase system with consistent properties throughout, no visible separation, and the absence of light scattering.
A) Alcohol and water
When ethanol and water are combined, they form a homogeneous mixture because their molecules are similar in polarity and size. This allows for complete miscibility, creating a single, uniform liquid phase. The mixture does not separate over time, does not scatter a beam of light (no Tyndall effect), and the solute particles are of molecular size, meeting all criteria for a true solution.
B) Fog
Fog is classified as a colloid, specifically a liquid aerosol, where tiny water droplets are suspended in air. The dispersed particles are larger than individual molecules, typically within the colloidal size range of 1 to 1000 nanometers. This structure causes visible light scattering (Tyndall effect) and indicates a mixture that is heterogeneous at the microscopic scale, distinguishing it from a molecular solution.
C) Italian salad dressing
This mixture, typically of oil and vinegar, is a heterogeneous combination. Due to the stark difference in polarity oil being nonpolar and vinegar (an aqueous acetic acid solution) being polar the substances are immiscible. They may temporarily mix when shaken but will quickly separate into distinct layers. The components are not dissolved into one another at a molecular level, and the mixture lacks uniformity.
D) White of an egg
Egg white, or albumen, is a colloid a dispersion of large protein molecules (like ovalbumin) in water. While it may appear homogeneous, the protein particles are too large to form a true solution. It exhibits the Tyndall effect (scatters light) and can undergo physical changes like coagulation, properties not characteristic of a stable, molecular-level solution.
Conclusion:
The defining feature of a solution is the complete and uniform dissolution of one substance into another at the molecular level. Among the choices, only the combination of alcohol and water fulfills this requirement, as it forms a single, stable phase without separation or light scattering. The other examples represent different classes of mixtures: colloids and heterogeneous combinations.
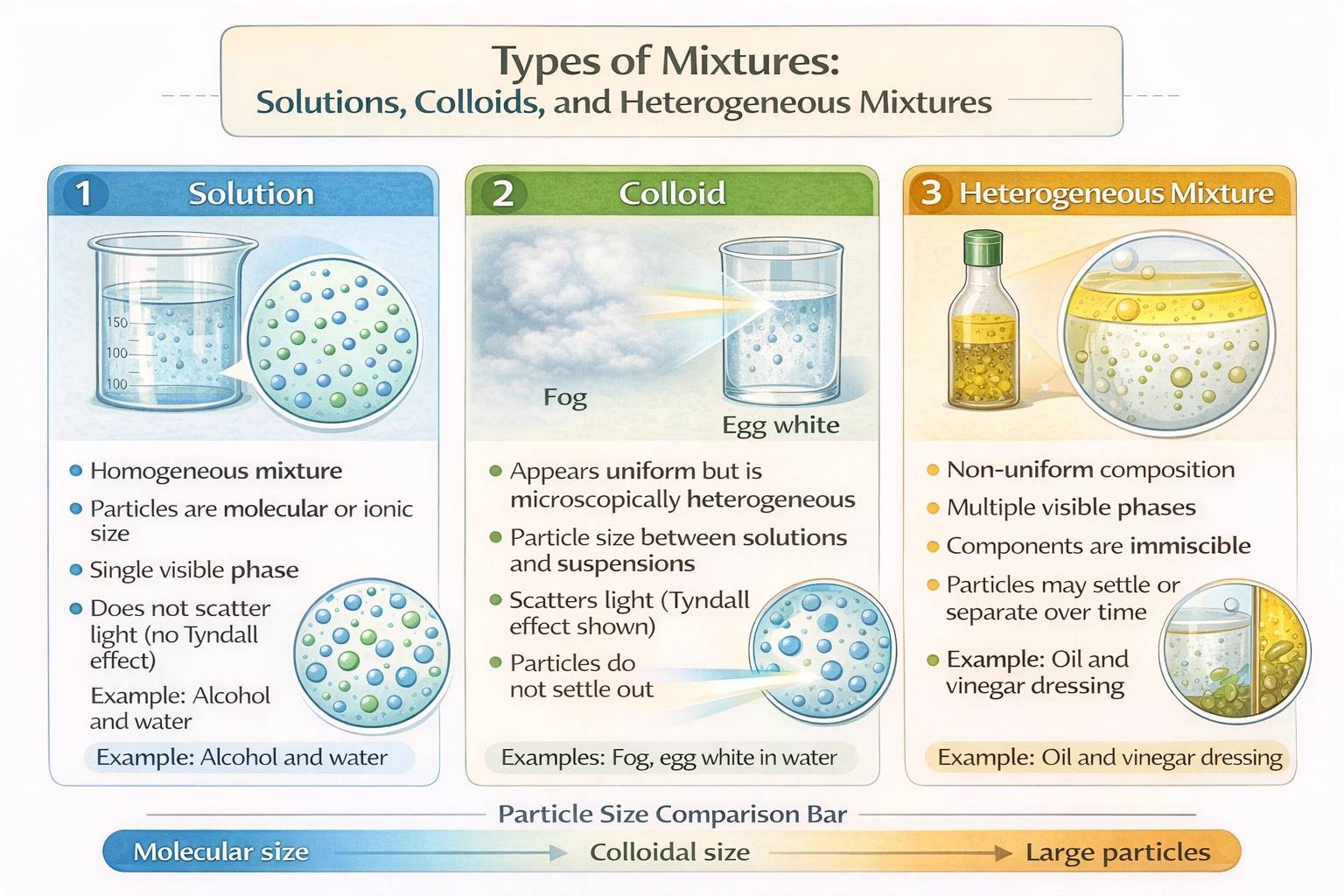
Which of Mendel's laws of heredity is the following statement based on? "Genes for different traits are sorted separately from one another so that the inheritance of one trait is not dependent on the inheritance of another."
A.
Dominance
B. ) Genes
C. Independent assortment
D. Segregation
Rationale
Independent Assortment directly describes Mendel's of heredity.
The law states that states that alleles for different traits separate and are inherited independently of one another during gamete formation, provided the genes are located on different chromosomes or are far apart on the same chromosome.
A) Dominance
Mendel's Law of Dominance explains the expression of traits in offspring when parents with contrasting traits are crossed. It states that in a heterozygous individual (carrying two different alleles for a gene), one allele (the dominant allele) will mask the expression of the other allele (the recessive allele). This law governs the interaction between alleles at a single gene locus and determines the phenotype of the offspring for that specific trait. It does not address how genes for different traits are distributed into gametes relative to each other.
B) Genes
"Genes" is not the name of one of Mendel's laws. It is the modern term for the units of heredity that Mendel referred to as "factors." While the statement is fundamentally about genes, the question asks for the specific Mendelian law that the principle illustrates. Therefore, this is an invalid choice as it names a concept, not a law.
C) Independent assortment
This is the correct law. Mendel's Second Law, the Law of Independent Assortment, states that during the formation of gametes (meiosis), the alleles for one gene segregate (separate) into gametes independently of the alleles for another gene. This means the inheritance of an allele for seed color, for example, does not influence which allele for seed shape is inherited. This law holds true for genes located on different chromosomes or far apart on the same chromosome. The provided statement perfectly paraphrases this principle of independent inheritance.
D) Segregation
Mendel's First Law, the Law of Segregation, states that an organism possesses two alleles for each trait, and these alleles separate (segregate) from each other during gamete formation so that each gamete carries only one allele for each trait. This law explains the mechanism behind the inheritance of a single trait from parents to offspring. It ensures genetic variation but is confined to the fate of alleles for one gene. It does not describe the relationship between the inheritance patterns of different traits, which is the subject of the given statement.
Conclusion:
The provided statement explicitly describes the independent inheritance of alleles for different traits during gamete formation. This is the core principle of Mendel's Law of Independent Assortment, distinguishing it from the laws governing dominance or the segregation of alleles for a single trait.
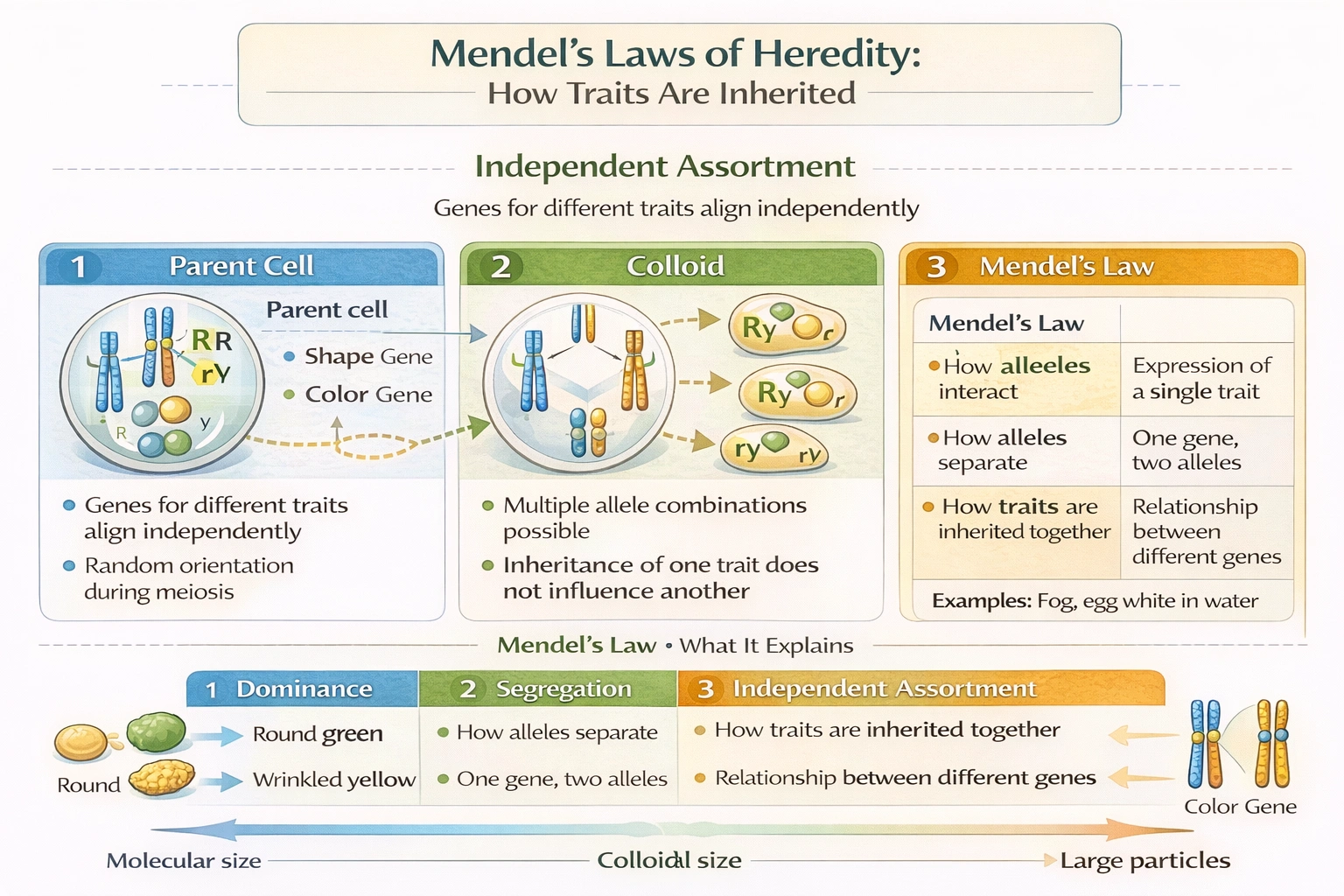
Steroidal hormones are lipids synthesized from
A.
amines
B. cholesterol
C. cortisol
D. holocrine
Rationale
Steroidal hormones are lipids synthesized from cholesterol.
All steroid hormones share a characteristic four‑ring chemical structure derived from cholesterol, a 27‑carbon lipid molecule. Cholesterol serves as the universal biochemical precursor that is enzymatically modified in steroidogenic tissues such as the adrenal cortex, gonads, and placenta to produce active hormones including cortisol, aldosterone, estrogen, progesterone, and testosterone. The conversion involves a series of cytochrome P450 enzymes and hydroxysteroid dehydrogenases that alter the cholesterol side chain and functional groups.
A. amines
Amines are a class of organic compounds derived from ammonia. In endocrinology, certain hormones (like epinephrine, norepinephrine, and thyroid hormones) are classified as amine hormones and are synthesized from amino acids such as tyrosine and tryptophan. These hormones have different structures and functions compared to steroid hormones. Steroids are not synthesized from amines; they are derived from cholesterol, which has a completely distinct four-ring lipid structure.
B. cholesterol
Cholesterol is the correct precursor for all steroid hormones. This 27-carbon lipid molecule, either obtained from the diet or synthesized in the liver, contains the essential four-ring framework that is chemically modified by enzymes in steroid-producing glands. Through processes involving cytochrome P450 enzymes, the side chain of cholesterol is cleaved and functional groups are added to create the various steroid hormones, including glucocorticoids, mineralocorticoids, and sex hormones.
C. cortisol
Cortisol is itself a steroid hormone specifically, a glucocorticoid produced by the adrenal cortex. It is an end-product of one branch of the steroid synthesis pathway, not a starting material. Cortisol is synthesized from cholesterol via intermediate molecules like pregnenolone and progesterone. Therefore, it is incorrect to state that steroid hormones are synthesized from cortisol; rather, cortisol is one of many hormones synthesized from cholesterol.
D. holocrine
Holocrine is a term that describes a mode of secretion in certain glands, such as sebaceous glands, where the entire secretory cell disintegrates to release its product. It refers to a cellular process of secretion, not a biochemical precursor. Hormone synthesis involves the chemical construction of molecules from precursor compounds, not the mechanism by which they are released from cells. Therefore, holocrine is unrelated to the synthesis of steroidal hormones.
Conclusion:
All steroidal hormones regardless of their specific type or function are biosynthesized from cholesterol. This fundamental biochemical pathway distinguishes steroid hormones from other hormone classes, such as those derived from amino acids (amines). Understanding cholesterol's role as the universal precursor is key to comprehending steroid hormone production and function in the body.
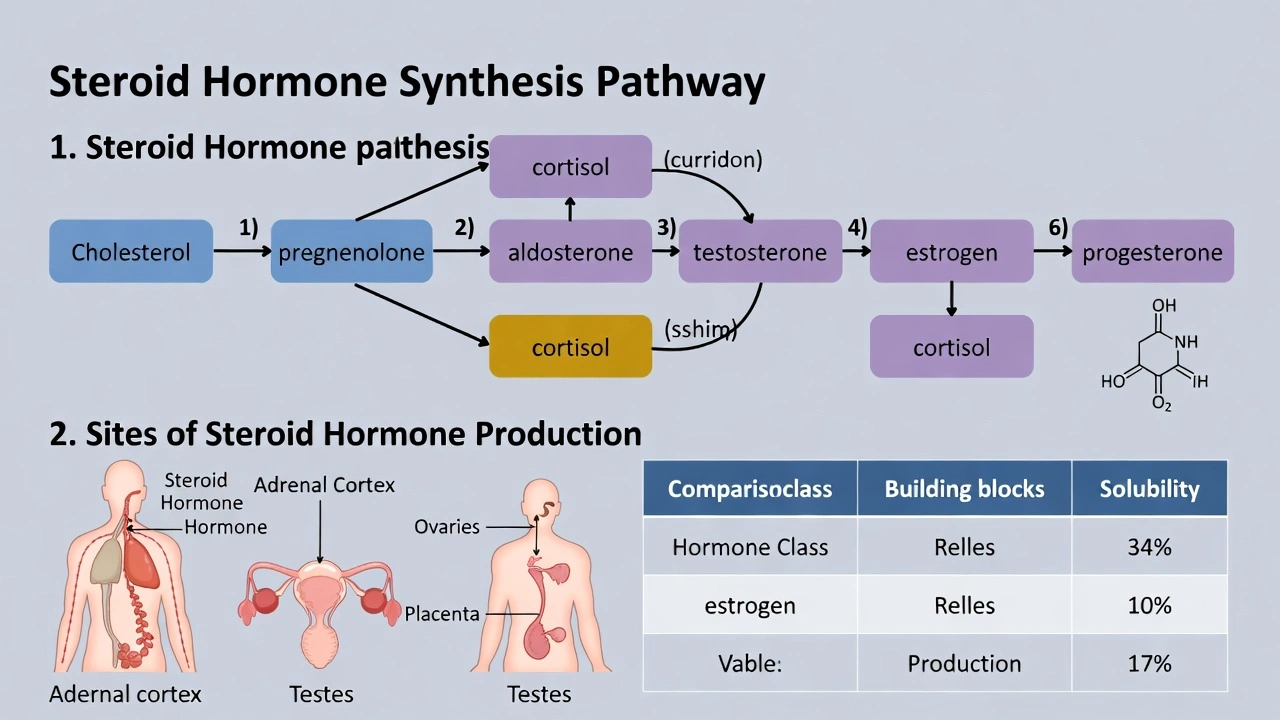
What gland is located on the upper surface of each kidney?
A.
adrenal
B. gonads
C. pancreas
D. thyroid
Rationale
The adrenal glands, also known as the suprarenal glands, are located on the upper surface of each kidney.
Each adrenal gland is a paired endocrine organ that sits atop the superior pole of a kidney, enclosed within the same fibrous renal fascia. Structurally, each gland is divided into two distinct regions: the outer adrenal cortex, which synthesizes steroid hormones such as cortisol and aldosterone, and the inner adrenal medulla, which produces catecholamines like epinephrine and norepinephrine. This precise anatomical position directly on the kidneys is a defining and unique characteristic of the adrenal glands.
A. adrenal
The adrenal glands are situated directly on the superior medial aspect of each kidney. They are retroperitoneal organs embedded in perirenal fat and share a fascial covering with the kidneys. This location is consistent and specific; no other endocrine gland occupies this position. The adrenal cortex and medulla serve critical roles in stress response, metabolism, electrolyte balance, and the "fight-or-flight" response, all facilitated by their intimate vascular and anatomical relationship with the kidneys and major abdominal vessels.
