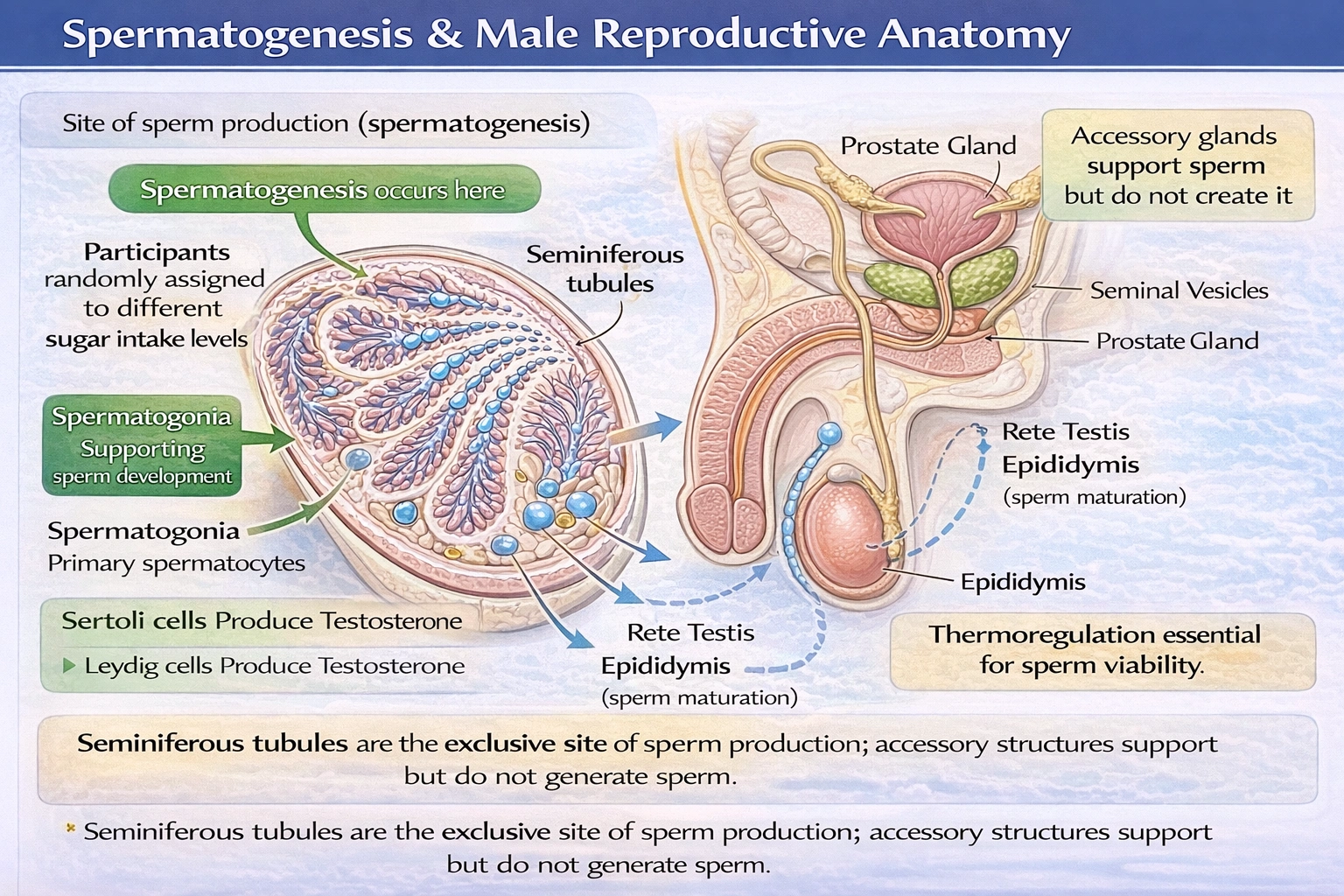
Which of the following creates sperm?
