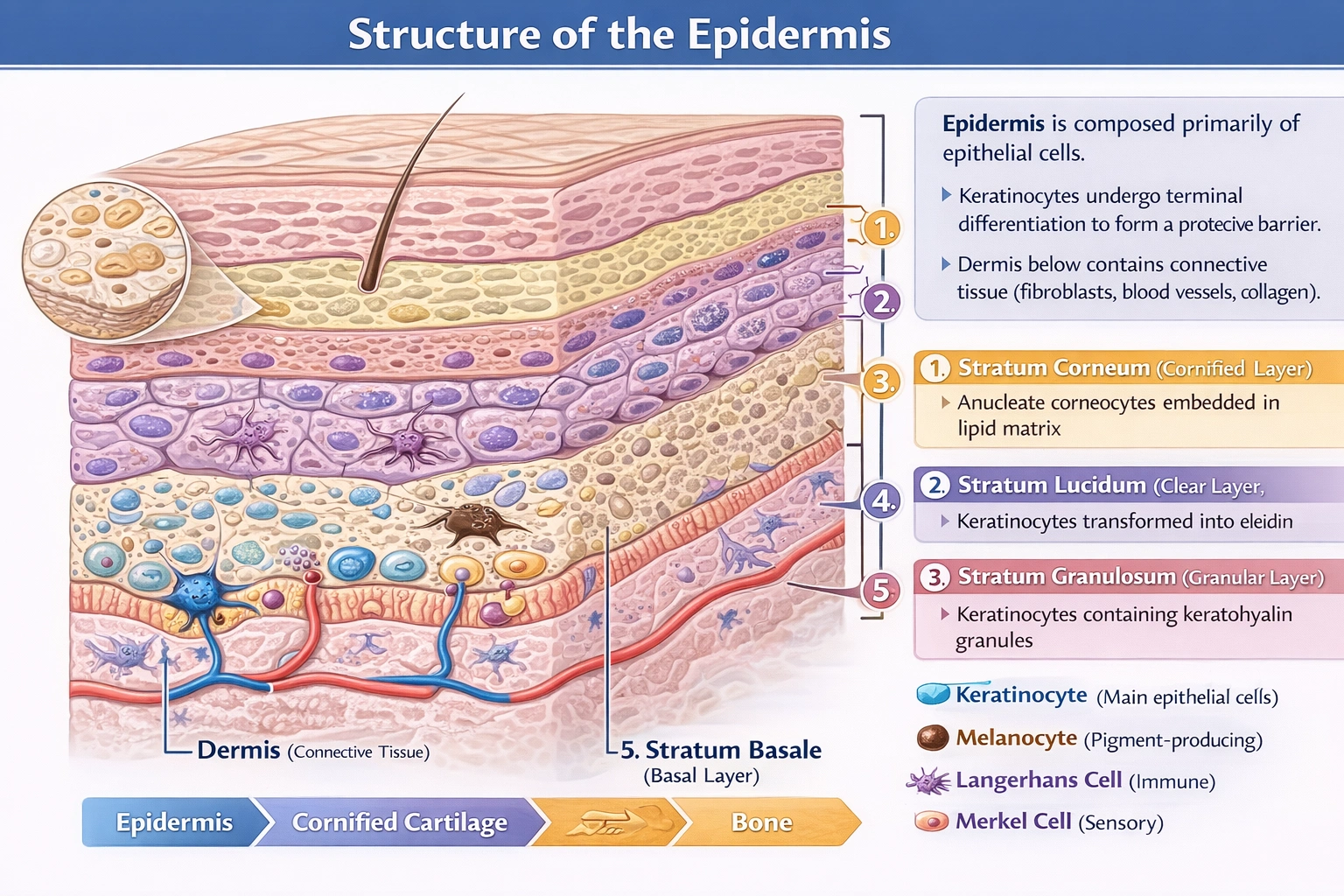
The epidermis is composed of what type of cells?
-
A
Osteoclasts
-
B
Connective
-
C
Dendritic
-
D
Epithelial
The epidermis consists primarily of stratified squamous epithelial cells.
Epithelial tissue characteristics define the epidermis: tightly packed cells with minimal extracellular matrix, apical-basal polarity, attachment to basement membrane via hemidesmosomes, and avascularity—distinguishing it from underlying dermal connective tissue that contains blood vessels, nerves, and extracellular matrix components like collagen and elastin.
A) Osteoclasts
Osteoclasts are multinucleated bone-resorbing cells derived from hematopoietic monocyte/macrophage lineage, functioning exclusively in skeletal tissue remodeling within bone marrow cavities and on bone surfaces. These cells express tartrate-resistant acid phosphatase and create resorption lacunae through proton secretion—activities entirely absent in epidermal tissue. Osteoclasts never appear in skin histology; their presence would indicate pathological bone invasion rather than normal epidermal composition.
B) Connective
Connective tissue comprises cells embedded in abundant extracellular matrix (collagen, elastin, ground substance) and includes dermis, adipose tissue, cartilage, and bone—not epidermis. The dermis underlying the epidermis contains fibroblasts, collagen bundles, blood vessels, and immune cells characteristic of connective tissue. Epidermal cells, by contrast, form tightly adherent layers with minimal intercellular substance, connected by desmosomes and tight junctions—hallmarks of epithelial rather than connective tissue organization. Confusing epidermis with dermis represents a fundamental histological error.
C) Dendritic
Dendritic cells (Langerhans cells in epidermis) represent a minor immune cell population comprising approximately 2–4% of epidermal cells—they are not the primary cellular component. These bone marrow-derived antigen-presenting cells migrate through epidermis to capture pathogens and activate T-cells in lymph nodes. While present and functionally important for skin immunity, dendritic cells do not constitute the structural or numerical majority of epidermal tissue; keratinocytes form over 90% of epidermal cells. Describing the epidermis as "composed of dendritic cells" misrepresents its fundamental histological composition.
D) Epithelial
The epidermis forms a keratinized stratified squamous epithelium composed predominantly of keratinocytes progressing through differentiation stages: basal layer (stratum basale) contains mitotically active cuboidal keratinocytes attached to basement membrane; spinous layer (stratum spinosum) features polyhedral keratinocytes connected by desmosomes; granular layer (stratum granulosum) contains keratohyalin granules; clear layer (stratum lucidum, thick skin only) shows eleidin transformation; and cornified layer (stratum corneum) consists of anucleate corneocytes embedded in lipid matrix. Additional epithelial-derived cells include melanocytes (neural crest origin) producing melanin and Merkel cells functioning as mechanoreceptors—but keratinocytes remain the defining epithelial component creating the barrier structure.
Conclusion:
Epithelial tissue organization defines the epidermis through its cellular architecture: avascular layers of tightly adherent keratinocytes undergoing terminal differentiation to form a protective barrier. While specialized cells like Langerhans dendritic cells, melanocytes, and Merkel cells contribute important functions, they represent minor populations within an overwhelmingly epithelial structure. Osteoclasts belong exclusively to bone tissue,
connective tissue characterizes the underlying dermis, and dendritic cells—though present—do not constitute the primary cellular composition. Option D correctly identifies epithelial cells as the fundamental building blocks of epidermal histology, essential for understanding skin barrier function, wound healing, and dermatological pathology.