B. gonads
The gonads the testes in males and ovaries in females are the primary reproductive organs. They are not located near the kidneys. The testes reside in the scrotum, outside the abdominal cavity, while the ovaries are positioned within the pelvic cavity, laterally to the uterus. Their functions involve gamete production and secretion of sex hormones like testosterone and estrogen. Their anatomical sites are entirely separate from the upper abdominal region where the kidneys and adrenal glands are found.
C. pancreas
The pancreas is a large, elongated gland that lies transversely across the posterior abdominal wall, primarily behind the stomach. It is a retroperitoneal organ with both exocrine (digestive enzyme) and endocrine (insulin and glucagon secretion) functions. While located in the upper abdomen, the pancreas is positioned anterior to the kidneys and the great vessels, with its tail extending toward the spleen. It does not contact or rest upon the upper surface of the kidneys.
D. thyroid
The thyroid gland is situated in the anterior neck, inferior to the thyroid cartilage and anterior to the trachea. It produces thyroid hormones that regulate metabolism, growth, and development. The thyroid is separated from the kidneys by the entire thoracic cavity and the diaphragm. There is no anatomical relationship between the thyroid in the neck and the kidneys in the retroperitoneal abdomen.
Conclusion:
Only the adrenal glands possess the unique and definitive anatomical location of being positioned directly on the upper surface of each kidney. The gonads, pancreas, and thyroid gland are all found in other body regions and do not share this specific relationship with the kidneys.
Androgens are responsible for regulating/stimulating
A.
the breakdown of glycogen in the liver.
B. ductless systems.
C. skin pigment.
D. cells for secondary sexual characteristics in the male.
Rationale
Androgens are responsible for regulating cells for secondary sexual characteristics in the male.
These steroid hormones, produced mainly by the Leydig cells of the testes and to a lesser extent by the adrenal cortex, exert their effects by binding to intracellular androgen receptors, which then act as transcription factors to modulate gene expression in target tissues.
A. the breakdown of glycogen in the liver.
Hepatic glycogenolysis is a catabolic process primarily regulated by the peptide hormones glucagon (during fasting) and epinephrine (during stress). These act via cell surface receptors and cyclic AMP signaling to activate glycogen phosphorylase. Androgens have general anabolic effects on protein synthesis and can influence liver metabolism, but they are not part of the acute, primary signaling cascade for carbohydrate mobilization during energy demand.
B. ductless systems.
The term "ductless systems" is an antiquated synonym for the endocrine system. Androgens are secretory products of this system, not regulators of it. The overall function and feedback of the endocrine system are coordinated by the hypothalamus and pituitary gland (e.g., GnRH regulating LH/FSH, which then regulate testosterone). Androgens participate in negative feedback loops but do not govern the entire system.
C. skin pigment.
Skin pigmentation is determined by melanin, produced by melanocytes. Its regulation is under the control of melanocyte-stimulating hormone (MSH), derived from pro-opiomelanocortin (POMC) in the pituitary and hypothalamus, and is influenced by UV radiation. Androgens affect skin by increasing sebum production (via sebaceous gland stimulation) and promoting hair growth in androgen-sensitive areas, but they do not directly regulate melanin synthesis or distribution.
D. cells for secondary sexual characteristics in the male.
Androgens are the key mediators of virilization. In puberty, they cause: growth of facial, axillary, and pubic hair; enlargement of the larynx and vocal cords, deepening the voice; increased sebaceous gland activity, which can lead to acne; development of a masculine body habitus with increased muscle mass and reduced subcutaneous fat; and growth of the penis, scrotum, and prostate. These effects occur through activation of androgen receptors in dermal papillae, laryngeal chondrocytes, sebaceous glands, muscle satellite cells, and genital tissues.
Conclusion:
The defining physiological role of androgens is to activate cellular programs that lead to the development, expression, and maintenance of male secondary sexual characteristics. This is a specific, well-defined endocrine function. The other options either describe acute metabolic processes, vague systemic concepts, or functions of other distinct hormonal pathways.
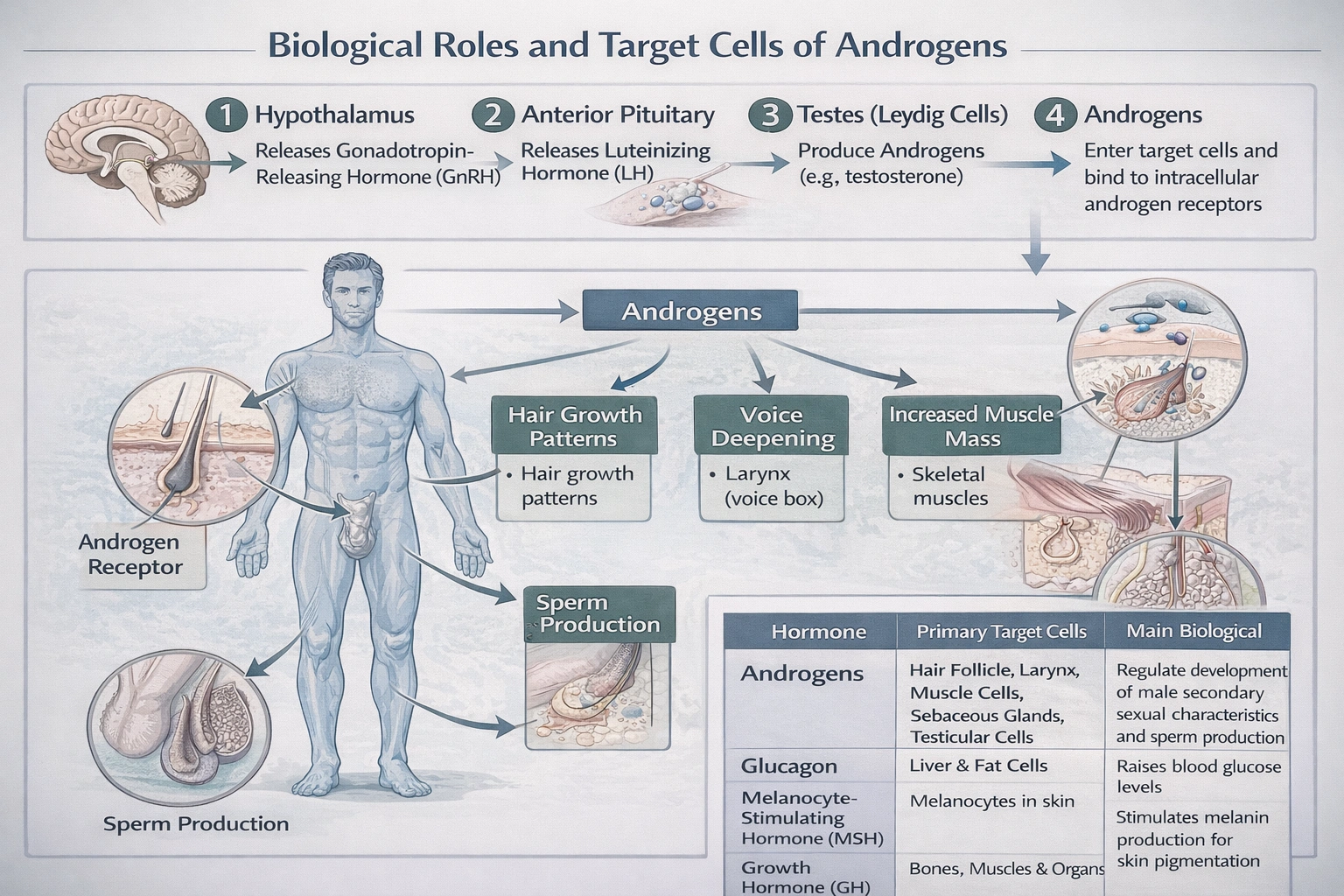
Luteinizing hormone (LH) stimulates all of the following EXCEPT
A.
the formation of corpus luteum from follicle.
B. the production of testosterone by the testes.
C. the production of secondary sexual characteristics.
D. the production of progesterone by the ovaries.
Rationale
Luteinizing hormone (LH) is a gonadotropin that stimulates steroid production and key reproductive events in the gonads.
In females, it triggers ovulation and promotes progesterone production; in males, it stimulates testosterone synthesis. However, LH does not directly cause the physical manifestations of secondary sexual characteristics.
A. the formation of corpus luteum from follicle.
The midcycle LH surge is the direct trigger for ovulation. After the oocyte is released, LH induces the remaining follicular cells to luteinize, transforming them into the corpus luteum. This new structure then secretes progesterone and estrogen under the continued influence of LH.
B. the production of testosterone by the testes.
In males, LH binds to receptors on Leydig cells in the testes, stimulating the synthesis and secretion of testosterone. This is a well-established, direct endocrine action of LH critical for male reproductive function and the maintenance of spermatogenesis.
C. the production of secondary sexual characteristics.
Secondary sexual characteristics (such as facial hair, voice deepening, breast development, and fat distribution) arise from the direct action of sex steroids testosterone and estrogenson peripheral tissues. While LH stimulates the gonads to produce these steroids, LH itself does not act on hair follicles, larynx, breast tissue, or other target organs to produce the physical traits. Therefore, LH does not directly stimulate the production of secondary sexual characteristics.
D. the production of progesterone by the ovaries.
Following ovulation, the newly formed corpus luteum produces progesterone. LH is the primary luteotropic hormone that supports the corpus luteum's function and sustains progesterone secretion during the luteal phase of the menstrual cycle and early pregnancy.
Conclusion:
LH's functions are specifically trophic to the gonads: it triggers ovulation and corpus luteum formation in females and stimulates testosterone production in males. The development of secondary sexual characteristics, however, is a consequence of the sex steroids produced in response to LH, not a direct effect of LH itself.
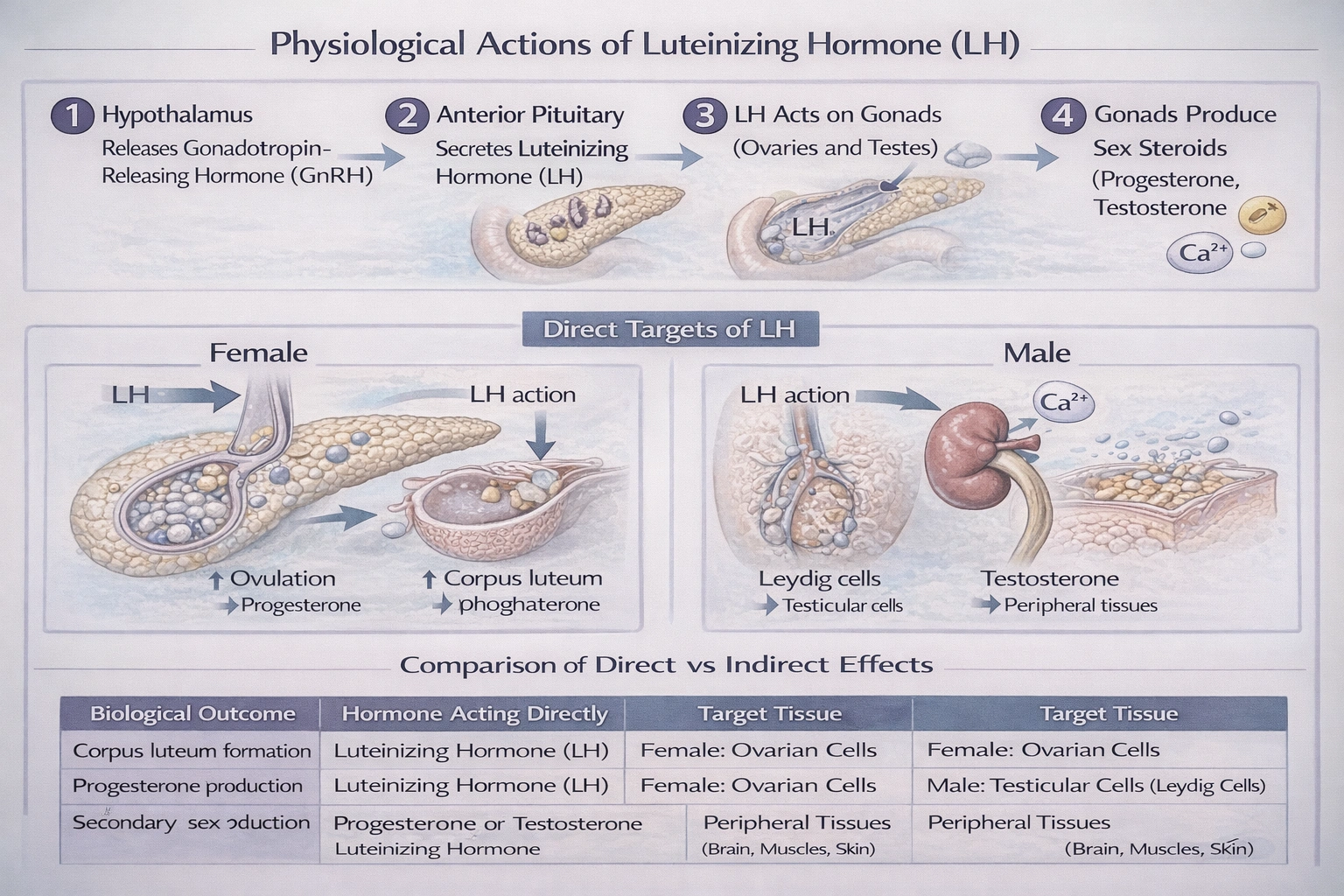
The ___________ prepares the body for the "fight or flight" response.
A.
adrenal medulla
B. apocrine gland
C. pineal gland
D. posterior lobe of the pituitary gland
Rationale
The adrenal medulla is the endocrine organ that prepares the body for the "fight or flight" response.
When activated by the sympathetic nervous system, it releases epinephrine (adrenaline) and norepinephrine (noradrenaline) into the bloodstream, triggering widespread physiological changes such as increased heart rate, elevated blood pressure, heightened alertness, and energy mobilization.
A. adrenal medulla
The adrenal medulla is composed of chromaffin cells, which are essentially modified sympathetic neurons. Upon stimulation from preganglionic sympathetic nerve fibers, it secretes large amounts of catecholamines, primarily epinephrine. These hormones act rapidly to increase cardiac output, redirect blood flow to muscles, dilate airways, and release stored glucose, collectively preparing the body to confront or flee a threat.
B. apocrine gland
Apocrine glands are a type of sweat gland found in areas like the armpits and groin. They secrete a thick fluid that contributes to body odor when metabolized by skin bacteria. Although emotional stress can stimulate apocrine sweating, this is a minor, localized response with no role in coordinating the systemic cardiovascular, metabolic, and neural changes that define the "fight or flight" reaction.
C. pineal gland
The pineal gland, located in the brain's epithalamus, secretes melatonin. This hormone regulates circadian rhythms and sleep-wake cycles, promoting rest and recovery functions that are physiologically opposite to the heightened arousal and energy expenditure required for "fight or flight."
D. posterior lobe of the pituitary gland
The posterior pituitary stores and releases oxytocin and antidiuretic hormone (ADH). While ADH can cause vasoconstriction at high doses and both hormones may be released under stress, the posterior pituitary is not the primary driver of the acute, whole-body "fight or flight" response. That role belongs to the sympathetic nervous system and the adrenal medulla.
Conclusion:
The adrenal medulla, through its rapid release of catecholamines, is the key endocrine component that amplifies and sustains the sympathetic "fight or flight" response, differentiating it from glands involved in local secretion, circadian regulation, or fluid balance.
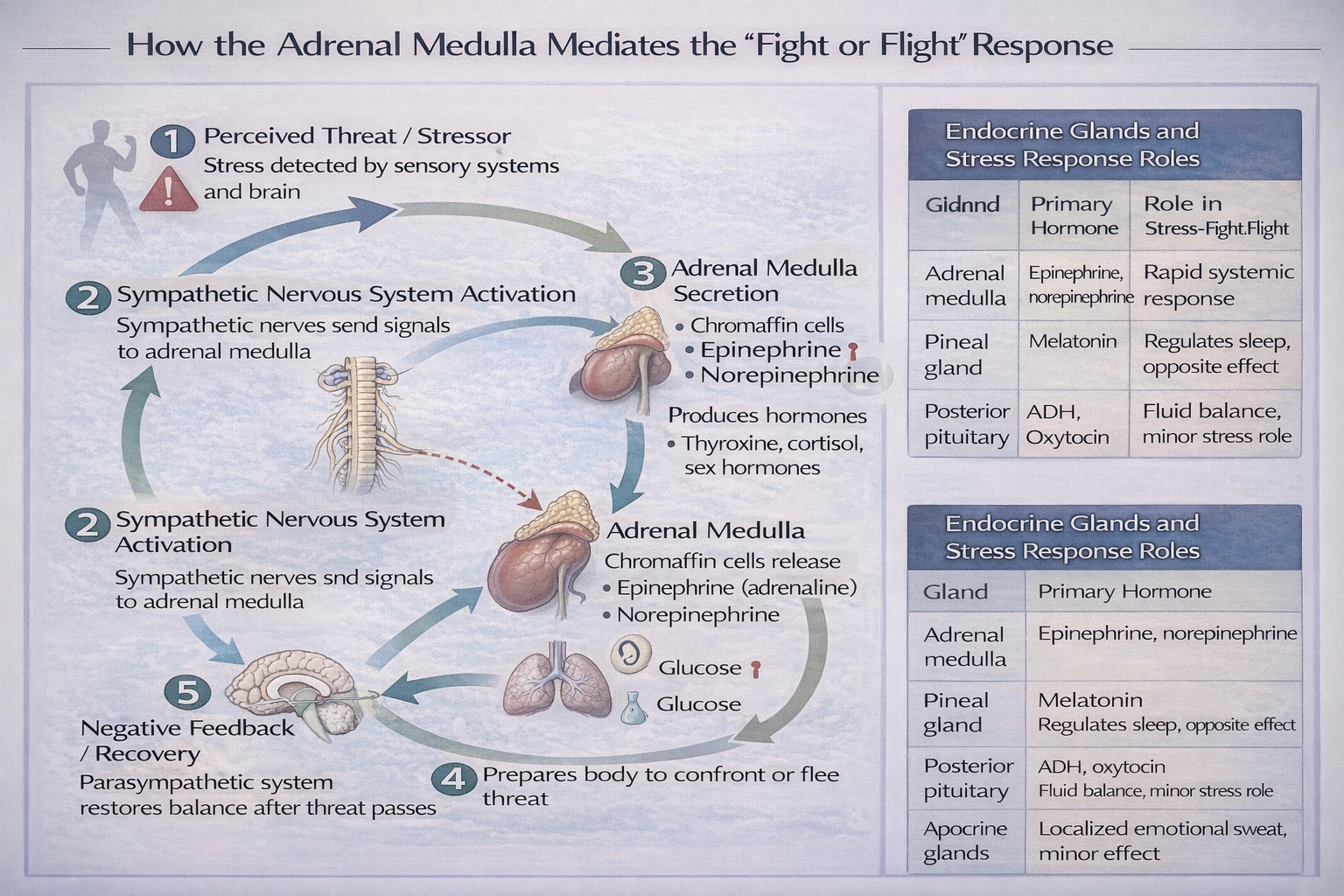
The hormone antagonist to insulin is
A.
calcitonin
B. digestive enzymes
C. glucagon
D. mineralocorticoids
Rationale
The hormone antagonist to insulin is glucagon.