-
A
Prostate gland
-
B
Seminal vesicles
-
C
Scrotum
-
D
Seminiferous tubules
Seminiferous tubules within the testes serve as the exclusive site of spermatogenesis.
These highly coiled tubules, comprising approximately 80% of testicular volume, contain specialized Sertoli cells that nurture developing germ cells through mitotic proliferation, meiotic division, and spermiogenic maturation over approximately 64 days in humans—ultimately releasing immature sperm into the tubule lumen for transport to the epididymis.
A) Prostate gland
The prostate gland contributes 25–30% of seminal fluid volume—a milky, slightly acidic secretion containing proteolytic enzymes (prostate-specific antigen), citric acid, zinc, and acid phosphatase that activate sperm motility and neutralize vaginal acidity post-ejaculation. However, the prostate produces no sperm cells; it functions solely as an accessory gland modifying the seminal environment. Prostatic fluid mixes with sperm and other secretions in the ejaculatory ducts but plays no role in germ cell production or maturation. Benign prostatic hyperplasia or prostatectomy may affect semen volume and consistency but does not eliminate sperm production if testes remain intact.
B) Seminal vesicles
Seminal vesicles contribute 60–70% of seminal fluid volume—producing a viscous, fructose-rich alkaline secretion that provides metabolic energy (fructose) for sperm motility and contains prostaglandins that stimulate uterine contractions to facilitate sperm transport. Despite their substantial contribution to semen composition, seminal vesicles generate no spermatozoa. Their secretions mix with sperm in the ejaculatory ducts during emission, but spermatogenesis occurs exclusively within testicular tissue. Men lacking seminal vesicles (congenital absence or surgical removal) produce reduced-volume semen but can still generate sperm if testicular function remains normal.
C) Scrotum
The scrotum functions as a thermoregulatory sac maintaining testicular temperature 2–3°C below core body temperature—essential for viable spermatogenesis, which fails at normal body temperature. Dartos and cremaster muscles adjust scrotal position relative to the body in response to ambient temperature, while the pampiniform plexus provides counter-current heat exchange cooling arterial blood entering the testes. Despite this critical supportive role, the scrotum contains no spermatogenic tissue; it serves purely as a protective, temperature-regulating container for the testes. Cryptorchidism (undescended testes retained in the abdomen) demonstrates that testicular tissue—not scrotal tissue—produces sperm, albeit with impaired function at elevated temperatures.
D) Seminiferous tubules
Seminiferous tubules house the complete spermatogenic sequence within their epithelial lining: Type A spermatogonia (stem cells) undergo mitosis to self-renew and produce Type B spermatogonia, which differentiate into primary spermatocytes entering meiosis I to form secondary spermatocytes, then meiosis II to produce haploid spermatids. Spermiogenesis transforms round spermatids into elongated spermatozoa through acrosome formation, flagellum development, nuclear condensation, and cytoplasmic shedding—all supported by Sertoli cells providing nutrients, growth factors, and blood-testis barrier protection. Mature sperm release (spermiation) deposits immotile sperm into the tubule lumen for transport to the rete testis and epididymis, where they gain motility and fertilization capacity. No other human structure performs this gametogenic function.
Conclusion:
Spermatogenesis occurs exclusively within seminiferous tubules of the testes, where precisely orchestrated mitotic, meiotic, and differentiation processes transform diploid stem cells into haploid spermatozoa. Accessory structures support reproduction through distinct functions: the scrotum provides thermoregulation, seminal vesicles and prostate contribute seminal fluid components, but none generate sperm cells. Understanding this anatomical specialization proves clinically significant male infertility evaluation focuses on testicular biopsy and hormonal assessment of spermatogenesis rather than accessory gland function, while vasectomy interrupts sperm transport without affecting production. Option D correctly identifies seminiferous tubules as the singular site of sperm creation, distinguishing gamete production from seminal fluid secretion or thermoregulatory support.