These two hormones, both secreted by the pancreatic islets, work in a counter-regulatory manner to maintain blood glucose homeostasis. While insulin lowers blood glucose levels by promoting cellular uptake and storage, glucagon raises blood glucose by stimulating hepatic glucose production.
A. calcitonin
Calcitonin is a 32-amino acid polypeptide hormone secreted by the parafollicular C-cells of the thyroid gland. Its primary physiological role is to reduce blood calcium levels by inhibiting osteoclast-mediated bone resorption and enhancing renal calcium excretion. It has no significant effect on carbohydrate metabolism and does not oppose insulin's actions on blood glucose.
B. digestive enzymes
Digestive enzymes (e.g., pancreatic amylase, lipase, trypsin) are proteins secreted by exocrine glands primarily the pancreas and salivary glands into the gastrointestinal tract. They catalyze the breakdown of complex nutrients into absorbable monomers. As exocrine secretions, they are not released into the bloodstream, do not act on distant targets, and are not involved in hormonal feedback loops regulating blood glucose.
C. glucagon
Glucagon, a 29-amino acid peptide secreted by pancreatic alpha cells, is the primary physiological antagonist to insulin. It acts predominantly on hepatocytes, binding to G-protein-coupled receptors to activate adenylate cyclase, leading to increased cyclic AMP and subsequent activation of glycogen phosphorylase and gluconeogenic enzymes. This promotes glycogenolysis and gluconeogenesis, thereby elevating blood glucose. Its secretion is stimulated by hypoglycemia, amino acids, and sympathetic activation, directly countering insulin's hypoglycemic effects.
D. mineralocorticoids
Mineralocorticoids, such as aldosterone from the adrenal cortex zona glomerulosa, regulate sodium reabsorption and potassium excretion in the kidneys, influencing extracellular fluid volume and blood pressure. They have minimal direct impact on glucose metabolism. While glucocorticoids (e.g., cortisol) can elevate blood glucose and antagonize insulin action indirectly, mineralocorticoids are not considered insulin antagonists.
Conclusion:
Glucagon stands as insulin's principal hormonal antagonist, ensuring a dynamic balance in blood glucose regulation. This precise counter-regulation is essential for preventing both hyperglycemia and hypoglycemia, distinguishing glucagon from hormones involved in calcium homeostasis, digestive function, or electrolyte balance.
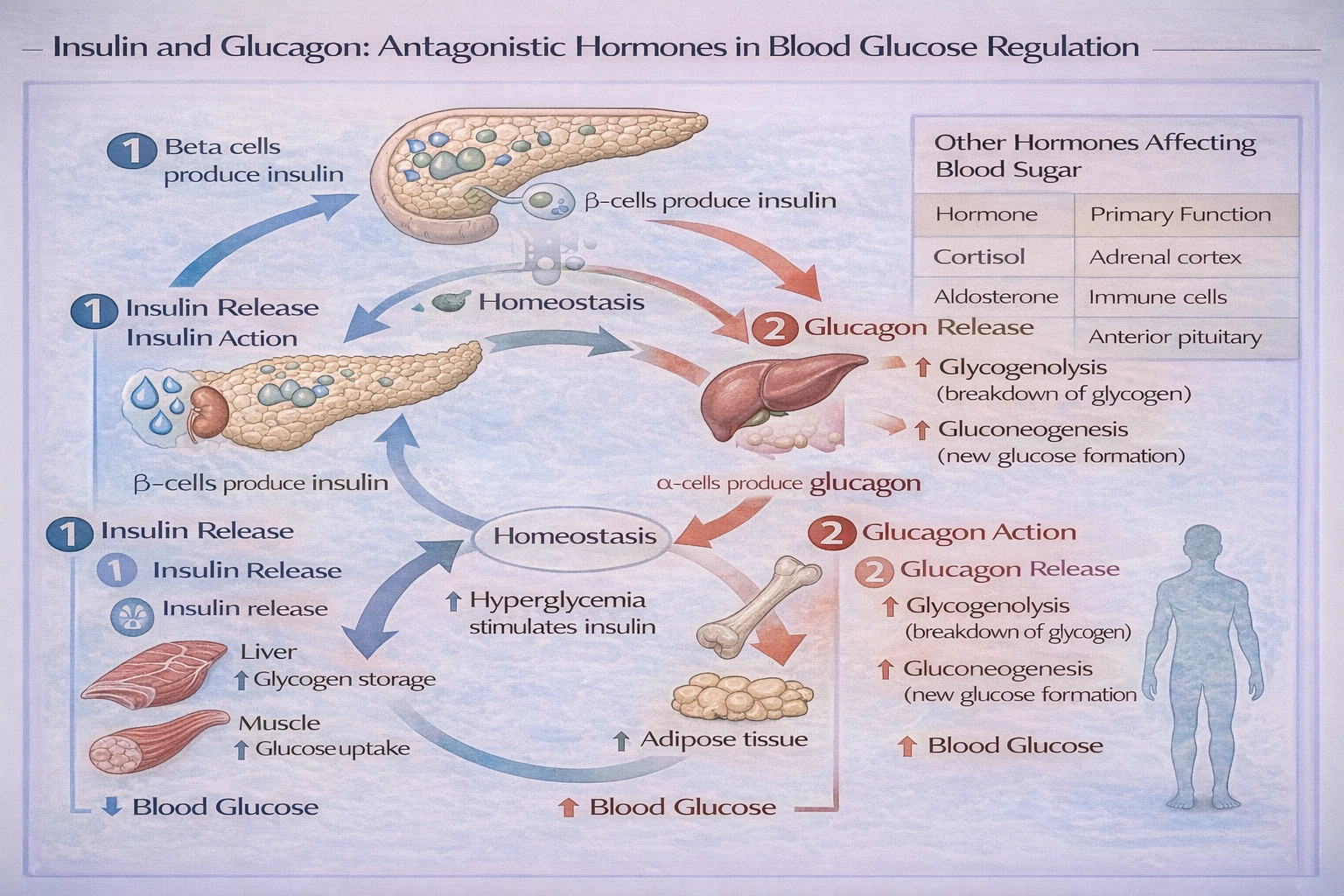
Which of the following is a primary function of lymph nodes?
A.
Carry lymph from the peripheral system to the veins.
B. Control lymph development.
C. Maintain T-lymphocytes.
D. Monitor lymph composition.
Rationale
A primary function of lymph nodes is to monitor lymph composition.
As lymph passes through the node, it is filtered and screened by resident immune cells that detect and respond to pathogens, foreign particles, and cellular debris, thereby playing a critical role in immune surveillance and defense.
A. Carry lymph from the peripheral system to the veins.
Transport of lymph is performed by lymphatic vessels, not lymph nodes. Lymphatic capillaries collect interstitial fluid, which then flows through afferent vessels into lymph nodes. After filtration, lymph exits via efferent vessels and eventually drains into the subclavian veins via the thoracic duct or right lymphatic duct. Lymph nodes are interspersed along this network as filtering stations but are not the primary conduits for lymph return to circulation.
B. Control lymph development.
Lymph formation results from the filtration of plasma from blood capillaries into interstitial spaces, driven by hydrostatic and oncotic pressures (Starling forces). The volume and composition of lymph are influenced by capillary permeability, interstitial fluid pressure, and activity of surrounding tissues. Lymph nodes do not regulate these physical processes; they act on the lymph once it has been formed and enters their sinuses.
C. Maintain T‑lymphocytes.
While lymph nodes are secondary lymphoid organs that provide an environment for activation and proliferation of T‑lymphocytes (and B‑lymphocytes), the primary site for T‑cell maturation and selection is the thymus. In the thymus, precursor cells develop into naïve, self‑tolerant T‑cells before migrating to peripheral lymphoid tissues. Lymph nodes maintain and expand populations of already‑mature lymphocytes during immune responses but are not responsible for their initial development.
D. Monitor lymph composition.
This is a fundamental function of lymph nodes. As lymph percolates through the subcapsular, trabecular, and medullary sinuses of a node, it encounters macrophages, dendritic cells, and lymphocytes. These cells phagocytose particulate matter, process antigens, and initiate adaptive immune responses if pathogens are detected. This continuous surveillance allows the immune system to identify infections, trap cancer cells, and remove debris from tissue fluid before lymph returns to the bloodstream.
Conclusion:
Lymph nodes serve as critical filtration and immune‑monitoring stations within the lymphatic system. Their role in screening lymph for foreign material distinguishes them from the transport function of lymphatic vessels, the pressure‑driven process of lymph formation, and the primary lymphoid function of the thymus. Thus, monitoring lymph composition is a core activity of lymph nodes.
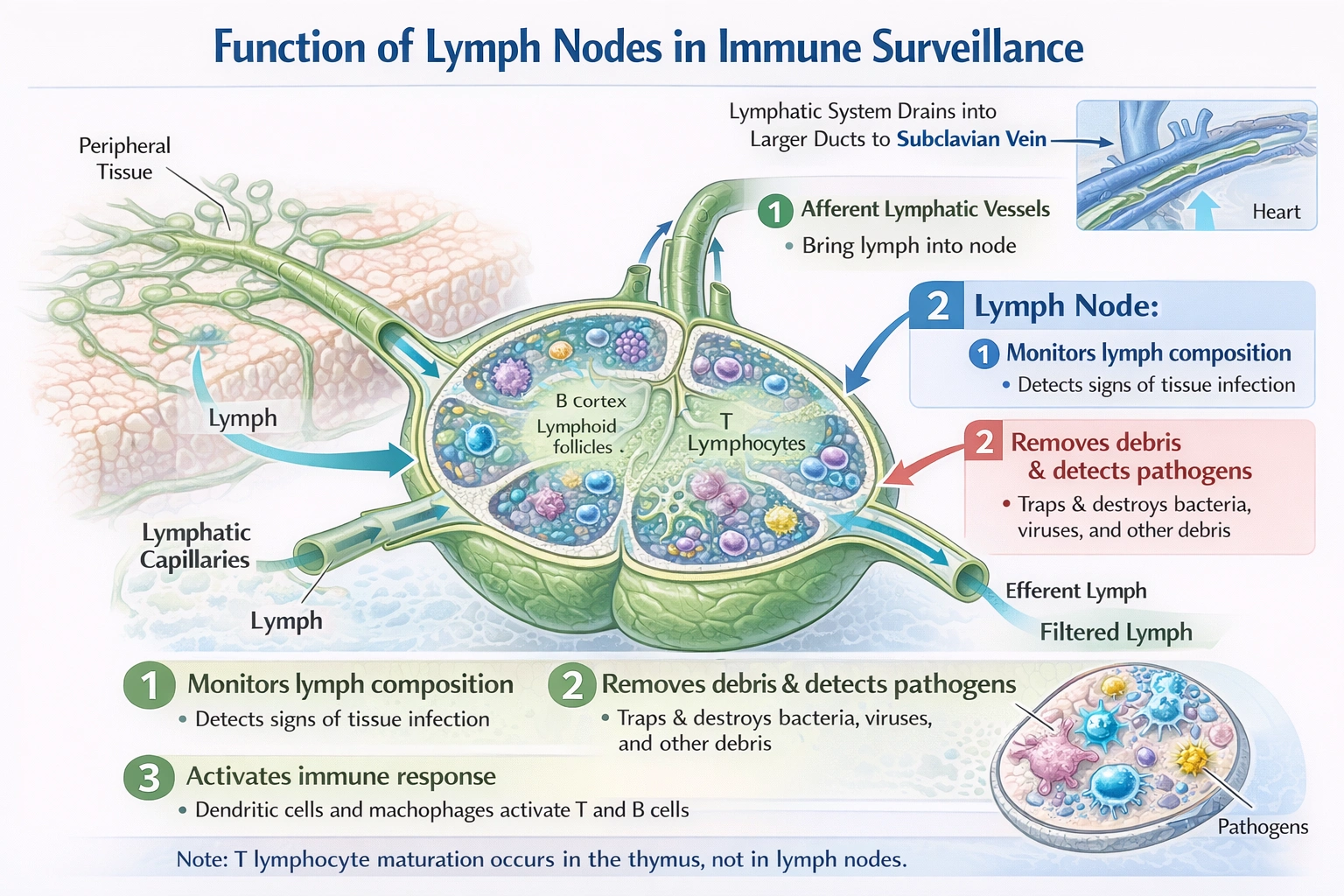
An individual at rest has a cardiac output of 4.745 liters/minute with a heart rate of 65 beats/minute. What is his stroke volume?
A.
73 milliliters/minute
B. 73 milliliters/beat
C. 308 milliliters/beat
D. 308 milliliters/minute
Rationale
Stroke volume is calculated using the formula:
Stroke Volume (SV) = Cardiac Output (CO) / Heart Rate (HR).
Given CO = 4.745 L/min and HR = 65 beats/min,
SV = 4.745 / 65 = 0.073 L/beat.
Converting liters to milliliters: 0.073 × 1000 = 73 mL/beat.
Stroke volume is expressed as volume per beat (mL/beat), not per minute.
A. 73 milliliters/minute
This unit (mL/min) describes a flow rate, not stroke volume. Stroke volume is defined as the volume of blood ejected per single heartbeat. Using "per minute" incorrectly conflates it with cardiac output, which is a minute volume.
B. 73 milliliters/beat
This is the correct answer. The calculation is: SV = CO / HR = 4.745 L/min / 65 beats/min = 0.073 L/beat. Converting liters to milliliters gives 73 mL/beat. This value represents the volume of blood pumped from the left ventricle with each contraction, which is within the normal resting range for an adult.
C. 308 milliliters/beat
This number results from a common calculation error, either multiplying cardiac output by heart rate (4.745 × 65 ≈ 308) or misplacing the decimal. The correct operation is division, not multiplication.
D. 308 milliliters/minute
This option combines the incorrect numerical value (308) with the incorrect unit (per minute). It does not represent a standard hemodynamic parameter; cardiac output is already given as 4.745 L/min (or 4745 mL/min), which is different from 308 mL/min.
Conclusion:
Stroke volume is properly calculated by dividing cardiac output by heart rate, yielding a volume per beat. The correct computation for the given values is 73 mL/beat.
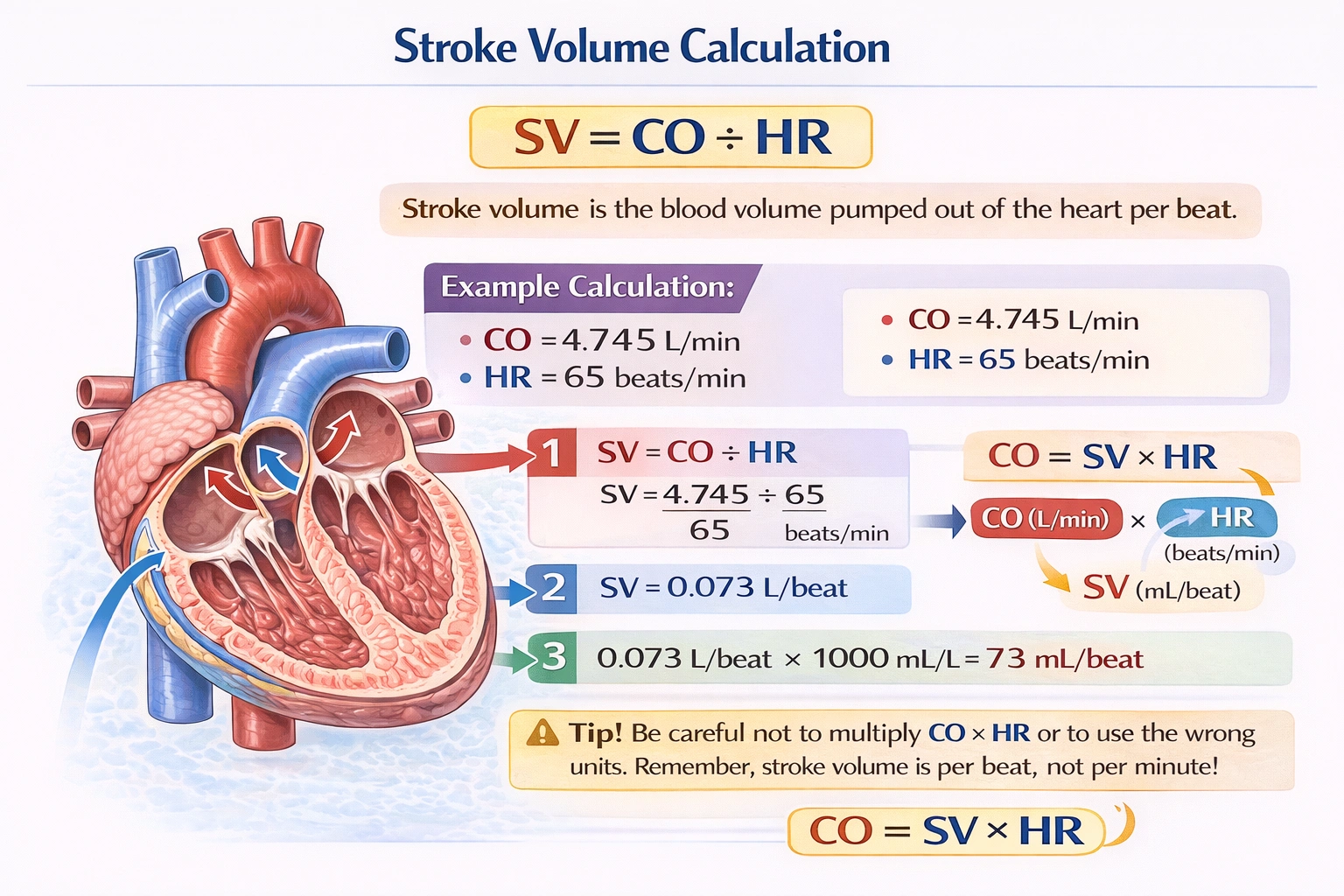
The distance that blood moves with respect to time is
A.
diastole
B. flow
C. preload
D. velocity
Rationale
The distance that blood moves with respect to time is defined as velocity.
In hemodynamics, velocity is defined as the speed of blood in a given direction, measured as distance traveled per unit of time (e.g., centimeters per second). It describes how fast blood flows through a particular segment of the circulatory system and varies depending on vessel size and total cross‑sectional area.
A. diastole
Diastole is a phase of the cardiac cycle during which the myocardium relaxes and the heart chambers fill with blood. It is a period of time, not a measure of motion or speed.
B. flow
Flow, specifically volumetric flow rate, refers to the volume of fluid passing a given point per unit time (e.g., milliliters per minute). It is a measure of volume over time, not distance over time. Cardiac output is an example of a flow rate.
C. preload
Preload is the degree of stretch of the ventricular cardiomyocytes at the end of diastole, which is determined by the volume of blood in the ventricle. It is a factor influencing the force of contraction (via the Frank-Starling mechanism) but is not a measure of the speed or distance of blood movement.
D. velocity
Velocity is the correct term for the rate of displacement distance traveled per unit time. In blood vessels, velocity varies inversely with the total cross-sectional area of the vascular bed: it is highest in the aorta and large arteries and lowest in the capillaries, where cross-sectional area is greatest, allowing for efficient exchange.
Conclusion:
Velocity is the specific physical parameter describing how far blood travels per unit time. It is distinct from flow (volume over time), phases of the cardiac cycle, or measures of cardiac filling.
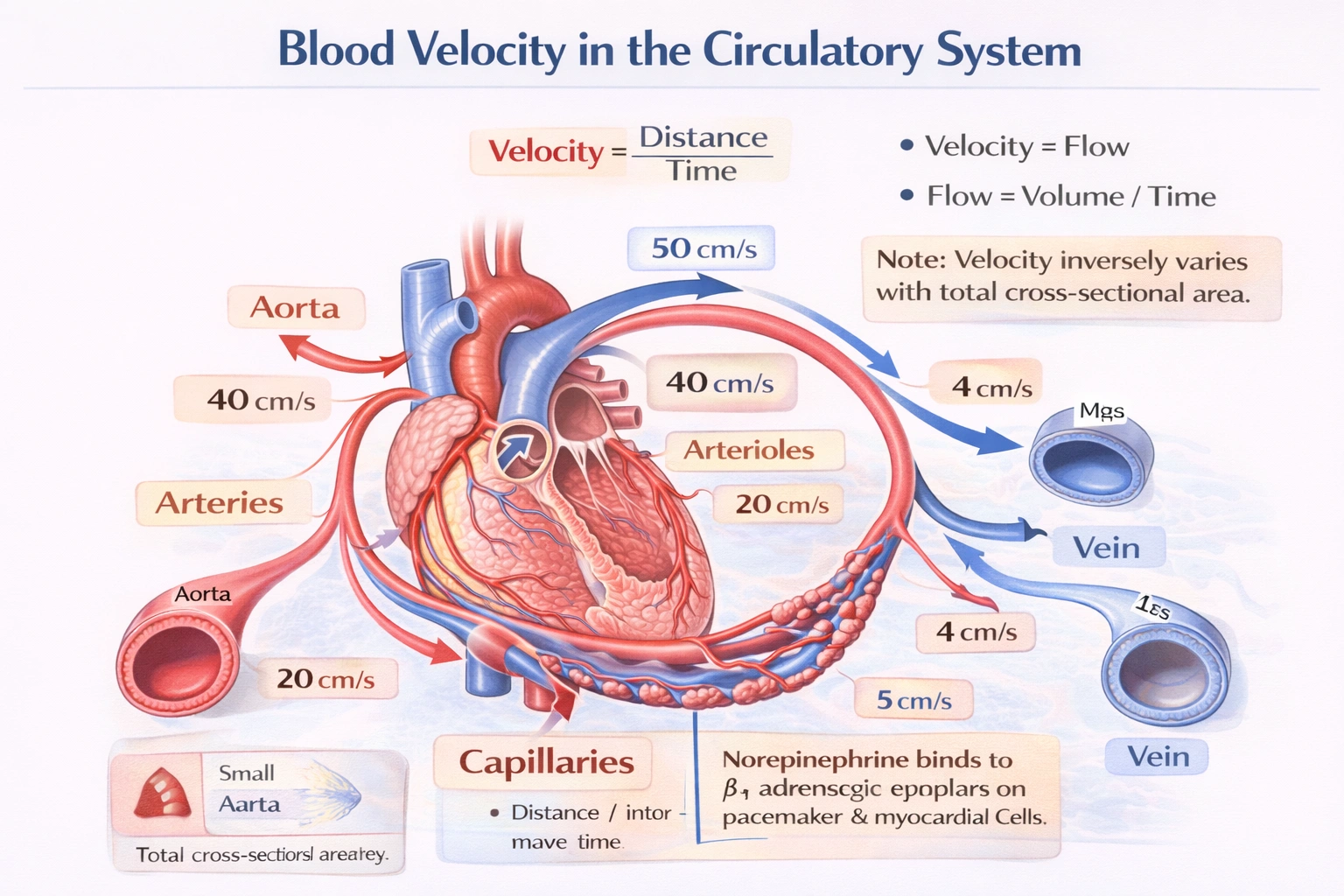
Which of the artery layers is able to withstand higher pressures than veins and has the ability to dilate or constrict?
A.
The inner layer (tunica intima)
B. The middle layer (tunica media)
C. The outer layer (tunica adventitia)
D. None of the above
Rationale
The artery layer able to withstand higher pressures than veins and has the ability to dilate or constrict is the middle layer (tunica media).
Arteries are exposed to higher, pulsatile pressures generated by the heart, and their walls are adapted to both withstand this pressure and actively regulate blood flow. The tunica media the middle layer of the arterial wall contains abundant smooth muscle cells and elastic fibers. The smooth muscle allows for vasoconstriction and vasodilation, while the elastic components provide resilience and recoil, enabling arteries to handle pressures far greater than those in veins.
A. The inner layer (tunica intima)
The tunica intima is the innermost lining of blood vessels, consisting of a single layer of endothelial cells over a thin basement membrane and a sparse subendothelial connective tissue. Its primary roles are to maintain a smooth, non‑thrombogenic surface for blood flow, regulate the exchange of molecules, and mediate local vascular signaling. While it contributes to vascular homeostasis, it lacks the muscular or elastic components necessary to withstand high pressures or to produce active changes in vessel caliber.
B. The middle layer (tunica media)
The tunica media is the dominant layer in arterial walls and is specially adapted for pressure resistance and vasomotor activity. In elastic arteries (e.g., the aorta), it contains numerous concentric sheets of elastic fibers that allow the vessel to expand during systole and recoil during diastole, dampening pressure fluctuations. In muscular arteries and arterioles, it is rich in circumferentially arranged smooth muscle cells that contract or relax in response to neural, hormonal, and local signals, thereby regulating blood flow and peripheral resistance. This combination of elasticity and contractility enables arteries to handle pressures that are substantially higher than those in veins and to actively adjust their diameter.
C. The outer layer (tunica adventitia)
The tunica adventitia (or externa) is composed mainly of dense, irregular collagen and elastic fibers that blend with the surrounding connective tissue. It functions to anchor the vessel, prevent over‑distension, and provide mechanical support. In larger vessels, it also contains the vasa vasorum (small vessels that nourish the outer wall) and autonomic nerves. Although it contributes to the overall structural integrity of the artery, it does not contain significant smooth muscle and therefore cannot actively constrict or dilate. Its role is more passive and protective rather than dynamic.
D. None of the above
Because option (B) accurately and specifically describes the arterial layer endowed with both pressure‑resistant and contractile properties, this choice is incorrect.
Conclusion:
The tunica media is the key architectural layer that distinguishes arteries from veins. Its robust composition of smooth muscle and elastic tissue allows arteries to tolerate the high, pulsatile pressures generated by the heart and to actively modulate blood flow through vasoconstriction and vasodilation. This functional specialization is central to cardiovascular regulation and hemodynamics.
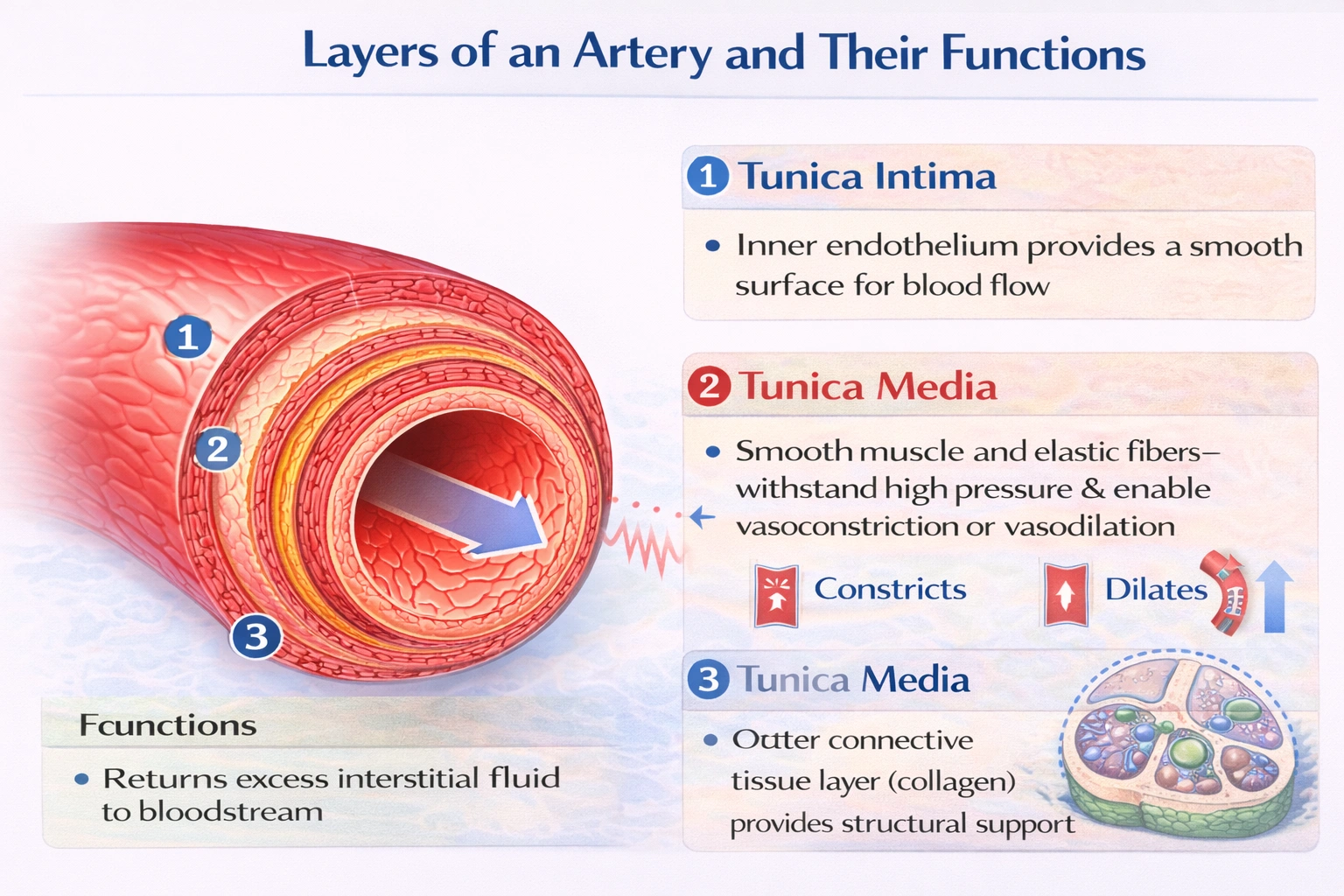
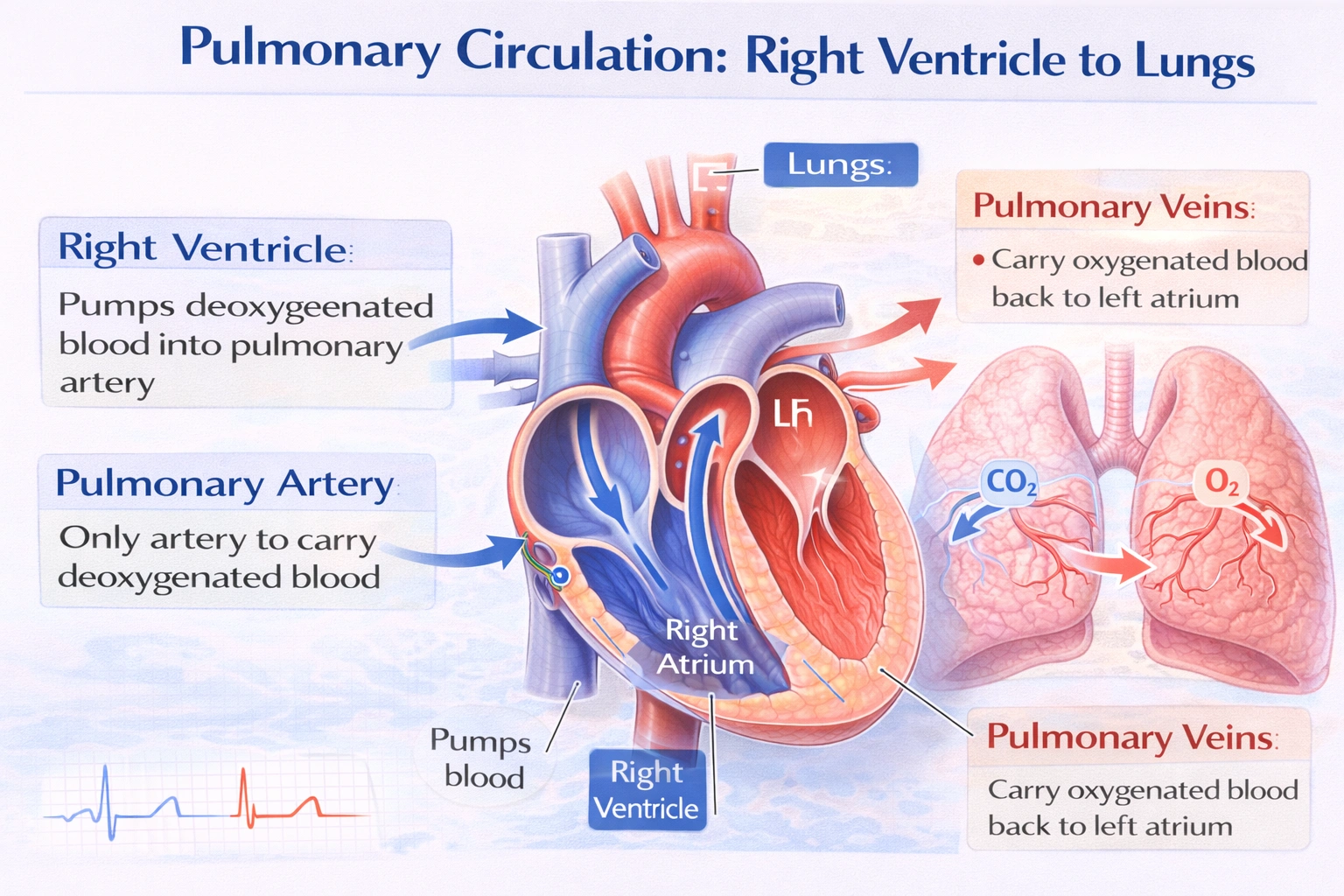
The pulmonary artery transports blood from the __________ to the __________.
A.
left atrium, aorta
B. left ventricle, body
C. right atrium, lungs
D. right ventricle, lungs
Rationale
The pulmonary artery transports blood from the right ventricle to the lungs.
The pulmonary artery is the large artery that arises from the right ventricle at the pulmonary valve. It carries deoxygenated blood directly to the pulmonary capillaries in the lungs, where carbon dioxide is exchanged for oxygen. This vessel is the sole conduit initiating the pulmonary circuit, which is separate from the systemic circulation.
A. left atrium, aorta
Blood flows from the left atrium into the left ventricle, and the left ventricle pumps oxygenated blood into the aorta for systemic distribution. The pulmonary artery is not involved in this pathway; it originates from the right side of the heart.
B. left ventricle, body
The left ventricle ejects oxygenated blood into the aorta, which then distributes it throughout the body. This describes the beginning of the systemic circulation. The pulmonary artery belongs to the right side of the heart and carries blood only to the lungs.
C. right atrium, lungs
The right atrium receives deoxygenated blood from the systemic veins and passes it to the right ventricle. It does not pump blood directly to the lungs. The pumping chamber for the pulmonary circuit is the right ventricle.
D. right ventricle, lungs
This is correct. The pulmonary artery arises from the right ventricle, carrying deoxygenated blood away from the heart to the lungs for oxygenation. It is the first and only artery in the body that transports deoxygenated blood.
Conclusion:
The pulmonary artery serves as the essential vessel that conveys deoxygenated blood from the right ventricle to the lungs, marking the beginning of the pulmonary circulation. This function distinguishes it from all systemic arteries and clarifies its unique role in the cardiopulmonary pathway.
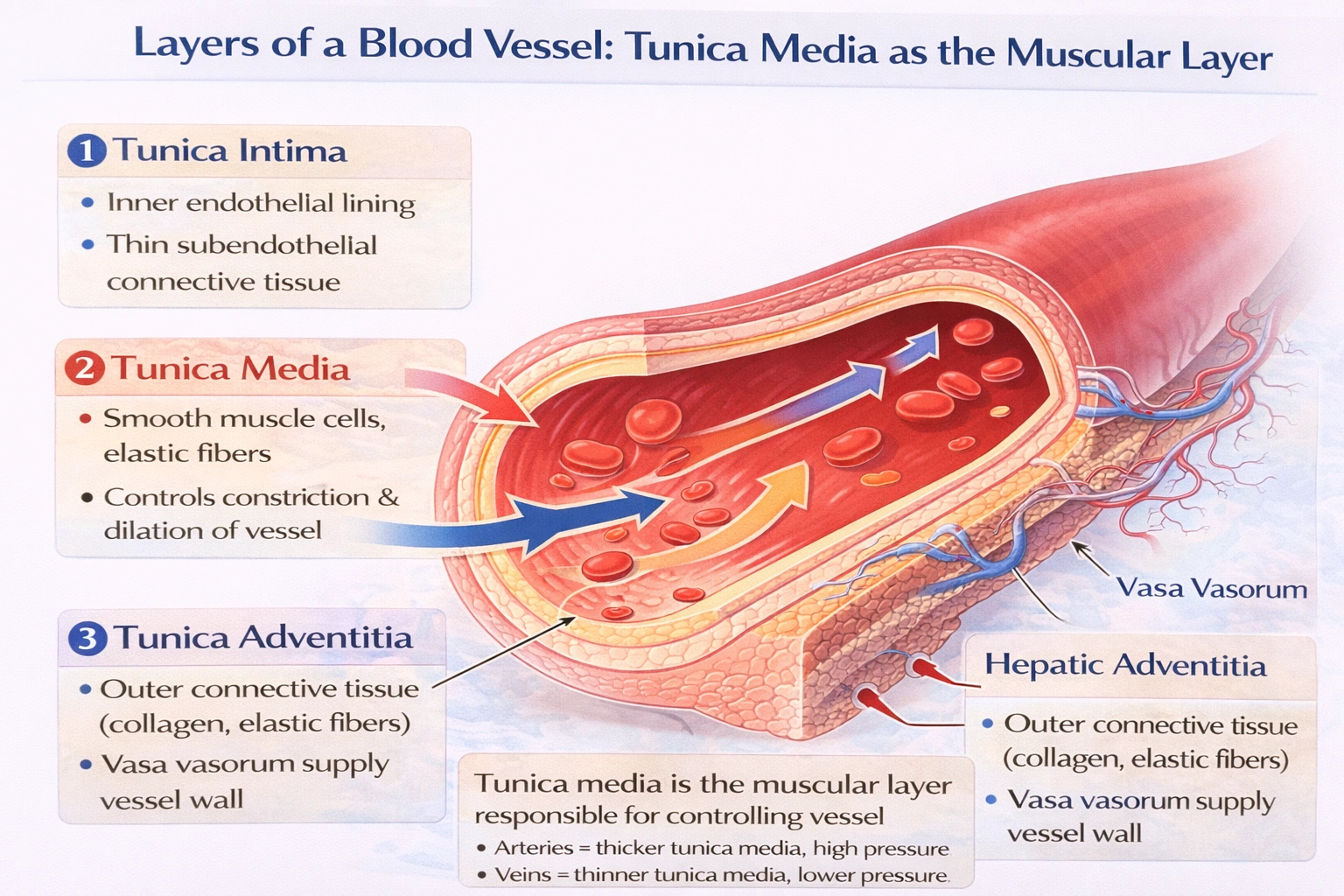
The muscular layer of a blood vessel is called the
A.
tunica adventitia
B. tunica intima
C. tunica media
D. vasa vasorum
Rationale
The muscular layer of a blood vessel is called the tunica media.
This middle layer of the blood vessel wall is predominantly composed of smooth muscle cells and elastic fibers. It enables vasoconstriction and vasodilation, allowing the vessel to actively regulate its diameter, which in turn controls blood flow and blood pressure.
A. tunica adventitia
The tunica adventitia (or externa) is the outermost layer of the vessel wall, composed mainly of dense, irregular connective tissue such as collagen and elastic fibers. Its primary functions are to anchor the vessel to surrounding tissues, provide structural support, and prevent over-distension. It contains nerves and, in larger vessels, the vasa vasorum, but it does not contain significant smooth muscle and is not considered the muscular layer.
B. tunica intima
The tunica intima is the innermost layer, consisting of a single layer of endothelial cells lining the lumen, a basement membrane, and a thin subendothelial connective tissue layer. It provides a smooth, non-thrombogenic surface for blood flow, regulates the exchange of materials, and secretes vasoactive substances. However, it lacks smooth muscle and is not involved in active changes in vessel diameter.
C. tunica media
The tunica media is the thick, muscular middle layer. In arteries, it is particularly well-developed and contains concentric rings of smooth muscle cells interwoven with elastic fibers. This structure allows arteries to withstand high pressure, maintain vascular tone, and actively constrict or dilate in response to neural, hormonal, and local signals. In veins, this layer is thinner but still contains smooth muscle, contributing to venous tone and capacitance.
D. vasa vasorum
The vasa vasorum are a network of small blood vessels that supply oxygen and nutrients to the walls of larger arteries and veins. They are embedded primarily in the tunica adventitia and the outer portion of the tunica media. While essential for nourishing thick vessel walls, they are not a structural layer of the vessel and do not contribute to muscular function.
Conclusion:
The tunica media is definitively the muscular layer of a blood vessel, responsible for active regulation of vessel diameter through its smooth muscle content. The tunica intima serves as the inner lining, the tunica adventitia provides external support and anchorage, and the vasa vasorum are nutrient vessels---none of which constitute the muscular layer.
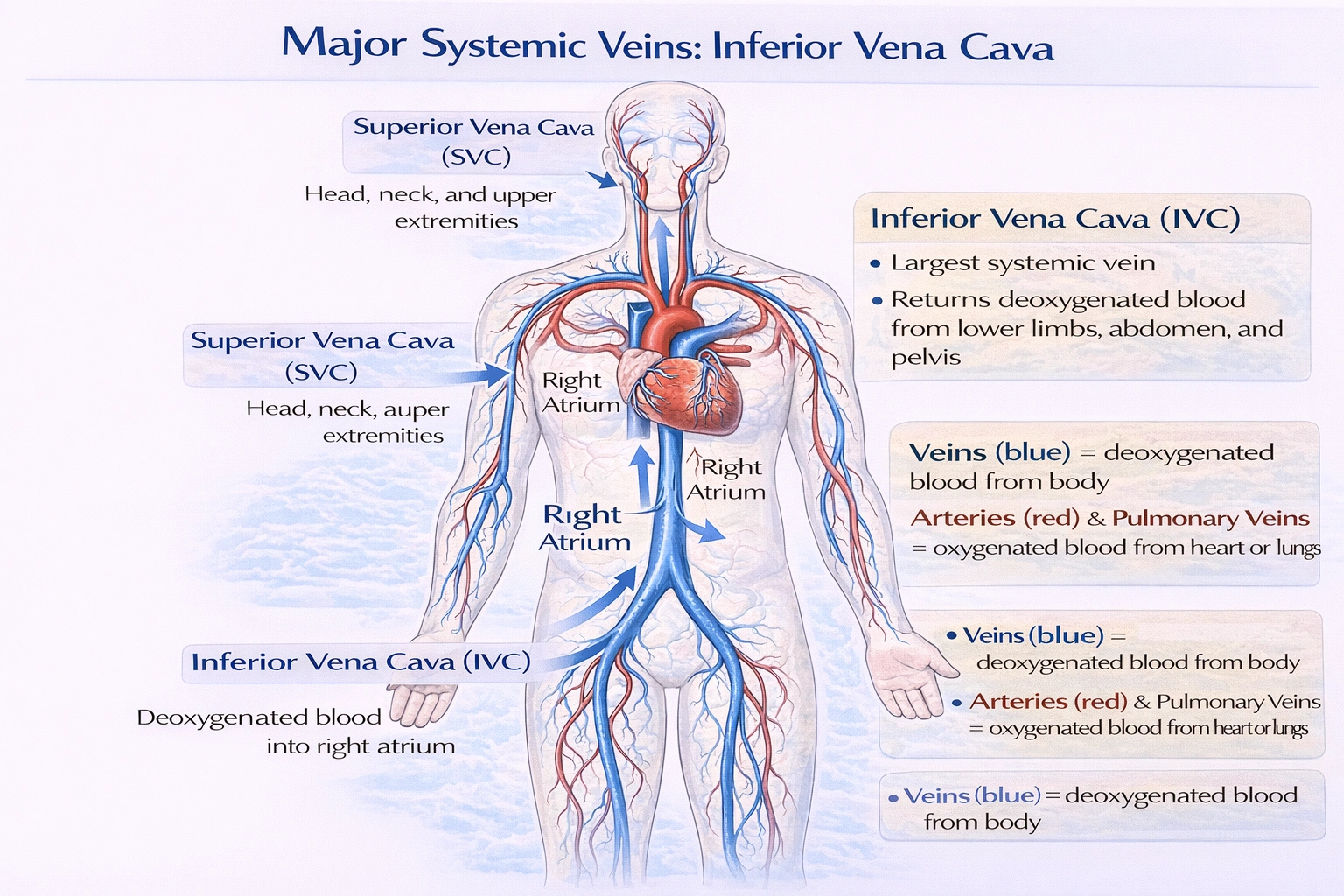
The major systemic vein in the body is the
A.
aorta
B. coronary sinus
C. inferior vena cava
D. pulmonary vein
Rationale
The major systemic vein in the body is the inferior vena cava.
The systemic venous system returns deoxygenated blood from the body to the heart. The inferior vena cava (IVC) is the largest systemic vein, collecting blood from all structures inferior to the diaphragm including the lower limbs, abdomen, and pelvis and delivering it to the right atrium. Together with the superior vena cava (which drains areas above the diaphragm), it forms the primary conduit for venous return to the heart
A. aorta
The aorta is the largest artery in the body, carrying oxygenated blood away from the left ventricle to the systemic circulation. It is not a vein.
B. coronary sinus
The coronary sinus is a major vein of the heart itself, draining deoxygenated blood from the myocardium into the right atrium. While important, its scope is limited to cardiac tissue and it is not the major systemic vein for the entire body.
C. inferior vena cava
This is correct. The IVC is a large-diameter vein that ascends through the abdomen and thorax, returning blood from the lower half of the body. It is a central component of systemic venous return.
D. pulmonary vein
Pulmonary veins carry oxygenated blood from the lungs to the left atrium. They belong to the pulmonary circulation, not the systemic venous system, and are not involved in returning deoxygenated blood from the body.
Conclusion:
The inferior vena cava is the principal systemic vein responsible for returning blood from the lower body to the heart, distinguishing it from arteries, cardiac-specific veins, and pulmonary vessels.
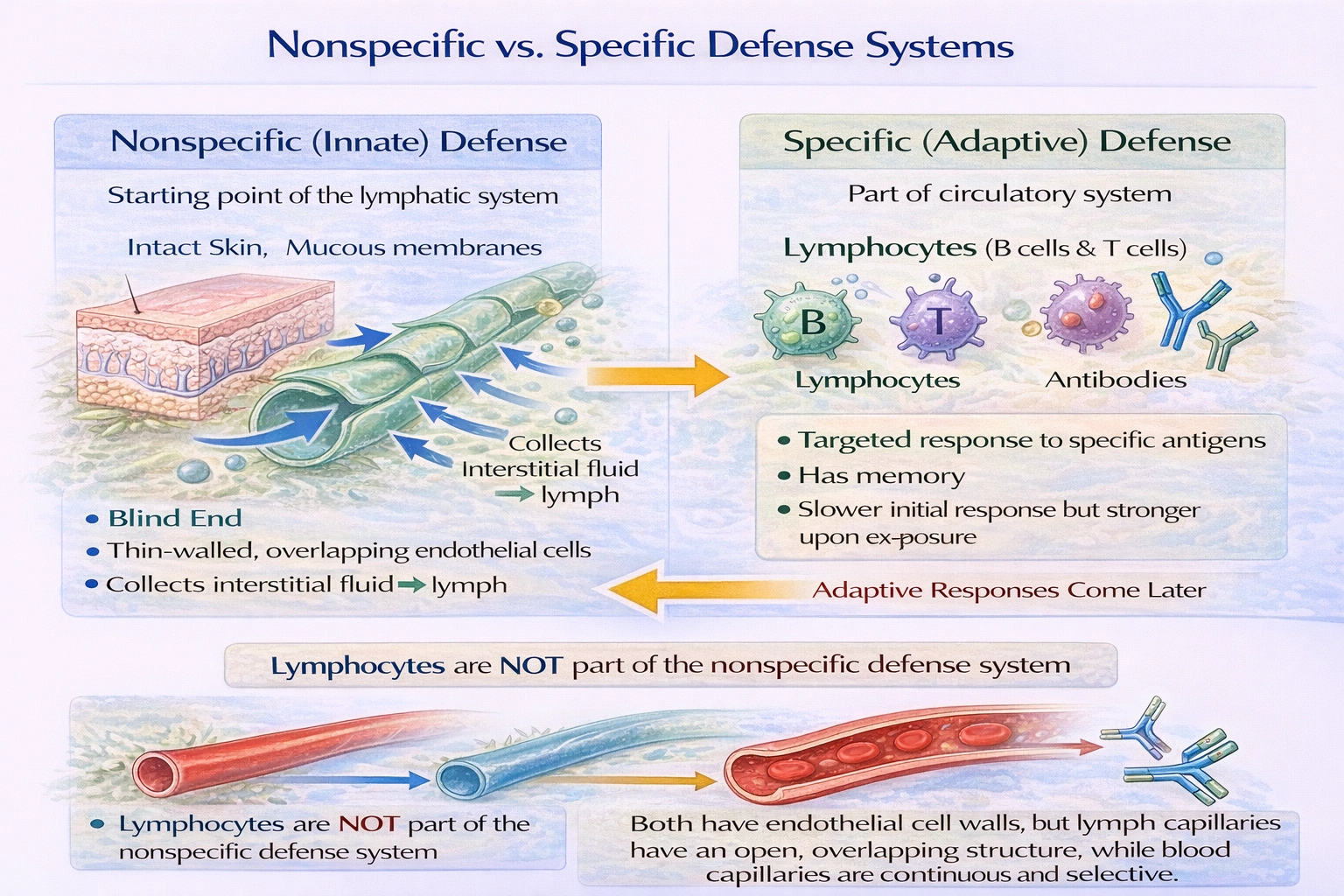
Which of the following is NOT a part of the body's nonspecific defense system?
A.
fever
B. inflammation
C. intact skin
D. lymphocytes
Rationale
The component that is NOT a part of the body's nonspecific defense system is lymphocytes.
The body's defense mechanisms are divided into two main categories: nonspecific (innate) defenses and specific (adaptive) defenses. Nonspecific defenses provide immediate, general protection against a wide variety of pathogens and do not require prior exposure. In contrast, specific defenses involve a targeted response tailored to a particular pathogen and are characterized by memory. Lymphocytes, which include B cells and T cells, are the central players in the specific adaptive immune system. They are responsible for recognizing specific antigens, mounting a targeted attack, and creating immunological memory, which are features absent from nonspecific defenses.
A. fever
Fever is a systemic, nonspecific defensive response triggered by pyrogens in response to infection or inflammation. By elevating the body's temperature, fever inhibits the growth of many temperature-sensitive microorganisms, enhances the activity of phagocytic cells, and accelerates metabolic processes that aid in repair. It is a general reaction that occurs regardless of the specific type of invader.
B. inflammation
Inflammation is a classic, localized nonspecific defense. It is initiated by tissue damage from any cause, such as a cut, burn, or infection. The cardinal signs---redness, heat, swelling, and pain---result from increased blood flow, vascular permeability, and the influx of leukocytes and plasma proteins. This process helps to isolate and destroy the injurious agent, remove debris, and initiate tissue healing, all through a standard sequence not tailored to a specific pathogen.
C. intact skin
Intact skin and mucous membranes form the first line of nonspecific defense. They act as continuous physical barriers that prevent microbial entry. Additionally, secretions like sebum (with a low pH) and sweat contain antimicrobial chemicals. The skin's protective role is constant and general, offering broad-spectrum defense without specificity.
D. lymphocytes
Lymphocytes are the key cellular components of the adaptive immune system. B lymphocytes produce antibodies that target specific antigens, and T lymphocytes directly attack infected cells or regulate the immune response. This system exhibits specificity (targeting particular pathogens), memory (faster and stronger response upon re-exposure), and adaptability---all hallmarks of adaptive immunity, not nonspecific defense.
Conclusion
While fever, inflammation, and intact skin are innate mechanisms offering immediate, generalized protection, lymphocytes are specialized cells of the adaptive immune system that provide a targeted, memorized response. Therefore, lymphocytes are correctly identified as the exception in this list of nonspecific defenses.
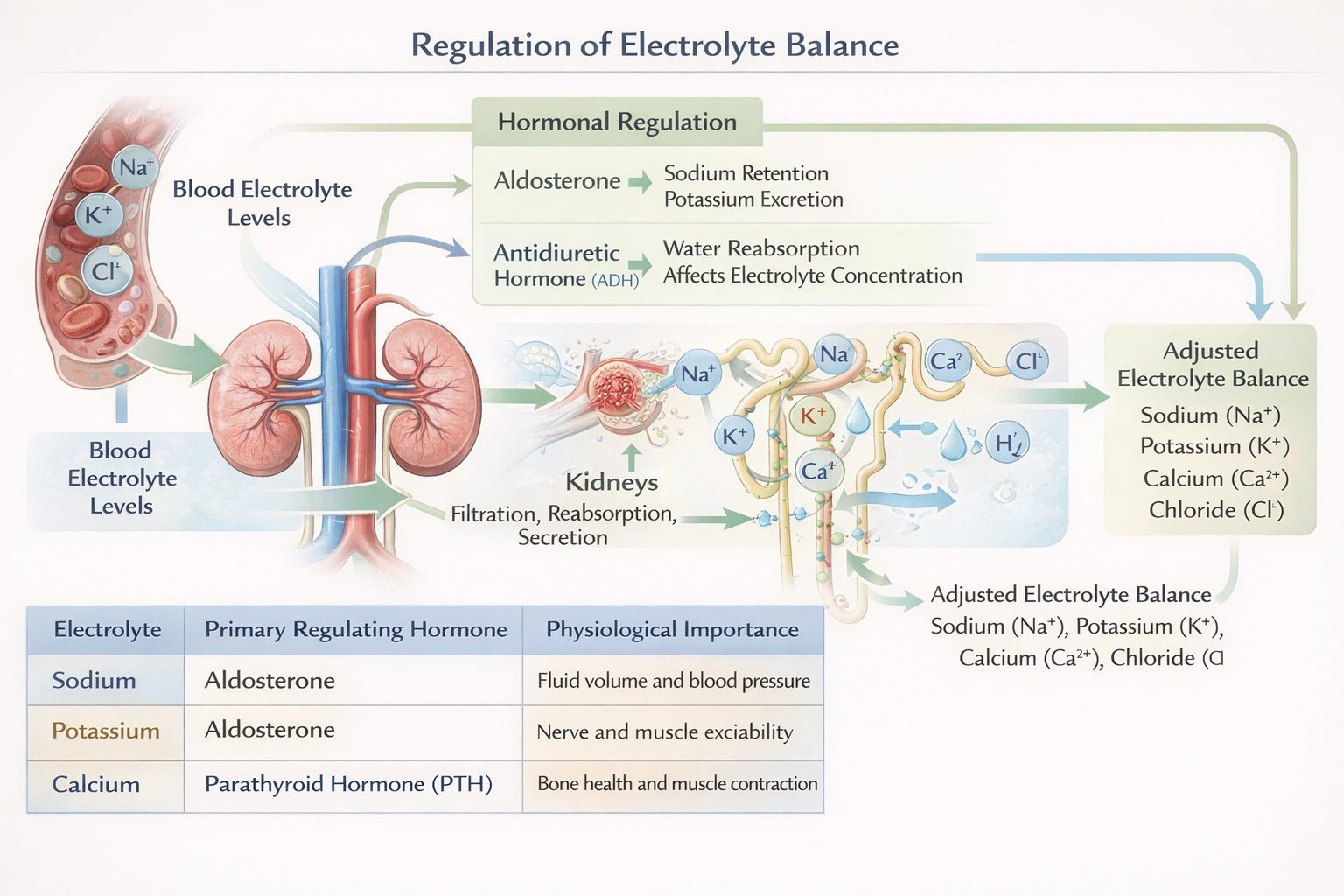
Renal and hormonal systems are regulators of
A.
base buffers.
B. electrolytes.
C. water-based solutes.
D. oxygen in the blood.
Rationale
Renal and hormonal systems are regulators of electrolytes.
The kidneys and the endocrine system work in a tightly integrated manner to maintain electrolyte homeostasis. Electrolytes are minerals in body fluids that carry an electric charge, such as sodium, potassium, chloride, calcium, and phosphate. The kidneys filter the blood and selectively reabsorb or excrete these ions based on the body's needs. This process is finely controlled by hormones, including aldosterone (regulates sodium and potassium), parathyroid hormone (regulates calcium and phosphate), antidiuretic hormone (regulates water balance, which affects electrolyte concentration), and others. This dual system ensures that electrolyte levels remain within narrow, optimal ranges, which is crucial for functions like nerve conduction, muscle contraction, and fluid balance.
A. base buffers
Chemical buffer systems (like bicarbonate, phosphate, and proteins) provide rapid, first-line defense against pH changes. The kidneys do play a slower, crucial role in acid-base balance by excreting hydrogen ions and regenerating bicarbonate, but their primary regulatory focus is not on managing the buffer molecules themselves. The term "base buffers" refers to substances that resist pH change, which is a component of, but not synonymous with, the primary electrolyte-regulating function of the renal-hormonal axis.
B. electrolytes
This is the correct and most precise description. The renal-hormonal system is specialized for the monitoring and adjustment of specific electrolyte concentrations in the blood and body fluids. For example, the kidneys adjust sodium excretion under the influence of aldosterone, and they regulate calcium and phosphate under the influence of parathyroid hormone and calcitriol.
C. water based solutes
This term is too vague. All dissolved substances in body water, including electrolytes, glucose, urea, and gases, are "water based solutes." While the kidneys process many of these, the unique and defining function of the renal-hormonal system is the targeted, independent regulation of specific electrolytes and water balance. The term lacks the specificity of option B.
D. oxygen in the blood
Oxygen levels in the blood are primarily monitored by chemoreceptors and regulated by the respiratory system (which adjusts ventilation) and the cardiovascular system (which adjusts delivery). The kidneys and fluid-balance hormones do not have direct sensors for or mechanisms to regulate the partial pressure of oxygen in the blood.
Conclusion
The integrated renal and hormonal systems are the principal regulators of electrolyte balance in the body. They achieve this through the kidney's filtering capacity directed by hormonal signals, ensuring precise control over the concentrations of ions critical for cellular function and homeostasis.
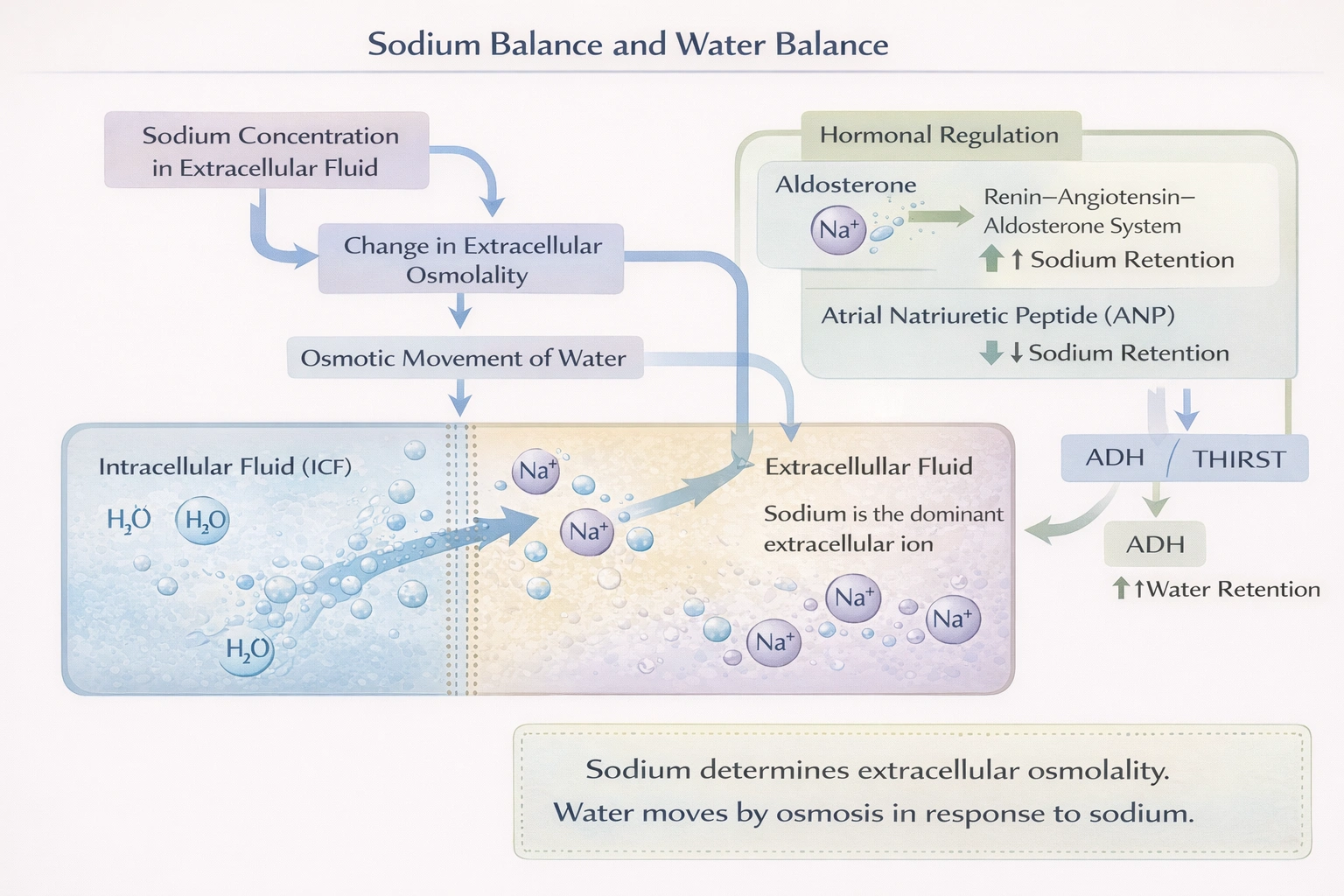
Water balance and sodium balance are closely related.
A.
This is a false statement if water losses are insensible.
B. This is a false statement if water losses are sensible.
C. This is a true statement because water follows sodium.
D. This is a true statement because sodium follows water.
Rationale
Water balance and sodium balance are closely related because water follows sodium osmotically.
Sodium is the primary extracellular solute, and its concentration and total body content are the principal determinants of extracellular fluid (ECF) osmolality. Water moves passively across cell membranes and capillary walls down osmotic gradients. Therefore, the body's regulation of total body sodium through hormonal systems like the renin-angiotensin-aldosterone system (RAAS) and atrial natriuretic peptide (ANP) directly controls ECF volume and, by extension, the distribution and balance of total body water. The statement's truth is derived from this fundamental biophysical principle.
(A) This is a false statement if water losses are insensible: Insensible water losses (e.g., from respiration and sweat) are pure water and can alter plasma osmolality. The body compensates for these losses by adjusting thirst, ADH release, and renal sodium handling, mechanisms that actively maintain the coupled relationship between sodium and water balance.
(B) This is a false statement if water losses are sensible: Sensible losses, such as urine, are a product of the kidney's integrated regulation. The kidneys precisely coordinate the excretion of water and sodium to maintain homeostasis, meaning the core relationship remains intact regardless of the excretory pathway.
(C) This is a true statement because water follows sodium: This option correctly identifies the causal relationship. Sodium is the actively regulated solute, and its movement or retention creates the osmotic forces that dictate passive water movement.
(D) This is a true statement because sodium follows water: This option inverts the true physiological relationship. While rapid water shifts can transiently alter sodium concentration, sodium ions are actively transported (e.g., by the Na+/K+ ATPase pump), and their regulation establishes the osmotic gradients that water follows.
Conclusion
The statement is true based on the law of osmosis; sodium balance is the regulated variable that governs extracellular fluid volume, and water balance is maintained by passively following sodium.
The primary controller of fluid balance in the body is
A.
chloride.
B. magnesium.
C. potassium.
D. sodium.
Rationale
The primary controller of fluid balance in the body is sodium.
Fluid balance is governed by the regulation of osmotic pressure between body compartments. Sodium (Naâº) is the dominant extracellular cation and the primary solute determining extracellular fluid (ECF) osmolality. Because water moves freely across membranes to equalize solute concentration, the total amount of sodium in the body directly dictates the volume of the ECF. The master hormonal systems for fluid regulation the renin-angiotensin-aldosterone system (RAAS), antidiuretic hormone (ADH), and atrial natriuretic peptide (ANP) all primarily function by sensing changes related to sodium (either its concentration or its effect on blood volume) and adjusting renal sodium handling. By controlling sodium reabsorption and excretion, these systems ultimately control water retention and total fluid volume.
(A) chloride: Chloride is the most abundant extracellular anion. Its movement is typically passive and coupled to the active transport of sodium to maintain electrical neutrality. While it contributes to the osmotic pressure of the ECF, its regulation is secondary and follows changes in sodium balance. It is not the primary independent regulator.
(B) magnesium: Magnesium is a crucial intracellular cation that acts as a cofactor for hundreds of enzymatic reactions. Its concentration in the ECF is very low and tightly regulated within a narrow range for functions like nerve conduction and cardiac rhythm. It does not exist in sufficient quantity or variability to control overall body fluid volume.
(C) potassium: Potassium is the dominant intracellular cation and is essential for maintaining the resting membrane potential of all cells. The body rigorously regulates plasma potassium levels due to their critical effects on cardiac and neuromuscular function. However, potassium's primary influence is on intracellular fluid volume and membrane excitability, not on the total volume of the extracellular compartment, which is the key to systemic fluid balance.
(D) sodium: As the principal solute in the ECF, sodium's concentration and total body content are the main determinants of ECF osmolality and volume. Hormonal pathways directly target sodium balance, making its regulation the central mechanism for controlling overall fluid balance.
Conclusion
Sodium is the primary controller of fluid balance because it is the chief osmotic determinant of extracellular fluid volume; regulating sodium retention and excretion is the body's fundamental strategy for maintaining total body water homeostasis.

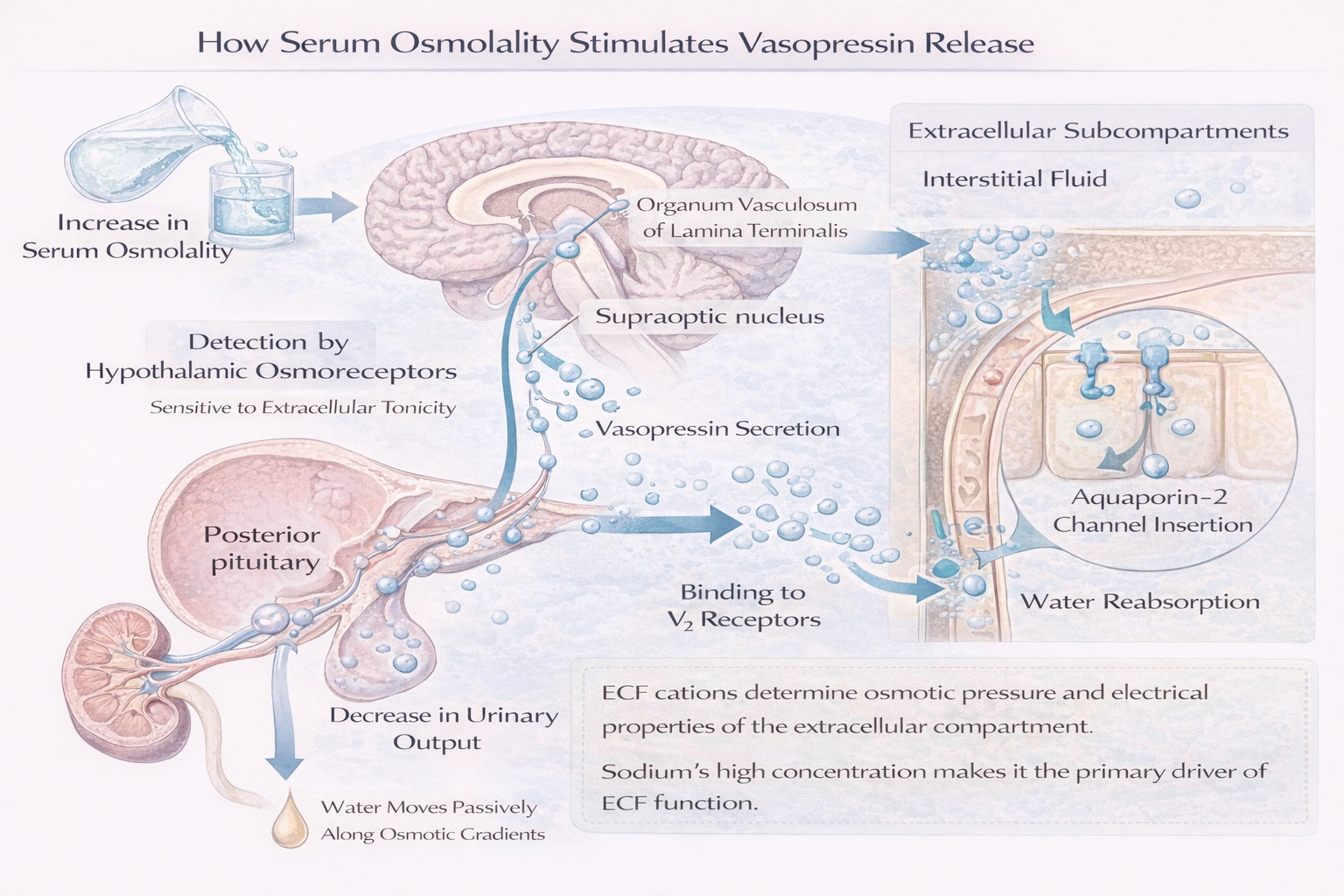
An increase in serum osmolality results in increased secretion of __________ from the pituitary gland, ultimately resulting in __________.
A.
the adrenocorticotropic hormone, less urinary output
B. prolactin, greater urinary output
C. the somatotropic hormone, greater urinary elimination
D. vasopressin, less urinary elimination
Rationale
An increase in serum osmolality results in increased secretion of vasopressin from the pituitary gland, ultimately resulting in less urinary elimination.
Serum osmolality, which reflects the concentration of solutes like sodium in the blood plasma, is closely monitored by specialized osmoreceptor neurons primarily located in the organum vasculosum of the lamina terminalis and the supraoptic nucleus of the hypothalamus. When these osmoreceptors detect an increase as small as 1-2%, they trigger action potentials in the neurosecretory neurons whose cell bodies reside in the hypothalamic supraoptic and paraventricular nuclei. These neurons synthesize vasopressin (antidiuretic hormone) and transport it down their axons to the nerve terminals in the posterior pituitary gland, where it is stored in vesicles. The increased firing rate causes exocytosis of these vesicles, releasing vasopressin into the systemic circulation. The hormone travels to its principal target organ, the kidney. There, it binds to V2 receptors on the basolateral membrane of principal cells in the late distal convoluted tubules and collecting ducts. This binding activates a cAMP second messenger pathway that leads to the insertion of aquaporin-2 water channels into the apical (luminal) membrane. The increased permeability allows water to move osmotically from the hypo-osmotic tubular filtrate into the hyper-osmotic renal medullary interstitium, and then into the bloodstream. Consequently, water is conserved, the urine becomes highly concentrated, and its volume decreases significantly, a process known as antidiuresis.
(A) the adrenocorticotropic hormone, less urinary output: Adrenocorticotropic hormone is a 39-amino acid peptide synthesized by corticotroph cells in the anterior pituitary. Its secretion is controlled by corticotropin-releasing hormone from the hypothalamus in response to circadian rhythms and stress, not by serum osmolality. ACTH stimulates the adrenal cortex's zona fasciculata to produce glucocorticoids like cortisol, which influence metabolism, immune function, and stress adaptation. While cortisol can have minor mineralocorticoid effects at high doses, it does not directly alter renal water permeability. Any effect on urine output would be indirect and not part of the body's primary osmoregulatory feedback loop.
(B) prolactin, greater urinary output: Prolactin is a polypeptide hormone secreted by lactotroph cells in the anterior pituitary. Its primary functions are the development of mammary gland tissue and the initiation and maintenance of lactation postpartum. Its release is tonically inhibited by dopamine from the hypothalamus and can be stimulated by suckling, stress, and certain medications. Prolactin receptors are found in various tissues, but in the kidney, they are involved in regulating ion transport and possibly osmoregulation in some fish species, not in humans. In human physiology, prolactin is not a diuretic hormone and does not respond to changes in plasma osmolality.
(C) the somatotropic hormone, greater urinary elimination: Somatotropic hormone, or growth hormone, is a protein hormone secreted by somatotrophs in the anterior pituitary. Its release is pulsatile, stimulated by growth hormone-releasing hormone and inhibited by somatostatin from the hypothalamus. GH promotes tissue growth, lipolysis, protein anabolism, and insulin resistance, largely through the induction of insulin-like growth factor-1. While GH can increase glomerular filtration rate and renal plasma flow, and has sodium-retaining properties, these are secondary to its growth-promoting and metabolic actions. It is not secreted in response to hyperosmolality, and its overall effect on fluid balance is complex and not diuretic in the context of osmoregulation.
(D) vasopressin, less urinary elimination: Vasopressin is a nine-amino acid neuropeptide synthesized as a larger prohormone in the magnocellular neurons of the hypothalamus. The precise mechanism involves osmoreceptor cells that are distinct from, but synapse with, the vasopressin-producing neurons. These osmoreceptors are intrinsically sensitive to extracellular fluid tonicity due to stretch-inhibited cation channels. Upon activation, they stimulate the vasopressinergic neurons. The released hormone has a very short half-life in the circulation. Its action on the kidney's collecting duct is not instantaneous; it involves a cascade leading to the phosphorylation of aquaporin-2 and its translocation via vesicular trafficking. This system is exquisitely sensitive, allowing for minute-to-minute regulation of water balance. The reduction in urinary elimination is not just a decrease in volume but also involves active urea transport and the generation of a steep medullary osmotic gradient, both of which are modulated by vasopressin.
Conclusion: The body defends against increased serum osmolality through a dedicated neuroendocrine reflex arc: hypothalamic osmoreceptors activate neurosecretory neurons, causing the posterior pituitary to release vasopressin, which then acts on renal collecting ducts to increase water permeability, promote water reabsorption, and produce a small volume of concentrated urine, thereby correcting the initial osmotic disturbance.
What substance is released from the juxtaglomerular apparatus in the nephron when the concentration of sodium in the blood is low?
A.
angiotensin I
B. angiotensin II
C. renin
D. sodium
Rationale
Renin is released from the juxtaglomerular apparatus in the nephron when the concentration of sodium in the blood is low.
The juxtaglomerular apparatus is a specialized structure located at the vascular pole of each renal corpuscle, where the afferent arteriole, efferent arteriole, and distal convoluted tubule converge. It consists of three main cell types: granular (juxtaglomerular) cells in the wall of the afferent arteriole, macula densa cells in the adjacent distal tubule, and extraglomerular mesangial cells. The release of renin, an aspartyl protease enzyme, is the key secretory function of the JGA. It is triggered by three primary stimuli, all related to low effective arterial blood volume or sodium content: 1) Renal Perfusion Pressure (Intrarenal Baroreceptor): A drop in blood pressure (e.g., from hemorrhage, dehydration) reduces stretch on the granular cells (which act as mechanoreceptors), leading to renin release. 2) Macula Densa Sensing (Chemoreceptor): The macula densa cells sense sodium chloride delivery to the distal tubule. Low sodium concentration (more precisely, low chloride ion load due to reduced Na+-K+-2Cl- cotransport) in the tubular fluid causes these cells to release prostaglandins (PGE2), which stimulate adjacent granular cells to secrete renin. 3) Sympathetic Nervous System Activation: Beta-1 adrenergic stimulation of granular cells via renal nerves directly promotes renin secretion. Upon release into the bloodstream, renin cleaves the liver-derived plasma protein angiotensinogen to form the inactive decapeptide angiotensin I. This is the rate-limiting step in the renin-angiotensin-aldosterone system. The subsequent conversion to angiotensin II leads to vasoconstriction and aldosterone secretion, which together increase sodium reabsorption, water retention, and blood pressure, thereby correcting the initial low sodium stimulus.
(A) angiotensin I: Angiotensin I is a biologically inactive precursor peptide. It is generated in the systemic circulation, not within or secreted from the JGA. Its production is entirely dependent on the action of renin on angiotensinogen. It serves solely as a substrate for angiotensin-converting enzyme, primarily on pulmonary endothelial cells, which converts it to the active angiotensin II.
(B) angiotensin II: Angiotensin II is a potent octapeptide effector hormone of the RAAS. It causes powerful arteriolar vasoconstriction, stimulates thirst, increases sympathetic outflow, and stimulates aldosterone release from the adrenal cortex. However, it is not stored or secreted by the JGA. It is formed enzymatically at distant vascular beds after the systemic release of renin initiates the cascade. The JGA's direct secretory product is renin.
(C) renin: Renin is synthesized, stored in cytoplasmic granules, and secreted by the modified smooth muscle cells of the afferent arteriolar wall within the JGA. The granular appearance of these cells is due to the stored renin. The secretion is a carefully regulated process integrating signals from macula densa NaCl sensing, arteriolar pressure, and sympathetic tone. Its enzymatic action on angiotensinogen is the committed step that activates the entire systemic RAAS, making renin release the critical initial event in the hormonal response to low sodium or volume.
(D) sodium: Sodium is an inorganic cation (Na+), the major extracellular electrolyte. It is the substance being regulated, not the regulatory signal itself. The nephron filters, reabsorbs, and excretes sodium. The JGA's function is to monitor sodium delivery (via the macula densa) and renal perfusion pressure (which correlates with sodium/volume status) and respond by secreting renin to mobilize hormonal systems that will ultimately increase sodium retention. Sodium itself is not a substance synthesized and secreted by the JGA cells.
Conclusion: In response to a low sodium concentration or low blood pressure, the juxtaglomerular apparatus functions as a biosensor and secretory unit, directly releasing the enzyme renin into the circulation to initiate the hormonal cascade that restores sodium balance and blood volume.
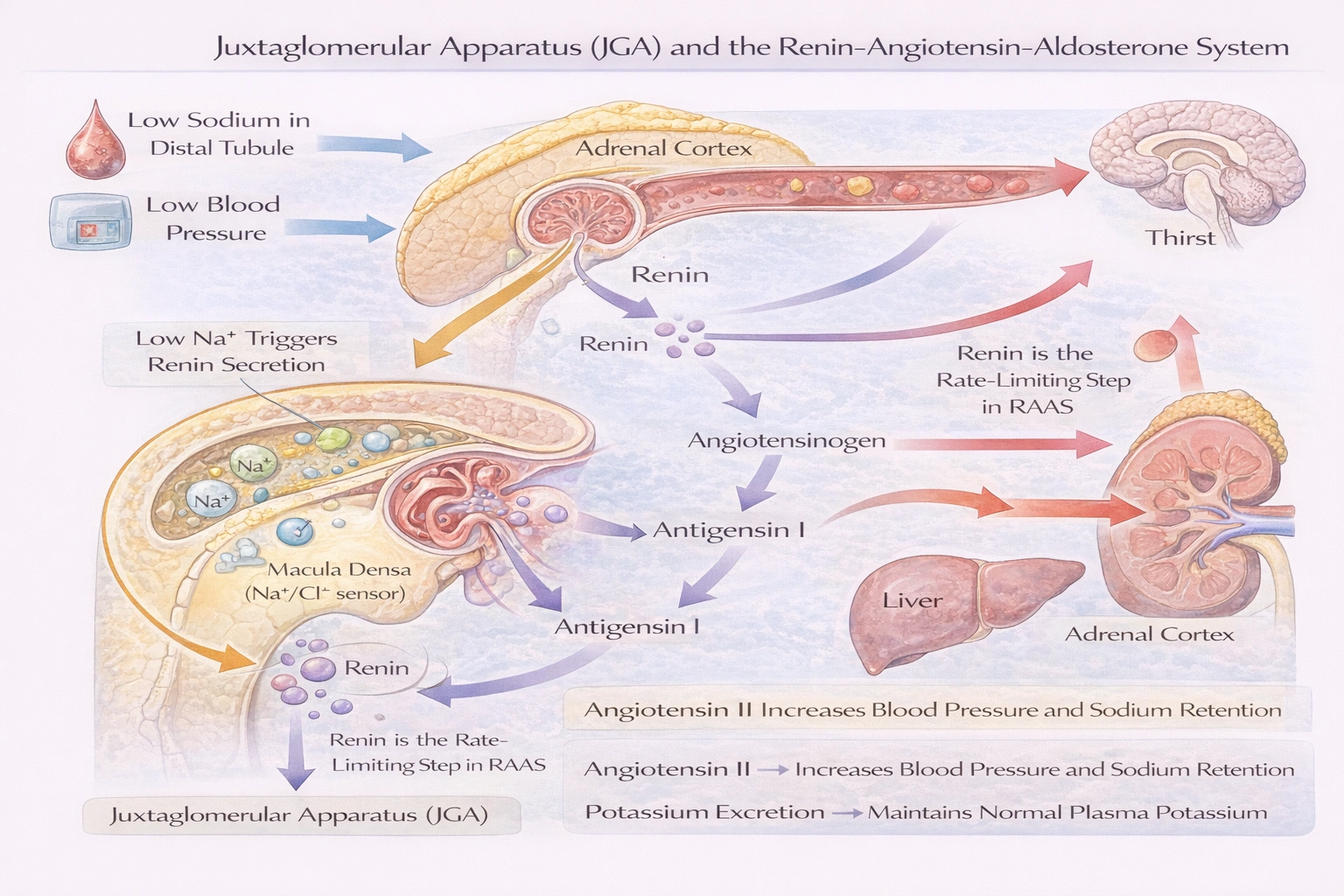
Included in the components of bile are
A.
bilirubin, bile salts, cholesterol, and lecithin.
B. ketone bodies, bilirubin, trace minerals, and glycerol.
C. proteolytic enzymes, bile salts, trypsin, and water.
D. synthesized hormones, bilirubin, bile salts, and pyruvic acid.
Rationale
Included in the components of bile are bilirubin, bile salts, cholesterol, and lecithin.
Bile is a complex, bitter-tasting fluid synthesized by hepatocytes in the liver, stored and concentrated in the gallbladder, and secreted into the duodenum via the common bile duct. Its primary functions are the emulsification of dietary fats to increase surface area for enzymatic action and the elimination of certain waste products. The major organic constituents that define its composition are: 1) Bilirubin: The principal pigment in bile, a yellow-orange compound derived from the catabolism of the heme portion of hemoglobin from senescent red blood cells, which is metabolized by gut bacteria to form stercobilin (giving feces its brown color). 2) Bile Salts: Amphipathic steroid molecules synthesized from cholesterol within hepatocytes (primary bile acids like cholic and chenodeoxycholic acid) that are later conjugated with glycine or taurine to form bile salts. Their hydrophobic and hydrophilic regions allow them to act as biological detergents, emulsifying large lipid globules into smaller micelles. 3) Cholesterol: A normal dietary lipid excreted in bile; it serves as both a precursor for bile salt synthesis and a waste product. Its solubility in bile is maintained by bile salts and lecithin; imbalances can lead to cholesterol gallstone formation. 4) Lecithin (Phosphatidylcholine): A phospholipid secreted by hepatocytes that works in concert with bile salts. While bile salts solubilize cholesterol, lecithin expands the bile salt micelles, greatly increasing their capacity to incorporate and transport cholesterol and fat-soluble vitamins in a soluble, non-precipitable form. Bile also contains water, electrolytes (sodium, potassium, bicarbonate), and bicarbonate ions which help neutralize gastric acid, but the listed organic components are its key functional and diagnostic constituents.
(A) bilirubin, bile salts, cholesterol, and lecithin. This list is a precise and complete catalog of the defining organic solutes in bile. Each component plays a critical and interconnected role: bilirubin for excretion and pigmentation, bile salts and lecithin as emulsifying agents facilitating fat digestion and cholesterol solubility, and cholesterol as both a metabolic substrate and excreted product. Their relative concentrations determine the lithogenicity of bile (its tendency to form stones).
(B) ketone bodies, bilirubin, trace minerals, and glycerol. Ketone bodies (acetoacetate, β-hydroxybutyrate, acetone) are water-soluble fuel molecules generated by hepatic mitochondria during states of carbohydrate deprivation (starvation, uncontrolled diabetes) for export to peripheral tissues like the brain and heart. They are metabolic intermediates, not secretory products destined for biliary excretion. Glycerol is a three-carbon molecule released during lipolysis of triglycerides in adipose tissue; it is metabolized in the liver for gluconeogenesis or glycolysis, not secreted into bile. While bile does contain trace amounts of minerals (e.g., calcium, which can precipitate as gallstones), these are not defining components, and their inclusion with ketone bodies and glycerol renders the list physiologically inaccurate for bile's standard composition.
(C) proteolytic enzymes, bile salts, trypsin, and water. This option incorrectly attributes digestive enzymes to bile. Proteolytic enzymes (e.g., pepsinogen, trypsinogen, chymotrypsinogen) are produced by the stomach and pancreas, not the liver. Trypsin, specifically, is a potent pancreatic protease secreted in its inactive form (trypsinogen) into the pancreatic duct, which merges with the common bile duct at the ampulla of Vater. However, it is not a constituent of bile itself; bile and pancreatic juices mix in the duodenum but are produced by separate organs. Water is the solvent base of bile (constituting about 97% of its volume), but its presence does not validate the erroneous inclusion of proteolytic enzymes.
(D) synthesized hormones, bilirubin, bile salts, and pyruvic acid. Hormones synthesized by the liver (e.g., angiotensinogen, thrombopoietin, insulin-like growth factor 1) are secreted into the bloodstream, not the biliary tree. Steroid hormones from other glands are metabolized by the liver and may be conjugated for biliary or urinary excretion, but they are not standard, primary "components" of bile in the same sense as bile salts. Pyruvic acid (pyruvate) is a central metabolite in glycolysis and gluconeogenesis; it is actively transported and metabolized within cells, not secreted in significant amounts into bile. Therefore, this list combines two correct components with two unrelated metabolic intermediates, making it an incorrect description of bile's composition.
Conclusion: The functional and characteristic organic constituents of bile are the waste product bilirubin, the emulsifying detergent bile salts and the phospholipid lecithin, and the lipid cholesterol, making option (A) the accurate and comprehensive list.
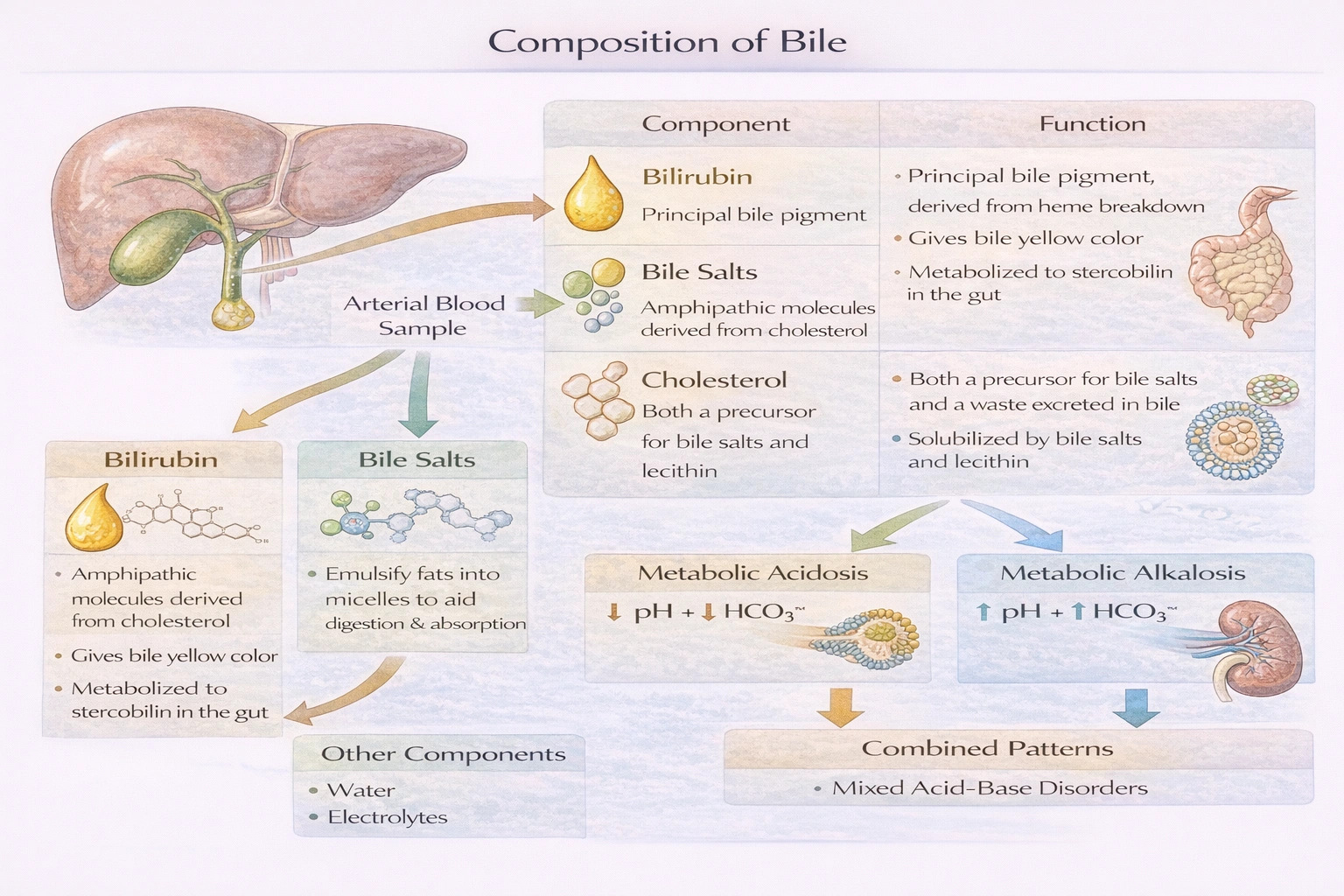
Which structure stores feces for elimination?
A.
appendix
B. lower gastrointestinal tract
C. pylorus
D. rectum
Rationale
The structure that stores feces for elimination is the rectum.
The final phase of colonic processing involves the temporary storage of solid waste material (feces) prior to voluntary expulsion, a function specifically localized to the rectum. The rectum is the distal 12-15 cm segment of the large intestine, following the sigmoid colon and preceding the anal canal. It is anatomically and physiologically specialized as a reservoir: its walls are highly distensible, featuring three permanent transverse folds known as the rectal valves (of Houston) that help support the weight of the fecal mass and prevent premature urge. When mass peristaltic movements of the descending and sigmoid colon propel feces into the rectum, the resulting distension activates stretch receptors in the rectal wall. This stimulates the defecation reflex, a spinal cord-mediated reflex that can be voluntarily inhibited or facilitated by the cerebral cortex. The rectum maintains continence through the tonic contraction of the internal anal sphincter (smooth muscle, involuntary) and the conscious control of the external anal sphincter (skeletal muscle, voluntary). No other segment of the gastrointestinal tract is primarily adapted for this static storage role; the colon forms and transports feces, while the rectum serves as the holding chamber.
(A) appendix. The vermiform appendix is a narrow, blind-ended, tubular structure attached to the posteromedial wall of the cecum. It is considered a component of the gut-associated lymphoid tissue (GALT) and functions as a secondary lymphoid organ involved in immune surveillance, particularly in early life. It may also act as a reservoir for commensal gut flora. Its lumen is minute, and it does not receive or store fecal material. Ingested contents do not routinely enter it, and its primary clinical relevance is its potential for inflammation (appendicitis), not fecal storage.
(B) lower gastrointestinal tract. This is a broad, non-specific clinical term that typically refers to the colon and rectum collectively. While the colon (ascending, transverse, descending, and sigmoid) is responsible for absorbing water and electrolytes, converting liquid chyme into semisolid feces, and propelling it forward via haustral churning and mass movements, it is not a dedicated storage structure. The term "lower gastrointestinal tract" is an anatomical region, not a single defined organ, and its functions are diverse, including fermentation, absorption, and transit, rather than static storage.
(C) pylorus. The pylorus is the funnel-shaped distal segment of the stomach that connects to the duodenum via the pyloric sphincter. Its functions are mechanical and regulatory: it acts as a grinding mill to further break down gastric contents and, critically, as a gatekeeper that regulates the rate of gastric emptying. It allows only small, liquefied amounts of chyme (partially digested stomach contents) to pass into the duodenum. It operates in the upper GI tract long before feces are formed and has no anatomical or functional relationship to the storage of solid waste.
(D) rectum. As described, the rectum is the specialized storage chamber. Its lining is simple columnar epithelium with abundant mucus-secreting goblet cells to lubricate the passage of feces during defecation. Its muscular walls (longitudinal and circular) are capable of sustained contraction to retain contents. The coordinated relaxation of these muscles and the anal sphincters allows for controlled elimination. Its sensory capacity to detect distension is fundamental to the defecation process.
Conclusion: The rectum is the definitive anatomical structure specialized for the temporary storage of fecal matter, acting as the sensory trigger point and reservoir that enables controlled defecation.
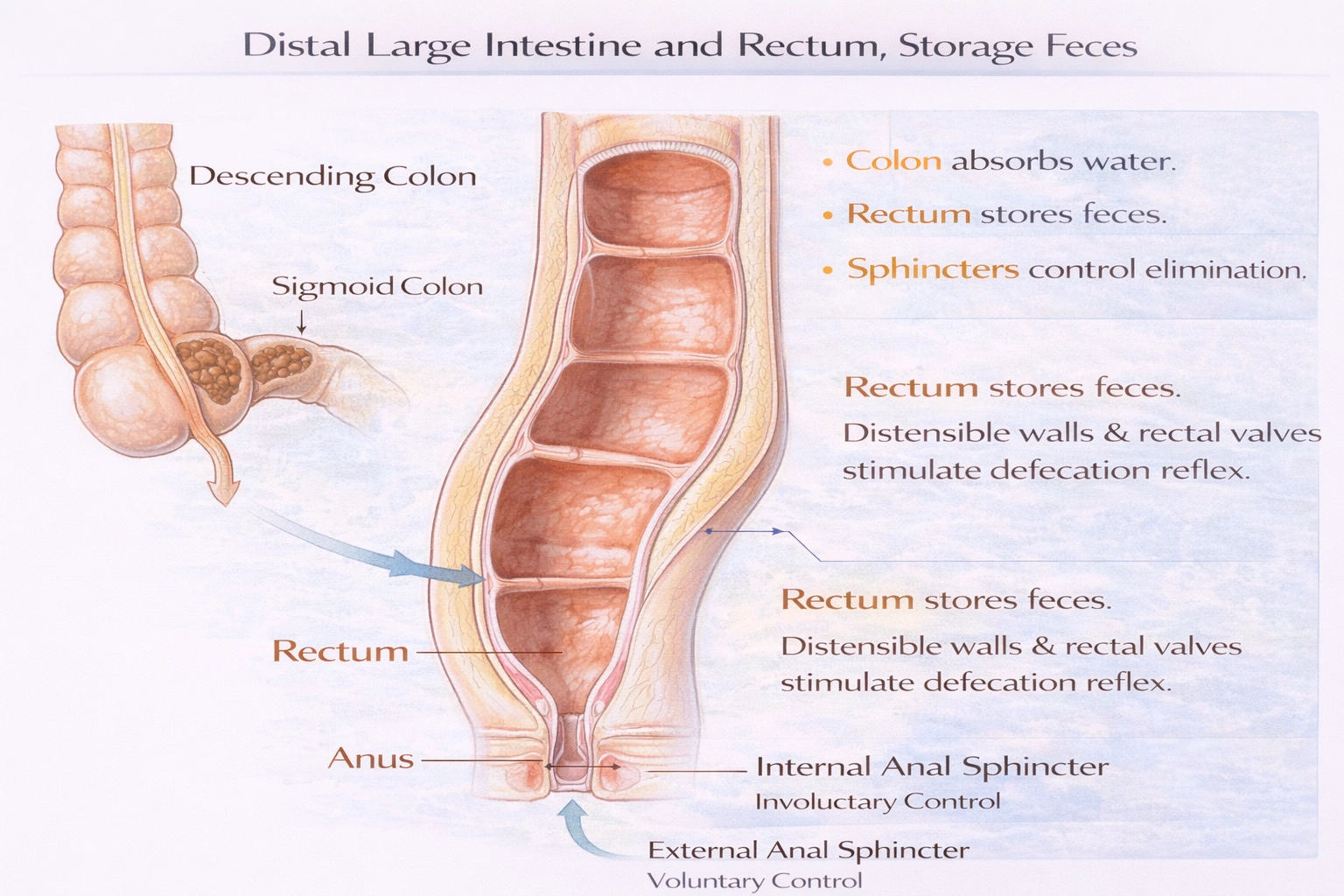
What valve prevents the return of feces to the small intestine?
A.
appendix
B. ileocecal
C. lower sphincter
D. sigmoid
Rationale
The valve that prevents the return of feces to the small intestine is the ileocecal valve.
The ileocecal valve (also termed the ileocolic valve) is the critical anatomical and functional structure that regulates the unidirectional flow of intestinal contents from the ileum (the terminal portion of the small intestine) into the cecum (the proximal pouch of the large intestine) and, most importantly, prevents the reflux of colonic material back into the ileum. Anatomically, it is not a true valve with cusps but rather a functional sphincter formed by the thickened circular smooth muscle of the terminal ileum as it invaginates into the cecal wall. This creates a nipple-like protrusion with a slit-like opening. Its functions are twofold: 1) Regulated Ileal Emptying: It relaxes in response to the "gastroileal reflex" (enhanced ileal motility after a meal) and hormonal signals like gastrin, allowing small amounts of liquid ileal chyme to pass into the cecum. 2) Reflux Prevention: Its tonic contraction, combined with the angulation of the ileocecal junction and the flap-like mucosal covering, creates a competent one-way barrier. This is essential to prevent the backflow of colonic contents, which contain a high density of bacteria (approximately 10¹¹ to 10¹² CFU/mL) and formed fecal matter, into the relatively sterile ileum. Such reflux could lead to small intestinal bacterial overgrowth (SIBO), malabsorption, and inflammation.
(A) appendix. The appendix is a blind-ended, tubular diverticulum arising from the posteromedial aspect of the cecum. It is primarily composed of lymphoid tissue and is considered part of the mucosal immune system. It may serve as a reservoir for beneficial gut flora. It has no valvular structure or sphincteric muscle and plays no role in regulating the flow of intestinal contents between the small and large intestines. It is an anatomical dead-end.
(B) ileocecal. This is the correct anatomical term. The ileocecal valve's competence is maintained by intrinsic myenteric plexus reflexes and the pressure gradient between the ileum and cecum. Distension of the cecum causes the valve to contract more tightly, enhancing its anti-reflux function. Its integrity is crucial for maintaining the distinct environments of the small and large intestines.
(C) lower sphincter. This is a vague, non-standard term. In different clinical contexts, "lower sphincter" might colloquially refer to the lower esophageal sphincter (LES) (at the gastroesophageal junction, preventing gastric reflux) or the internal anal sphincter (part of the anal canal, involved in fecal continence). The LES is located between the esophagus and stomach, and the anal sphincters are at the distal end of the GI tract. Neither is situated at the ileocecal junction or prevents coloileal reflux.
(D) sigmoid. "Sigmoid" refers to the sigmoid colon, the S-shaped segment of the colon between the descending colon and the rectum. It functions as a conduit and a temporary reservoir for feces before they enter the rectum. It possesses strong circular muscle layers that generate mass movements, but it is not a valve and does not separate the small and large intestines or prevent retrograde flow at the ileocecal junction.
Conclusion: The ileocecal valve is the specialized functional sphincter at the junction of the small and large intestines that ensures one-way movement, effectively preventing the retrograde flow of fecal material and bacteria into the small intestine.
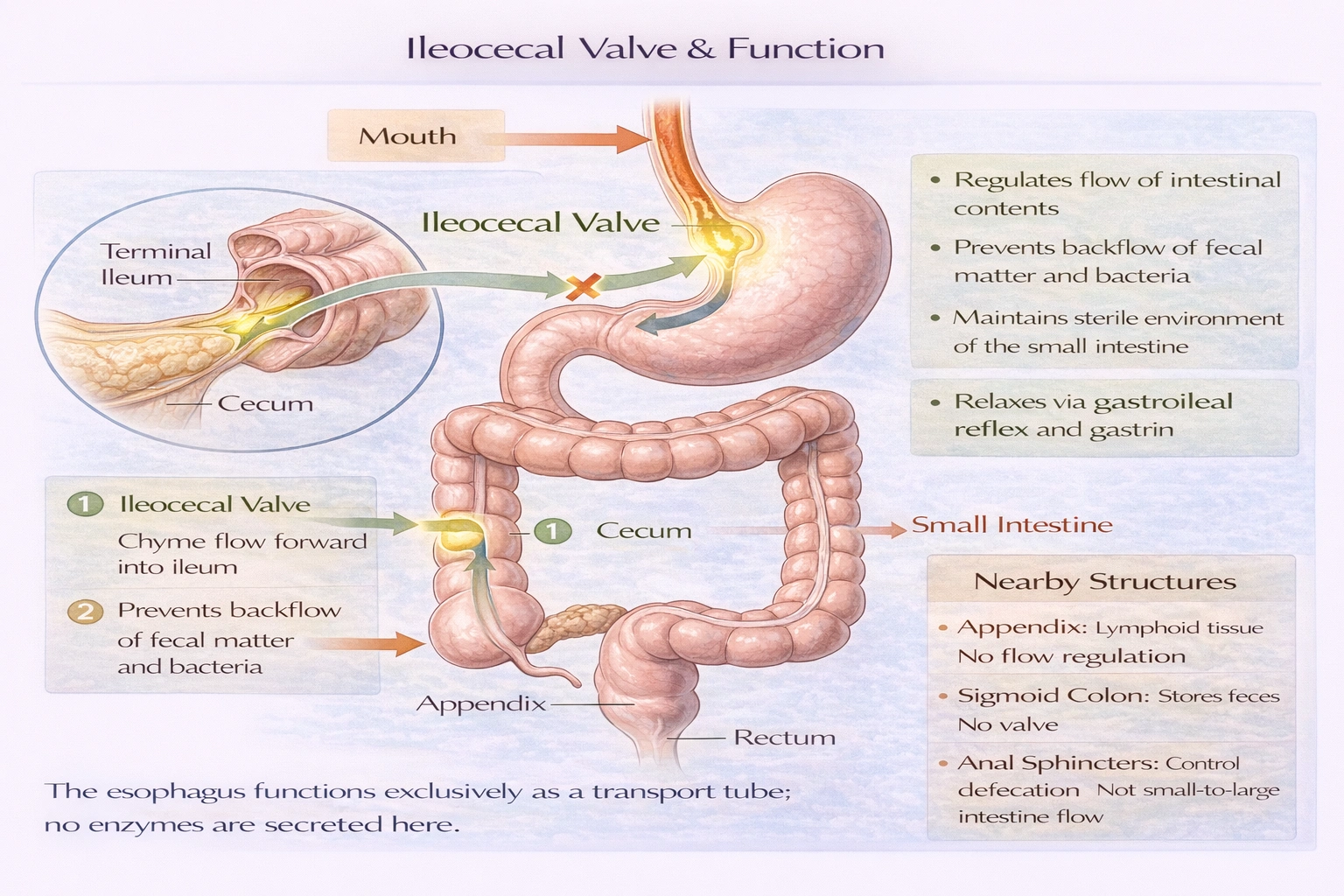
HESI A2 Exams
Biology Quizzes
3 Practice Tests
Biology Quizzes
3 Practice Tests
Chemistry Quizzes
3 Practice Tests
Chemistry Quizzes
3 Practice Tests
Reading Quizzes
4 Practice Tests
Reading Quizzes
4 Practice Tests
Grammar Quizzes
3 Practice Tests
Grammar Quizzes
3 Practice Tests
Vocabulary Quizzes
3 Practice Tests
Vocabulary Quizzes
3 Practice Tests
Physics Quizzes
3 Practice Tests
Physics Quizzes
3 Practice Tests
HESI Quizzes
3 Practice Tests
HESI Quizzes
3 Practice Tests